Journal of
eISSN: 2373-6410


Case Report Volume 10 Issue 6
1 Professor of javeriana University cali, Colombia
2 Internal medicine physician at Valle University Hospital, Colombia
3 Familiar medicine postgraduate student of javeriana University cali, Colombia
Correspondence: Carlos Andrés Clavijo Prado MD MsC, Neurologist Medical director of pacific neurological institute
Received: November 20, 2020 | Published: December 7, 2020
Citation: Clavijo CAP, Franco KMM, Gallego AC. Symptomatic seizure and covid-19: A case report. J Neurol Stroke. 2020;10(6):206-208. DOI: 10.15406/jnsk.2020.10.00440
acute symptomatic seizures, COVID-19, epilepsy, SARS-CoV-2, seizure, neurology manifestation
Neurotropic and neuroinvasive capabilities of coronaviruses have been detected described in humans since December 2019 when it was first diagnosed, and then declared as a global emergency by the world health organization (WHO) later in March 2020.1 Neurological problems found in patients with coronavirus infection include: new onset of symptomatic seizures such as febrile seizures, loss of consciousness, encephalomyelitis, and encephalitis among others. Coronavirus disease (COVID-19) is caused by SARS-CoV2. In severe cases, patients may develop severe pneumonia, acute respiratory distress syndrome, and acute cardiac injury. While seizures and status epilepticus have not been widely reported in the past seven months since the onset of the COVID-19 pandemic, patients with the disease may experience hypoxia, multiorgan failure, and severe metabolic and electrolyte disarrangements; hence, it is plausible to expect clinical or subclinical acute symptomatic seizures2 as found in patients where a structural, metabolic and infectious cause was ruled out, finally finding a heart rhythm disorder with no other associated finding.
A previously healthy 18-year-old man with 2 weeks of hyposmia, global pulsating headache of medium to severe intensity, dry cough, hyaline rhinorrhea, who presented a daytime seizure 15 days after symptoms onset, characterized by eye opening, ocular supraduction, generalized axial symmetric tonic posture of 40 seconds duration, associated with marked diaphoresis and palpitations, with a new episode of the same characteristics witnessed by an internist on duty who controlled the seizure with 5 mg of midazolam, he was seizure free until today, on valproic acid 1000 mg/day for 2 months, without any requirement of mechanical ventilation or any other intervention for seizure. His oxygen saturation was 87% at admission time improving with oxygen per cannula at 2lt / min, achieving 98% and his body temperature was 37°C.
Ahead computed tomography (CT) was normal, a contrasted brain magnetic resonance was performed did not show infectious or vascular processes, a chest CT was scanned to rule out COVID-19, showing peripheral ground glass-like opacity in left dorsal lung (Figure 1). The laboratory analysis revealed a white blood cell count 7,630 per microliter lymphocyte percentage of 20 %, platelet count of 168.000 per microliter, C-reative protein of 3.5mg/L D- dimer of 100 ng/ml and INR of 1.25, cerebrospinal fluid of transparent appearance, cellularity 0.0 LDH 54, proteins 25 mg / dl, glucose 47 mg / dl, negative culture and negative viral panel, it was not possible to perform a SARS-COV-2 PCR test because of unavailability in the hospital. He had no previous contact with any positive patient for SARS-CoV 2 however, considering the hyposmia and the findings in the chest CT scan thus a real-time polymerase chain reaction assay (RT-PCR) was performed, which showed positive results for SARS-CoV-2, treatment was started on hydroxychloroquine (600 mg/day) and Lopinavir/ritonavir 400mg/100mg PO q12hr for 4 days. After the treatment started, the patient's clinical condition improved, a new test for SARS-COV2 was performed twice, being negative, so he was discharged on day 15 with an EEG that did not show epileptogenic alterations or periodic patterns but it could be perceived in the electrocardiogram lead an irregular R-R interval and a significant increase in heart rate during hyperventilation, reproducing presyncope dysautonomic symptoms (Figure 2A & 2B).

Figure 1 Radiological findings. A chest CT scan on admission showing the peripheral ground glass-like opacity in Right dorsal lung.
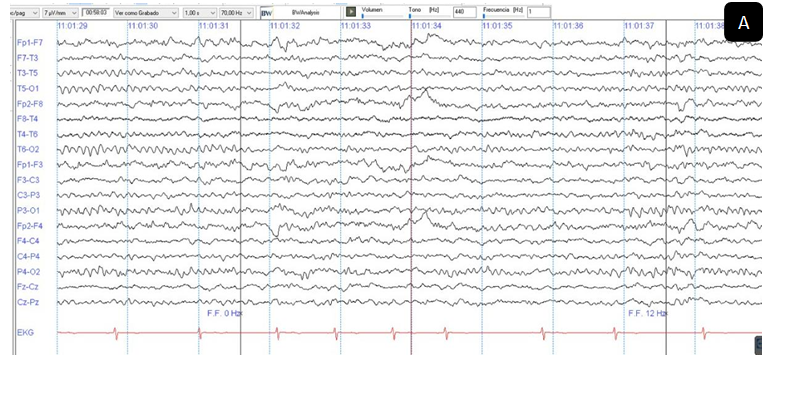
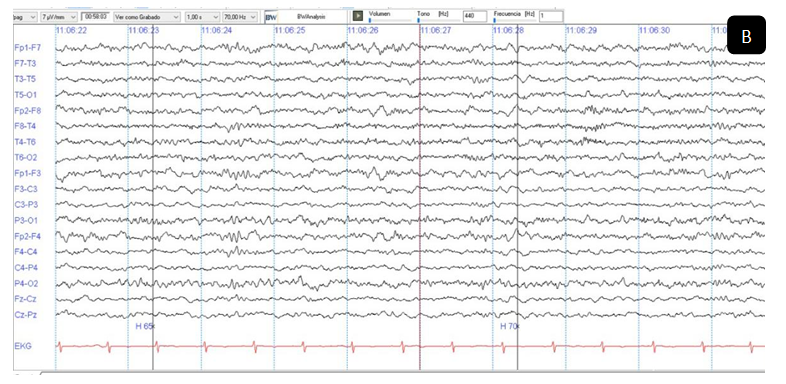
Figure 2 Electroencephalographic and electrocardiographic findings. LFF 1Hz and HFF 70Hz A. During photo stimulation at 12 Hz photo driving response is seen, the ECG showed irregular R-R interval; B. During hyperventilation, he presented tachycardia and went from 56 beats per minute to 90 beats per minute, presenting dysautonomic symptoms.
Neurological complications have been described for approximately 6 months with new findings as more is known about the disease, delving into vasculitic complications, encephalitis, hyposmia, but little about seizures or status epilepticus in the context of the disease.
After a few months, an attempt has been made to establish the probable etiologies and structural alterations have been defined, encephalitis and vascular causes being of low frequency occurrence. Patients with COVID 19 may experience hypoxia, multiple organ failure, severe metabolic and electrolyte alterations, or cardiac involvement, variables that could explain the clinical or subclinical manifestation of symptomatic seizures, as happened with this patient who despite not having a complicated infection, presented dysautonomic symptoms which could explain a probability to convulsive syncope.3,4
Another key finding to keep in mind is that medications used in the treatment of COVID-19 can present a high risk of potential interactions with antiepileptic drugs, given the tendency of the latter to interact with other drugs due to their capacity to induce or inhibit the metabolism ,1 therefore, it is vital to check the interactions on a real-time basis to add or adjust the treatment with an antiepileptic such as levetiracetam, considering that this medication does not present hepatic interactions. On the other hand, the incidence of seizures as well as their causes and severity are uncertain, therefore, future epidemiological and research studies should be carried out to clarify doubts of our current knowledge.
Finally, it is important to carry out an adequate analysis of the patients’ biological variables related to symptomatic seizures because in some particular cases this infection does not necessarily target the central nervous system but that can trigger a seizure such as dysautonomias, arrhythmias, hypoxia, hypoglycemia, fever or hydroelectrolyte disorders, so before starting antiepileptics, different possibilities should be ruled out to avoid further damage.
None.
The authors declare no conflicts of interest.

©2020 Clavijo, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.