International Journal of
eISSN: 2574-8084


Case Report Volume 10 Issue 5
1Department of General Surgery, Hospital Ángeles Lomas, México
2General physician, Hospital Ángeles Lomas, México
Correspondence: Alejandro Weber Sánchez, Vialidad de la Barranca s/n C410, Valle de las Palmas, Huixquilucan, 52763, Estado de México, México, Tel 52469527
Received: December 15, 2023 | Published: December 28, 2023
Citation: Weber-Sánchez A, Weber-Álvarez P. Resection of a giant gastrointestinal stromal tumor and subsequent gastric reconstruction. Int J Radiol Radiat Ther. 2023;10(5):135-137. DOI: 10.15406/ijrrt.2023.10.00369
Gastrointestinal stromal tumors (GIST) are the most common mesenchymal neoplasms of the digestive tract (80%). The stomach is the most commonly affected organ. Complete resection of the tumor is the only curative treatment. The size and number of mitoses are parameters to determine the prognosis and the use of adjuvant therapies. Although sometimes the GIST is giant it should be completely resected and if possible the stomach reconstructed to preserve function and quality of life.
Keywords: GIST, gastrointestinal stromal tumors, gastric tumors, resection, gastric reconstruction
Gastrointestinal stromal tumors (GIST) are uncommon, 0.1–3% of all gastrointestinal malignancies, yet are the most common mesenchymal tumors of the digestive tract.
The stomach is affected in 40-60% of cases. Complete tumor resection with negative margins is the standard treatment for these tumors. Size is important to determine surgical conduct, functionality, and prognosis.
A 59-year-old male patient with a history of Mediterranean anemia. He started a month earlier with crampy abdominal pain 5/10, and distension, accompanied by hiccups, burps, and early satiety. On physical examination, the abdomen was distended, not painful, with dullness on percussion.
The ultrasound showed a large solid abdominal mass in the upper abdomen. The computed tomography reported a solid tumor with dimensions of 223.1mm X 142.9mm with peripheral vascularity, central necrotic areas, and displacement of splenic artery and biliary sludge. (Figure 1) The endoscopy revealed an ulcerated tumor that extended from the cardia to the posterior part of the upper third of the body of the stomach. The biopsy confirmed gastrointestinal stromal tumor (GIST). Therefore, informed consent was obtained for the surgical procedure and he was scheduled for tumor resection and cholecystectomy.
During surgery, a subserous, large exophytic tumor was found, affecting the posterior gastric wall of the body and fundus in the upper third. The tumor growth was mainly outside the gastric wall, and the bottom of the mass was closely adhered to the upper and anterior border of the pancreas and the spleen, so a splenectomy had to be performed. The tumor could be completely removed, (Figures 2&3) resected along with the gastric wall, preserving gastric wall edges without apparent tumor throughout the periphery. After the gastric reconstruction, a gallbladder resection was performed while the histopathologic report of the borders of the gastric wall was available. The histopathological report of the edges of the tumor in the gastric wall was reported as margins free of tumor. Therefore, despite the large resection, a gastric tube was constructed in the upper third of the stomach, being able to preserve part of the gastric body and the antrum.
The esophago-gastroduodenal series taken a week after surgery (Figure 4) showed acceptable reconstruction of the stomach, without leaks, and adequate passage of contrast media.
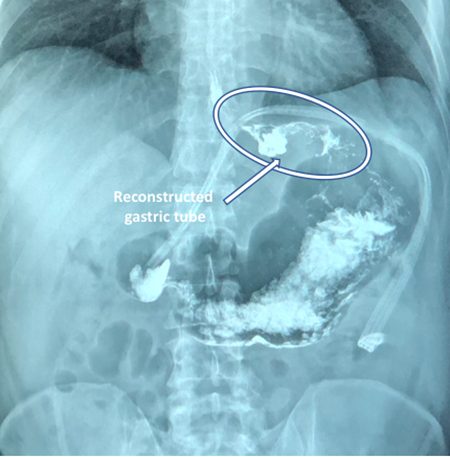
Figure 4 Esophago-gastroduodenal series taken a week after surgery with acceptable gastric reconstruction forming an upper gastric tube.
The patient's postoperative course was uneventful, and he was discharged being able to tolerate the oral route. Currently, he is under chemotherapy with Imatinib. We obtained his written consent to publish his case and images and the approval by the Hospital Review Board.
GISTs constitute 1% of all gastrointestinal neoplasms and are the most common mesenchymal tumors of the gastrointestinal tract.1 Its origin comes from Cajal cells. Its incidence is 4 to 10 cases per million inhabitants per year, although a twofold amount has been reported in Korea.2
They generally occur in people over fifty, with a slight male predominance.3 They are usually solitary, well-circumscribed masses that may present intra or extraluminal parietal growth or mixed growth. Sixty percent are usually submucosal.4
These tumors can be found in any part of the gastrointestinal tract; however, their most frequent location is the stomach in 40 to 60% of cases, mainly in the body, followed by tumors in the small bowel.3
Their size varies between 2 to 10cm5-7, the largest GIST reported was 49cm.8 Large masses usually have an exophytic growth towards the lumen, with mucosa ulceration in 20 to 30% of cases. They can also protrude outside the serosa with a large extra parietal component, as the case of this patient, who was asymptomatic up to a month before surgery.9 There is no consensus on what is considered a giant gastric tumor, however, the size of most of the tumors reported in this way exceeds 20cm, such as the case we report here.
The clinical presentation may be asymptomatic in the early stages of the disease. In many cases, they are radiological or endoscopic findings. Its clinical manifestations are related to the location of the tumor.10 Symptoms may be vague, such as weight loss, vomiting or abdominal pain, anemia, or digestive tract bleeding. In advanced stages, gastrointestinal bleeding is the most common presentation (86%) due to ulceration of the mucosa, followed by anemia due to this same cause.11,12 However, GISTs are a rare cause of massive gastrointestinal bleeding less than one percent.13
Contrast-enhanced computed tomography (CT) and magnetic resonance imaging (MRI) are the methods of choice for the characterization of these tumors; large ones usually show growth towards the lumen, with mucosa ulceration in 20-30% of cases. They can also protrude the serosa with a large extra parietal component, making it difficult to determine the digestive origin in imaging techniques. Sometimes it is difficult with CT to differentiate between tumor adherence or involvement of neighboring organs, or to detect metastases smaller than 2 cm.
Many GIST tumors have a benign behavior, however, all tumors larger than 1 cm can be malignant.10 Findings that suggest malignancy are extra gastric location, tumors larger than 5cm, and a high mitotic index in the histopathological study. The percentage of metastases is generally low at the time of diagnosis: the liver, spleen, and regional lymph nodes are the most common locations. Metastasis to lymph nodes occurs in less than 10% of the cases, so, extensive lymphadenectomy is usually not required.13 The standard treatment is complete surgical resection of the tumor with negative margins.14 If adjacent organs are affected, an en-bloc resection should be performed. For large tumors, or with metastatic disease, adjuvant therapies are used to prevent recurrence.
In this report, we present a patient with a giant gastric GIST tumor. It is evident that the larger the tumor, the more difficult it is to remove. The location of the tumor can also make surgery difficult, as in this case, since it was located on the posterior wall of the body and gastric fundus, closely adhered to adjacent structures such as the pancreas and large blood vessels. Therefore, in addition to tumor removal, the best possible reconstruction must be planned for the patient's function and quality of life.
Giant gastric GIST tumors are rare tumors. Imaging studies can help plan resection and subsequent reconstruction to preserve function and quality of life.
None.
Authors declare that there is no conflicts of interest.

©2023 Weber-Sánchez, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.