Journal of
eISSN: 2574-9943


Research Article Volume 2 Issue 4
1Departmnet of Pharmacy and Biochemistry, Potiguar University (UNP), Brazil
2Department of Biotechnology, University Center of Rio Grande do Norte (UNIRN), Brazil
3Department of Physiotherapy, University Center of Rio Grande do Norte (UNIRN), Brazil
4Department of Health Sciences, Potiguar University, Brazil
5Physiotherapy, Mauricio de Nassau College (UNINASSAU), Brazil
6Department of Dermatology, Brazilian Dermatology Society, Brazil
7Department of Health and Medical Services Dubai, Dermatology Specialist, UAEs
Correspondence: Patrícia Froes-Meyer, BS in Pharmacy and Biochemistry, Lecturer-Potiguar University (UNP), 59054-180 Natal, RN, Brazil
Received: February 19, 2018 | Published: July 25, 2018
Citation: Patrícia F, Eneida MC, Nayre BMD, et al. Analysis of a protocol for the treatment of buttocks folliculitis. J Dermat Cosmetol. 2018;2(4):185-189. DOI: 10.15406/jdc.2018.02.00074
Background: The folliculitis occurs when there is infection of the hair follicles, caused by bacteria such as Staphylococcus aureus, with origin in the hair and the sebum, which are fundamental for the skin’s natural protection. Among the treatment resources, the phototherapy is in evidence, as it is cited in literature as an efficient wound treatment method.
Objective: To check the effects of a protocol treatment for folliculitis pustules and lesions that associates phototherapy with active principles from cosmetics. The authors attempted to verify if a simple protocol with such association may contribute in the resolution of this pathology.
Methods: The sample consisted of 10 female volunteers, aged between 15 and 45years old. The instruments of measurement and data collection used in the research were an adapted questionnaire, a photographic camera. The protocol sequencing was the following: hygienization and exfoliation; Blue LED application; invisible infrared laser application; use of antifolliculitis cream. The volunteers were submitted to four sessions of forty minutes each, once a week.
Results: In the photographic analysis, there was a decrease in size of some pustular lesionsand the disappearance of others. There was an overall appearance improvement of 42.42% according to lesion count and photographic analyses results.
Conclusion: A reduction in the number of lesions was observed, suggesting that the proposed protocol could be a treatment option for folliculitis of mechanical origin.
Keywords: folliculitis, laser, phototherapy, healing, cosmetics, physiotherapy
LLLT, low intensity laser therapy; SEM, scan electron microscopy;; SPSS, statistical package for the social science; ATP, adenosine triphosphate; GM-CSF, granulocyte macrophage conoly stimulating factor
One of the most important characteristics of the folliculitis is its marked chronicity. The treatment of folliculitis represents a great challenge, with numerous relapses and maintenance of its activity for long period.1 Combination therapies with antiseptic lotions, long-term systemic antibiotics, topical antibiotics and prevention of risk factors are essential to control the disorder. However, it is generally refractory to most forms of therapy and its progression is difficult to halt.2 A promising phototherapy option for folliculitis treatment, but still uncommon in clinical practice, is the LED (light emitting diode) which is semiconductor diodes. The LED emits light of wavelength that range from 450nm (blue) to 940nm (infrared). The photostimulation resulting from these light acts on the cell in permeability, stimulating the mitochondria, the ATP synthesis and the production proteins such as collagen and elastin. This light also acts as an antimicrobial and an anti-inflammatory agent, depending on the applied wavelength and, therefore, the LEDs are indicated for the treatment of several inflammatory affections.33 Low intensity laser therapy (LLLT) has been widely used in the conditions of scarring processes, for faster healing of wounds, as well as for overall scar condition improvement.4 The low-power laser has biostimulating properties that accelerate the healing of biological tissues, and its wavelength determines its position in the spectrum of electromagnetic radiation and the interaction with the irradiated tissue.5 Shun Lee et al.6 also say that infrared laser may expand the lacunar system by creating temporary channels through the corneal extract, as evidenced by scan electron microscopy (SEM) investigations. Through these channels, it is possible to facilitate the penetration of active principles in the skin.
The objective of this research is to verify the effects of a treatment protocol for folliculitis that associates phototherapy and active principles. It is sought to verify if a simple protocol with this association may contribute to the resolution of this pathology. Folliculitis, like many dermatological disorders, may cause discomfort to the patient and may lead to psychosocial imbalances, such as anxiety and low self-esteem, impairing the establishment of healthy relationships, contributing to social isolation, making it even more difficult to seek help.7 Research, therefore, is a justified means of prevention and treatment.
This study is characterized as an experimental, descriptive and comparative research. The sample consisted of 10 female volunteers. All subjects were submitted to the folliculitis treatment protocol. Among the inclusion criteria, volunteer subjects presented folliculitis in the gluteal region, aged between 15 and 45 with capacity for understanding and preserved local sensibility. The exclusion criteria were applied to volunteers who presented allergy to the cosmetics included in the protocol, those who did not provide timely treatment and those who were absent for more than three sessions. The data collection and measuring instruments used in the research were: an adapted questionnaire addressing the following topics: identification, anamnesis, and fifteen specific questions about the effects that folliculitis causes physically and psychologically, in addition to including the Global Aesthetic Improvement Scale (GAIS),8 described in Table 1, applied at the end of treatment, which measures the level of satisfaction and improvement of the lesions through the opinion of the volunteers, as well as a Canon 60DS model camera , Ultrasonic peeling Derma F, device of phototherapy ECCO®: blue LED light with wavelength 450nm and invisible infrared laser with wavelength of 940nm.
Degree |
Description |
Exceptional Improvement |
Excellent corrective result |
Very improved patient |
Marked improvement of the appearance, but not completely optimal |
Improved patient |
Improvement of the appearance, better compared with the initial condition, but a touch up is advised |
Unaltered patient |
The appearance substantially remains the same compared with the original condition |
Worsened patient |
The appearance has worsened compared with the original condition |
Table 1 Global aesthetic improvement scale (gais)
The cosmetics used were: an apricot seed exfoliating gel, to accelerate cell renewal and to improve blood circulation,9 an antifolliculitis cream with ammonium lactate, for skin thickening with compaction of the stratum corneum and desquamation control with skin barrier functions,10 melaleuca oil, bactericidal and antifungal action against various human pathogens,11 allantoin, used for its healing properties such as keratolytic, moisturizing, epithelizing12 and WonderlightTM (Sederma, Le Perray-en-Yvelines, France), A depigmenting substance that fights dendritogenesis, responsible for the melanin distribution and deepening in the skin, blocking the release of GM-CSF (Granulocyte Macrophage Conoly Stimulating Factor).13 Specific software (CorelDRAW x8, Corel Corporation, Ottawa, Canada) was used to outline the 10cm² treatment area in the gluteal region photos and to standardize lesion count. The protocol was developed after the approval of the Ethics Committee of the Potiguar University. After subjects’ selection, the volunteers received guidelines regarding the protocol and treatment and signed the Informed Consent Form, in concurrence. Patients were also asked to sign a photography consent form so that the figures could be published in articles. Their identity was carefully preserved and the questionnaire with inquiries related to folliculitis was answered. The camera used was the same in all shooting sessions. Placed on a tripod at a height of 76cm from the ground and 1.23m from the volunteer, the records were performed on the 1st and 3rd sessions and one week after the 4th session.
After the first photographic record, the volunteer was placed in a ventral decubitus, for protocol treatment with procedures as follows: Manual hygienization of the treated area with apricot seed exfoliant gel; ultrasonic peeling application; blue LED application (4Joules/40s; invisible infrared laser application (32s); antifolliculitis cream with ammonium lactate, melaleuca oil and WonderlightTM. The selected volunteers were submitted to four full protocol 40-min-sessions, once a week. Data analysis was performed using CorelDRAW x8. The three photos obtained from each volunteer during and after treatment were submitted to outline demarcation of a 10cm² areas in the gluteal region, left hemibody, corresponding to the treated area, selecting each folliculitis lesion contained in this space, thus quantifying the total number of lesions. Statistical analysis was performed using the Statistical Package for the Social Science (SPSS) (version 22.0). Descriptive statistics were presented in the form of tables and graphs. Data were checked for normality by the Kolmogorov-Smirnov test. When the normality of the data was verified, the following test was used: T test paired to compare the values between the groups. The level of significance of the results obtained was 95% with p <0.05).
Among the volunteers, only 80% started treatment, 20% were only submitted to the evaluation, and were disregarded due to absence for more than three sessions. The final sample consisted of eight subjects with an average of 29.5years of age. The volunteers answered questions about how long the folliculitis has been present, (average of 5years and 1month); and for how long the subjects remain seated, (average of 3h 42min). In addition to the questionnaire, the volunteers were also asked if they underwent any previous treatment. 60% answered NO and 40% answered YES. Out of the 40%, only 10% could inform what treatment was applied and what medications were used, and 40% reported lesions recurrence after end of treatment. Within the evaluated group, 100% answered the questionnaire; 100% had their first photo taken and 80% completed the treatment taking all the three scheduled photos for data analysis and comparison.
Photographic analysis
Figures 1A-1C were obtained at the 1st and 3rd sessions and one week after the 4th session, corresponding to the initial evaluation, revaluation and final evaluation, respectively. It was possible to observe the change that occurred during and after the proposed protocol sessions, resulting in visible appearance improvement and lesion reduction. The initial evaluation photos presented a large quantity of follicular pustules and some presented hyperchromia. During the treatment, a decrease in the follicular pustules diameter was observed, as well as the absence of some previously registered lesions, as shown in Figure 2. This result was also observed with other volunteers who attended all the 4 sessions. Bleaching of the lesions pigmentation in the volunteers who presented hyperchromia when compared to the data collected in the initial and final evaluation. In summary, when analyzing the figures recorded before, during and after treatment, improvement of skin condition and a decrease in the number of pustules were evident. However, volunteers who abstained from treatment for more than one session did not show significant change in the appearance of folliculitis.
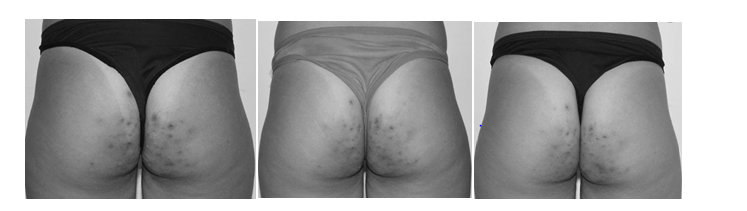
Figure 1 (A) Initial evaluation–Date: 02/01/2017; (B) revaluation- Date: 02/15/2017; (C) Final evaluation- Date: 03/01/2017.
Evaluation according to the CorelDRAW x8 program
After outlining the treated area and counting the number of folliculitis pustules within the analyzed 10cm²-area, as shown in Figure 2, the degree of improvement levels was established as follows: 100/X=NF1/NF3, in which x is the improvement rate in percentages, NF1 is the pustules count in Figure 1, and NF3 is the pustules count in Figure 1A. The mean improvement percentage value was 48.42%. Volunteers 2, 4, 5 and 6 had rates greater than 50%, showing a progressive reduction in the amount of folliculitis from the first to the last count. Volunteers 3 and 8 maintained the result from the first count until the end of the treatment. Volunteer 7 presented an increase in the number of lesions after the first session, which may be justified by the failure to comply with the weekly treatment as proposed, but nevertheless, it obtained a significant evolution at the end of the treatment seen in Table 2.
Lesion count |
||||
Volunteer |
Figure 1 |
Figure 2 |
Figure 3 |
Improvement rate (%) |
1 |
28 |
24 |
21 |
25 |
2 |
39 |
29 |
13 |
67 |
3 |
20 |
15 |
15 |
25 |
4 |
19 |
18 |
7 |
63 |
5 |
13 |
9 |
5 |
61 |
6 |
19 |
16 |
8 |
57 |
7 |
36 |
50 |
21 |
41 |
8 |
17 |
36 |
36 |
- |
Table 2 Number of lesions and improvement rate
Assessment according to statistical analysis
Figure 3 shows the statistical difference in the number of lesions found in the three evaluations, and evidences statistically significant difference when comparing the reevaluation numbers with the first evaluation, apart from finding a relevant statistical difference when comparing first and last evaluation numbers. Table 3 describes the mean and standard deviation in the quantity of folliculitis lesions identified in the photos, noting that there was an increase in mean and standard deviation between the first evaluation and the reevaluation, due to noncompliance of the weekly protocol by 2 volunteers, with an increase in the number of folliculitis lesions in both cases. These facts caused the mean values to deviate from the tendency evidenced with by most of the volunteers. Regarding the result, there was 50% reduction in the mean number of folliculitis pustules between the first and the last evaluation, as well as data convergence, observed in the standard deviation decrease. This indicates that the mean is less dispersed and more reliable. The accuracy of the data can be verified in Table 4, where the reduction of the attribute (p) may be extracted, with more tangible data, going from 0.03 (3%) in the revaluation to 0.005 (0.5%) in the final evaluation.
|
MD |
SD |
Initial evaluation |
23,87 |
9,41 |
Revaluation |
24,62 |
13,35 |
Final evaluation |
12,5 |
7,09 |
Table 3 Mean and standard deviation of the identified folliculitis lesions quantity
Comparison |
p value |
Initial evaluation X Revaluation |
0,084 |
Revaluation |
0,03 |
Final evaluation |
0,005 |
Table 4 p values on each evaluation
Global Aesthetic Improvement Scale (GAIS)
At the end of the treatment, the GAIS scale was applied to evaluate the level of satisfaction after the proposed protocol application. The results show that out of eight (8) volunteers, equivalent to 100% of the patients who completed the treatment, five (5) of them, that is, 62.5% rated their response to treatment as 2, two (2) volunteers (25%) rated treatment satisfaction as 1, and one (1) volunteer (12.5%) ranked satisfaction level as -1.
The folliculitis caused by S. aureus may be superficial or deep. The surface may not be primarily of infectious origin, and they may also originate in physical or chemical traumas.14 Table 2 shows that the volunteers remain seated for approximately 4hours/day, coinciding with the author’s citation1,2about the physical trauma-originated folliculitis, as the contact of the seat with the gluteal region generates friction. Lesions and pustules resulting from folliculitis may be chronic, usually painless or slightly painful.15 In the findings described in Table 1, lesion chronicity was reported by volunteers and registered for analysis, and they pointed out an average chronicity period of 5years and 1month. Several studies on the bactericidal effect of visible light have been carried out, most dealing with blue light (400-500nm) for its broad action spectrum characteristics, reaching several pathogens.16 The blue LED has a wavelength that is very close to the one of the ultraviolet light’s, showing similar bactericidal action, and today, it is a substitute for the ultraviolet treatment,17 which corroborates with the findings in the photographic analysis in which a decrease in the quantity of pustules was observed, confirming the blue LED’s bactericidal action. Fortuny et al.,18 also reports that LED light also acts as an antimicrobial and anti-inflammatory agent, so it is indicated for various inflammatory conditions.
By the end of the quantitative analysis, a significant reduction in the number of lesions was observed, with p<0.005, in comparison to the initial and the final results. It is probable that the phototherapy and cosmetic associated treatment contributed to this positive response. Rocha Junior et al.,19 cites that when the laser light interacts with cells and tissues at the appropriate dose, certain cellular functions may be stimulated, occurring lymphocyte stimulation, mast cell activation, increased mitochondrial ATP production, and proliferation of several types of cells, thus promoting anti-inflammatory effects and inducing the healing process. The healing of the area that suffers mechanical trauma is fundamental for the prevention of folliculitis processes. In addition, the infrared laser at 940nm has its action related to the drug delivery system and in this study, the authors aimed to associate a previous formulation of antifolliculitis cream composed of ammonium lactate, Melaleuca oil, allantoin and WonderlightTM with phototherapy, as according to Whelan et al.,20 the use of LED therapy alone or in combination greatly accelerates the wound healing process.6
Hyperchromic affections of epidermal origin present as brown spots (Hyperchromias proper) that result from increased melanin in the epidermis due to increased activity and number of secretory melanocytes and increase in the number of melanosomes.21 During treatment, satisfactory results were observed regarding the healing process of the lesions, with improvement in pigmentation. It is probable that the uses of WonderlightTM, combined with the skin preparation with peeling, reduces skin sweeping and facilitate the penetration of active principles with the aid of infrared laser.
The results were more effective with the volunteers who followed the treatment weekly, without a long interval from one session to another, proving the importance discipline and steadiness with agreed treatment protocols.
The limitations of this study are the scarce literature on folliculitis, the difficulty in finding volunteers willing to undergo treatment and their difficulty to follow continued homecare procedures, with consequent sample loss, being an obstacle to the data statistical analysis. Thus, a study with similar methodology is suggested; however, with a larger sample more than 4sessions for perennial results. The interest in the analysis of other types of folliculitis that may be treated with the same or other sequential protocols is also incentivized. A follow-up of months and years should be considered for a better evaluation of the effect of this treatment regarding the use of medications.
In conclusion, the effects of the use of the 450nm LED and 940nm infrared laser, associated to the use of specific cosmetics, promoted a change in lesion pigmentation, proven with photo comparison and through the analysis of the level of satisfaction of the volunteers. Statistical analysis showed a reduction in the number of lesions, suggesting that the proposed protocol could be a treatment option for folliculitis of mechanical origin.
The authors declare that they participated in the design, analysis of results and contributed effectively in carrying out this research and make public responsibility for its contents, in which any affiliations or financial agreements between authors and companies that may be interested in publishing this article have been not omitted.
None
Authors declares that there is no conflict of interest.

©2018 Patrícia, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.
 May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.
May is universally acknowledged as Skin Cancer Awareness Month, a pivotal
period to spotlight its prevalence, contributing factors, and the essential role of safeguarding skin from UV exposure.
This year’s theme, “ExposetheTruth #SharetheFacts,” emphasizes the individual burden of this widespread condition and
the urgency for heightened vigilance and preventive action. In alignment with this initiative, the Journal of Dermatology
& Cosmetology (JDC) encourages scholars to disseminate knowledge, raise awareness, and educate people on effective strategies
to reduce risk. To encourage timely submissions, JDC is pleased to extend a 30% reduction on APC fees for all manuscripts
submitted during May 2026.