Journal of
eISSN: 2574-9943


Case Report Volume 3 Issue 1
1Department of Dermatology, University Hospital Hassan II Fez, Morocco
2Department of Traumatology B4, University Hospital Hassan II Fez, Morocco
Correspondence: Kaoutar Laamari, Hassan II Universitary Hospitals, Department of Dermatology, F, Tel 0021 2673 1534 35
Received: December 26, 2018 | Published: January 11, 2019
Citation: Laamari K, El Marfi A, Rasso A, et al. An unusual localization of Shwannoma. J Dermat Cosmetol. 2019;3(1):1-2. DOI: 10.15406/jdc.2019.03.00104
Benign schwannomas are the most common nerve tumors. These tumors occur with predilection in the adult of 20 to 50 years, and always indifferently the man and the woman. The time of appearance of the first signs is usually long. Magnetic resonance imaging can guide the diagnosis, but it is histology that confirms it. The treatment is essentially based on surgical enucleation. Evolution is generally favorable. We report a rare case of schwanoma developed on the anterior side of the leg.
Keywords: shwannoma, leg, young patient, surgical enucleation
Primary tumors of the peripheral nerves account for 1 to 2% of soft tissue tumors. Benign schwannomas and neurofibromas should be distinguished from malignant tumors that usually occur during Recklinghausen disease.1 We report a case of benign solitary schwannoma developed in the leg and mimicking a centrofollicular b-lymphoma in a 34-year-old patient.
A 35-year-old man presented with a solitary nodule on his leg. The lesion had first appeared 3 years earlier as a small skin nodule. The cutaneous lesion was erythematous, well demarcated and measured 3 cm in diameter (Figure 1). The patient had no other abnormalities and no evidence of neurofibromatosis such as cafe´-au-lait spots or cutaneous neurofibroma. Physical examination did not reveal any enlargement of regional lymph nodes.
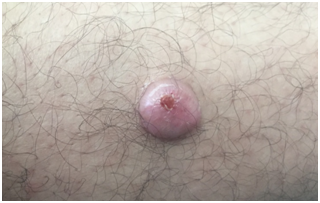
Figure 1 Well-defined nodule, roughly rounded, about 2cm long axes, located at the anterior side of the leg.
The patient underwent surgical excision. Histological examination showed a subatrophic polypoid epidermal coating with fusiform cells arranged in wavy bays. They are provided with regular elongate ovoid nuclei arranged in places in blanks of palisades with rolls of nodules in places (Figure 2).The patient benefited from an excision with good evolution without recurrence after one year.
Benign schwannomas; formerly known as neuromas, are the most common nerve tumors.2 They develop at the expense of schwann cells, forming a macroscopically smooth, rounded, yellowish and encapsulated proliferation.2,3 They are easily cleavable from the nervous beams which they repress to invade them; thus allowing a complete enucleation of the tumor. The malignant transformation is exceptional or even discussed, it would occur mainly in the context of a Recklinghausen disease.4 Tumeur primitive’s des nerfs périphériques Tumeur primitive’s des nerfs périphériques Tumeur primitive’s des nerfs périphériques Tumeur primitive’s des nerfs périphériques. These tumors occur with predilection in the adult of 20 to 50 years, and always indifferently the man and the woman. They preferentially localize to the anterior surface of the upper limbs, typically at the level of the large nervous trunks.5 The lower extremities are rarely the seat of benign schwannomas and pose more the problem of diagnosis.6 In this localization they concern both the large nervous trunks and the superficial sensory nerves. It is necessary to know how to evoke the diagnosis in front of a pain or paresthesia of a lower limb without obvious clinical abnormality. Generally, it's a solitary tumor. However, multiple localizations may be part of a Reckling Haussen disease.
MRI can guide the diagnosis by objectifying an aspect in favor of schwannoma. It can show in T1 a signal of the same intensity or slightly higher than the muscle, in T2 a hyperintense signal sometimes a "target image" with a hyperintense peripheral halo and a hypo-intense center.7 The confirmation of the diagnosis remains histological.8‒11 The optimal treatment is surgical excision12,13 since it is an easily extirpable tumor. After complete excision, there is no recurrence. The malignant degeneration of schwannoma is controversial. No case of malignant degeneration has been described. In our case, the excision was complete without any local recurrence.
Benign schwannoma located at the level of the lower limbs is rare and pose a real problem of diagnosis. Histology as well as imaging is tools that allow the diagnosis of this entity and the surgical exeresis remains the best treatment. It should always be evoked in case of a young patient who has a painful nodule or subcutaneous mass.
None.
Authors declare that there is no conflict on interest.

©2019 Laamari, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.
 May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.
May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.