eISSN: 2377-4304


Case Report Volume 13 Issue 4
1Department of General Surgery, The Brooklyn Hospital Center, USA
2Department of Obstetrics and Gynecology, The Brooklyn Hospital Center, USA
Correspondence: Dmitry Youshko, MD, FACOG. The Brooklyn Hospital Center. 121 Dekalb Ave, Brooklyn, NY, 11201, USA, Tel 718-250-7494
Received: July 05, 2022 | Published: July 19, 2022
Citation: DOI: 10.15406/ogij.2022.13.00652
Background: Gossypiboma is a foreign object left in the cavity after surgery causing a fibrinous reaction. We report a case of asymptomatic abdominal gossypiboma missed for ten years after an abdominal myomectomy at an unaffiliated facility.
Case presentation: A 57-year-old postmenopausal woman presented to our clinic for a second opinion regarding a palpable mid- abdominal mass. A computed tomography scan revealed an abdominal mass with an unidentifiable retained foreign object. Patient underwent exploratory laparotomy with mass resection which was noted to be a laparotomy pad. Her postoperative course was uncomplicated and was subsequently discharged.
Conclusion: Gossypiboma cases have been reported previously, however, they are uncommonly encountered in gynecological surgeries. Therefore, an abdominal mass in patients who have undergone prior laparotomy may be undetected for extended periods of time.
Keywords: Gossypiboma, Retained Foreign Body, Sponge, Abdominal Mass, Fibrous Mass, Gynecologic Surgery Retained Body
Teaching points:
Gossypiboma is the term given to a surgical sponge, gauze, or towel retained in the body after surgery causing a fibrinous reaction. Granted a very rare condition, it is a preventable complication in which cases are seldom reported due to medicolegal implications.1 Due to the under-reporting of retained foreign object cases, incidence numbers are difficult to articulate. Common risk factors identified in published studies include emergent surgical interventions, inconsistent operative counts, obesity, inexperienced staff, inadequate number of staff, disorganization, deep seated operative locations, and usage of gauze and sponge in locations with minimal visibility.2–4 Most affected sites are abdomen (56%), pelvis (18%), and thorax (11%).5 Majority of Gossypiboma typically present within the first few days of surgery, but can be missed and remain undiagnosed for many years.6 Delay in diagnosis may occur due the number of diverse differential diagnoses in the context of post-operative complications. The most common presenting symptom is pain, however patients can present with nonspecific abdominal pain or distention, fever, lump, diarrhea, abscess, nausea, vomiting, anorexia, and weight loss.7 As a result of various cases being presented, revisions have been implemented - careful inspection of surgical sites and the addition of radio frequency chip identification have been more commonly used.1
We report a case of a missed retained surgical sponge at the time of an abdominal myomectomy; which later presented as a non-tender mid-abdominal mass ten years later.
57-year-old multiparous, postmenopausal female with past medical history of hyperlipidemia on simvastatin and aspirin. Surgical history is significant for three cesarean sections and a myomectomy ten years prior to presentation. Patient came to clinic for a second opinion due to palpable abdominal mass. A computed tomography (CT) scan was performed and showed a 10.8x11x11.4cm (length by width by AP) rounded, complex-appearing mass in the central to right-sided lower abdomen, upper pelvis (Figure 1). The mass incorporated two dense foreign bodies. One had a ring configuration and the other had the appearance of the distal portion of a surgical drain. It was decided by both general and gynecologic surgical services to proceed with an exploratory laparotomy. Prior to surgery, previous records, including abdominal myomectomy operative report, were reviewed and found to be non-contributory.
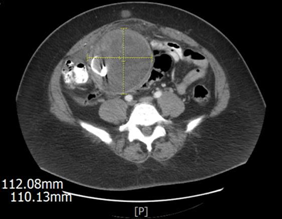
Figure 1 Transverse section of CT Abdomen/Pelvis with PO contrast, with and without IV contrast. Note the abdominal mass containing a radio-opaque object.
In the operating room, dense abdominal adhesions were noted, and lysis of adhesions was performed to gain entry into the abdominal cavity. A large, encapsulated mass was found adherent to the mesentery of the small bowel, the right colon, and the sigmoid colon. The mass was found to contain one laparotomy pad with ring (Figures 2) (Figure 3) and purulent material. Bowel adhesions were dissected off the mass using both blunt and sharp dissections. During the dissection of the mass, the bowel was inadvertently entered, requiring resection with an end-to- end anastomosis. Before closure, needle, sponge, and laparotomy pads were counted and found to be correct, x2.
The patient had an uncomplicated post-operative course. After tolerating regular diet she was discharged home on post-operative day three. One week post-operative evaluation consistent with normal expected recovery. Pathology results showed sclerosed, hemorrhagic and fibrosed round tissue containing foreign body.
A retained foreign body, while rare, can be a detrimental for the patient. Most retained foreign bodies include surgical sponges, pads, needles, forceps and rubber tubes, and pieces of broken instruments. Strikingly, 50% of gossypiboma’s are discovered five years or more after the day of procedure, and only 40% are found within the first year.8 Sponges and laparotomy pads are inert in nature, however, when left in the body, two types of reactions can occur. The first is a septic reaction with an exudative response.9 The human body recognizes the foreign body as not native and attempts to extrude it either externally or internally in a hollow viscous thus creating an abscess or fistula.8 The second type is aseptic and fibrinous which results in dense adhesion formation. The body encapsulates the foreign object and forms a granuloma.9 This granulomatous reaction is also termed a gossypiboma. The term gossypiboma is of Latin derivation from the word gossypiium, meaning cotton as most surgical sponges are cotton, and from the Kiswahili word boma, meaning place of concealment.10 Gossypibomas may remain clinically silent for years after the surgery. As such, these retained foreign bodies may be found incidentally on imaging or when a patient presents with nonspecific complaints that mimic an obstructive mass, as in this case. Examples of possible nonspecific symptoms include nausea, vomiting, and abdominal pain or discomfort, and even palpable nontender mass or protusion. Occlusive symptoms come from the space occupying lesion the body develop around the sponge. The gossypiboma has even been found to penetrate the alimentary and urogenital tracts by local pressure necrosis.
Radiographic evaluations can be useful in identifying a retained foreign body. Many instruments and sponges used today have radiographic markers that can be identified on imaging. Plain x-ray films easily identify the marker without discrepancy. However, in cases where the body walls the sponge or instrument off, the patient may not become symptomatic for decades, as in our case, and these markers are known to break down over time.8 On CT scan, the preferred modality for identification, the gossypiboma will be described as having a whorled appearance; characteristic for a retained sponge.10 However, over time with gossypiboma formation, CT scan will show a well- defined mass with a thick wall and a heterogeneous interior.8 In our case, the heterogeneous interior also showed a radio-opaque marker. Unlike metal surgical instruments, which can easily be detected on X-ray imaging.
Gawande et al. found that the incidence of retained foreign bodies varies from 1 in 8,801 to 1 in 18,760 in non- specialty acute care hospitals. They also found an increased incidence of retained foreign bodies after emergency surgery; as well as during an unexpected change in the procedure.11 A higher incidence of a gossypiboma was found in patients who underwent lower pelvic surgery and are obese, these factors present greater challenges related to difficult visualization.8 As noted by Kaiser et al.,12 most cases of retained surgical sponges have occurred after a documented correct sponge count.12
In preventing future complications of Gossypiboma, the final operative count, effective communication between operating room personnel and the medical team is crucial in any surgical setting to prevent additional patient safety complications, decrease health care costs, and mitigate the possibility for litigation. Surgical safety considerations and instrument counts should not only be limited to gauze pads but should be comprehensive including surgical instruments. When evaluating patients who present post-operatively, providers of the medical team should not overlook imaging findings; imaging slides should be confirmed with final written imaging dictations. Although modern day technology and imaging has improved detection, it is important to perform a thorough physical exam.
None.
None.
No potential conflict of interest was reported by the authors.

©2022 , et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.
 On the occasion of the International Day to End Obstetric Fistula (May 23rd), we join the global effort
to raise awareness about obstetric fistula, a preventable childbirth injury that continues to affect women worldwide. Often resulting from
prolonged, obstructed labor without timely medical care, obstetric fistula leads to severe physical and social consequences, yet it is both
preventable and treatable.
To highlight the importance of maternal health and to support this vital campaign, we are offering a 40% discount on any article submitted
to OGIJ. Together, let’s raise awareness, advocate for safe childbirth practices, and champion the rights of women to live with dignity and
access quality healthcare.
On the occasion of the International Day to End Obstetric Fistula (May 23rd), we join the global effort
to raise awareness about obstetric fistula, a preventable childbirth injury that continues to affect women worldwide. Often resulting from
prolonged, obstructed labor without timely medical care, obstetric fistula leads to severe physical and social consequences, yet it is both
preventable and treatable.
To highlight the importance of maternal health and to support this vital campaign, we are offering a 40% discount on any article submitted
to OGIJ. Together, let’s raise awareness, advocate for safe childbirth practices, and champion the rights of women to live with dignity and
access quality healthcare.