eISSN: 2379-6367


Review Article Volume 7 Issue 5
Departamento de Farmacologia, Farmacognosia y Botanica, Facultad de Farmacia, Universidad Complutense, Spain
Correspondence: Sagrario Martin-Aragon, PhD. Departamento de Farmacologia, Farmacognosia y Botanica, Facultad de Farmacia, Universidad Complutense, Plaza Ramon y Cajal s/n, 28040 Madrid, Spain, Tel +34 91 394 17 67
Received: August 02, 2019 | Published: September 24, 2019
Citation: Gonzalez MP, Benedi J, Bermejo-Bescos P, et al. Plants with evidence-based therapeutic effects against neurodegenerative diseases. Pharm Pharmacol Int J. 2019; 7(5): 221-227. DOI: 10.15406/ppij.2019.07.00255
Neurodegenerative diseases are a group of illnesses, which affect both central and peripheral nervous system inducing physiological dysfunctions related with loss of movements and mental integrity, among others. In general, these diseases are incurable and only few drugs may alleviate the symptomatology or prolong the survival of patients. In this setting, medicinal plants might constitute adjuvant therapies with conventional pharmacotherapeutics in order to reduce or remedy the neurodegenerative illness. The aim of this review is to present the neuropharmacological activity of some phytochemicals from noteworthy medicinal plants that have been used in traditional medicine. Particularly, we will focus on medicinal plants with evidence‐based therapeutic effects against neurodegenerative diseases.
Crucial among these plants is Daphne Genkwa, with its active components genkwanine N and yuanhuacin, which are both able to activate the transcriptional function of the Nurr1 receptor. Another plant to be highlighted is Jatropha multifida containing apocynin, a selective inhibitor of the phagocyte NADPH oxidase. Galanthus nivalis is a remarkable plant for its content in galantamine, an inhibitor of the acetylcholinesterase enzyme and an inhibitor of the nicotinic acetylcholine receptor (nAChR) with a mechanism consistent with open‐channel pore blockade. Galantamine is currently used in Alzheimer’s disease and dementias. Ginkgo biloba is known for its leaves as a natural source of flavonoids and polyphenolic compounds and it is used in the treatment of progressive neurodegenerative disorders such as Alzheimer’s disease. Glycine max or soybeans contain isoflavones such as genistein, daidzein and glycitein. Among these phytochemicals, genistein should be underlined for its potential to alleviate neurological symptoms present in most lysosomal storage diseases by decreasing the biosynthesis of accumulating substrates.
Keywords: genkwanine N, galantamine, genistein, Ginkgo biloba, neurodegenerative diseases
Aβ, β-amyloid; AChE, acetylcholinesterase enzyme; AD, Alzheimer’s disease; ALS, amyotrophic lateral sclerosis; AMPA, α-Amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid; ApoE, human Apolipoprotein-E; APP, amyloid precursor protein; BH4, tetrahydrobiopterin; CaMKII, Ca2+- and calmodulin-dependent protein kinase II; CREB, cyclic adenosine monophosphate response element-binding protein; GAG, glycosaminoglycans; EGb 761, a standardized Ginkgo biloba extract; GCH1, GTP cyclohydrolase I; GSK-3, glycogen synthase kinase-3; HD, Huntington’s disease; hIAPP, human islet amyloid polypeptide; H2O2, hydrogen peroxide; INF-γ, interferon-γ; IL-1, interleukin-1; IL-6, interleukin-6; IL-β, interleukin-β; JNK, c-Jun N-terminal kinase; LPS, lipopolysaccharide; MPO, myeloperoxidase; MPTP, 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine; nAChR, nicotinic acetylcholine receptor; NFκB, nuclear factor kappa B; NMDA, N-methyl-D-aspartate; NOX2, NADPH oxidase enzyme; NR4A2, nuclear receptor subfamily 4 group A member 2; Nurr1, nuclear receptor related 1 protein; polyQ, proteins containing glutamine repeats; ROS, reactive oxygen species; SOD1, superoxide dismutase 1; TBP, TATA box-binding protein; TFEB, transcription factor EB; TH, tyrosine hydroxylase; TLR4, toll-like receptor 4; TNF-β, tumor necrosis factorα
Phytochemicals are chemical compounds produced by plants, generally to help them thrive or defend from competitors, predators or pathogens. Numerous phytochemicals may have curative properties because herbs and plants have been used to cure all sorts of illnesses for centuries. To establish an efficient therapy to protect or treat a disease it is necessary to know both the dysfunction of the disease and the characteristics of the active agent. To date, most drugs used are synthesized compounds whose structures are based on active components from plants. Although the knowledge of neurology dates back to prehistoric times, the real advances in this discipline occurred in the Renaissance and its knowledge has been widely advanced until now.
Neurodegeneration is the progressive loss of structures and functions and eventually the death of neurons. To date, neurodegenerative diseases are incurable and share numerous similarities. There is a great parallelism between different neurodegenerative dysfunctions including atypical protein assemblies (Alzheimer, Corea, Parkinson, prion diseases) as well as cellular death (Parkinson, Corea)1,2 and nervous demyelination (Multiple sclerosis, Amyotrophic lateral sclerosis). The discovery of these similarities offers a great help for therapeutic advances that might prevent or reduce the progress or disturbances of these diseases. Taken all this into account we must consider that the neurodegenerative diseases share similar dysfunctions as cellular death, inflammation and oxidative stress, resulting from specific mechanisms that might be target by certain phytochemicals. Moreover, the increasing life expectancy and the rising in the incidence of these disorders should urge the need for therapies to delay its progression. As for the rates of prevalence, it is intriguing that in the case of dementia, there is a growing consistency of reports indicating a potential decrease3,4 not ascribed to better treatment. This effect is probably the result of changes in lifestyle, which includes chronic consumption of plants and/or plant-derived products containing phytochemicals with antioxidative, anti-amyloidogenic, anti-inflammatory and anti-apoptotic properties, among others.
Plants contain a great number of active components that may have an application in medicine although many of them have been synthetized by the pharmaceutical industry. In the developed countries, plant-derived drugs may be important, and, plant extracts and active principles prepared from plants are quite a lot representing a potential therapeutic interest.5 In the preset review, we aimed to outline the main molecular mechanisms responsible of the dysfunctions that occurred in the phenomena of neurodegeneration as well as the evidence-based mechanisms of action of particular phytochemical compounds in order to suggest and propose rational and consistent preventive therapies. We have not described separately the different active principles from a certain plant but the plants that may have some application in the therapy of neurodegenerative diseases due to its active constituents.
Daphne genkwa
Daphne genkwa is a plant species from the Thymelaeceae family and is one of the main herb used by the traditional Chinese medicine known as “yuan huä”. The flowers buds of this plant are use with diuretic, antitussive, expectorant and antitumor purposes. But, beside that a methanol extract of the roots of this plant activated the transcriptional function of Nurr1, an orphan nuclear receptor that is essential for the differentiation6‒10 and maintenance of dopaminergic neurons in the brain6 what may signify a therapeutic target for Parkinson’ and other neurodegenerative diseases. The active components isolated from Daphne genkwa have been identified as genkwainine N and yuanhuavin. Both compounds have shown to enhance the function of Nurr 1 and inhibit the neuronal death induced by 6-hydoxydopamine on SH-SY5Y cells and, in addition, they have proved a beneficial effect on the neuroinflammation mediated by lipopolysaccharide (LPS) in BV-2 microglial cell line.7 Nurr1 inhibits the expression of proinflammatory genes in microglia and astrocytes. The repression of inflammation by Nurr1 activation decreases the loss of dopaminergic neurons in vivo and in vitro models,10 signifying a protective mechanism in Parkinson’s disease.
It is known that the human NR4A2 gene encodes Nurr1 and, although its ligand is not well identified, it is known that Nurr1 protein is a member of the nuclear receptor family of the intracellular transcription factor, which plays a role in maintaining the dopaminergic system in the brain. This lies on the fact that Nurr1 abnormalities turn into damage of the function of dopaminergic system causing Parkinson’s disease and a wide range of inflammatory and neurological diseases, including rheumatoid arthritis, schizophrenia and manic depression. Nurr1 is expressed in developing and mature dopaminergic neurons and is required for both its survival and its complete differentiation.7,11 Nurr1 also enhances the transcription of tyrosine hydroxylase (TH), the limiting enzyme of dopamine biosynthesis as well as of the GTP cyclohydrolase I (GCH1), the first enzyme in the biosynthesis of tetrahydrobiopterin (BH4), which is an essential factor to TH activity.12,13
Genkwanine and yuanhuacin obtained from extracts of Daphne genkwa activate the nuclear receptor Nurr1. This receptor is bound to different regions (sequences) of DNA from the cell nucleus and may actuate as transcriptional activator or transcriptional repressor depending on the cellular context. As a transcriptional activator may induce different survival signals which maintain the survival and development of dopaminergic neurons. Nurr1 also may enhance the transcription of both tyrosine hydroxylase and GTP-cyclohydrolase I enzyme. Reduced Nurr1 expression might result in dysfunction and progression of degenerative changes of dopaminergic neurons. The availability of molecules capable of activating this receptor might provide a promising therapy for neurodegenerative diseases, mainly Parkinson’s disease. Due to the action of the active ingredients (genkwanine N and yuanhuacin of Daphne genkwa) on Nurr1 functions, one may suggest that this plant may exert neuroprotective, neurogenic or anti-inflammatory effects.
Jatropha multifida
Jatropha multifida is a plat species from the family Euphorbiaceae and is a shrub or treelet. The genus Jatropha comprises about 170 species of woody trees, shrubs, subshrubs or herbs. They are used in medicine to cure several diseases in Africa, Asia and Latin America. Plants extracts are reported for cytotoxicity, tumor-promoting, antimicrobial, antiprotozoal, anticoagulant, immunomodulating, anti-inflammatory, and antioxidant properties and acetylcholinesterase inhibitors.14‒16
All parts of this plant, but mainly the seeds, have strong purgative properties and are insect repellents. Jatropha multifida contains apocynin (4’-hydroxy-3’-methoxyacetophenone or acetovanillone), a selective inhibitor of the phagocyte NADPH oxidase (NOX2 enzyme) which produces reactive oxygen species (ROS) being a well know element in host defence. Besides, there is evidence for a regulatory role of NOX2 in adaptative immunity suggesting a role in autoimmune diseases.17 Regarding this point, there is sufficient evidence suggesting that inflammatory mediators have a significant influence on the pathogenesis of neurodegenerative diseases what may propose apocynin as a potential treatment of neurodegenerative diseases because microglia cells are the main resource of NOX2 in the brain. This enzyme, when activated, induces reduction of O2 to superoxide (O2-). Superoxide may kill bacteria and fungi by mechanisms that are not yet fully understood.18 It may also forms hydrogen peroxide spontaneously that undergoes further reactions to generate H2O2, other ROS formation that can be used to kill bacteria and fungi by the immune system and to inevitably drive cell death mediating neurodegenerative brain injury.
When this enzyme is inhibited by apocynin, ROS formation is prevented and then neurodegeneration does not occur. The mechanism by which apocynin induces its action is not well known. However, apocynin is a selective inhibitor of NADPH oxidase and therefore it may prevent the production of superoxide in human white blood cells or neutrophils without interfering with the defences of the immune system. This might be due to the fat that apocynin is not an inhibitor of the NADPH oxidase from immune system cells as it occurs in the case of the NADPH oxidase from vascular smooth muscle cells.19 Apocynin mechanism from experimental studies may be summarized as follows:
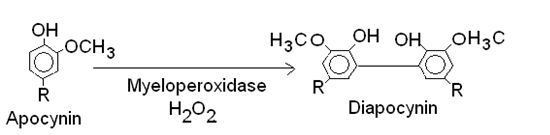
One important issue is that microglia cells not only express NOX2 but also secrete MPO after activation what might potentiate the apocynin action.
The pharmacological profile and low toxicity of apocynin might be considered for its use as a neuroprotective treatment. In this sense, some researchers have found that NOX2 inhibition promotes anti-inflammatory microglial activation during neuroinflammation.21 This may imply that suppression of NOX2 with apocynin might restore microglia healthy. Other authors have shown that apocynin decreases the production of IL-1, TNF-a and nitric oxide by microglia. However, although the exact inductor of microglia activation in neurodegenerative disease is still uncertain it could be of interest should be note that glutamate toxicity requires NOX2 activation and that this may be inhibited by apocynin.22 On the other hand, remarkable effects of apocynin have been observed in mouse models of neurodegenerative diseases such as amyotrophic lateral sclerosis (ALS) pathology whose motor neurons containing aggregates of superoxide dismutase 1 (SOD1) are hallmarks of ALS caused by mutations in the gene encoding SOD1. Harraz et al.,23 have observed that oral administration of apocynin in drinking water to mutated SOD1 mice prolonged animal survival and delayed motor defects. They also observed that ALS mice treated with apocynin significantly increased their average lifespan. However, although this study was promising, other studies performed with the same mutants indicated that apocynin has not this beneficial effects.24
Other authors have administered apocynin as a daily dose via drinking water to a transgenic mouse model of Alzheimer’s disease and observed a significant reduction of amyloid plaque size within cortex and hippocampus and a reduction of microglia content in cortex but not in hippocampus. However, this treatment could not imply any improvement in the tests of spatial memory.25 Apocynin may be extracted from different plants as Apocynum cannabinum and it has been identified as an active substance in the roots of Picrorhiza kurroa (Scrophulariaceae), a perennial plant from alpine Himalaya.
Galanthus nivalis
Galanthus nivalis is a plant species from the Amaryllidaceae family that contains galantamine, an isoquinoline alkaloid produced by the plant. It was first discovered in 1958 by the Bulgarian Chemist D. Paskov and it was firstly used in the poliomyelitis treatment and the neuropathic pain and as an anesthetic.26 Nowadays, galantamine is obtained from bulbs of Galanthus woronowi Losinsk and Galanthus alpines and by synthesis. Galantamine has a unique dual mode of action affecting the cholinergic system as a reversible inhibitor of the acetylcholinesterase (AChE) enzyme.27 In concentrations ranging from 10nM to 1μM, galantamine did not display direct modulatory effects at any receptor combination tested. At concentrations from 10μM and above, galantamine inhibits AChE activity through a mechanism consistent with open‐channel pore blockade at all receptor types.28 Galantamine may cross the blood-brain barrier making it a condition to be used for neurological diseases. Galantamine also prevents mitochondrial dysfunctions protecting mitochondrial membrane potential due to its antioxidative properties.29 Galantamine is currently used in Alzheimer’s and dementia diseases30 and its effectiveness has been confirmed in several clinical trials. In these patients, galantamine might achieve the efficiency of cholinergic system helping improving the cognitive function. Galantamine may also potentiate antioxidative activity31 and prevent memory extinction in guinea pig exposure to organophosphorus pesticides. Galantamine may improve the AMPA receptor-mediated signalling, which could be neuroprotective improving memory in schizophrenia. Combination of galantamine and memantine (an antagonist of NMDA glutamate receptor) improves cognition in schizophrenia.32 In addition, galantamine could improve cognitive and behavioural symptoms in Alzheimer’s disease and may have disease-modifying and neuroprotective properties. Moreover, galantamine could induce amyloid clearance33 mediated via stimulation of microglial nicotinic acetylcholine receptors.34
In the 1960 and 1970 the drug produced from Galanthus nivalis was commercialised under the name “Nivalin” being used in the Eastern European to treat polio and increase neurotransmission in the brain. However, this drug was more widely recognised in 1980 and used in the Alzheimer’s disease treatment in 1990s.
Ginkgo biloba
Ginkgo biloba is a unique species of tree in the world that belongs to the Ginkgoaceae family. It is native to China and it is named as “yin xing”. It is to Engelbert Kaempfer (1651-1716), a German scientist that the first description of the ginkgo and the name of the arboreal genus is due. Ginkgo biloba has been used in the traditional Chinese medicine and recently, it has begun to be used in the United States to treat physical and cognitive disorders related with age.35 Ginkgo biloba possesses a great variety of biological and pharmacological activities. The leaf extract of Ginkgo biloba (EGb761) has been used for years to treat memory deficits, including Alzheimer’s disease and dementia36 and Parkinson’s disease.37,38 Extracts of Ginkgo biloba leaves are a natural source of flavonoids and polyphenolic compounds that can stimulate the expression of genes related with antioxidant enzymes. The most benefits associated with the use of food rich in polyphenols include a reduced risk of coronary diseases and prevention of cancer and some neurodegenerative diseases.39‒41
Ginkgo biloba extract is obtained from green leaf and has several properties as phychoanaleptic against dementia. It contains two bioactive components, a glucoside flavonoide and a lactone from terpenes (trilactone), denominated ginkgolides and bilobalide.42 It contains ginkgolic acid A, B, and C with allergenic properties. It is believed that the therapeutic mechanism is due to its antioxidant and antiedema action. The EGb 761 extracts from leaf possess neuroprotective properties and have been used in the treatment of progressive neurodegenerative disorders in Alzheimer’s disease.43 It has also been shown that Ginkgo bioactive agents as ginkgolides and bilobalide exert beneficial effects in animal models of acute neurodegeneration induced mainly by hypoxia and ischemia.44‒46 Mdzinarishvili et al.,47 showed that pre-treatment with EGb761 extracts strongly reduce cellular oedema formation and neurodegeneration under ischemia conditions and that the mechanism could be related to a reduction of excitotoxicity due to high glutamate release during ischemia.
Huang et al.,48 observed suppression of excitotoxicity and apoptosis by treatment with extract EGb761 from Ginkgo biloba in a model of type 17 spinocerebellar ataxia. This is a polyglutamine disease caused by the expansion of CAG/CAA repeated groups in the TATA box-binding protein (TBP) gene that leads to protein aggregates in these patients. This founding suggests that EGb761 may be a potential therapeutic agent for treatment of this disease. Using a cellular model of Huntington’s disease (HD) by employing cells expressing pathological variants of a polyglutamine protein (polyQ protein), some authors have shown that the EGb761 extract modulates proteasome formation by inducing proteasomal protein degradation suggesting a therapeutic function of this extract in neurodegenerative disorders with disturbances in protein homeostasis.
It has been also shown that in Alzheimer’s disease the treatment with EGb761 induces protective effect under distinct mechanisms, such as: 1) antioxidative;49,50 2) scavenging of free radicals;51 3) anti-amyloidogenic;52,53 4) anti-inflammatory;54 and 5) anti-apoptotic.55 Although the mechanism of action of EGb761 extracts from Ginkgo biloba is not well known several reports may be taken into account. It has been found that bilobalide improves mitochondrial activity and preserves ATP level during ischemia.56 Schwarzkopf et al.,57 concluded that neuroprotection by bilobalide may involve a mechanism in which this compound reverses ischemia-induced changes in mitochondria, leading to a reduction of glutamate release. Other constituents of EGb761, as flavonoids and ginkgolides, seem to have beneficial effect in models of neurodegenerative diseases.58
Li et al.,59 have studied the pharmacological action of YY-1224, a terpene trilactone extract of Ginkgo biloba, against b-amyloid (Ab) toxicity and found that the protective effects of YY-1224 against Ab toxicity may be associated with the inhibition of the Ab-mediated pro-inflammation of microglia as well as with its neurotrophic and antioxidant effects. Some authors have proven that EGb761 reduces neuronal apoptosis and promotes angiogenesis in experimental intracerebral haemorrhage via RSK1/GSL3b pathway.57 It has been observed that the neuroprotection accounted for EGb761 derived-flavonoid monomers in an in vitro three-dimensional stem cell-derived neural model was mainly related to its antioxidant effect and inhibition of caspase 3 activity.60
Genista tinctoria
Genista tinctoria is a flowering plant that belongs to Leguminosae (Fabaceae) family, gender Genista. It is native to meadows and pastures in Europe and Turkey. This plant was used from ancient times for producing a yellow dye. This plant contains an isoflavone, which was first isolated from this plant in 1899 and was denominated genistein. The medicinal parts are the flowering twing and it has been used in popular medicine in skin diseases and other uses, even in modern times. Although, the identification, in this plant, of a yellow dye has led to be widely used in textile industry, however, genistein is an isoflavone with a great therapeutic use. In nature, genistein is found in several edible plants as lupin, soy, beans, coffee and so on61‒63 and medical plants as Flemingia vestita64 and Flemingia macrophylia. Genistein is one of the major isoflavones in soybeans with phytoestrogenic activities and may contribute to its potential anti-inflammatory, anticarcinogenic and hypocolesterolemic effects.65‒69 Genistein is bound to the cell to an estrogenic receptor beta agonist and represents an alternative to oestrogen in treating neurodegenerative disorders. Due to its estrogenic nature, genistein has a mechanism through its bound to estrogenic receptors localized in the cellular nucleus promoting activation and deactivation of determinate genes regulators of the protein synthesis.70,71 The are numerous evidences supporting the protective effect of genistein in ischemia.72 Soy isoflavones have several uses not only as endogenous estrogens in hormonal pathologies but also in inflammatory neurodegenerative diseases and pain.73 Soy contains isoflavones like genistein, diadzein74 and glycitein, an o-methylated isoflavone that presents a weak estrogenic activity.75 Isoflavones are polyphenol compounds with phytoestrogen activity and involved as potential beneficial factor in cardiovascular diseases and other actions as protectors in the repair of the brain injury in rats.76,77 Several studies on the cognitive effects of soy isoflavone have been reported presenting benefit,78 no effect79 and possible harm80 in older patients with difficulties in memory.
It has been proposed that genistein (5,7-dihydroxy-3-(4-hydroxyphenil9-4H-1-benzopyran-4-one) may be a potential drug for therapy of mucopolysaccharidoses, a group of metabolic diseases caused by mutations which lead to inefficient degradation of glycosaminoglycans (GAGs) and may cause neurological symptoms. This disease may be detected by the presence of heparin sulphate in urine and may be cause of different neurology symptoms. It has been demonstrated that genistein can cross the blood-brain barrier, making it a potential drug for the treatment of neurological symptoms present in most lysosomal storage diseases. Malinowska et al.,81 observed that in neurodegenerative metabolic disorders, such as mucopolysaccaridosis III B or Sanfilippo disease, genistein administered at high doses to MPSIIIB mice, significantly reduces lysosomal storage of GAGs, heparin sulphate substrate and neuroinflammation in the cerebral cortex and hippocampus, resulting in correction of behaviour defects. The mechanism by which genistein make its action is not well known. Genistein aglycone is a non-specific inhibitor of tyrosine kinase82,83 at pharmacological doses and reduces GAG substrate which is accumulated in fibroblasts of several mucopolysaccharidosis.84 Genistein administered to MPS IIIB mice significantly reduces liver lysosomal storage85 and inhibits lipopolysaccharidosis induced by TNFα in astrocyte cultures86 and protects dopaminergic neurons by inhibiting microglial activation.87 Moskot et al.,88 observed that the molecular mechanism of genistein action involves not only the GAG synthesis but the lysosomal metabolism by activating the transcription factor EB (TFEB). TFEB has been demonstrated as a crucial regulator of lysosomal biogenesis and autophagy. Accumulated studies suggest that TFEB has beneficial effects on neurodegenerative diseases, and also regulates cell clearance in lysosomal storage disorders.89 Ren et al.,90 observed that genistein has an anti-aggregant effect on both amyloid β-peptide associated with Alzheimer’s disease and human islet amylin (hIAPP) associated with type 2 diabetes. Park et al.,91 found a protective effect of genistein against neuronal degeneration in ApoE-/- mice demonstrating that genistein induced significant inhibition of oxidative stress and alleviated neuroinflammation. Genistein supplementation also reduced Aβ-deposition by reducing gene expression of APP-processing enzymes and decreased tau hyperphosphorylation by inactivating GSK-3 and JNK in the hippocampus and cortex and hyperphosphorylation in ApoE-/- mice fed with a high diet in genistein. This study also provides that dysregulated cholesterol metabolism may lead to an accumulation of Aβ and increases in oxidative stress and neuroinflammation.
It is increasing the knowledge that obesity, diabetes mellitus, hypercholesterolemia and non-alcoholic steatohepatitis are associated with multiple aspects of brain pathogenesis.92 It is believed that altered cholesterol metabolism play a role in major pathophysiological neurodegenerative diseases and some studies have demonstrated that the absence in apolipoprotein E (ApoE), the main apolipoprotein released by astrocytes and microglia that transports cholesterol between glial cells and neurons,93 leads to an increased susceptibility to neurodegeneration.
Yu et al.,94 found neuroprotection mediated by genistein in cortical neurons treated with Aβ-amyloid 25-35. These authors observed that genistein protected cortical neurons against apoptosis and maintained mitochondrial function damaged by Aβ-amyloid 25-35. Xi et al.,95 observed that SH-SY5Y cells incubated with Aβ-amyloid 25-35 induced down regulation of synaptophysin and postsynaptic marker as NR1 and NR2B which are subunits of the NMDA glutamate receptor. The author also detected that Aβ-amyloid 25-35 induced, on these cells, down regulation of mRNA and protein expression of Ca2+/calmodulin, CaMKII/pCaMKII and CREB/pCREB. However, pre-treatment with genistein reversed all these effects indicating that genistein mediated this action with the regulation of synaptic markers and activation of CaM/CaMK/CREB signalling pathway.
McDowell et al.,96 found that genistein prevented apoptosis in cultured ventral spinal cords cells exposure to supernatant of activated microglia by INF-γ. This protection was associated with increased expression of estrogen receptor β suggesting that genistein may promote neuroprotection via receptor-mediated pathways. Ma et al.,97 found that genistein may induce neuroprotective effect against action of Aβ-amyloid 25-35 in C6 cells. When these cells were treated with Aβ-amyloid 25-35 there was a loss of cell viability, increase of TNFα and IL-β, inflammatory markers, as well as upregulation of mRNA and protein expression of TLR4 and IκB. When the treatment was performed in presence of genistein there was an increase in cell viability, decrease of inflammatory markers (TLR4 and IL-β) and reversion of the deregulation of TLT4 and Iκ B. From these results, these authors inferred that the action of genistein might be mediated through the regulation of TLR4/NFκB signalling pathway and the abolition of inflammatory response.
Beneficial actions of genistein on mitochondrial DNA damage induced by Aβ-amyloid 25-35 in C6 glioma cells has been detected by Ma et al.,98 confirming that genistein could alleviate the mitochondrial-targeted oxidative damage induced by Aβ-amyloid 25-35. This finding suggests to the authors that genistein may be used by the treatment of neurodegenerative diseases. Liu et al.,99 using a model of rat ovariectomized to which was induced Parkinson by treatment with MPTP, observed significant decrease in dopamine and dihydroxyphenylacetic acid, a dopamine metabolite, and homovanillic acid in the striatum. This action was restore with genistein or estrogen pretreatment indicating that genistein may have neuroprotective effect on dopaminergic neurons.
In neurodegenerative diseases, genistein may have different effects such as estrogenic, anti-inflammatory, antioxidant and anti-aggregating. The estrogenic effect is mediate through the binding of genistein on nuclear estrogenic receptor promoting gen regulators of protein synthesis. The anti-inflammatory action is mediate by regulation of inflammatory markers as TLR4 and IL-6. The antioxidant action is promoted by the mitochondrial protection mediated by genistein that decreases ROS formation. The anti-aggregating action is due to the action of genistein preventing the protein binding (aggregation) and, as consequence, avoiding the aggregated protein that may be the cause of cellular death.
We are concerned that the approach of the ethnobotanical research should change, as most research on medicinal plants emphasizes the scientific documentation of plants and its uses for the benefit of large transnationals. We claim with this review for an interdisciplinary approach of ethnobotany based on the spread of knowledge on the phytochemical principles and its mechanisms for preventing neurodegenerative disorders as a right of any member of society. What is more, within an ageing society, the knowledge of natural sources and its potential consumption for disease prevention should be disseminated as part of the health education.
Authors pay tribute to the human groups that have collaborated with both their traditional knowledge and collection of the plants reviewed.
All authors declare no actual or potential conflicts of interest.

©2019 Gonzalez, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.