Journal of
eISSN: 2373-6453


Case Report Volume 9 Issue 3
MBBS, FRCPE, FRSTM & H, Liver Foundation Nepal, Kathmandu, Nepal
Correspondence: Santosh Man Shrestha, MBBS, FRCPE, FRSTM & H, Liver Foundation Nepal, Sitapaela Height Nagarjun Mincipality 4, Kathmandu, Nepal
Received: November 11, 2022 | Published: December 9, 2022
Citation: Shrestha SM. Liver Cirrhosis in Chronic Hepatitis B: is it due to Hepatic Vena Cava Syndrome: case report. J Hum Virol Retrovirol. 2022;9(3):65-73. DOI: 10.15406/jhvrv.2022.09.00251
Chronic hepatitis B (CHB) is a common chronic viral infection of man. Hepatitis B Virus is not a cytopathic virus. Extensive intrahepatic viral replication is compatible with normally functioning hepatocytes. Patients with CHB in the West manifest as a ‘healthy carrier’, whereas in Asia and Africa some develop liver cirrhosis and hepatocellular cancer. Liver cirrhosis in CHB is assumed to evolve through chronic hepatitis but its pathogenesis and the geographic difference in the outcome of CHB is not explained adequately.
Nepal is a country with low prevalence of CHB, where patients with CHB have hepatic vena cava syndrome (HVCS) as a comorbid condition. HVCS is a bacterial infection induced chronic obstructive disease of inferior vena cava at the site of hepatic vein opening. It is clinically characterized by long asymptomatic courses and occasional episodes of acute exacerbation precipitated by bacterial infection that result in hepatic venous outflow obstruction. Increased frequencies of acute exacerbations led to development of hypersplenism, liver cirrhosis and hepatocellular carcinoma.
Long time follow up of patients with CHB in Nepal showed development of cirrhosis in many but it was not related to the severity of viral replication or to the duration of the viral infection. Cirrhosis developed more frequently in patients with hypersplenism and those with severe and recurrent acute exacerbation of HVCS. These observations suggested that the development of cirrhosis in CHB in Afro-Asian countries may be due to the presence of HVCS as a comorbid condition. Reported here are a few cases of CHB that illustrate this point. Pathogenesis of cirrhosis in these patients is discussed.
Keywords: hepatitis B, liver cirrhosis, Nepal
HVCS, hepatic vena cava syndrome; CHB, chronic hepatitis B; VEGF; vascular endothelial growth factor
There are about 4 million people in the world with chronic hepatitis B (CHB) infection, 80 % of whom are in Asia and Africa. CHB is considered a common cause of liver cirrhosis and hepatocellular carcinoma in men based predominantly on epidemiological and clinical studies.1,2 CHB is usually asymptomatic and the majority of infected persons are unaware of it at the time of diagnosis. Natural course of CHB consists of an early replicative phase (HBeAg positive with high HBV DNA level) followed by non-replicative phase (HBeAg negative with decline in HBV DNA). In endemic areas both replicative and non-replicative phases lasted for several decades. About 3% of the patients achieved resolution of infection with loss of HBsAg, but may remain HBV DNA positive. CHB thus often is a life-long infection. HBV is not a cytopathic virus.3–5 Extensive ongoing intra-hepatic replication of the virus is compatible with normally functioning hepatocytes and presence of viral antigen in the hepatocytes showed no relation to liver damage.5–7
CHB patients behaved differently in different regions of the world. Patients in Western countries remained asymptomatic with normal transaminases and had very low risk of liver cirrhosis and hepatocellular carcinoma, and hence were labeled ‘healthy carriers’.8,9 In India a high proportion of patients both in the replicative and non-replicative phase had ALT elevations and showed some abnormalities in liver biopsy.10 Patients in China and Taiwan had intermittent elevation of transaminases labeled as acute flare and had histological changes in liver that varied from non-specific to chronic hepatitis and many developed liver cirrhosis and hepatocellular carcinoma.11–13
Liver cirrhosis in CHB is assumed to develop through chronic hepatitis. The frequently observed changes in liver biopsy of asymptomatic patients however were mostly non-specific or chronic persistent hepatitis that usually remained stable for many years. The outcome of chronic hepatitis was unpredictable.9,14 Patients with chronic persistent hepatitis have been observed to develop liver cirrhosis, whereas others with chronic active hepatitis had a benign course. A large number of CHB children from the West with chronic active hepatitis and chronic persistent hepatitis followed for 10 years none developed liver cirrhosis.15
According to the World Health Organization about 1/3rd of the world population acquired acute hepatitis B infection16 almost all of whom recovered spontaneously without any sequel. Liver damage in hepatitis B is immune mediated lysis of the hepatocytes.3,4 Patients with fulminant hepatitis that survived did not develop cirrhosis.17 About 5% of the patients in whom the virus had succeeded in evading the host immune system developed CHB. Liver cell damage that occurred in CHB during transition from replicative to non-replicative phase was also immune mediated as in acute hepatitis.18 The pathogenesis of liver cirrhosis in CHB patients from Asia and Africa thus remained unexplained.12
Nepal is an Asian country with low prevalence of HBsAg in population of 0.9% and low prevalence of HCV infection.19,20 But liver cirrhosis and hepatocellular carcinoma is common.21–23 In Nepal HBV spread occurred predominantly by horizontal transmission in the preadolescent age group.24 Replicative phase of CHB lasted for about two decades followed by a long non-replicative phase. And about 3% of the infected person achieved control of infection at around 4th decade becoming HBsAg negative but often remained HBV DNA positive. Among adult CHB patients about 80% were in non-replicative phase with low HBV DNA. One small community with high incidence of CHB and spread of infection by vertical transmission was identified.25 Those who acquired HBV by vertical transmission had a long replicative phase with very high HBV DNA levels that often extended to the 5th decade.
Hepatic vena cava syndrome (HVCS) a bacterial infection-induced disease of the hepatic portion of inferior vena cava that results in hepatic venous outflow obstruction (HVOO) is endemic in the country.26 The disease is seen predominantly among people of poor socio-economic background. .HVCS is a chronic disease with a long asymptomatic course. The initial lesion in the disease in inferior vena cava is a localized thrombophlebitis or endophlebitis at the site of hepatic vein openings which on resolution converts it to stenosis with development of cava-caval collaterals.27,28 The disease is diagnosed by ultrasonography and color Doppler (US/CD) examination of inferior vena cava and liver (Figure 1a&1b).29 An important clinical feature of the disease is the occurrence of recurrent acute exacerbations precipitated by bacterial infection. Acute exacerbation is marked by neutrophil leukocytosis, elevated level of C-reactive protein and ESR with mild elevation of transaminases and/or bilirubin. Severe acute exacerbation occasionally occurs with sudden development of ascites with or without pleural effusion associated with simultaneous development of bacterial peritonitis.30 Patients with recurrent acute exacerbations develop mild splenomegaly with hematological features of hypersplenism commonly neutropenia and/or thrombocytopenia.31 Acute exacerbation results in further deposition of thrombophlebitis at the site of the lesion that extends along its posterior wall and into intra-hepatic veins. Past episodes of acute exacerbations are indicated by presence in inferior vena cava of thrombophlebitis of different ages (Figure 2a–2d). Subsequent organization of the thrombophlebitis leads to development of a membrane in inferior vena cava in a few patients (Figure 2e). Recurrent acute exacerbations result in the development of thrombophlebitis, intimal thickening and stenosis of intra-hepatic veins and increase in echo-texture of the liver parenchyma that progress to cirrhosis (Figure 2e–3b). Medical management of the disease has been described.32
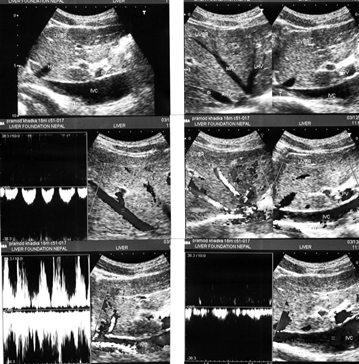
Figure 1a Hepatic vena cava syndrome is diagnose by ultrasonography and color Doppler (US/CD) examination of inferior vena cava and liver. This is a US/CD of young boy with CHB in replicative phase. It shows stenosis of the inferior vena cava at the site of hepatic vein opening with thick posterior wall and organized thrombophlebitis on it, the distal segment is dilated. Hepatic veins are prominent and show obstruction to blood flow at their outlets. The blood flow pattern in inferior vena cava and hepatic veins are abnormal.
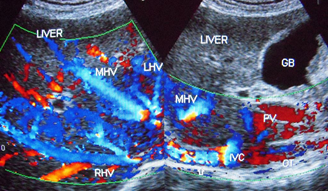
Figure 1b Ultrasonography & Color Doppler of inferior vena cava and liver showing stenosis of the vein at the site of hepatic vein opening with obstruction to blood flow, distal segment dilated with presence of old organized thrombus along posterior wall. of hepatic portion. Hepatic veins prominent with obstruction to blood flow at the outlets.
Figure 1 Diagnosis of Hepatic Vena Cava Syndrome.
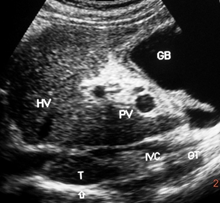
Figure 2a Recurrent acute exacerbations of HVCS: Inferior vena cava showing thrombophlebitis of different ages.
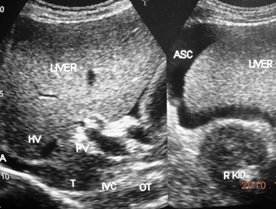
Figure 2b Severe Acute Exacerbations: Inferior vena cava showing thrombophlebitis of different ages with large recent thrombus at the mouth of hepatic veins causing ascites.
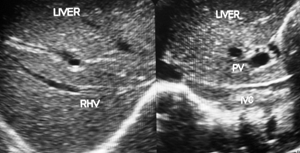
Figure 2c Development of chronic liver disease from recurrent acute exacerbations. It shows thrombophlebitis of different ages in inferior vena cava and thrombophlebitis and intimal thickening in Intra-hepatic veins with increase echo-texture of liver parenchyma.
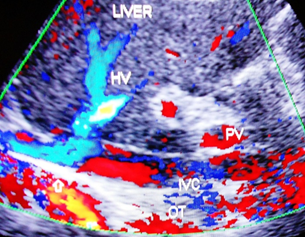
Figure 2d Color Doppler ultrasonography: Show stenosis of inferior vena cava at the site of hepatic vein opening and distal dilated segment of vein with old organized thrombophlebitis. Organized fibrosed thrombi on posterior wall show development of capillaries. Liver parenchyma has increased echo-texture.
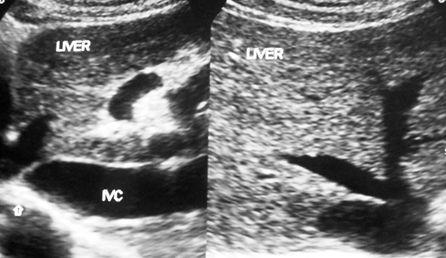
Figure 2e Development of membrane in inferior vena cava: The thrombophlebitis in inferior vena cava has organized into a membrane just distal to the opening of middle hepatic vein. Liver parenchyma shows feature of early cirrhosis.
Figure 2 Recurrent Acute exacerbation of Hepatic Vena Cava Syndrome is indicated by presence of thrombi of different ages in inferior vena cava and diffuse presence of thrombus or intimal thickening of intra-hepatic vein and progressive increase in echo-texture of the liver parenchyma .
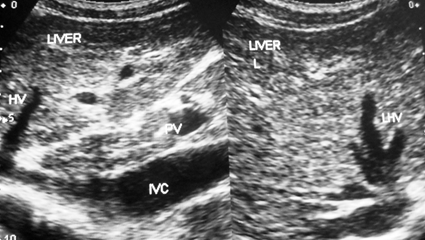
Figure 3a A young boy with CHB in replicative phase showing stenosis of a long segment of inferior vena cava filled with thrombus close to the site of hepatic vein. Distal segment is dilated and liver parenchyma shows features of cirrhosis. Middle hepatic vein is patent and dilated.
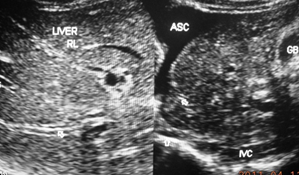
Figure 3b This patient with cirrhosis developed ascites from recurrence of acute exacerbation. The hepatic portion of inferior vena cava was filled with thrombophlebitis. Intra-hepatic veins are thrombosed with intimal thickening. There is a layer of peri-hepatitis around the liver and gall bladder wall is thick. Patient responded to medical treatment.
Figure 3 Development of liver cirrhosis in hepatic vena cava syndrome.
HVCS is complicated by high incidence of liver cirrhosis and moderate incidence of hepatocellular carcinoma.33 Liver cirrhosis developed from sinusoidal hypertension and its occurrence was related to severity or frequencies of acute exacerbations and not to the severity of the caval obstruction. Study of patients with liver cirrhosis and hepatocellular carcinoma in Nepal showed the majority had CHB and HVCS as common comorbid conditions.23
A long term follow up of a large cohort of CHB patients in Nepal showed that CHB evolved insidiously from replicative phase to non-replicative phase and to controlled infection asymptomatically over the period of several decades. Clinical manifestations and development of liver cirrhosis in CHB patients was related to the acute exacerbations of HVCS and not to the severity of viral replication or to the duration of the viral infection. Described below are a few cases of CHB that developed liver cirrhosis that illustrated the above points.
# 1. C163-08 AD 10 F
This young girl had recurrent episodes of bacterial infections since early infancy. In 2000 at the age of 2 years she was diagnosed with acute lymphatic leukemia and received multiple blood transfusions. She achieved remission from leukemia in November 2002, but was detected HBsAg positive. The girl’s father was employed in the Indian Army and was stationed in New Delhi, India where she received treatment in a military hospital from 2000 to 2010.
Blood tests showed HBeAg positive, anti HBe negative, anti-HCV and HCV RNA negative and a very high level of HBV DNA. She received antiviral treatment from 2002 to 2010. As she did not respond to the treatment the drug was changed from lamivudine to interferon, then to pegylated interferon and then to lamivudine and adefovir. HBV DNA assayed regularly remained around 2,606,706 IU/ml throughout this period. She had intermittent elevation of ALT/AST about 1.4 X to 4.0 X ULN with neutrophil leukocytosis during this period and developed progressive increase in echo-texture of liver parenchyma. A liver biopsy in 2003 showed the presence of cirrhosis.
In August 2008 while on a visit to Nepal the patient attended this clinic with chest infection and mild elevations of transaminases and bilirubin. US/CD showed evidence of HVCS. Liver had increased coarse echo-texture with diffuse presence of intimal thickening of intra-hepatic veins. She responded to treatment with oral antibiotic.
With father’s retirement the family moved to Nepal in early 2010 and attended this clinic to discuss the use of entecavir which had been prescribed. As antiviral treatment so far had been ineffective it was decided to discontinue its use and to have a regular follow-up for a few years which they did till 2016. During this period she had an episode of septic arthritis of right knee in November 2010, chest infection with Klebsiella bacteremia in 2012, ascites from HVOO in 2015, all of which was associated with elevation of transaminases up to 5 X ULN. She responded to treatment with antibiotic and diuretic. The counts of WBC and platelets were now on the low side. US/CD showed features of cirrhosis and mild splenomegaly. In November 2010 HBeAg become negative. When last checked in August 2016 she remained well with HBeAg negative and anti HBe positive with normal transaminases.
Comments: This girl with CHB in the replicative phase and recurrent acute exacerbations of HVCS precipitated by bacterial infection developed cirrhosis within a year of acquiring hepatitis B infection. Antiviral treatment was ineffective in controlling the viral replication and in preventing acute exacerbations and cirrhosis. She spontaneously converted to non-replicative phase 8 years after acquiring the infection.
# 2. C 109-016 NS 30F
This 30 year old female attended a local hospital from March 2012 to November 2016 with recurrent pelvic infections. Ultrasonography of the abdomen done in March and August 2012 showed normal liver but one done in October 2014 showed liver with increased echo-texture and mild splenomegaly. Routine blood tests showed HBsAg positive, anti-HCV negative and minimal elevations of bilirubin and transaminases.
She attended this clinic in November 2016. She was HBeAg positive, anti-HBe negative with HBV DNA level of 3,190,000 IU/ml and elevation of ALT/AST 1.5 X above upper limit of normal (ULN), serum bilirubin 2.1/0.9 mg/dl, WBC count 4000 neutrophil 60% and platelet count 86,000/cu mm. US/CD showed evidence of HVCS, splenomegaly and features of cirrhosis with prominent hepatic veins with obstruction to blood flow at the outlets. Inferior vena cava had stenosis at the site of hepatic vein opening and thrombophlebitis at different stages of organization along its posterior wall. The blood flow pattern in IVC and hepatic veins were continuous instead of triphasic. Gallbladder wall was thick. Upper gastro-intestinal endoscopy showed mild esophageal varices.
Family checks of HBsAg showed none were positive. She probably acquired hepatitis B infection from the tattoo she had in left arm 1 year back. Review of her blood tests done from March 2012 showed that counts of her WBC varied from 3900 to 5100, platelet was around 63,000/cu mm and hemoglobin from 7 to 12g, liver tests showed minimal elevation of ALT/AST of about X 1.1 to 1.3 ULN. A diagnosis of liver cirrhosis due to HVCS with hypersplenism in a patient with CHB in the replicative phase was made. She was prescribed entecavir to prevent spread hepatitis B to her family members.
In July 2017 while she was still on entecavir she developed fever with bloody diarrhea and was admitted to her previous hospital. A mild ascites was detected at ultrasonography and endoscopy showed grade III esophageal varices. She had elevated levels of transaminases. She improved on treatment with antibiotic and diuretic. And variceal ligation was done.
She became HBeAg negative and anti HBe positive in June 2017. HBV DNA was 480 IU/ml on 6’017 and became undetectable by 5’018. The level of transaminases fluctuated mildly from 1.1 to 1.8 X ULN. WBC count was around 2800 to 3100, platelet from 49000 to 95,000 and hemoglobin from 10 to 12 g. As her leukopenia did on improve on filgrastim treatment and WBC count dropped to 1,630/cu mm with 36% neutrophil and platelet count to 43,000/cu mm splenectomy was done on 22.6.018. Presence of micronodular cirrhosis was detected at the operation (Figure 4a). HBV DNA level at this time remained undetectable. Operation was followed by fever and neutrophil leukocytosis of 19,100 with 93% neutrophil and C-reactive protein 78 mg/L and development of ascites within a week. The condition responded to treatment with oral antibiotic and diuretic. During follow-up till February 2020 she remained well with WBC count of about 3400–6200 with hemoglobin around 12g and platelet count that varied from 170,000 to 380,000. In this period she had an episode of fever in September 2018 associated with elevation of CRP to 24 mg but no increase in WBC count. Entecavir controlled the viral replication but had no effect on the levels of transaminases which remained elevated to 1.3 to 2 X ULN. She remained HBsAg positive, HBeAg negative, anti-HBe positive with low HBV DNA 41 IU/ml when last seen in October 2022.
Comments: This young lady who acquired HBV infection probably from tattooing in 2015 was in an active replicative phase when she developed hypersplenism and liver cirrhosis from recurrent acute exacerbations of HVCS. Antiviral treatment did not prevent development of ascites and elevation of transaminases precipitated by operation.
# 3. A 162-03 K.S. M 60
HBsAg was detected in this 60 year old man on a routine test in 1997. Liver tests were normal and ultrasonography showed a normal liver with a calculus in gallbladder. This patient had intermittent mild leg swelling and recurrent urinary tract infection since 1979, had hematuria once in 1988 and dental care with filling done 6 X in 1996.
He attended this clinic in 2003 with acute jaundice. Blood tests showed serum bilirubin 14.0/11.2 mg %, ALT 40.6 X ULN, alkaline phosphatase 1.6 X ULN, protein 7.6g and albumin 3.2g; HBsAg positive, HBeAg negative, anti- HBe positive, anti-HBc positive; anti-HCV, anti-HAV IgM, anti-HEV IgM and HEV RNA negative; anti-HEV IgG positive, WBC count 9,500/cu mm, neutrophil 80% and platelet count 150,000/cu mm. A diagnosis of CHB non-replicative phase with non A-E hepatitis was made.
He suddenly developed ascites a month later. Ultrasonography showed ascites with free floating particles indicating presence of bacterial peritonitis, hepatomegaly with uniform increased echo-texture of the liver and prominent hepatic veins with mild splenomegaly. Inferior vena cava showed mild stenosis at the site of hepatic vein opening with thick posterior wall and a large recent thrombus. His blood tests showed WBC 6500/cu mm, neutrophil 70%, platelet 140,000/ cu mm, CRP positive, bilirubin 3.9/1.8mg%, ALT 12.6 X ULN and AP 1.9 X ULN with normal protein and albumin. He refused diagnostic paracentesis. A diagnosis of severe acute exacerbation of HVCS with ascites was made. Jaundice a month back was retrospectively diagnosed as mild acute exacerbation of HVCS. It was supported by mild neutrophil leukocytosis noted at that time. He was treated with oral antibiotic and furosemide. He became free of ascites with ALT 4 X ULN at 1 month and 1.8 X ULN at 3 month. He however, noticed increased pigmentation of the face. The US showed liver with uniform increased echo-texture and endoscopy detected grade I esophageal varices. Possibility of development of cirrhosis was considered. He was hesitant about liver biopsy. As he had gallstone which might act as a focus of infection he agreed for cholecystectomy. At operation the liver was found cirrhotic. Biopsy showed mixed nodular cirrhosis. He remained well with normal ALT. Two years later in July 2009 he developed minimal elevations of ALT 1.8 X ULN followed by recurrence of ascites with dilated superficial veins over abdomen. It responded to treatment with antibiotic and diuretic. He remained HBsAg positive, HBeAg negative, anti-HBe positive and his HBV DNA was 2,410 IU/ml, normal or minimal elevation of ALT elevation during follow up till December 2011 when he migrated to UK to live with his son who is settled there.
Comments: This patient with CHB in non-replicative phase with low HBV DNA had remained asymptomatic till he developed acute exacerbations of HVCS precipitated by urinary tract infection marked by jaundice followed a month later by ascites with rapid development of cirrhosis.
# 4. C100-06 NL 57M
This patient was detected HBsAg positive when he was admitted to a hospital in December 2003 with high fever and acute abdomen pain. Appendectomy was done. A month later he had recurrence of the symptoms and went to a hospital in Bangkok where he was operated for intestinal obstruction. Investigation showed neutrophil leukocytosis, mild elevation of transaminases, HBsAg positive, HBeAg negative, anti-HBe positive and HBV DNA < 500 copies/ml and normal liver in ultrasonography.
He attended this clinic in May 2006. US/CD examination showed presence of HVCS with localized mild stenosis of inferior vena cava at the site of hepatic vein opening and old organized thrombi along the posterior wall of the hepatic portion of the vein and normal looking liver. His CHB status remained stable with low HBV DNA. He gave history of two episodes of jaundice at 35 and 37 years of age and 4 episodes of minor illnesses with diarrhea or upper respiratory tract infection associated with mild neutrophil leukocytosis, CRP positive and mild elevation of ALT.
In October 2009 while he was in Blou, France he suddenly became unwell with sore throat, anorexia and marked fatigue. Investigation there showed elevation of ALT and AST 11 X ULN and 63.8 X ULN respectively. WBC and platelet counts were on low side with 70% Neutrophil; HBsAg positive, anti-HBc IgM negative, anti-HBe positive, anti-HAV IgM and anti-HCV negative. His ALT level was still high at about 6.8 X ULN three months later when he returned to Nepal. The WBC and platelet counts were on lower side. HBV DNA level was 4,818 IU/ml and check for auto-antibodies were negative. US/CD showed features of cirrhosis with evidence of hepatic venous outflow obstruction- dilated HV with obstruction to blood flow at the outlets. There were multiple stones in gallbladder. He received a course of antibiotic. ALT level declined to 1.2 X ULN and remained so. Liver biopsy was suggested to confirm cirrhosis. Instead he went to Bangkok to his previous hospital in February 2011 where cirrhosis was confirmed by MRI. The transaminases level was normal, HBeAg negative, anti HBe positive, but HBV DNA was high at 2,500,000 IU/ml. He was put on entecavir 0.5 mg daily with advice to continue it for indefinite period which he strictly adhered. Regular checkup showed that HBV DNA declined to < 150 IU/ml within 3 months and remained undetectable throughout. But he had 3 episodes of mild ALT elevations 2.9 X, 1.8 X and 5.5 X ULN in 2012, 2013 and 2014 associated with fever while still on entecavir and were treated with short course of antibiotic. Presence of cirrhosis was also confirmed by fibroscan.
Comments: This patient with CHB in non-replicative phase with very low HBV DNA and HVCS as comorbid condition had multiple episodes of ALT elevations associated with minor or severe illness. In 2009 after a prolonged episode of acute exacerbation of HVCS he developed cirrhosis probably from hepatic venous outflow obstruction. There was no change in his CHB status but developed a high level of HBV DNA once in 2010 which rapidly declined to undetectable levels with antiviral treatment. Antiviral treatment did not prevent the recurrence of ALT elevations.
# 5. C126-015 MR 66M
This 66 years man was detected on routine check minimal elevations of transaminases 1.2 X ULN and low counts of WBC and platelets when he attended an orthopedic clinic in March 2015 for shoulder pain. He was referred to a hematologist. Bone marrow biopsy was normal. Ultrasonography showed a feature of liver cirrhosis with mild splenomegaly, and was referred to a hospital. Cirrhosis was confirmed by fibroscan. Detailed iron, copper studies, tests for autoantibodies and anti-HCV were negative, but HBsAg was positive. Anti-HBc IgM and HBeAg were negative and anti-HBe positive with HBV DNA 15,421 IU/ml. Mild esophageal varices were detected and ligated.
He attended this clinic in September 2015. US/CD showed evidence of liver cirrhosis, mild splenomegaly and HVCS. IVC had localized stenosis at the site of hepatic vein opening with distal segment dilated with old organized thrombi of different ages along its posterior wall. Color Doppler showed obstruction to blood flow in inferior vena cava and hepatic veins and abnormal blood flow patterns in these veins. Family check showed all negative for HBsAg. His father had died from cirrhosis with ascites 23 years back and was detected HBsAg positive.
In the follow-up period from 2015 to 2022 he remained well with counts of WBC that varied from 2,300 to 4,200/cu mm and platelets from 10,000 to 140,000 and liver tests remained normal except for minimal elevations of ALT/AST. CHB status remained stable with low levels of HBV DNA.
Comments: This 66 year old man with liver cirrhosis and leukopenia and thrombocytopenia from hypersplenism probably acquired CHB at a young age from his father and is now in a non-replicative phase with very low HBV DNA. Development of hypersplenism and cirrhosis was consistent with the clinical course of HVCS.
# 6. (a) C178-012 SSJ, M 59 & (b) C 97-019 AJ, M 36
The 59 year old father was detected with HBsAg in July 2012 when he developed jaundice following a bout of prolonged diarrhea. Blood tests showed bilirubin 8.4/3.0 mg/dL, ALT/AST 9.7/18.4 X ULN, AP 1.2X ULN, serum protein 6.9g and albumin 2.8g; WBC 7900 with 66% neutrophil, CRP positive and blood culture grew Klebsiella organism, stool was loose with mucus and plenty of pus cells and RBC. His CHB profile showed HBeAg positive, anti-HBe negative with HBV DNA 48,666,666 IU/ml.
US/CD showed evidence of HVCS. The inferior vena cava had marked intimal thickening with mild stenosis at the site of hepatic vein opening with thick layers of old organized thrombi of different ages along the posterior wall. Color Doppler showed obstruction to blood flow at outlets of hepatic veins and inferior vena cava and abnormal blood flow pattern continuous instead of triphasic in these veins.
A diagnosis of CHB in the replicative phase with acute exacerbation of HVCS precipitated by Klebsiella infection was made. He was treated with oral ciprofloxacin. C-reactive protein, and bilirubin and ALT/AST returned to normal within a month. To prevent spread of infection to others he was put on entecavir which he took for 4 years. During follow-up for next 9 years he remained well with normal liver tests except for an episode of mild elevation of ALT with recurrence of diarrhea in December 2013. HBeAg became negative, anti-HBe positive with undetectable HBV DNA in December 2013 and had remained so up to December 2021.
Family check revealed that of his 5 sibs, 3 younger brothers were HBsAg positive, all in non-replicative phase with low HBV DNA levels. This patient probably acquired the infection by vertical transmission that resulted in prolonged replicative phase. Of his five children only the youngest son was HBsAg positive.
AJ, M 36
This youngest son of the above patient attended a local clinic at the of age 36 years with sudden development of ascites and leg edema that followed 2 months of recurrent fever from urinary tract infections. Splenomegaly was detected at ultrasonography. Blood test showed HBsAg positive; anti-HCV negative, HBeAg negative and HBV DNA was 25, 957 IU/ml. He had mild elevation of transaminases; WBC was 3300, neutrophil 83% and platelet 96,000. He was treated with diuretic and entecavir. His HBV DNA declined rapidly to undetectable level within two months but he remained very ill with ascites.
Two and half months later he attended this clinic. He was wasted with palpable spleen, moderate degree of ascites and bilateral pedal edema. US/CD showed evidence of hepatic venous outflow obstruction due to HVCS. Liver showed increased coarse echo-texture with rounded edge consistent with liver cirrhosis. He remained HBeAg negative, anti-HBe positive with undetectable HBV DNA. He improved on treatment with oral antibiotic and diuretics and was free of ascites with minimal elevation of ALT/AST < 2X ULN. He continued to have marked neutropenia and thrombocytopenia which failed to improve on treatment with filgrastim. Patient was unwilling to consider splenectomy. In December 2021 with recurrence of fever he had small bouts of blood vomiting which responded to medical treatment.
Comments: Of the five members of this family with CHB most of whom remained asymptomatic except above two patients one in replicative and another in non-replicative phase. Symptoms in these were due to bacterial infection. Son in non-replicative phase with very low HBV DNA but with severe acute exacerbation of HVCS with ascites developed cirrhosis rapidly but father with longer duration of CHB in replicative phase with very high HBV DNA had no cirrhosis.
# 7. 90-03 RK, 54 M
At 21 years age this patient suffered from prolonged chronic diarrhea and jaundice. At 39 years he had recurrence of diarrhea, fever, jaundice followed two months later by ascites. A few months later in November 1987 he attended CMC Hospital, Vellore, India where he was detected HBsAg positive, minimal elevation of ALT, mild cytopenia, mild hepatosplenomegaly with increased echo-texture of liver and grade III esophageal varices. A diagnosis of CHB related chronic liver disease was made. In 1989 he had 2 admissions in the same hospital with variceal bleeding and had sclerotherapy. In July 1990 he attended a hospital in Bangkok where splenectomy was done for severe hypersplenism. Presence of micronodular cirrhosis was confirmed at liver biopsy.
In May 2003 he attended this clinic with fever and US/CD examination showed presence of liver cirrhosis with prominent middle and left hepatic veins with intimal thickening and a membrane at the common ostia. IVC showed stenosis with complete obstruction by organized thrombi at the site of hepatic vein opening and dilatation of the distal segment that had organized thrombi of different ages along its posterior wall. Routine hematology and liver tests were normal but levels of ESR and C-reactive protein were elevated. Anti-HCV was negative HBsAg was positive, HBeAg was negative and anti-HBe positive. He improved on oral ofloxacin. At follow-up at 3 months he became HBsAg negative but HBV DNA was still positive. His HBV genotype was A.
Comments: The symptomatic clinical course and development of liver cirrhosis in this CHB patient was due to bacterial infection induced acute exacerbations of HVCS. He achieved spontaneous control of HBV infection at the age of 54 years.
CHB patients in Nepal developed liver cirrhosis but it was not related to the activity of viral replication or the duration of CHB infection. Two patients with very high HBV DNA developed liver cirrhosis at an early replicative phase almost within 1 year of acquiring the infection. One developed almost at the end of the non-replicative phase and the rest at variable periods in non-replicative phase. Liver cirrhosis developed rapidly following severe acute exacerbations with ascites as in case # 3, case 6 (b) and 7. Of the two CHB patients in a family in case # 6, father in replicative phase with very high HBV DNA remained asymptomatic for long period with occasional episode of bacterial infection with elevation of transaminases but his son in non-replicative phase with low HBV DNA who had prolonged and recurrent bacterial infection developed severe hypersplenism and ascites followed by development of liver cirrhosis. Antiviral therapy controlled viral replication except in a young patient in early replicative phase but it failed to control or prevent the occurrence of elevation of transaminases and ascites. The clinical courses of these patients - development of hypersplenism, recurrent elevations of the levels of transaminases or development of ascites precipitated by bacterial infection with US/CD evidence of HVOO was due to HVCS. These observations suggested development of symptoms and liver cirrhosis in CHB patients in a developing country was due to HVCS.
Patients with HVCS also had long silent courses but developed liver damage from HVOO. What is the mechanism of liver damage in HVOO? Unlike capillaries at other sites, hepatic sinusoids are highly porous because of the presence of some unique features such as absence of basement membrane and presence of holes or fenestrae arranged in sieve plates. This is of course designed to promote close contact between hepatocytes and the incoming blood from portal vein rich in nutrient and hormones and hepatic artery rich in oxygen. To prevent the loss of fluid from this highly porous vascular bed sinusoidal pressure is maintained very low. The pre to post sinusoidal pressure gradient is 49:1 compared to pre to post capillary in skeletal muscle of 4: 1. The maintenance of low sinusoidal pressure is vital for normal functioning of the hepatocytes. Occurrence of sinusoidal hypertension from HVOO resulted in increased passage of protein rich fluid and blood cells into the space of Disse and in between liver cell plates. To minimize the fluid loss into the space of Disse the sinusoidal hypertension induces reflex decrease in hepatic artery inflow and reverse flow in portal vein.34 The combined effect of these changes resulted in ischemic damage of liver cells around terminal hepatic veins.35 Ischemic liver damage stimulates stellate cells in the hepatic sinusoids to synthesize collagen36 which are deposited at the site of ischemic liver damage and along the sinusoidal wall. Loss of hepatocytes from ischemia fails to regain normal pattern and is replaced by the lesion of parenchymal extinction consisting of remnants of damaged tissue, elements of repair as fibrosis, neovascularization and arteriovenous shunting, which on resolution converts to fibrous septa.35 Hepatocytes at the edge of ischemic liver damage show regenerative activity with formation of hepatocellular nodules whose pressure results in curved shape of the fibrous septa. Presence of a curved shape of fibrous septa makes cirrhosis easily recognizable.35 Recurrent acute exacerbations with scattered focal areas of vascular damage going on for several years resulted in development of cirrhosis. Fibrosis is a dynamic process. Collagens deposited following activation of stellate cells are removed within a few weeks of cessation of injury.36 The evolution of fibrosis to cirrhosis is dependent on the perpetuation and resolution of underlying injury. Recurrent ischemic liver damage associated with recurrent episodes of acute exacerbation is considered critical for development of cirrhosis. When the thrombophlebitis formed in inferior vena cava at the site of hepatic vein ostia during acute exacerbation is large enough to block all hepatic vein ostia (Figure 2b) it result in severe sinusoidal hypertension with massive oozing of the fluid beyond the capacity of the hepatic lymph to drain resulting in ascites.37,38 Severe sinusoidal hypertension also results in baroreceptor mediated renal sodium retention that plays an important role in the sustenance of ascites.39 Patients with ascites developed cirrhosis rapidly within a few months.
Hepatic sinusoidal layer at the molecular level also plays an important role in the pathogenesis of cirrhosis. Hypoxic liver damage that follows sinusoidal hypertension is a potent stimulator for hepatocytes to synthesize vascular endothelial growth factor (VEGF).40 VEGF acts on VEGF receptors of sinusoidal endothelial cells. Its action on VEGF receptor-1 results in secretion of hepatocyte growth factor (HGF) and interleukin-6 that stimulate growth and proliferation of hepatocytes. And through its action on VEGF receptor-2 of the endothelial cell it promotes angiogenesis- formation of new blood vessels at the site of ischemic damage. These changes play an important role in the genesis of cirrhosis.
Cirrhosis was of micronodular type initially as in case # 2 (Figure 4a) but in patient with recurrent of acute exacerbations it converted to mixed nodular type as in case # 3. Continued prolonged or recurrent acute exacerbations resulted in conversion to macronodular type as was seen in a young boy reported earlier (Figure 4b).41 Thus though the common type of cirrhosis in diseases of HVOO is micronodular in HVCS with recurrent acute exacerbations it eventually evolved into macronodular type.
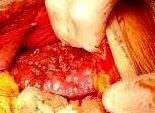
Figure 4a Micronodular cirrhosis seen during splenectomy for severe hypersplenism in 30 year old CHB patient in replicative phase Case # 2.
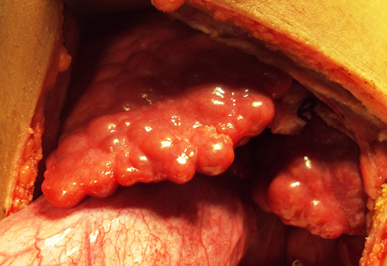
Figure 4b Macronodular cirrhosis seen in a young boy with recurrent acute exacerbation of hepatic vena cava syndrome during cholycystectomy for gallstone (reproduced with permission SM Shrestha, S Shrestha . Hepatic vena cava syndrome: a common cause of liver cirrhosis in children in Nepal, Trop Gastroenterol 2014;4:35:85-95).
Figure 4 Liver Cirrhosis in CHB patient with Hepatic Vena Cava Syndrome.
HVCS induced liver cirrhosis at an early stage showed some characteristic US/CD features that make it clinically recognizable.42 In liver cirrhosis due to other causes hepatic veins are often attenuated and not visible. HVCS induced cirrhosis may show dilated hepatic veins with evidence of HVOO, and occasional other findings as intimal thickening of intra-hepatic veins, edematous or thick gallbladder wall, and presence of calcified foci in the liver and a thick layer of peri-hepatitis around the liver due to past ascites with bacterial peritonitis (Figure 3b). Re-occurrence of jaundice or transaminases elevation or ascites in HVCS induced cirrhosis is frequently due to acute exacerbation and not due to hepatic decompensation (Figure 3b).42 Splenomegaly and development of esophageal varices are regarded as important features of advanced cirrhosis with portal hypertension in the West. HVCS patients with recurrent acute exacerbations developed splenomegaly with hematological features of hypersplenism long before development of cirrhosis, as was seen in some of the patients reported here. Sinusoidal hypertension during acute exacerbation resulted in backflow in portal vein resulting in portal hypertension with mild esophageal varices and dilatation of veins in the splenic hilum. Such patients with thrombocytopenia may have mild episodes of self-limiting variceal bleeding during acute exacerbations. Some rarely also develop hepatic encephalopathy before the development of liver cirrhosis due to bypassing the liver by splanchnic blood and returning to systemic circulation through dilated collaterals around the spleen. Development of these features should not be taken as signs of hepatic decompensation and an indication for liver transplantation in HVCS induced cirrhosis.
HVCS occurred the West and in Japan in the past.43–47 It has now become very rare in these areas.48 It is now reported mainly from some Asian and African countries, areas endemic for CHB, where the disease is recognized late in patients with membranous obstruction or after development of hepatocellular carcinoma.49–55 In many countries the disease is managed by vascular surgeons or interventional radiologists.50–52 Wang and his colleagues from Beijing in 2004 reported one of the largest series of 2564 patients 95% of whom were managed by surgery or interventional,52 indicating the common occurrence of the disease in China.
The clinical course of chronic hepatitis B infection alone in developing countries also otherwise is a long asymptomatic where the early replicative phase merges imperceptible into late non-replicative phase, each phase lasting for some decades and a few around 4th or 5th decades achieved the control of the infection with loss of HBsAg. HVCS also has a long asymptomatic clinical course because of the development of an extensive network of collaterals. Development of occasional symptoms and liver cirrhosis in CHB in Asian and African countries may be due to associated comorbid condition HVCS. Reports of recurrent mild elevation of transaminases and jaundice with development of splenomegaly in children with CHB in Taiwan and occurrence of leg edema, splenomegaly and hypersplenism in CHB patients that developed liver cirrhosis in Hong Kong suggested of the possible association of HVCS in these patients.56,57
It is suggested that the development of liver cirrhosis in chronic hepatitis B patients in developing countries is due to the presence of hepatic vena cava syndrome as a comorbid condition.
None.
This study has received no financial support.
The author has no conflict of interest to declare.

©2022 Shrestha. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.