Journal of
eISSN: 2574-9943


Conceptual Paper Volume 2 Issue 3
1Director, Center for Dermatology and Cosmetic Surgery, El Salvador
2Associated Professor, Center for Dermatology and Cosmetic Surgery, El Salvador
Correspondence: Enrique Hernández Pérez, Director, Center For Dermatology and Cosmetic Surgery, Villavicencio Plaza, Suite 3‒1 and 3‒2, San Salvador, El Salvador, Tel 503 2264 2240
Received: December 13, 2017 | Published: June 5, 2018
Citation: Pérez EH, Pérez JEH, Pérez MH. Skin cancer: an overview regarding treatment and its cosmetic repair. J Dermat Cosmetol. 2018;2(4):147-149. DOI: 10.15406/jdc.2018.02.00065
Skin malignancies are very common. Among them, the commonest one is the Basal Cell Carcinoma (BCC). Although there is many forms on it treatment, in our opinion nothing substitutes the surgical approach. In only one session is possible to remove the tumor and correct the defect, having many different forms of flaps or grafts, getting good results. For this procedure we propose the term Cosmetic Cutaneous Oncology.
Keywords: basal cell carcinoma, electrodessication, sun exposure, cryosurgery, clavulanic acid
Skin cancer continues being very common, Instead of continuous appeals to protect the skin from the solar damage; in our surgicenter we operate at least 3 to 4cases a week. We insist to our patients as verbally as in the screens of our waiting room, as and in brochures that genetics is the main and unavoidable cause of the problem, but sun exposure is the other causal problem. However, “the sunny beaches are so attractive…”
Basal cell carcinoma is the most frequently observed, and fortunately if the patient consults early, the cure is the rule; around 80% of all cutaneous malignancies are of this type.1 At the beginning of our formation as dermatologists we learned to treat basal cell carcinomas using curettage and electrodessication; then, in the decade of 80´s it was the turn of cryosurgery. At that moment we thought that we were in the right way. At the present time,1 however, our form of thinking is that among the multiple forms of treatment, our preferred, with no discussion, is the surgical one. Is the only one who allows us not only to remove the tumor, but to study in depth the margins around it? Even more: generally is possible to perform the tumor removal and its cosmetic repair at once, in only one session (Figures 1‒6).2‒5
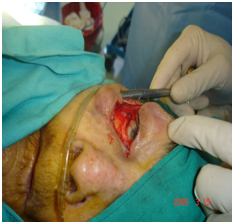
Figure 2 Tumor has been removed. The undermining is very wide, outlining an MUSTARDÉ flap, with the matter to avoid an ectropion.
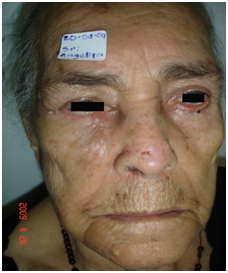
Figure 3 Two weeks later. Scar is barely noticeable. Compare with the senile ectropion at her left eyebrow.
Prior to the 60´s, Dermatologists were considered as the masters in clinical diagnosis, but the surgical removal was left in the hands of surgeons of other specialties, mostly plastic ones. Great dermatologists with a superb surgical skills burst in the field of dermatologic surgery and paved the way for hundreds of colleagues who, following their steps showed us the techniques most important to treat, first the skin tumors and then all the universe of Cosmetic surgery.4 Names of Ted Tromovitch, Sam Stegman, Perry Robins and Larry Field, among others, are reminded with special gratitude for all of those working in cutaneous surgery.
The first step is the microscopic confirmation of the diagnostic. A 3mm punch biopsy is a must. And those oriented to surgery have to know also at least the basis of the microscopic aspect of the tumors, as well as the form of staging with prognostic purposes.1,2,4 The general principles are the same for all surgical procedures. Given that most of the patients harboring these tumors are seniors, it is convenient be sure that doesn´t exist any problem with the use of local anesthesia: as the majority of tumors are placed on the face, we prefer always use epinephrine in the local anesthesia. Nevertheless, it is necessary never forget the interaction epinephrine‒beta blockers.1 No matter the amounts, such drug interaction could carry to lethal consequences.1,2,4 If the patient is using this drug (heart diseases, migraine), it must be stopped or changed for another one, previous consultation with the cardiologist, from who we demand a written statement. As local anesthesia, we use lidocaine plus epinephrine (0.5% and 1 in 400.000 respectively) below and around the tumor mass. In the rest of the area, we use tumescent anesthesia, prepared at the moment; in general 100cc at all is enough, even in large flaps.5‒9
With the matter to avoid unpleasant memories because of surgery, we operate most of our patients under IV sedation, administered by a certified anesthesiologist. Midazolam and Fentanyl are the commonest drugs. Also here we consider necessary for the surgeon to know the properties, doses, and side effects of the medications.1At the end, the surgeon is the captain of the ship, being certainly responsible of the end results. Preoperatory antibiotic, yes or no? Discussion regarding its value in clean surgeries is certainly open, but everybody use it. We prefer oral amoxicillin plus clavulanic acid starting one day before and keep along 5days at all. In case of allergy, we change to ceftriaxone 1gIM 1hour before.
Remotion of the tumorThe intention is the removal of the tumor and its cosmetic repair in only one session. And that is possible in most of the cases.1,10 The forms to accomplish satisfactorily both aims are open for any surgeon owning enough skillness and creative mind. Skillness really is increased with practice and escapes from the aim of this short paper. The following photographs are showed only to illustrate some flaps, in the manner of a sample, which is possible to reach in a private surgicenter. At the end, we may coin the term Cosmetic Cutaneous Oncology.
None
The authors declared that there are no conflicts of interest.

©2018 Pérez, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.
 May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.
May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.