MOJ
eISSN: 2574-8130


Research Article Volume 3 Issue 1
1Graduate Program in Gerontology, Federal University of Santa Maria, Brazil
2Universidad de Ciencias Empresariales e Sociales, Argentina
3Graduate Program of Pharmacology, Federal University of Santa Maria, Brazil
4Brain Institute, Pontifical Catholic University of Rio Grande do Sul, Brazil
5Open University of the Third Age, State University of Amazonas, Brazil
Correspondence: Ivana BM da Cruz, Graduate Program in Gerontology, Federal University of Santa Maria, Brazil
Received: January 26, 2018 | Published: February 26, 2018
Citation: Praia RDS, Reboredo J, Barbisan F, et al. Brazilian elderly affective disorders and suicide: trends on morbi-mortality and health service costs . MOJ Gerontol Ger.2018;3(1):109-114. DOI: 10.15406/mojgg.2018.03.00095
Affective disorders (AD), including depression have important epidemiological impact on elderly morbi-mortality been also associated to elevate suicide rates. However, AD impact on trends elderly mortality, morbidity and Brazilian health service cost (hospitalization and outpatient care) need to be more deeply investigated. Therefore, this study evaluated the trends of AD and suicide mortality in Brazilian elderly population (1996-2015) and in use of health services (hospitalization and outpatient care) and their costs in 2009 to 2015 period by a socio-ecological analysis using databank evaluable for Health Unic System (DATASUS, Brazil Ministry). The study was performed just in elderly subjects (> 60 years old) considering as co-variables: sex ad age. Linear, Joint point and multivariate regressions were used to detect change in the trends of AD and suicide mortality. Total AD mortality was slightly higher in women (1.2/100.000) than men (1.0/100.000). At contrary, suicide mortality rate was higher in men (13.5/100.000) than females (2.5/100.000). In both mortality causes, occurrence was age-dependent, with higher rates in oldest-old group (> 80 years). Hospitalizations by AD was also higher in older group, in both sex. However, hospitalization costs trend to decrease in the last four years. The whole of results suggests the necessity to construct specific preventive and treatment programs for elderly people, since this population presents important biological, functional, health and social specificities that are different of find in adults.
Keywords: aging population, depression, mental health, mortality, hospitalization, health service costs
AD, affective disorders; BPR, brazilian psychiatric reform; ICD-10, – international code of diseases; SUS, single health system; SIM, brazilian mortality information.
Mental disorders, affect about 350 million people worldwide representing approximately 12% of total diseases.1 Due their characteristics, in general population, psychiatric disorders are associated with a strong presence of epidemiological panorama, since can interact, aggravate, or even constitute independent risk factor for several types of non-transmissible diseases, such as cardiovascular diseases.2-4 In elderly population, affective disorders (AD), especially depression is often undetected and inadequately treated.5
Furthermore, despite depression to presents similar symptom between elderly and younger populations is more common the occurrence of other concomitant medical disorders and cognitive impairment.5 Therefore, in elderly, close association between AD and other organic diseases elevate the use of health services (hospitalization and outpatient cares), decreasing patient´s life quality and increasing mortality prevalence for direct or indirect mental health causes, including suicide.6
For this reason, elderly AD could be considered a strategic point in the clinical and social management of geriatric patient. It is not an easy task, mainly considering middle-income countries, such as Brazil that have experienced a rapid increase in their proportion of elderly people (> 60 years old). In this country, the protection and rights of people with mental disorders are regulated by a law known as the Brazilian Psychiatric Reform (BPR), by Psychological Care Network inserted in the Single Health System (Sistema Único de Saúde, SUS), that is a Brazilian universal free healthcare system for all population. This network organizes all SUS services related to mental care treatments including 1) primary care, 2) accident and emergency care, 3) psychosocial care, 4) hospital and ambulatory specialized care, and 5) health surveillance.7
Despite advances in Brazilian mental illness care BPR associated, there is necessity to evaluate if general mental health services could impact positively in elderly population, or there is necessity to consider differential structuration of mental health services to attend clinical and social specificities of the elderly population. Based in this context, the present study evaluated trends of mortality of elderly AD-diagnosed or who committed suicide from 1996 to 2015, and also morbidity (hospitalization and outpatient care) and Brazilian health service cost related to elderly AD-diagnosed.
Study design
A socio-ecological study was carried out to determine AD mortality, depression hospitalization and its health service cost of elderly people (> 60 years old). All data used in the analysis were obtained from databank provided by SUS (DATASUS) maintained with government information of Brazil Health Ministry.
Ad and suicide mortality trend analysis
The AD and suicide mortality trend in Brazilian elderly were performed considering 1996 to 2015 years. In this period all death causes were classified according International Code of Diseases, ICD-10 making it possible to compare them over time. In the analysis, are included two years that mark important events in mental health care in Brazil. In 2001 BPR was approved and in 2011 was implanted Psychological Care Network which manages all services related to mental health in Brazil. To perform these analysis, data were obtained from Brazilian Mortality Information (SIM) coordinated by Department of Health Analysis Situation of Secretariat of Health Surveillance, Brazilian Health Ministry together with the States and Cities Health Secretariats. In this study were analyzed number of deaths counted according to the place of residence of the deceased. AD mortality causes are group in the F30-39 ICD-10 classification that includes follow psychiatric diseases: manic episodes (F30), bipolar disorder (F31), depressive episodes (F32), depressive recurrent disorders (F33), humor disorders (F34), affective mood persistent disorders (F34) and other affective humor disorders (F38). We consider all AD disorders to analyzed mortality trend since depressive symptoms are present in most of these morbidities. Furthermore, sometimes is not possible to perform an accurate psychiatric diagnosis in elderly people due presence of comorbidities and other intervenient variables. Co-varieties influence on AD and suicide mortality include sex, and three elderly age group: 60 to 69; 70 to 79 and >80 years.
AD morbidity analysis
Brazilian elderly morbidity presenting AD diagnosis was evaluated by hospitalization trend considering data from 2009 to 2016 period, since this period presented all governmental evaluable data to conduct epidemiological analysis. From BPR law, psychiatric hospitalizations is limited to general hospitals and just when occur critical psychiatric conditions of patients, which can mean a threat to the patient's own life or to the lives of others. In other words, at principle there is no long-term hospitalization in Brazil for mental health patients. Therefore, analysis of elderly AD hospitalizations could be considered an indicator of this psychiatric problem. To conduct this analysis, morbidities data were obtained from the Hospital Information System of SUS-SIH/SUS, managed by the Ministry of Health, through the Department of Health Care, together with the State Health Secretariats and the Municipal Health Secretariats, being processed by DATASUS – Department of Informatics of the SUS, of the Executive Secretariat of the Ministry of Health. The hospital units participating in the SUS (public or private agreement) send the information of hospitalizations made through the IAH – Authorization for hospital admission, for municipal managers (if in full management) or state (for others). This information is consolidated in DATASUS, forming a valuable database, containing data of most of the hospitalizations performed in Brazil. Outpatient care costs were also obtained from this same databank information. However, the period analyzed was shorter (2009 to 2016) than AD and suicide-mortality analysis, since just from 2008 these data are available for analysis.
Statistical analysis
Epidemiological data were organized in Excel program datasheet. Annual total number of deaths in > 60 years was included for the analysis of mortality trends. Trends were analyzed here using Jointpoint regression analysis using free software developed by Surveillance Research Program, National Cancer Institute (USA) that is also use to analyse trends by other mortality causes. The tests of significance use a Monte Carlo Permutation method. The models may incorporate estimated variation for each point (e.g. when the responses are age adjusted rates) or use a Poisson model of variation. In addition, the models may also be linear on the log of the response (e.g. for calculating annual percentage rate change). In Joint point regression the jump model and comparability ratio model provide a direct estimation of trend data where there is a coding change, which causes a "jump" in the rates, but is assumed not to affect the underlying trend. The software automatically locates the discontinuity or "jump" halfway between this last data point and the next one.8 This analysis can be use to evaluate the effect of regulatory action by health services as performed by Wheeler et al.9 that performed an ecological study to analyse the impact on the incidence of suicide and non-fatal self-harm of regulatory action in 2003 to restrict the use of selective serotonin reuptake inhibitors (SSRIs) in under 18s.
Figure 1 presents general AD and suicide trends for Brazilian elderly according sex and age-group. Total AD mortality rate was low and slightly higher in women (1.2/100.000) than men (1.0/100.000). On the other hand, total suicide mortality rate was higher in men (13.5/100.000) than females (2.5/100.000). In both mortality causes, occurrence was age-dependent, with higher rates in oldest-old group (> 80 years), intermediary rates in 70 to 79 years and lower rates with elderly 60-69 years old.
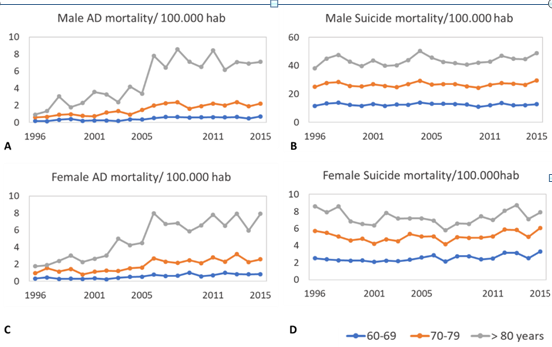
Table 1 shows a synthesis of main data of AD and suicide mortality analysis, describing annual percentage change (APC) and regression significance data according sex and age-groups. In males, AD mortality trend did not change significantly among period analysed here (Figure 2). At contrary, females with 60 to 79 years presented a significant linear increase in AD mortality frequency with an estimated 5.58% increment in AD deaths by year. Oldest-old females follow similar tendency of AD increase mortality until 2006, with higher APC value (near to 20% by year). However, from 2006 to 2015 this trend stabilized, even though AD mortality rates remained higher than observed in younger women (Figure 3).
Sex |
Age-group |
APC |
Regression data |
||
(years) |
Period |
Value |
Equation |
p value |
|
AD-Male |
60-69 |
1996-2015 |
-0.1 |
Y= 4.51 – 0.0009x |
0.378784 |
70-79 |
1996-2015 |
0.54 |
Y = -8.10 + 0.005x |
0.053468 |
|
> 80 |
1996-2015 |
0.73 |
Y = -11.74 + 0.007x |
0.111706 |
|
AD-Female |
60-69 |
1996-2015 |
6.29* |
Y = -122.97 + 0.063x |
0.000007 |
70-79 |
1996-2015 |
4.87* |
Y = -95.1 + 0.054x |
0.00026 |
|
> 80 |
1996-2006 |
19. * |
Y = -349.06 + 0.74x |
0.000314 |
|
2006-2015 |
0.55 |
Y = -9.57 + 0.0055x |
0.771058 |
||
Suicide-Male |
60-69 |
1996-2015 |
-0.1 |
Y = 4.51 – 0.00099x |
0.695546 |
70-79 |
1996-2015 |
0.1 |
Y= - 8.10 + 00053x |
0.053468 |
|
> 80 |
1996-2015 |
0.73 |
Y = - 11.74 + 0.0072x |
0.111706 |
|
Suicide-Female |
60-69 |
1996-2015 |
1.75* |
Y = - 33.79 + 0.017x |
0.000675 |
70-79 |
1996-2007 |
-2.79* |
Y = 57.578 – 0.028 |
0.002757 |
|
2007-2015 |
3.48* |
Y= -67.85 + 0.034 |
0.006248 |
||
> 80 |
1996-2015 |
-1.24 |
Y = 25.80 – 0.012 |
0.162679 |
|
Table 1 Annual percentage chance (APC) and statistical data of Brazilian elderly affective disorders (AD) and suicide mortality, by sex and age-group in 1996-2015 period
*Indicates that the Annual Percentage change (APC) is significantly different from zero at alpha = 0.05 level
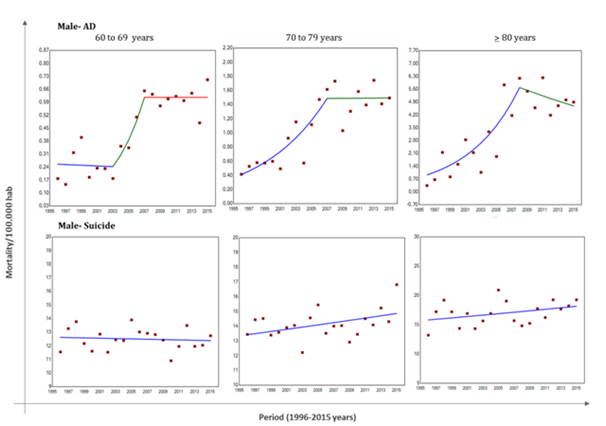
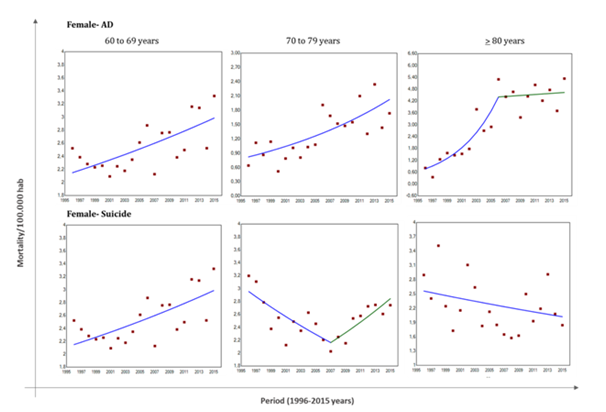
In relation to suicide mortality trends, males showed stable and higher rates without significant changes (Figure 2). On the other hand, females aged with 60-69 years increased significantly suicide mortality rates. Females aged with 70-79 presents change in their suicide mortality pattern. From 1996 to 2007 suicide rates decreased significantly. However, from 2007 to 2015, the curve reversed, with a significant increase in these deaths (Figure 3). Similar to men, oldest-old women (> 80 years) presented higher and no change suicide mortality rates.
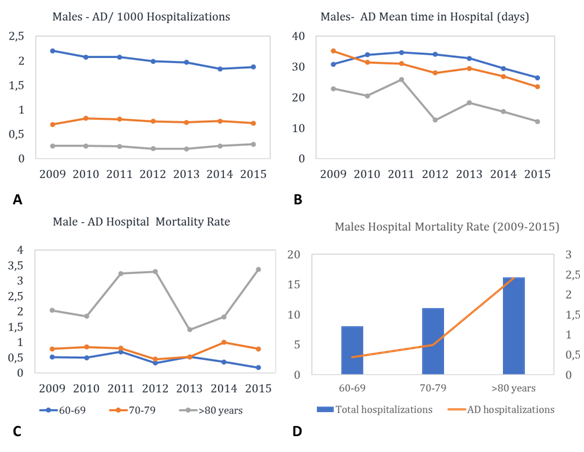
Second analysis performed here is respect to AD hospital morbidities indicator. Main results are presented in Figure 4, for men and Figure 5 for females. Data obtained from 2009 to 2015 indicated higher frequency of AD-males hospitalized with age ranging 60 to 69 years (1.99 ± 0.127/ 1000 hospitalizations) than males grouped to 70-79 years (0.75 ± 0.04/ 1000 hospitalizations) and > 80 years (0.24 ± 0.03/1000 hospitalizations). Complementary analysis showed no-changing pattern in this frequency in the period analysed here (Figure 4A). Other variable analysed is respect to mean time (days) that AD patients remained in the hospital. Again, elderly grouped to 60-69 years presented higher mean time of hospitalization than other AD subjects. However, in general mean times of hospitalization present a trend to decrease from 2012 year (Figure 4B).
Hospitalization mortality rate was also compared among AD elderly with different age groups. As expected older-group (> 80 years) presented higher mortality rate frequency than younger elderly. Among 2010 to 2012 occurred increase in the mortality frequency with elderly > 80 years (Figure 4C).
After a brief decline in this frequency, that occur in 2013 year, this indicator started to rise again (Figure 4C). A complementary comparison was performed between all-causes and AD-hospital mortality rate. As can see in Fig. 5D both death groups showed trend to increase according to age, despite the hospital mortality rate to be lower in AD-group than all-cases group.
In females, AD-hospitalization frequency presented a similar pattern observed in elderly males, with higher number of AD-hospitalization concentred in elderly aged among 60 to 69 years (Figure 5A).
Mean time (in days) than elderly females remained in the hospital was influenced by age just from 2013 year that older females started to remain more time hospitalized than younger female (Figure 5B). Comparison between hospital mortality rates in the period analysed showed similar results found to elderly males, trending to increase according age (Figure 5C). Other information about this variable is respect that hospital mortality rate in the period analysed here was higher in men (11.76±1.19/100.000 hospitalizations) than females (10.93±0.90/100.000 hospitalizations) (Figure 5D).
Health cost indicators were also analysed of Brazilian elderly AD-diagnosed in the period of 2009 to 2016. Considering large similarity in the values found to males and females, we opted to present these data jointed information obtained for each sex (Figure 6). Economic costs of AD hospitalization were initially evaluating considering % of these cost in relation to cost of hospitalization for all-diagnosed causes. In general, AD-hospitalization costs represented 0,25±0.05 % of all costs. Most cost were spent with AD-older patients (>80 years) trended to decreased from 2012 year (Figure 6A). Mean value for each hospitalization (in U$ dollar) is presented in Figure 6B. As can see this value was similar among different age-groups and trended to decrease from 2011 year. Another analysis from these data showed that mean value of each hospitalization trend to be similar between AD-patients and patients hospitalized by all-diagnosed causes (Figure 6C). In both groups values trend to decrease in the period investigated mainly in older patients (>80 years-old) (Figure 6D).
The present investigation performed a socio-ecological trend analysis of Brazilian elderly AD mortality, also considering suicide mortality that is an important mental health condition. Additionally, some morbidity indicators in AD elderly patients were also evaluated, as well as, associated-hospitalization costs. AD-mortality presented similar trend between males and females, whereas number suicides in elderly males was consistently higher that females. In both mortality causes, older subjects (>80 years old) presented higher mortality rates. Trends in these mortality rates trend to change in some situations, as well as morbidity indicators suggesting influence of health services actions related to management of these psychiatric morbidities. Therefore, it is important to discuss these points to evaluate potential impact of BPR on elderly population that present some AD clinically diagnosed or some psychiatric condition that cause suicide death.
AD diseases have important role in the elderly health and life quality, since depressive states including major depression has been associated with morbi-mortality in this age-group. However is not easy to evaluate general impact of depression on elderly mortality considering socio-ecological data. This reason of difficulty is related to fact that depression or depressive states associated with other psychiatric disorders can be considered a heterogeneous syndrome. Furthermore, effect psychological and somatic symptoms can be highly variable. An analysis of a sample of patients identified 1030 different profile symptoms in elderly subjects according diagnosed DSM-V criteria.10 For this reason, we opted to include in our mortality analysis elderly clinically diagnosed by some AD conditions included in the F30-39 ICD-10 classification. It is important to comment that, due lower number of elderly that mortality cause is considered some AD condition, we are not able to find large number of ecological studies involving similar analysis. On the other hand, there are great number of studies about suicide and suicide attempt in elderly population, including previous Brazilian investigations.11-15
Considering AD trends mortality analyzed here, is important to point out that population-based studies have demonstrated that over 8% of community-dwelling older people aged 50 years and over have clinically relevant depressive symptoms.16 This prevalence is higher if is considered elderly >70 years old.17 A cross-sectional study performed in 49,025 Brazilian adult subjects showed that 9.7% presented some degree of depressive symptoms and 3.9% had major depression. However, despite authors performed an age-correction of these values AD prevalence on elderly population was not specifically studied.18 In fact, nowadays is well established that depression and depressive states are related to poor prognosis of other somatic and metabolic diseases including cardiovascular morbidities.19 Depression as also closely related to cognitive decline, dementia and frailty in the elderly population.20
For this reason, we consider that mortality evaluation by AD-cause could be “the tip of iceberg” and did not represent all extension of mortality impact of this psychiatric disease on elderly mortality. Even so, as the diagnosis of mortality by mental health conditions has been improved in Brazil analysis of AD mortality trends could be considered relevant. Data analysis performed here showed an interesting trend in the elderly mortality by AD and suicide causes. Clearly, older elderly died by AD and suicide more frequently than younger elderly population. However, whereas suicide deaths presented higher and stable frequency in the period analyzed, deaths by AD-causes trend to increase in > 80 years subjects, and this trend was similar between males and females. However, morbidities indicators showed that younger elderly were more frequently hospitalized than older subjects, despite frequency of deaths in hospitals to be higher in older group than others.
From these results, two relevant issues could be considered here. First, is respect to increase of AD mortality trends in older subjects (> 80 years). Despite the increment in AD-mortality to be potentially related to improvement in the diagnosis of psychiatric mortality causes, prior investigations, as performed by Crumpacker21 consider that depression in later life is an important risk factor for death by suicide. Estimative have indicated that almost 800,000 persons die by suicide attempt.22 In relation of association between sex and suicide, is well known that its mortality cause is higher in male than females, and therefore, older male could be considered main suicide risk group. In order to explain these important epidemiological gender differences was developed the “concept of male depression” that could present differential and many times no detectable depressive symptoms, that many times are not recognized as depression.23 Recent studies about this epidemiological evidence, as performed by Briggs et al.24 have suggested that maintenance of suicide rates in older subjects could be associated to significant proportion of undetected or untreated cases of AD, especially depression.
The maintenance of high frequency of suicide in very older elderly is not universal and is potentially reversible. For example, studies such as developed by Shah et al.25 estimated a suicide decline in later life, suicide rates remain high in older people.25 Therefore, suicide rates found in Brazilian elderly > 80 years could be treated as important public health with specific preventive program with aim could be prevent suicide attempt.
However, as is commented by Briggs et al.24 interventions aimed at improving detection and treatment of depression and suicidal behavior in later life need to be targeted at several different levels. On the other words, these programs could be more specific considering the impact of complex social, biological, functional and health factors that act on elderly behavior leading to suicide attempt. In this respect, authors comment that if public awareness campaigns have been successful in reducing the stigma around mental health conditions in younger people, similar efforts are required to focus on later life subjects with suicide risk. From our results, we also suggest that, in elderly population these programs could extend their action to prevent concomitantly suicide and AD diseases.
Considering the specific Brazil context, Joint point regression curve analysis of AD and suicide mortality performed here suggest that current health services constructed to attend BPR law did not present affective actions to decrease mortality and morbidities indicators of AD elderly subjects. This because, despite to be occurred a decrease in the frequency of AD hospitalizations, mainly from 2012 year, as well as in the period of hospitalization (in days) and in the hospitalization costs, in general the number of AD and suicide deaths did not consistently decrease in the period analyzed here. Considering that exist a very good structure of mental health services belong to Brazilian Psychological Care Network, efforts to improve specific attention to elderly subjects could be constructed in the next years. Similar to other risk factors to chronic non-transmissible diseases, such as glucose to screening diabetes mellitus type 2, blood pressure, waist circumference, cholesterol levels to screening cardiovascular diseases, mammography to screening breast cancer risk, a program of AD detection in basic health units would be feasible through of trained nurse professionals in use of tools to identify possible depressive symptoms. There are several easy and ship instruments, such as geriatric depressive scale (GDS) that could to identify potential depressive and suicide elderly people. In this context, present study could be use as base to develop intervention investigations related to detection of AD and suicide ideation on elderly group. Furthermore, this initiative could have some economic impact in the hospitalizations and cost of these services.
Finally, it is important to comment that there are some methodological limitations to our study that must be noted: (1) this is a socio-ecological study, therefore we don´t know the exact context that AD deaths were determined; (2) some important variables are risk to AD and suicide mortality, such as education level, marital status and presence of comorbidities and frailty. Despite for some variables analyzed here we have data of educational and marital status; we opted to focus just sex and age as co-variable due a high Brazilian cultural, social and environmental heterogeneity. Therefore, complementary studies to evaluate influence of these and other social variables in AD and suicide mortality trends of Brazilian elderly, needs to be performed from future investigations.
None.
Authors declare that there are no conflicts of interest.

©2018 Praia, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.