Journal of
eISSN: 2373-6410


Case Report Volume 8 Issue 5
1Neurólogist Hospital Universitario Clínica San Rafael, Bogotá, Colombia
2Internal Medicine Resident, Hospital Universitario Clínica San Rafael, Colombia
3Internal Medicine specialist, Department -Hospital Universitario Clínica San Rafael, Colombia
Correspondence: Millan-Pérez Sonia, Neurólogist Hospital Universitario Clínica San Rafael, 17A 7 c – 49, T4 apto 121, Bogota, Colombia, Tel 573163329114
Received: September 18, 2018 | Published: October 30, 2018
Citation: Sonia M, Catalina A, Sandra C, et al. Hemi chorea as a first clinical manifestation of diabetes type 2. Case report and review of literature. J Neurol Stroke. 2018;8(5):270-271. DOI: 10.15406/jnsk.2018.08.00324
Diabetes is a metabolic disease that is often is associated with different systemic manifestations. Among these, there are some neurologic disorders that are the result of micro and microvascular damage. However, in some instances there can be movement disorders such as chorea and ballismus that are consequences of the direct effect of hyperglycemia in the basal ganglia, specifically in the sub thalamic nucleus.1‒3 In the next pages we present the case of a female patient with hemi chorea and hemiballism as the first manifestation of diabetes mellitus, conducting a discussion on the clinical manifestations, the pathophysiology, the radiological findings and the therapeutic options. Our aim is to point out the importance of an early detection of this reversible and treatable condition.
Keywords: Chorea, movement disorders, diabetes mellitus, hyperglycemia
Diabetes mellitus is an endocrine disorder that can present abnormal movements both at the beginning and during the course of the disease, especially when there is poor metabolic control of it.4Typically, within the manifestations of diabetes mellitus that compromise the nervous system, cranial mono neuropathies stand out, mainly affecting the third or fourth cranial nerves and peripheral polyneuropathy.5 However, other manifestations have also been described, among which are the abnormal movements within which chorea and ballism are found.1,2,4,5
Although the association between abnormal movements and diabetes mellitus has been known since the mid-1980s, there are few reports of chorea or ballism as an initial symptom of diabetes mellitus, with movement disorder being more frequent throughout the evolution of diabetes.4,6
The movement disorders are grouped by three main conditions: Parkinsonism, tremor and dystonia. These are commonly present in much pathology or due to an adverse effect to medication. The hemi chorea consists in the appearance of involuntary, continuous, writhe, rapid and abrupt contractions that affect half of the body.3,6‒8 Its more severe form is called hemiballism. Within the etiology of the hemi chorea-hemiballism syndrome, the non-ketotic hyperglycemia is the second most frequent cause, the first one being of vascular origin.9,10
Herein report describes the case of a woman who presented a sudden onset of symptoms characterized by choreic movements diagnosed simultaneously with diabetes mellitus.
A 68year old woman, without any medical history, consulted for seven days of non-rhythmic involuntary distal movements of sudden onset on the right upper extremity. Also, she presented wide brupt proximal movements, with variable amplitude and frequency. With the passing of the hours the movement compromised the ipsilateral lower extremity limiting the gait. Associated to this sherefered 12kg of weight loss in 2weeks, polyuria and polydipsia. In the physical exam right hemiballism and hemi chorea was present with an additional athetosical component. In the cerebral computed axial tomography no alterations were documented but the cerebral nuclear magnetic resonance shows in the T1 weighted sequence a hyper intensity in the left ventricular nucleus which is Hypointense in the FLAIR and does not generate vasogenic edema or mass effect Figure 1.
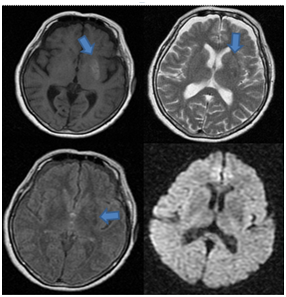
Figure 1 Cerebral nuclear magnetic resonance shows in the T1 weighted sequence a hyper intensity in the left lenticular nucleus which is Hypointense in the T2 and FLAIR sequences and does not generate changes in diffusion.
Within the laboratories, on admission there was a blood glucose level of 467mg/dl and glycosylated hemoglobin of 15%. During the hospitalization diabetes acute de compensation was dismiss. Once a better metabolic control was reached, symptoms decreased in a progressively, consequently she was discharged after a few days.
Although abnormal movements are a frequent manifestation of diabetes mellitus either at the time of diagnosis or during the course of the disease, there are few reported cases of chorea-ballism related to the onset of said pathology.
Although the exact cause of this syndrome has not been accurately determined, there are theories suggesting that elevated plasma glucose levels correlate directly with cerebral hypo perfusion causing activation of anaerobic metabolism and depletion of gamma-amino butyric acid (GABA) in the neurons of the basal nuclei, specifically in those of the striatum contra lateral to the affected body. The basal nuclei are a group of neuronal cells formed by the striatum (caudate and putamen), the globus pallidus, the subthalamic nucleus and the substantia nigra. These nuclei along with the cerebellum, the thalamus and the frontal cortex, compound the system responsible for the execution of normal movement patterns.3,7,8,10
This neurological disorder has been documented predominantly in postmenopausal women with diabetes mellitus in whom hyperglycemia can induce alterations in the dopaminergic activity of the striatum. In addition, since most of the published cases have occurred in Asian people, it has been suggested that there might be a racial influence or an underlying genetic predisposition. Additionally, most of the reports come from developed countries.3,4,6,9‒12
The cerebral computed axial tomography can be normal or demonstrate hyper density in the putamen, in the caudate nucleus or in both, always contra lateral to the hemi chorea. Normally, there is not surrounding edema or mass effect. In the magnetic resonance imaging a hyper tense lesion can be identified in the basal nuclei in the T1 sequence and a variable signal in the T2 and FLAIR.3,13
The cornerstone of the treatment is the glycemia intensive control with a resolution in most of the hemichorea and hemiballism cases. Occasionally, symptoms persist despite hypoglycemic treatment, reflecting a permanent damage. In such circumstances, deep brain stimulation of the internal globus pallidus has been evaluated as an alternative treatment. For this reason, diabetes must be include in the differential etiological diagnosis of chorea.10,14,15
In conclusion, although hemiballism-hemi chorea is one of the rare complications of involuntary movements induced by hyperglycemia, it is advisable to check blood glucose whenever patients with this type of movement disorder are found. It is a rare manifestation that deserves attention because it is reversible with the correction of hyperglycemia, for this reason its early diagnosis and treatment are essential to avoid adverse results.
None.
Author declares that there is no conflict of interest.

©2018 Sonia, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.