eISSN: 2373-6372


Review Article Special Issue Pancreatic Disorders
1Medical Oncology Department, Northern Cancer Institute, Australia
100Radiation Oncology Department, Royal North Shore Hospital, Australia
2University of Sydney, Australia
3Medical Oncology Department, Royal North Shore Hospital, Australia
4Hepatobiliary Surgery Department, Royal North Shore Hospital, Australia
5NHMRC Clinical Trial Centre, Australia
6Palliative Care Department, Royal North Shore Hospital, Australia
7Radiology Department, Royal North Shore Hospital, Australia
8Nuclear Medicine Department, Royal North Shore Hospital, Australia
9Pathology Department, Royal North Shore Hospital, Australia
Correspondence: Malinda Itchins, Northern Cancer Institute and University of Sydney, 38 Pacific Highway, St Leonards, New South Wales, Australia, 2065,, Tel 61409589488, Fax +61 02 80374111
Received: February 16, 2017 | Published: September 19, 2018
Citation: Itchins M, Arena J, Pavlakis N, et al. Pattern of care and survival of pancreatic ductal adenocarcinoma in a multi-disciplinary high-volume centre. Gastroenterol Hepatol Open Access.2018;9(5):185-189. DOI: 10.15406/ghoa.2018.09.00323
Introduction: Pancreas cancer remains a deadly disease. High volume specialist centres offer the potential of optimising patient outcomes and minimising the disparities in treatment delivered and survival outcomes.
Methods: A retrospective cohort analysis of all patients managed with pancreatic ductal adenocarcinoma (PDAC) across public and private campus hospitals in Northern Sydney, Australia was performed between 2010-2016. Data were collected and presented on baseline demographics, diagnostic and treatment pathways, toxicity and survival.
Results: Between January 1 2010 and April 1 2016, 442 patients were diagnosed. Median overall survival (mOS) for patients who received neoadjuvant treatment (NA) was 25.9mo (95% CI 21.1, 43.0), not statistically significantly different to those in the upfront operable group 26.9mo(95% CI 19.7,32.7) HR=0.90, (95% CI 0.61,1.32; log ranked p value=0.58). Within the NA arm, in those treated with neoadjuvant chemotherapy (NAC) alone the mOS was 25.9 mo (20.8, upper limit not reached (NR)). In the NAC/RT group mOS was 29.0 mo (17.3, NR); log ranked p-value=0.99. Median OS in all metastatic patients at diagnosis was 7.66 mo(95% CI 6.22,8.78 mo). In the sub-group who received palliative chemotherapy, mOS was 9.61 mo (95% CI 7.83- 11.58 mo).
Conclusion: This real-world report on the pattern of care and experience in the management of PDAC in a high-throughput centre demonstrates superior outcomes to those reported from national registries.
Keywords: pancreatic, adenocarcinoma, survival, multidisciplinary, high volume, surgery, neoadjuvant, adjuvant, palliative, metastatic
PDAC, pancreatic ductal adenocarcinoma; NA, neoadjuvant; NAC, neoadjuvant chemotherapy; NART, neoadjuvant radiotherapy; UO, upfront operable; Os, overall survival; MDT, multi-disciplinary team; MDM, multi-disciplinary team meeting; CNC, clinical nurse care coordinator; PEI, pancreatic enzyme insufficiency; RECIST, response evaluation criteria in solid tumours; mo- months; LHD, local health district; HR, hazard ratio; CI, confidence interval; Mfolfirinox, modified fluorouracil, irinotecan, Oxaliplatin; folfox, fluorouracil, Oxaliplatin; folfiri, fluorouracil, Irinotecan; TTR, time to relapse; Gy, gray
Pancreatic ductal adenocarcinoma (PDAC) is the 14th most common cause of cancer in developed regions, but the fifth leading cause of cancer death.1 In Australia, the one-year survival is 20%, 5-year survival 6%, in keeping with the global life expectancy from this disease.2,3 Unfortunately, over 80% of patients present at an unresectable stage, thus PDAC is a systemic disease from the time of diagnosis.4
Surgical resection offers greatest potential for long-term survival and cure; however, an Australian population based study found resection was attempted in only 20% of cases and completed in 15%. Furthermore, adjuvant chemotherapy was then only completed in 43% of patients, demonstrating an underutilization of cancer-directed therapies.5
Thus, in Australia, fewer patients receive recommended treatments than is desirable and there is significant disparity in the care delivered between cancer treatment centres.5,6 Patient socioeconomic factors and treatment of patients in small volume, non-specialised centres appear to at least partly explain these findings.6-9
Higher quality of care has demonstrated improved survival, particularly in operative patients which may be contributed to by access to tumour specific specialists and care in high case volume centres.10,11 Implementation of interventions which ensure that all patients are managed by such centres would improve the disparities which currently exist. Less than one-third of pancreas cancer patients in Australia are referred to a multi-disciplinary pancreas cancer specialist team (MDT).12
Neoadjuvant therapy (NA) is emerging with the potential to become the new standard of care in a select group of upfront operable (UO) and ‘borderline’ resectable population to improve survival outcomes.13,14 This modality cannot currently be offered without an MDT consensus.
We report on the pattern of multi-modality care delivered in a high-volume tertiary referral centre and the impact on disease outcomes including survival.
Patients
Approval for the conduct of this study was obtained from the Northern Sydney Local Health District Human Research Ethics Committee.
A retrospective cohort analysis of all patients managed with PDAC across public and private campus hospitals in Northern Sydney, Australia was performed between 2010-2016.
Patients were identified by searching electronic medical records. Patients reviewed as a second opinion who continued treatment with their external specialist were not included.
All patients were discussed in a multidisciplinary meeting (MDM) by a panel of pancreas cancer specialists directing their treatment pathway. Teleconference facilities were available for external specialists to join the MDM from remote locations.
Patient Pathway
Patients underwent evaluation including clinical history, physical examination, complete laboratory assessment and preoperative imaging with triple-phase CT scans. In July 2016, radiology reporting introduced a standardized template to define radiological stage and resectability.
Histopathological/cytological confirmation of PDAC was required in all patients unless deemed infeasible.
Investigations were coordinated by the pancreas cancer clinical nurse care coordinator, introduced in 2012, who was referred all new diagnoses and followed the patient throughout their treatment pathway from diagnosis.
In the operative work-up, laparoscopy and peritoneal washings were recommended. Abdominal MRI and/or PET scans were performed as required by the MDM.15
Patients deemed potentially resectable were considered for NA therapy if there was: any degree of local vessel involvement on imaging (stage 1b-3); if they were enrolled on a clinical trial evaluating NA therapy without vessel involvement;16 based on patient factors such as age, comorbidities or preference. Only borderline resectable patients were deemed appropriate for NA radiotherapy (RT).
All patients were considered for a clinical trial if available.
Neoadjuvant, peri-operative, adjuvant and metastatic treatment could have been performed by specialist teams practicing outside of the referral centre, however ongoing MDM review continued in collaboration.
Patients proceeding to resection received mandatory perioperative cardiothoracic assessment. Additionally, they were referred to a dietician or the pancreatic enzyme deficiency clinic (PEI).
Two surgeons performed all operations (JS, AM).
The pathological characteristics at resection were assessed using a standardized structured surgical pathology report17 and an R0 margin was defined as being > 1mm clear of tumour (R0>1mm).
All operable patients were considered for 6 months of chemotherapy pre, peri or post operatively and if deemed appropriate, 25-30 fractions of NA RT with radio sensitising fluorouracil based chemotherapy after completion of ‘induction’ neoadjuvant chemotherapy (NAC). The chemotherapy regimen utilised was at the discretion of the treating physician based on patient assessment of tolerability. Patients were reviewed with each cycle of chemotherapy by the oncologist or if there was excessive toxicity.
Metastatic patients were assessed at appropriate time points for alterations in systemic chemotherapy, use of palliative radiotherapy to symptomatic sites, palliative nerve blocks or liver directed therapy at the physicians’ discretion, guided by MDM recommendations.
In the palliative setting, generally, the standard of care first-line in those assessed as very good performance status was modified FOLFIRINOX, in good performance status gemcitabine and nab-paclitaxel, borderline performance status single agent gemcitabine and poor performance status best supportive care. In subsequent lines of therapy FOLFOX, FOLFIRI, liposomal irinote can, capecitabine were all considered and prescribed.
Review from the surgeon continued despite incurable status and in carefully selected patients with long-term disease stability, metastasectomy was performed.
Palliative care referral was offered to operative patients with greater requirement for symptom management and to all metastatic patients.
Patients who travelled from remote and rural areas for treatment covered their own personal expenses to do so, supported by government sponsored travel schemes.
Patient support group information sessions have been introduced.
Statistical analyses
Time to death and relapse were calculated using the time between the date of diagnosis and the date of death or last known contact. Survival data were presented using the Kaplan Meier method. Median survival times for each subgroup were reported with 95% confidence intervals; and with log-rank statistics used to compare the curves.
A Cox proportional hazards model was used to compare survivals of the UO and NA cohorts.
Length of stay in hospital was described using median and (interquartile range) IQR and the comparison between UO and NA was done using a Mann-U –Whitney test.
All analyses were performed in Stata version 14.0 (2015, StataCorp, Texas, USA).
Patients
Between January 1 2010 and April 1 2016, 442 patients were diagnosed with PDAC in our institutions.
Median age of patients was 69 years (range-38-94 years) and 233 (43%) were male. Performance status at diagnosis was not consistently recorded.
There was an increase in the number of patients diagnosed annually with 34 (8%) in 2010 and 86 (19%) in 2014. The proportion of patients receiving NA also increased; one patient (4%) in 2010, compared with 39 (40%) in 2015.
Two-hundred and twelve (48%) were deemed potentially operable at diagnosis with 230 (52%) inoperable. One hundred and thirty-three patients (30%) received curative intent UO. Eighty-seven patients (20%) were treated with NA, 85 (19%) with NAC and 24 (5%) with NA RT (Figure 1). Seventy-nine percent (n=69) NA patients proceeded to resection.
One-hundred and eighty-three patients (41%) were managed in the public sector and 261 (59%) in private centres.
Two-hundred and thirty-two (52%) resided within the local health district (LHD) and 210 (48%) outside.
Twenty patients (5%) were managed on a clinical trial including across neoadjuvant, adjuvant and metastatic settings.
From 2013 to 2016 there were 86 patients diagnosed who lived within the LHD and 62 (72%) of these cases received specialist palliative care input.
Treatment
In the operative cohort the median duration of NAC was 3 months (mo) (range: 1-6 mo). The majority of patients received NA gemcitabine/nab-paclitaxel, n=50 (59%); and adjuvant gemcitabine, n=31 (67%). Modified FOLFIRINOX was the third commonest protocol prescribed (Table 1). Median duration of adjuvant chemotherapy after NA was 3 mo (range 1-6). Patients completed 6 mo total perioperative chemotherapy.18 Of the NA patients intended to receive adjuvant chemotherapy, 46 (85%) initiated it with only 2 (6%) not completing the course.
In the NA RT cohort the median dose received was 50 Gy (range: 45-54), in 25 fractions (range: 25-30), over 40 days (range: 30-47).
In the UO group, 115 patients (88%) commenced six months of adjuvant chemotherapy and 98 (92%) received adjuvant gemcitabine with the remainder receiving gemcitabine and nab-paclitaxel via a clinical trial.19 From mid-2016, capecitabine has been combined with gemcitabine in the adjuvant phase.20
In the metastatic setting, an accurate account of chemotherapy regimens is not presented in this report. One-hundred and twenty-three patients (53%) received at least one cycle of palliative chemotherapy, 11% did not. In 81 patients (35%) their treatment status was not available.
Chemotherapy |
Neoadjuvant n=85 |
Adjuvant n=46 |
Gemcitabine/Nab-paclitaxel |
50(59%) |
7(15%) |
Gemcitabine |
15(18%) |
31(67%) |
FOLFIRINOX |
14(16%) |
2(4%) |
Gemcitabine/Capecitabine |
0 |
1(2%) |
Unknown |
6(7%) |
7(15%) |
Table 1 Chemotherapy schedules given in the neoadjuvant and adjuvant settings in those managed with perioperative treatment.
Efficacy
Median follow up at data cut-off (December 18 2016) was 3.2 years. At two years 32.6% of the entire cohort were alive; 53.7% of all patients deemed operable at diagnosis and 55.9% of those managed with NA.
In the operative cohort median overall survival (mOS) for patients who received NA was 25.9 mo (95% CI 21.1,43.0), not statistically significantly different to those in the UO group 26.9 mo (95% CI 19.7,32.7) HR=0.90, (95% CI 0.61,1.32); log-ranked p-value= 0.58) (Figure 2A).
Median OS in metastatic patients at diagnosis was 7.66 mo (95% CI 6.22-8.78 mo). In the sub-group who received palliative chemotherapy, mOS was 9.61 mo (95% CI 7.83,11.58 mo) (Figure 2B).
Within the NA arm, in those treated with NAC the mOS was 25.9 mo (20.8, upper limit not reached (NR)). In the NAC/RT group mOS was 29.0 mo (17.3, NR); log ranked p value=0.99.
Survival by radiological stage at diagnosis in the NA group showed no difference with stage 1 having a mOS 22.3mo (16.3, NR); stage 2 mOS 25.9mo (17.3, NR) and stage 3+ mOS 30.2mo (9.0, NR); log ranked p-value=0.77.15
In the NAC alone group, mOS in those treated with gemcitabine/nab-paclitaxel (n=46) was 23.0 mo (18.5, NR); gemcitabine (n=14) mOS was 29.0 mo (9.1, NR) and in mFOLFIRINOX mOS was 25.9 mo (11.8, NR); log-ranked p-value 0.92. Three patients had a complete pathological response following NA treatment.
Fifty-two NA patients (75%) had an R0 resection including 44 (88%) NAC patients and 8 NA RT (62%). The mOS for NA patients with an R0 resection was 29.5 mo (25.26, NR); and in those with an R1 resection mOS was 20.8 mo (12.8, 43.0); log-ranked p-value p=0.15. Sixty-eight patients (51%) in the UO were R0 at resection with mOS of 30.7 mo (21.5, 47.7) versus the 54 (41%) UO R1 group, mOS was 19.74 mo (14.6, 26.2); log-ranked p-value=0.77, the R stage for 11 patients was unknown. In the NA/RT resected R0 group, mOS was not reached at data-cut and for the NA/RT R1 resected (n=5) mOS was 43.0 mo (14.0, NR); log-ranked p-value=0.15.
For the 22 (28%) NA patients with an N0 nodal status at operation, mOS was 69.2 mo (21.2, NR). In the 44 (68%) NA with N1, mOS was 29.0 mo (17.2, 43.0); log-ranked p-value=0.09. For UO, 107 (82%) were N1, and the mOS was 21.5 mo (16.8, 29.2). In the 24 (18%) UO who were N0, median OS had not yet been reached; log-ranked p-value=0.02.
Figure 2Kaplan-Meier plot of overall survival in
A) All neoadjuvant and upfront operable cohorts.
B) Inoperable cohort.
The mOS in all-comers living within the LHD with survival data available (n=224) was 13.96 mo and outside (n=205) 17.14mo (HR 1.23; 95% CI 1.008-1.50; p=0.21). In the operative cohort patients living within the LHD (n=89) mOS was 27.27 mo versus outside (n=118) mOS 26.87 mo (HR 0.99; 95% CI 0.67-1.44; p=0.80).
Thirty-five (40%) NA relapsed and all had palliative chemotherapy. Sixty-eight (52%) upfront operable relapsed, 51 (68%) received palliative chemotherapy, five did not (7%) and in the remainder it was unknown.
Median time to Relapse (TTR) from the date of surgery for all NA patients was 21.44 mo (15.7,43.0); NAC was 18.3 mo (15.1,32.7) and NAC/RT was 43.0 mo (7.1, NR). UO mTTR was 15.9 mo (12.7,23.4). The log ranked p-value for NA versus UO was p=0.99 (Figure 3).
Seventy (81%) NA had distant disease at diagnosis of relapse while 19 patients (28%) had local disease only and two patients had distant and local relapse. Two patients with RT relapsed locally. Eighty-three (63%) UO had distant disease at relapse; 51 (39%) local (3 patients local and distant).
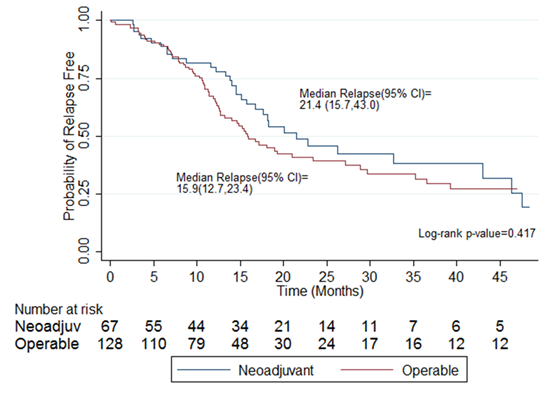
Figure 3 Kaplan-Meier plot of median time to disease relapse from operation in neoadjuvant and upfront operative cohorts.
Safety
Chemotherapy toxicity was as expected for the published protocols.
Radiotherapy caused no grade 4 or 5 toxicities, and was generally well tolerated with only one case of grade 3 diarrhoea. The most common toxicity was grade 1 lethargy in twelve patients (50%) and nausea in 11 (46%).
No NA patient died within 90 days. Two UO patients died within 30 days, one between 30-90 days.
Median length of post-operative hospital stay was 14 days in the UO cohort (11,19) and 13 days in the NA cohort (10,17); log-ranked p value= 0.15.
We present a real world tertiary-referral centre approach to the management of pancreas cancer and consequent outcomes in consecutive patients. These data support the hypothesis that involvement of a high-volume centre in patient care improves survival.
Our treatment paradigm is evolving with the updated literature and the results appear to be superior to trial reports across disease stages involving highly selected populations.13,19,21,22
Patients are increasingly managed with NA, particularly those with borderline and locally advanced disease. Despite the higher stage of disease at diagnosis, the NA group performed as well as the UO.
In our experience, with close multi-disciplinary support and expertise patients undergo timely and comprehensive diagnostic work up, with less toxicity from therapy managed pre-emptively and proactively and fewer complications. In particular perioperative mortality in this cohort was very low.
Our centre does not have an operational prospective patient database which is imperative in moving forward to provide a comprehensive report on patient care with accuracy, particularly with reference to quality of life information.
Almost half of the patients in this group travelled from outside of the LHD. Although selection bias is expected, these patients achieved comparable outcomes to those within. Furthermore, over half of all patients were managed in the private sector.
Given the retrospective nature of this study it is subject to reporting bias. An effort was made to capture all palliative patients; this patient group may however be underrepresented. The involvement of palliative care in a majority of cases in the sub-group of patients reviewed was encouraging.
Disappointingly only 5% of patients were enrolled in a clinical trial highlighting the lack of emerging clinical research opportunities for patients over the last five years. Despite multi-modal therapy being delivered, survival in this aggressive disease remains very disappointing. Furthering effective drug development is crucial as is understanding patient selection for optimal treatment pathways.
We aspire to reach future in which we measure survival outcomes in PDAC in years not months.
This report on the pattern of care and experience in the management of PDAC in a high-throughput centre demonstrates the impact of such a model in achieving comparable if not superior patient outcomes to the enriched clinical trial data to date.
None.
Author declares that there is no conflict of interest.

©2018 Itchins, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.