Journal of
eISSN: 2373-6410


Case Report Volume 5 Issue 3
1General physician, Kashan University of Medical Sciences, Iran
2Department of Pediatrics, Kashan University of Medical Sciences, Iran
3Department of Neurosurgery, Kashan University of Medical Sciences, Iran
Correspondence: Saeed Banaee, Assistant professor of neurosurgery, Department of Neurosurgery, Kashan University of Medical Sciences, IR Iran
Received: April 23, 2016 | Published: November 18, 2016
Citation: Motaghedifard M, Talebian A, Fakharian E, Banaee S, Jafarian A (2016) Bilateral Subdural Hygroma in a Case with Sylvian Arachnoid Cyst. JNeurol Stroke 5(3): 00179. DOI: DOI: 10.15406/jnsk.2016.05.00179
Arachnoid cysts are congenital lesions developing from arachnoid membrane. The incidence of arachnoid cysts in the general population is around 0.1% and their most common place is middle fossa. Arachnoid cysts usually present during childhood and are identified incidentally. When symptomatic, the most common presentation includes headache and seizure. The popular treatment for this lesion is surgery. In this case report, we describe a 12-year-old boy with a middle cranial fossa arachnoid cyst presenting with progressive headache, and bilateral subdural hygroma following a trivial trauma.
Keywords:Bilateral Subdural Hygroma, Arachnoid cyst, Trauma
Arachnoid cysts are congenital lesions developing within the arachnoid membrane. They are non-neoplastic, benign lesions filled with cerebrospinal fluid (CSF) or a fluid similar to it.1 Their most common place is in the middle fossa. They are enclosed by the arachnoid membrane.2,3
Arachnoid cysts are relatively rare. Their incidence in the general population is around 0.1% on the base of autopsy studies, with an estimated incidence between 0.5% and 1.6%.4 Arachnoid cysts most commonly present during childhood and are usually identified incidentally. About 75% of intracranial arachnoid cysts presented before 3 years of age in one series.5 The most common symptoms include headache and seizures.
When there is hydrocephalus or intracranial hypertension the common treatment is surgery.6
Intracranial hypertension secondary to arachnoid cyst rupture especially in the subdural space is a rare clinical entity.7,8
In this case report, we describe a 12 year old boy with bilateral subdural hygroma and a middle cranial fossa arachnoid cyst presenting with progressive headache following a trivial head trauma. Based on our best knowledge this is not reported in the literature.
A 12-year-old boy had a falling down while playing about 40 days before his admission to the hospital. His occiput was injured in the event.
He had only dizziness immediately after trauma for 2-3 minutes but had no laceration, bleeding, nausea, vomiting, loss of consciousness (LOC), seizure, post-traumatic amnesia (PTA), etc. He had mild, left parietal beating headache that gradually changed to a generalized one associated with nausea and progressive non bloody vomiting, 3 days after trauma. Vomiting was correlated with eating.
He was referred to neurosurgery clinic. On neurological examination his optic disk was flat and cranial nerves were normal. His meningeal signs were positive. Computed tomographic (CT) scan of brain (Figure 1) showed a hypo-dense lesion in left middle cranial fossa with some squeezing of the ventricular system without midline shift. Brain magnetic resonance imaging (MRI) showed the lesion in the same place, widening Sylvian fissure, compressing temporal lobe and squeezing lateral ventricles. It had the same intensity as cerebrospinal fluid (CSF). There was also fluid collection in both frontal subdural spaces hypo-intense on T1 Figure 2 and hyper-intense on T2 images Figure 3. The findings were suggestive of Sylvian fissure arachnoid cyst and bilateral subdural hygroma.
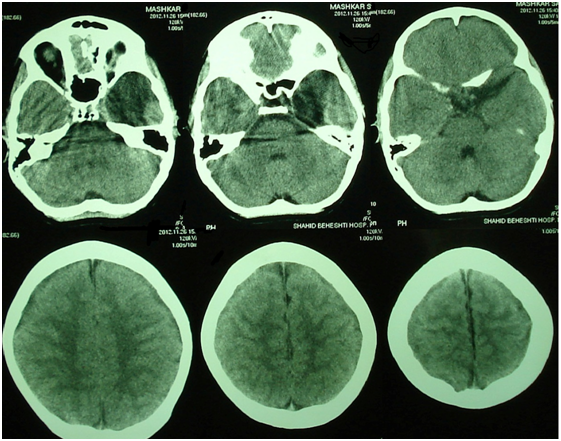
Figure 1 Brain CT scan revealed an extra-axial cystic lesion in the left middle fossa and Sylvian fissure suggestive of arachnoid cyst.
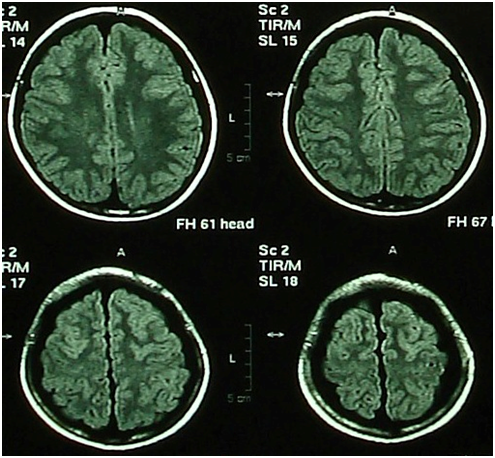
Figure 2 Magnetic resonance imaging of brain showed T1W subdural hypointensity in the left middle fossa compressing temporal lobe and bilateral fronto-parietal convexities.
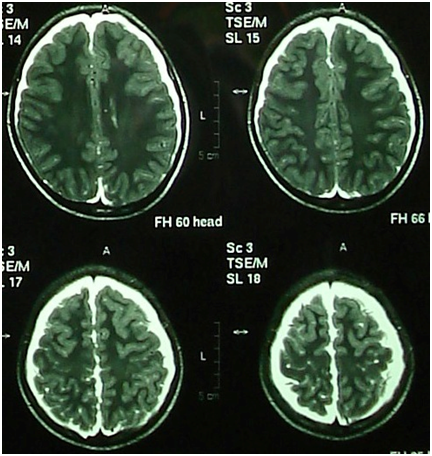
Figure 3 Magnetic resonance imaging of brain. showed T2W subdural hyperintensity in the temporal region and bilateral convexities compressing temporal lobe on the left side.
He was admitted to hospital for craniotomy, fenestration and marsupialization of the cyst into subarachnoid spaces, and evacuation of hygroma. Postoperative imaging Figure 4 showed resolution of subdural hygroma with small extracranial collection of CSF. He discharged from hospital in good condition with disappearance of all of his complains. In follow up visit, he had no meningeal signs. His neurologic examination was also normal.
Intracranial arachnoid cysts are congenital malformations that form by the splitting of the arachnoid membranes due to an increased pulsation of the CSF.9
They are considered intra arachnoidal in location and account for 1% of the intracranial mass lesions.10 They are located in the middle cranial fossa in 25-80% of cases. Almost all of these cysts are unilateral, with a slight predilection for the left side.11
A progressive increase in cyst volume may occur in many cases.12 Intra-cystic hemorrhage, an osmotic gradient allowing a passive fluid-diffusion into the cyst, a ball-valve mechanism or an active secretion from the cyst wall and pulsation of intracystic fluid of venous or arterial origin are some theories for explaining the cyst growth.10,13,14
Surgical indications and techniques should be based on the type of arachnoid cyst (communicating or non-communicating), growth of the cyst, compression or displacement of the surrounding neurovascular structures, and most importantly the patient’s symptomatology and on-going clinical course.
Sixty to ninety percent of arachnoid cysts present during childhood.15,16 Clinical presentation varies primarily by age and location of the lesion. Some arachnoid cysts remain asymptomatic throughout life.
The most common presenting symptom is headache, which may be due to local mass effect, high intracranial pressure (ICP), or hydrocephalus.17 Arachnoid cysts of the middle cranial fossa may be associated with hemorrhage, but this complication has been considered very infrequent. Hemorrhage into or around an arachnoid cyst is primarily precipitated by minor trauma and, very rarely, can be spontaneous. Several reports have been published on the association of arachnoid cysts with subdural hygroma and subdural hematoma after minor head injuries.7,8,16,20
Arachnoid cysts may cause cognitive disorders and deficits of any aspect of psychologic system.18
Even a trivial trauma can cause rupture of the cyst as seen in the presented case, where a simple falling down while playing resulted in the formation of hygroma.
The indication for surgery and the mode of surgical treatment are still a matter of debate. Different types of surgical approaches can be performed. Cyst fenestration, stereotactic punction, endoscopic cyst fenestration, cystoperitoneal shunt, cyst marsupialisation into the subarachnoid space and complete or partial resection of the cyst wall are the main options.19
Although the risk of hemorrhage of arachnoid cyst is very low but when the hemorrhage occurs it is treated by hematoma evacuation in most cases, but sometimes there is a need for fenestration of the cyst into basal cisterns by endoscopy, microsurgical or cystoperitoneal shunt.20
In our case, patient age, minority of trauma and symptomatology were similar to what is reported in literature, but formation of subdural hygroma in both sides of the brain where falx cerebri acts as a barrier cannot be explained and this is the interesting point in our report which mandates specific attention to this quaint case.
In patients with arachnoid cyst it is important to keep in mind that a trivial event can produce a significant intracranial complication, in both sides of the brain.
None.
None.

©2016 Motaghedifard, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.