eISSN: 2377-4304


Research Article Volume 12 Issue 3
1Clinica PRONATAL (Bité Médica Hospital), México
2Clínica de Salud Femenica, Mexico
Correspondence: Vargas Hernández Víctor Manuel, Clínica de Salud Femenica, Mexico, Tel 5552179782
Received: January 19, 2021 | Published: May 10, 2021
Citation: Estuardo LIJ, Carlos DM, Roberto HR, et al. Prevalence of the type of delivery in Mexican patients at the private level. Obstet Gynecol Int J. 2021;12(3):124-128. DOI: 10.15406/ogij.2021.12.00564
Background: Childbirth is a physiological event for the expulsion of the fetus. It has a low maternal morbidity or mortality, does not present problems in subsequent pregnancies and it has a lower risk of fetal death and neonatal morbidity. Despite this, there are circumstances where cesarean section is the best option.
Objective: To determine the prevalence of delivery and cesarean section, and identify whether maternal age is an influencing factor when choosing the route of birth.
Methods: Retrospective, observational and cross-sectional study, carried out in Mexican women in private institutions during the period from 2015 to 2019. Inclusion criteria: women who attended the private hospital and had a medical history including maternal age, gestational age, number of deliveries and cesarean sections (emergency and elective) were included. Exclusion criteria were twin pregnancies and preterm births. Three age study groups were formed for deliveries and caesarean section A) 18 to 29years of age, B) 30 to 39 years of age and C) 40 to 45years of age and differences between deliveries and caesarean sections were compared. The SPSS Statistics package, version 25, was used; Descriptive statistics were performed including mean (±) standard deviation or percentage and comparison of groups by Chi-squared test.
Results: The decrease in childbirth is directly proportional to the increase in maternal age, with a higher prevalence of childbirth in women between 18 and 29years of age (Group A=60.79%) and a higher prevalence of cesarean delivery in women between 40 and 45years of age, age (Group C=48.19%). A statistically significant difference was found only in Groups A vs B, when comparing the prevalence of deliveries (60.79 vs 51.81%, p=0.05) and cesarean sections (29.21 vs 48.19%, p=0.05).
Conclusions: physiological delivery is preferred in our private institution; although, complications during pregnancy and childbirth associated with maternal ageing influence the higher rate of cesarean section.
Keywords: delivery, cesarean section, maternal age, private hospital
Labor is a chain of physiological events that allow the fetus to embark on the journey from the uterus to the external world. The mean duration of a single pregnancy is 40 gestational weeks (GW) (280 days) counted as of the last normal menstrual period. A pregnancy that lasts from 37 to 42 weeks is called full-term pregnancy.1
Vaginal delivery shows a low morbidity or mortality for the mother, it does not cause problems with future pregnancies, and represents a lower risk of fetal death and neonatal morbidity.2 Despite all of this, there are circumstances where cesarean section has to be considered as a delivery option, as with suitable indications it may effectively prevent maternal and neonatal morbidity and mortality.3,4 A small maternal pelvis, placental and possibly fetus infections, eclampsia, HELL syndrome, asphyxia and fetal acidosis, umbilical cord prolapse, placenta previa, and uterine rupture are examples of this.5 In addition, fetal suffering, dystocia, abnormal positioning, and previous cesarean sections, have been reported in 90% of the indications to carry out a cesarian section.6 Also, it has been observed that the development of instruments for fetal monitoring has increased the number of cesarean sections practiced as a result of the discouraging signs observed by obstetricians.7 Additionally, cesarean sections by election have increased the practice of this kind of sections up to unprecedented levels, with a rate of 40.5% in Latin America and the Caribbean, where Dominican Republic shows a rate of 56.4%, and 42.9% in South America, where Brazil shows a rate of 55.6%.8 These rates exceed by far the recommendation of the World Health Organization (WHO) about no to practice cesarean section in more than 15% of pregnancies, established in the 80’s,9,10 as well as the Mexican Official Standard 007 that establishes a maximum of 15% in 2nd level hospitals and 20% in 3rd level hospitals.11
As previously described, labor may expose women and babies to many risks. For this reason, it is very important the choice of the route of delivery.12,13 This decision should be taken by evaluating closely the mother and the fetus during pregnancy, which may also be affected by factors such as the mother’s age, perinatal alterations, and the mother’s choice.1,14 Older women (35 years or more) may have a higher risk of adverse obstetric and perinatal results,15 reason by which the delivery by cesarean section might be their best option.16
Accordingly, the objective of this Article is to determine the prevalence of vaginal and cesarean delivery, and to identify if maternal ageing is an influencing factor for the choice of the delivery route in women attending to Pronatal clinic (Hospital Bité Médica, CDMX, Mexico).
This is a retrospective observational and cross-sectional study, carried out in women whose labor was attended at the Bité Médica hospital between 2015 and 2019. Inclusion criteria: women who attended to the hospital showing a medical history, with any maternal age, number of deliveries and cesarean sections (emergency and elective), with ≥ 1 deliveries, all the deliveries of each patient, and gestational age of 37 to 42 GW. Exclusion criteria were twin pregnancies and preterm births. Parameters to be studied: Age, vaginal delivery and delivery by cesarean section.
Clinical variables: Vaginal delivery and delivery by cesarean section.
Patients were followed during their pregnancies and, when convenient, the clinical or personal decision of the type of delivery was taken. Once obtained the data, a study population was selected. Three study groups were formed: Group A: vaginal deliveries and deliveries by cesarean section in women from 18 to 29years old; Group B: vaginal deliveries and deliveries by cesarean section in women from 30 to 39years old; and Group C: vaginal deliveries and deliveries by cesarean section in women from 40 to 45years old. The prevalence of vaginal deliveries and deliveries by cesarean section was evaluated in all the patients per study group, and the differences between the two types of delivery were compared, and the same comparison was made for each one of the years studied (2015 to 2019).
The software SPSS Statistics, ver. 25 was used for the descriptive statistics. The mean±standard deviation or percentage and group comparison by chi-squared were determined.
Two thousand, two hundred and twenty records of women who gave birth between 2015 and 2019 in the Bité Médica Hospital were reviewed. The range of age was 34±5.8years old. A higher prevalence of vaginal delivery was observed compared to delivery by cesarean section, as shown in Table 1.
Deliveries between 2015 aND 2019 (Bité Médica Hospital) |
||
Maternal age [years (mean ± SD)] |
34 ± 5.8 |
|
n |
% |
|
Cesarean Section |
945 |
42.56 |
Vaginal Delivery |
1275 |
57.43 |
Total |
2, 220 |
100 |
Table 1 Prevalence of each type of delivery in the whole patient population. Data are given in per cent; n, number of individuals per group)
The evaluation of vaginal delivery versus cesarean section in the several groups of age shows that the decrease in vaginal deliveries is proportional to the increase of maternal age, with showing a higher prevalence of vaginal delivery in women from 18 to 29years old (A=60.79%), and a higher prevalence of cesarean section in women from 40 to 45 years old (C=48.19%). However, a statistically significant difference was found only in Groups A vs B when comparing the prevalence of vaginal delivery (60.79 vs 51.81%, p=0.05) with delivery by cesarean section (29.21 vs 48.19%, p=0.05) (Figure 1).
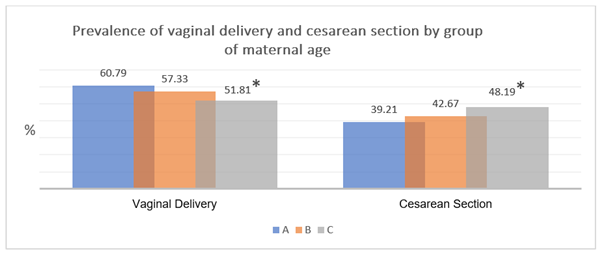
Figure 1 Prevalence of vaginal delivery and delivery by cesarean section by group of maternal age.
*Significant difference between Groups A and B (p≤0.05).
Table 2 and Figure 2 show that from 2017 to 2019 there was a decrease in vaginal deliveries and, therefore, an increase in cesarean sections associated to maternal ageing. Data are statistically significant only for 2017 in vaginal delivery (A=73.24% vs B = 60.10% vs C=41.67%, p≤0.05) as well as cesarean section A=26.76% vs B=39.90% vs C=58.33%, p≤0.05). On year 2016, data did not show a significant difference, and showed an increase of vaginal deliveries directly proportional to maternal ageing (A=51.85% vs B=55.47% vs C=63.4%) in contrast to cesarean sections (A=48.15% vs B=44.52% vs C=36.36%).

Figure 2 Prevalence of type of delivery by maternal age in each one of the years evaluated (2015-2019). Data are given in percentage.
*A vs B and C of year 2017 show a significant difference (p≤0.05); and **B vs A and C of year 2017 show a significant difference (p≤0.05).
Table 2 shows a numerical decrease of deliveries by cesarean section from 2015 to 2018 (45.41 a 41.78%), and a small increase in 2019 (44.2%).
|
2015 (n=401) |
2016 (N=379) |
2017 (N=530) |
|||
Age |
Vaginal delivery |
Cesarean section |
Vaginal delivery |
Cesarean section |
Vaginal delivery |
Cesarean section |
A, % (n) |
54.54 (42/77) |
45.45 (35/77) |
51.85 (28/54) |
48.14 (26/54) |
73.23 (52/71)* |
26.76 (19/71)* |
B, % (n) |
55.36 (165/298) |
44.63 (133/298) |
55.47 (162/292) |
44.52 (130/292) |
60.09 (247/411)** |
39.9 (164/411)** |
C, % (n) |
53.84 (14/26) |
46.15 (12/26) |
63.63 (21/33) |
36.36 (12/33) |
41.66 (20/48) |
58.33 (28/48) |
Total, % (n) |
54.58 (221/401) |
45.41 (180/401) |
56.98 (211/379) |
43 (168/379) |
58.32 (319/530) |
41.66 (211/530) |
|
2018 (N=503) |
2019 (N=407) |
||||
Age |
Vaginal delivery |
Cesarean section |
Vaginal delivery |
Cesarean section |
||
A, % (n) |
62.31 (43/69) |
37.68 (26/69) |
60.34 (35/58) |
39.65 (23/58) |
||
B, % (n) |
59.54 (237/398) |
40.45 (161/398) |
54.6 (178/326) |
45.39 (148/326) |
||
C, % (n) |
52.77 (19/36) |
47.22 (17/36) |
52.17 (12/23) |
47.82 (11/23) |
||
Total, % (n) |
58.20 (299/503) |
41.78 (204/503) |
55.7 (225/407) |
44.2 (182/407) |
||
Table 2 Prevalence of delivery associated with maternal age in each year studied (2015-2019). Data are shown as percent; n, number of individuals per group. *A vs B and C of year 2017 show a significant difference (p≤0.05); and **B vs A and C of year 2017 show a significant difference (p≤0.05)
Finally, on year 2015, the prevalence of vaginal delivery was higher compared to the cesarean sections carried out and values kept similar in the different groups of age for vaginal deliveries (A=54.55 vs B=55.37 vs C=53.85%), as well as cesarean sections (A=45.45 vs B=44.63 vs C=46.15%) (Table 2) (Figure 2).
In Mexico, the Official Mexican Standard NOM-007-SSA2-2016 for taking care of women during pregnancy, delivery and puerperium [Official Gazette of the Federation (DOF) 2016], establishes that it is necessary to prioritize the normal or vaginal delivery and to reduce the rate of cesarean sections.
Vaginal delivery has important benefits such as the prevention of mayor surgery, a faster recovery, and a shorter hospitalization. Additionally, the benefits for the product include a “natural” physiological adaptation to the external environment, fewer infections theoretically, and an immune function potentially improved with respect to the intestinal function in the short and long term, among others.17 Because of the benefits of the vaginal delivery, in Pronatal (Bité Médica Hospital) we give priority to this procedure, with a prevalence of 57.4%, which contributes to generate less risks for mothers caused by unnecessary cesarean sections. Even with this ideology, there are situations where the only delivery option is the cesarean section, which shows a prevalence of 42.56% in this study that allows us to keep values similar to those of the INEGI (46.1%) in 2019,18 and Private Hospitals of Mexico, that showed a prevalence of cesarean sections of 42.4 to 48.1% between 1994 and 1997.19 These data clearly reveal a trend favoring the preference of vaginal delivery by our physicians which has decreased the practice of cesarean sections compared to what is currently reported in private clinics, that at the national level have shown a prevalence of up to 85.6% during recent years.20 This means that private institutions show the highest number of deliveries by cesarean section, followed by clinics and hospitals of social security, and public hospitals for beneficiaries.21
With respect to maternal age, there are studies that report a higher probability of cesarean section with a prevalence of up to 43.1% in women older than 35 years compared to 21.7% in women under 25years old.16,22,23 This is similar to what we observed in this study, where we report an increase of cesarean sections directly proportional to maternal ageing, where said increase in women ≥40years old is statistically significant compared to women < 30years old (48.19 vs 39.21%, p=0.05). On the other hand, Bernal C, 2018, in a review of the status of the delivery by cesarean section, found that primiparous women from 12 to 19years old and ≥35years old constitute the group with the highest exposition to cesarean section, with a probability of up to 61% in women ≥35years old.21
As can be observed, women of higher age during pregnancy may show an increased prevalence of delivery by cesarean section possibly associated to a higher rate of conditions such as maternal chronic hypertension, maternal diabetes mellitus type 1 or 2, and gestational, maternal cardiac diseases, gestational hypertension, preeclampsia, intrauterine growth restriction, premature placental rupture, placenta previa, and placental detachment, as some studies have reported.24–28
All of this in addition to the increase of elective cesarean sections, which are multifactorial and complex as a result of cultural factors specific of the situation, along with previous experiences and interactions with health professionals (Donovan & Donovan, 2018).
In turn, maternal mortality, amniotic fluid embolism, venous thromboembolism, infections (endometritis, urinary tract infections, and infections of wounds), lesions (bladder and intestinal) and post-operatory ache, as well as disorders that appear in the long term or in subsequent pregnancies such as abdominal adhesions, placenta previa, placenta accreta, peripartum hysterectomy, uterine rupture, urinary and intestinal incontinence,30–36 including in newborns in the short term, slow lactation starting, respiratory disorders; and in the long term, reduction of intestinal microbiota, obesity, diabetes mellitus, and autoimmune diseases, are complications that might increase in number if the rate of cesarian sections practiced in private and public institutions is not limited.36–41
In contrast, controlled random assays have found that the induction of labor is associated to a better maternal outcome in women with mild hypertensive disorders after 37 weeks of gestation,24 and with a lower risk of shoulder dystocia and morbidity in large fetuses compared to the expectant management.6 Additionally, it might be the saving-life option for the mother as well as the fetus when indicated for cases such as small maternal pelvis (which makes impossible a vaginal delivery), chorioamnionitis (requiring immediate delivery), eclampsia, and HELLP syndrome (potentially mortal pregnancy complications), fetal asphyxia or acidosis (potentially mortal situations for the fetus that might cause fetal hypoxia), umbilical cord prolapse between the fetus head and the vagina, placenta previa (anomalous placental position preventing vaginal delivery), anomalous fetal positioning (prevents vaginal delivery), and uterine rupture (acute condition that threatens the life of both of them).42–44
Finally, the data obtained in this study were the result of the philosophy of giving the patients the natural delivery as a first option, in which the physician is present only to guide the patient and to intervene in case of complications, which has been achieved by a good management of patients considering factors such as maternal age, indications of delivery induction, the existence of previous cesarean sections, the obstetric or perinatal indications, and the uniform report of the fetus wellbeing by ultrasound and cardiotocographic records.
None.
None.
The author declares that there is no conflict of interest regarding this study.

©2021 Estuardo, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.