International Journal of
eISSN: 2574-8084


Clinical Paper Volume 9 Issue 5
1Master of Science, 2nd Degree Specialist in Orthopedics and Traumatology, Assistant Professor, General Teaching Hospital “Dr. Juan Bruno Zayas Alfonso”, Cuba
2First Degree Specialist in Anesthesiology and Resuscitation, “Dr. Juan Bruno Zayas Alfonso” General Teaching Hospital, Cuba
Correspondence: Luis Enrique Montoya Cardero, Hospital General Docente “Dr. Juan Bruno Zayas Alfonso”, avenida Cebreco, km 1 ½, reparto Pastorita, Santiago de Cuba, Cuba
Received: November 02, 2022 | Published: November 25, 2022
Citation: Cardero LEM, Piñeiro ML. Cutting disc injury. Int J Radiol Radiat Ther. 2022;9(5):148-151. DOI: 10.15406/ijrrt.2022.09.00340
The clinical case is described of a 46-year-old patient, attended at the Traumatology office of the Centro de Diagnóstico Integral de Chuao, Baruta municipality, Miranda state, Venezuela, who suffered a right leg injury as a result of an accident at the mechanic workshop where he worked. He went for consultation a week after the accident with a compartment syndrome of the anteroexternal region of the leg. A wound with stitches in the affected area attracted attention. Radiographic studies confirmed the presence of a large shear disc fragment. The fragment was removed under regional anesthesia and after 6 weeks she returned to her usual work activities.
Keywords: shear disc, compartment syndrome, regional anesthesia
The aggressive action of cutting discs is directly related to professional malpractice, especially the use of products without quality certification or of machines that are not suitable for the type of disc, since each cutting machine has a diameter limit allowed for the disc; another cause is the deterioration of the disc components because they have passed their expiration date; the poor adjustment of the disc in the machine, as well as the inexperience and lack of training of the operator also have an influence. In the worst case, the operator or other workers can be seriously injured, depending on the size of the disc, its composition, speed, distance and the characteristics of the tissues of the human target where it impacts, so it is essential for the operator to wear personal protective equipment, which should consist of appropriate clothing, a mask, eye protection, hearing protection and protective gloves.1
The anterior region of the leg is bounded medially by the anterior border of the tibia and laterally by a groove that separates the peroneal muscles from the soleus muscle, below the fascia the anterior intermuscular septum of the leg, divides this anterior region into two cells, one anterior and one lateral. The anterior cell contains 4 muscles that fundamentally dorsiflex the foot (tibialis anterior, extensor hallucis longus, extensor digitorum longus, and peroneus anterior or third peroneus) and the vasculonervous bundle formed by the anterior tibial artery that continues in the foot with the pedia artery, its satellite veins, the lymphatic vessels and the deep peroneal nerve that also innervates the first interosseous space. The lateral cell is constituted by the peroneus longus and brevis muscles, by the termination of the common peroneal nerve and the superficial peroneal nerve.2,3
Compartment syndrome (CS) was discovered by Richard von Volkmann, although the first to describe it was Hamilton in 1850.3 It is defined as an increase in pressure in a closed osteofibrous space, which can cause, depending on the intensity of the trauma, certain local anatomical characteristics and the time of diagnosis, a variety of symptoms depending on the intensity of the trauma, certain local anatomical characteristics and the time of diagnosis, a varied symptomatology that depends on the elevation of intracompartmental pressure values, ranging from a local microcirculation disorder that causes ischemia,4 neuromuscular dysfunction and, if not treated promptly, loss of the limb, to endangering the patient's life due to multiorgan failure.5
It affects about 3.1 patients per 100,000 inhabitants in the western world, with a predominance of men over women 10:1, as well as young patients, with 32 years being the average age of presentation for the general population, 30 years for men and 44 years for women. Male patients under 35 years of age have a higher prevalence due to greater muscle density and compact muscle compartments, in addition to more traumatic professions and behaviors.4,6,7
The most frequent location is in the leg due to the exposure of this region to trauma, it can manifest itself immediately after the trauma or hours or days later. The anterior compartment of the leg is small and not very elastic, which makes it more prone to present an increase in intracompartmental pressure.3,5
Depending on the clinical severity, a distinction is made between incipient compartment syndrome (ICS) and overt compartment syndrome (OCS). The former is distinguished by a virtually intact microcirculation without the presence of neuromuscular dysfunction and is characterized by severe pain that is difficult to control with medication. The pathognomonic sign is the pain produced by muscle contraction due to the reduction of the fascial space, the consistency of the compartment varies from tense-elastic to hard as a stone, while the second presents the symptoms mentioned above, in addition to a neurological deficiency with alterations in sensitivity and loss of motor functions5. Other authors consider that this syndrome has two forms of presentation, an acute and a chronic form, the acute form is severe and occurs as a result of trauma, which in many cases requires decompressive fasciotomies to avoid necrosis of muscles and nerves.3
It is very objective and practical to classify it as acute, subacute and recurrent; In acute CS, the symptoms are compatible with an increase in compartment pressure that does not resolve by itself; subacute CS, although it does not have the same clinical characteristics as acute CS, but also leads to the typical sequela (Volkmann's ischemic contracture); and recurrent CS occurs in sports patients and patients with certain professions while they are engaged in physical activity, with muscle weakness and pain, but at rest they are asymptomatic; compartment pressure at rest may be elevated due to hypertrophy of the muscle mass.8
The muscles of the extremities are distributed in compact compartments, delimited by fasciae, connective tissue septa and bony structures, these compartments constitute a closed system with little tolerance to pressure increases, through which blood vessels, lymphatics and nerves pass. The leg with its 4 compartments (anterior, lateral, superficial posterior and deep posterior) is the most affected anatomical region, the anterior being the most frequent,4 Rorabeck describes a fifth compartment formed by the posterior tibial.3
Matsen and Krugmire described the capillary arterio-venous gradient theory, which considers the normal intracompartmental pressure to be 10 mm/hg and suggests that a significant increase in intracompartmental pressure, caused by an increase in intracompartmental volume (hemorrhage or edema) or by a decrease in compartment volume (tight bandages or splints), causes an increase in intracompartmental pressure, causes an increase in intraluminal venous pressure and alters the normal arterial-venous pressure gradient at the capillary level, affecting the blood flow that usually flows in the microcirculation from arterioles to venules and from higher to lower pressure, causing a decrease in the tissue supply of oxygenated arterial blood and the impossibility of drainage of deoxygenated venous blood. The subsequent elevation of hydrostatic pressure causes an increase in capillary permeability, leakage of plasma into the interstitium and tissue edema, which steadily increases compartment pressure. This vicious circle in which pressure rises as capillary flow deteriorates eventually collapses lymphatic vessels and finally compromises arterial blood supply, culminating in cellular anoxia and irreversible necrosis. The intracompartmental pressure capable of compromising normal tissue perfusion is between 10 to 30 mm/hg, relatively close to the diastolic pressure and oxygenation is affected to the extent that it approaches or exceeds the mean arterial pressure, so the development of compartment syndrome depends not only on the pressure of the muscle compartment, but also on the systemic blood pressure and because of this hypotensive patients, such as polytraumatized patients, are at greater risk of developing it.3
Longer periods of ischemia imply greater morbidity and mortality for the patient; reversible nervous alterations appear after 30 minutes and muscular alterations after 2 to 4 hours, while irreversible changes at the muscular level appear after 6 hours and nervous alterations after 12 hours. This short period of time poses a diagnostic challenge for the treating physicians.3
Trauma is the main etiological factor, particularly when associated with fractures 69% and soft tissue injury is the second most frequent etiology 23%, especially when associated with vascular lesions, the extent of the trauma to the soft tissues and systemic hypotension,4 Muscle damage is the most common cause of edema, the latter being proportional to the damage, since the muscles dissipate the greatest amount of energy from the trauma.3
Diagnosis is made by history and clinical manifestations or by measurement of intracompartmental pressure by means of specialized devices. Cardinal signs of ischemia include pain, paresthesias, poikiloderma (irregular reddish-brown pigmented skin lesions), pallor, paralysis, and absence of pulse. Pain may be absent, but its presence as the only symptom is of extraordinary value, is characterized by being disproportionate to the physical findings, occurs with passive stretching of the involved muscles or palpation of the involved compartment, and is associated with swelling of the compartment.4,6 Symptoms can be further divided into pre-ischemic (pain and paresthesia) and postischemic (paresthesia that can become anesthesia, paralysis and absence of pulse), in patients with disorders of consciousness, the subjectivity of most of these symptoms makes diagnosis difficult.3
CS of the anterior compartment of the leg is characterized by pain that increases with passive plantar flexion of the ankle and foot, loss of sensation of the first interosseous space and pain and limitation of active dorsal flexion of the ankle and foot.3
A compartment pressure greater than 30 mm/hg or greater than 20 in a hypotensive patient or a delta value less than 30 is diagnostic. Tissue perfusion pressure or delta pressure is obtained by subtracting the compartment pressure from the diastolic pressure, which allows a more accurate diagnosis especially when the result is less than 30 mm/hg and is of particular use in the polytraumatized patient.9
The differential diagnosis is difficult, but is mainly made with cellulitis, osteomyelitis, stress fracture, tenosynovitis and deep vein thrombosis, but the most complex is made with arterial occlusion and neuropraxia, which can sometimes concomit with these diseases.3
Upon suspicion of compartment syndrome the patient should be evaluated by a surgical team with experience in the management of this disease, initially the limb is elevated and bandages are removed, it is important to reduce displaced fractures, treat pain and restore the circulating volume. Early fasciotomy is associated with a better functional outcome, shorter hospital stay and lower complication rate; closure is usually performed late primary (7-10 days).3,4
This is a 46-year-old patient with an apparent health history, who arrives for consultation with a healthy limb, along with several injured victims of the social unrest, being received in campaign conditions; He refers that he was treated in the emergency room about a week ago, after suffering a wound at the level of the anteroexternal face of the right leg, this injury was caused by an accident that occurred in the mechanical workshop where he works, when a cutting disc broke and hit his leg, he refers that the medical attention was quite difficult due to the social unrest that was happening. He received disinfection and stitches approximately 10 hours after arriving. He then took some analgesic medication on his own and was unable to heal the wound or change the bandage because of the difficulty of leaving his home due to the complex social situation. On the third day after the injury she noticed a discreet increase in the volume of her leg and a marked increase in pain at the injured site, making it difficult for her to ambulate and with very little relief from the painkillers she was taking, these symptoms intensified significantly, with the appearance of an annoying tingling sensation, so she decided to come to us a week after the initial injury.
On physical examination we found moderate increase in volume of the leg at the expense of the anteroexternal compartment, wound with stitches of approximately 15 centimeters (cm), unshaved surgical site, imperceptible pedial pulse, marked pain and decreased active mobility of dorsal flexion of the left ankle and foot, passive mobility of plantar flexion of the ankle and foot extremely painful, decreased sensitivity in the first interosseous space, heart rate 108 beats per minute and axillary temperature of 37.8 degrees Celsius.
Radiographic studies (Figure 1) showed the presence of a large shear disc fragment in the soft tissues of the leg and hematological studies showed leukocytosis with a predominance of segmented.
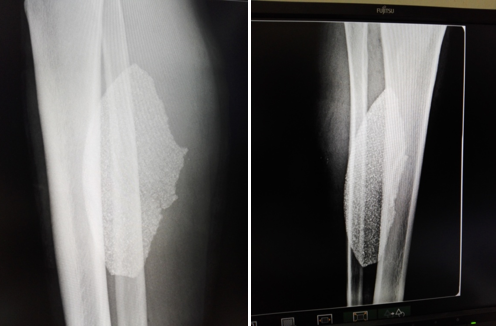
Figure 1 Radiographic images extend the antimicrobial spectrum and perform polyvalent antitetanus and antigangrenous prophylaxis.
After antibiotic prophylaxis with intravenous cefazolin 2 grams, a regional anesthetic block of the sciatic nerve in the popliteal fossa is performed posteriorly, after removing the stitches and evacuating abundant purulent material, we remove the fragment of the cut disc (Figure 2), place drainage, expand the antimicrobial spectrum and perform polyvalent antitetanus and antigangrenous prophylaxis.
The pedial pulse reappeared quickly, after recovering from the anesthesia we were able to confirm the recovery of sensitivity and disappearance of pain. The drainage was removed after 72 hours, the patient evolved favorably the following days, so we performed deferred primary closure 10 days after disc removal, institutional discharge 14 days later, reconstructed 4 weeks after the intervention indicating general rehabilitation, 6 weeks later she returned to her usual activities without sequelae.
Deciding on a medical-surgical conduct or complying with the established protocols in extraordinary situations of any kind is difficult due to several factors, the most frequent being, according to our criteria: the influx of several injured in a short period of time, not having a medical institution with an organized structure to perform massive reception of the injured, limited medical supplies, scarce qualified personnel and exhaustion of medical and paramedical personnel. All this affects the quality of medical care and may affect the quality of life of patients.
During the entire care of this patient, a series of negative factors converged and ended up with his hospitalization, due to the fact that all the procedures from the accident to the disc extraction were carried out in practically field conditions.
Downplaying the importance of the trauma mechanism, led the colleagues who acted beforehand to omit the possibility that a fragment of the cut disc was lodged in the soft parts of the leg, without downplaying the importance of the influence of the social context indicated; Therefore, they limited themselves to suturing the superficial planes without exploring the deep planes and did not indicate imaging studies that would have revealed the characteristics of the foreign body and ruled out a possible bone lesion; all these actions delayed the patient's recovery and endangered the viability of the leg and foot.
Our conduct was justified by the vascular compromise of the leg and foot, the impossibility of intervening in the operating room occupied with several emergencies and the impossibility of referring him due to the closure of the main roads in the city, so we decided to block him regionally and remove the fragment of the cutting disc.
The decision to block the sciatic nerve in the popliteal fossa by posterior approach was taken because of our experience in this type of block, in addition to the risk of greater contamination of the tissues near the foreign body involved in anesthetic punctures, since we were convinced that around the disc fragment there was abundant purulent material, responsible together with the fragment for the symptomatology.
This clinical case makes us reflect, as many bibliographies do, on the value of subacute CS, so it is very important to give an adequate follow-up to patients after a traumatic injury, no matter how insignificant it may seem, giving the patient and his family the possibility that at the slightest suspicion that something is not right, to come back to us for reevaluation and thus avoid complications that may affect the patient's function or life.
None.
Dr. Luis Enrique Montoya Cardero: conceptualization, data curation, project administration, methodological design, responsibility for management of the activity, as well as writing-revision and editing of the work. Approval of the final report. Participation: 50%.
Dr. Mileidys León Piñeiro: data curation, formal analysis, research process, data collection, validation, visualization, computer processing, supervision and writing of the original draft. Participation: 50%.

©2022 Cardero, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.