eISSN: 2379-6367


Research Article Volume 12 Issue 2
1Department of Pharmacology and Toxicology, University of Puerto Rico School of Medicine, PO Box 365067 San Juan, Puerto Rico
2Universidad Metropolitana–Cupey, Puerto Rico
Correspondence: José G Ortiz, Department of Pharmacology and Toxicology, University of Puerto Rico School of Medicine, PO Box 365067, San Juan, Puerto Rico 00936-5067, Tel 17874381051
Received: April 15, 2024 | Published: April 29, 2024
Citation: Peña-Jiménez JA, Suárez-Zayas EA, Licier R, et al. Kratom (Mitragynia speciosa), seizure latency, anxiety, and “social” behavior in the zebrafish. Pharm Pharmacol Int J. 2024;12(2):71-73. DOI: 10.15406/ppij.2024.12.00436
Kratom (Mitragyna speciosa) is used as a stimulant, an opioid-like analgesic, and a sedative. However, Kratom consumption has profound effects, such as seizures, withdrawal, hallucinations, coma, and cardiac or respiratory arrest. We tested Kratom's effects on pentylenetetrazole-induced seizures in adult zebrafish (D rerio) using hydroethanolic Kratom extracts. Kratom extracts have pro-convulsant effects at low concentrations (10-4-10-1 mg/mL), while sedation occurs at higher concentrations. In the open-field test, Kratom has no anxiolytic effects; however, "social" behavior was lost at high concentrations (1.0 mg/mL). Our results confirm the possible proconvulsant role of Kratom while questioning its anxiolytic effects.
Keywords: Kratom, zebrafish, pentylenetetrazole, seizures, open-field
KR, kratom (Mitragyna speciosa); KR, kratom; PTZ, pentylenetetrazole; NE, norepinephrine; 5HT, serotonin; MOR, mu-opioid receptor
Kratom, Mitragyna speciosa, is used in Southeast Asia as a stimulant, as an opioid-like analgesic, and as a sedative.1–4 Recreational use of Kratom has gained popularity in the last decade5 as an opioid substitute, and it is readily accessible. Kratom consumption has resulted in severe effects such as seizures, withdrawal, hallucinations, coma, and cardiac or respiratory arrest.6,7 A small number of deaths are linked to kratom products, and nearly all cases involve other drugs or contaminants.8,9
Zebrafish is increasingly popular in modeling human brain disorders, including drug addiction.10,11,12 There are safety questions on KR use; thus, we examined the effects of KR on pentylenetetrazole-induced seizures. Furthermore, we tested the reputed anxiolytic effects of KR, using the open-field behavior and sociability ("shoaling").
Chemicals Pentylenetetrazole (PTZ) was obtained from Sigma-Aldrich. All stock solutions were prepared in deionized water. Kratom (crushed leaves) – Super Powder was obtained from The Iamshaman Shop (https://www.iamshaman.com).
Animals: Adult 4 to 6-month-old male and female wild-type zebrafish (Danio rerio) were obtained from Caribe Fisheries, Inc. (Lajas, Puerto Rico). Deionized tap water supplemented with 60 mg/L Instant Ocean® Sea Salt (Spectrum) was used in the aquaria. Fish tanks were maintained with constant mechanical and biological filtration and aeration. The water temperatures were maintained at 25– 27°C using water heaters. Illumination (572 ± 20 lx) was provided by ceiling-mounted fluorescent light tubes on a 14h light/10-h dark cycle. Animals were fed twice daily with a 1:1 mixture of flake food –Tetramin® Tropical fish flake food (Tetra Co.) and Nutrafin Max® brine shrimp flakes formula and freeze-dried brine shrimp (Hagen Pet Food, Inc) [ 33]. All the experiments were approved by the University of Puerto Rico – Medical Sciences Campus, Institutional Animal Care and Use Committee.
Kratom extract: Freshly (daily) crushed leaves were extracted in 70% ethanol at 25°C and agitated for 1 hour at room temperature (22-24ºC) daily. The extract was then decanted. "Aged" extracts are fresh extracts stored in a refrigerator (2-4 ºC) for at least 21 days.
PTZ Seizures
The latency to the abrupt movements followed by loss of posture ("seizures") was determined from randomly selected untreated zebrafish placed for 1 hour in a 15 ml chamber with different Kratom concentrations prepared in aquarium water. After this, animals were transferred to a transparent tank with a final volume of 100 mL of PTZ (3mg/mL/22 mM) prepared in aquarium water. Experiments were recorded using an Olympus FE340 camera.13
Open-field ("anxiety") Behavioral testing occurred in three fish groups between 9:00 and 17:00 h during the light cycle. At least two fish had to be in one of the compartments to determine their preference. Zebrafish were placed in the center of an acrylic chamber 36.5 cm by 36.5 cm. divided into 6 cm by 6 cm squares, and recorded for 5 minutes. Zebrafish swimming behavior was recorded in a top-view for 5 minutes. Zebrafish movements were monitored to ensure the animals were active and not sedated. The percentage of time spent by the group in the center of the arena ("anxiety") was quantified and expressed as a percentage of total time.
"Dispersion" (loss of shoaling) The experiment was performed in the open field; however, the loss of group cohesion was quantified. "Dispersion" was defined as departing more than 2 "fish length" (approximately 7 cm) from the other fishes.
Statistical Analysis: Data were normalized to the control mean and expressed as mean values ± standard error of the mean (SEM) of at least three independent experiments (12-15 fishes). Curve fitting and statistics were performed using GraphPad Prism 9.4 (https://www.graphpad.com/scientific-software/prism).
Figure 1A shows the effects of different Kratom concentrations on seizure latency induced by PTZ Fresh KR extracts markedly reduce seizure latency at low concentrations (10-4-10-1 mg/mL). However, at 1.0 mg/m, the proconvulsant effects are lost. Latency at higher concentrations could not be tested because of the excessive sedation. In contrast, Fig 1B shows that "aged" KR extracts lose the proconvulsant effects, becoming anticonvulsant at 0.01 mg/ mL or higher.
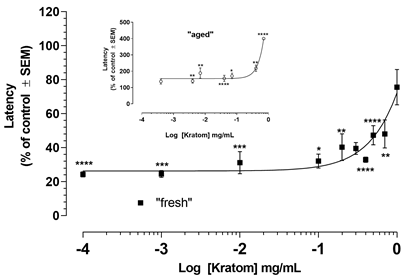
Figure 1a Pentylenetetrazole-induced seizure latency. At low doses, Kratom decreases the seizure latency. However, at high doses, the effects of Kratom on seizure latency are lost.
Figure 1b possibly because of sedation. (* p < 0.05, ** p< 0. 01, ** p < .001, *** p < 0.001, **** p < 0. 0001 vs 100 % control).
Kratom did not affect the time spent in the central area of the open field arena shown in Figure 2A. In contrast, "dispersion" (shoaling) was lost at 1mg/mL Figure 2B.
Pain management, opioid withdrawal, and fatigue are among Kratom's traditional uses.1,14 However, liver toxicity, seizures, and death have been reported.15,16 Furthermore, Kratom may potentiate the toxicity of co-administered medications through modulation of cytochrome P450, P-glycoprotein, and uridine diphosphate glucuronosyltransferase enzymes.17,18
Kratom induces analgesia and mild euphoria, yet with a lower risk of respiratory depression or adverse central nervous system effects than conventional opioids, prompting its use in managing the opioid crisis.19,4,20 Its effects and safety have resulted in national and international attention due to increased hospital visits and deaths in several countries.21
Mitragynine and its metabolite, 7‑Hydroxymitragynine, interact with opiate receptors and are credited with Kratom's effects.22,23,24 Mitragynine is a low-affinity antagonist in human mu-opioid receptor (MOR) in vitro, whereas 7-hydroxymitragynine acts as a partial agonist and has a 9-fold higher affinity than mitragynine.24 Recent studies24,25,17 attribute Kratom's reduced respiratory depression to the lack of interaction of mitragynine and several related compounds with the β-arrestin-2 signaling pathway. Kratom also interacts with NE and 5HT,26,27 and could be mediating the euphoriant, antidepressant, and antipsychotic effects.28 Seizures are among Kratom's symptoms.29 Our results are consistent with the proconvulsant effects of "fresh" Kratom extracts. The sedative effects observed at greater than 0.5 mg/ml KR could be "masking" its proconvulsant effects. This interpretation is indirectly supported by the results of the "aged" KR anticonvulsant effects.
Zebrafish form social groups, "shoals".30 The highly social nature of this species makes zebrafish particularly useful for examining the complexity of social behaviors and underlying biological mechanisms.12,31 On the other hand, KR alters social interactions at high concentrations. Alternatively, the loss of shoaling could reflect the effects of sedation. Using the open-field test, we could not find evidence for the anxiolytic effects attributed to KR. Commercial Kratom products are likely to contain artificially elevated concentrations of 7-hydroxymitragynine (among others), stressing the importance of increased dietary supplement oversight of Kratom-containing supplements.32,33 Moreover, our "aged" Kratom results suggest that the stability of different preparations may be a significant parameter in the reported effects and mechanistic studies.
Ethanolic Kratom extracts have proconvulsant effects (10-4-10-1 mg/mL), while at 1 mg/mL, severe sedation is observed. We could not detect its reputed anxiolytic effects.
E.A. Suarez-Zayas was sponsored by REU-CRIB Program University of Puerto Rico Rio Piedras.
The authors declare that they have no conflicts of interest.

©2024 Peña-Jiménez, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.