eISSN: 2469-2794


Research Article Volume 14 Issue 2
Divisao de Pneumologia, Instituto do Coraçao (InCor), Hospital das Clinicas HCFMUSP, Brazil
Correspondence: Telma de Cássia dos Santos Nery, Divisao de Pneumologia, Instituto do Coraçao (InCor), Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de São Paulo, Sao Paulo, Brazil
Received: April 01, 2026 | Published: April 14, 2026
Citation: Nery TCS, Roio LD, Carvalho CRRD. Telemedicine as a tool for smoking cessation - analysis of 154 cases in 2 years in the largest city in Latin America. Forensic Res Criminol Int J. 2026;14(2):80-83. DOI: 10.15406/frcij.2026.14.00471
Tobacco use is the leading preventable cause of death in many countries. Smoking is linked to high mortality. Therapies linked to cessation are always important. Cognitive-behavioral therapy (CBT) is a fundamental part associated with other therapeutic methodologies. During the pandemic period, CBT was initiated via telemedicine by video, comprising 4 sessions, with the other drug therapies being maintained. Aim: to analyze the use of telemedicine with CBT and smoking cessation. Methodology: descriptive study. Period: 2021 to 2023. Data analyzed: frequency in 4 weekly sessions, age, gender, color/race, reduction in the number of cigarettes and smoking cessation. Result: 154 enrolled cases were analyzed, 120 women (78%), with a mean age of 54 years. 81 (54%) white, 66 (42%) black. 121 (78,6%) people attended the first session, 108 (87,1%) the second session. 83 (54%) people attended all four sessions. 8 (5,2%) people stopped smoking after the first session. 4,5% after the second session, 22 (14%) people after third session and 29 (18%) people at fourth session. 9,7% reduced ≥ 50% on the first session, 25 (16%) people reduced by ≥ 50% in the second session,13% on third and 9,7% on the fourth session .14 (9,1%) people gave up or had difficulties. Conclusion: Brazil has been recognized internationally for actions in the field of regulation, education, prevention and governance for tobacco control. Thinking about strategies using telemedicine can enhance actions and strengthen UN Sustainable DGs. Telemedicine with CBT was important for the reduction of smoking in the four week period and can be an important tool in smoking cessation.
Keywords: telemedicine, cognitive-behavioral therapy, tobacco cessation
Smoking is the leading cause of preventable death in the world.1 It is associated with high mortality and is an important preventable risk factor for cardiovascular and respiratory diseases and malignant neoplasms.1,2 In 2019, 7.69 million deaths worldwide were attributed to smoking, and 5.96 million (77.5%) occurred in low- and middle-income countries.3
The global age-standardized prevalence of smoking decreased by 27.5% in men and 37.7% in women aged 15 years and older between 1990 and 2019. However, there was significant population growth during this period, resulting in an increase in the number of smokers from 0.99 billion in 1990 to 1.14 billion in 2019, with an equivalent consumption of 7.41 trillion (7.11–7.74) tobacco cigarettes in 2019.3
Structuring and defining treatment methodologies is essential. Brazil has been a signatory to the World Health Organization Framework Convention on Tobacco Control since 2005.4 It has a national tobacco control program that aims to reduce the prevalence of tobacco users and nicotine addicts, and the resulting morbidity and mortality related to the consumption of tobacco products, through actions to promote health, prevent and treat tobacco use and nicotine addiction. Clinical protocols and therapeutic guidelines for tobacco use are used, which are updated periodically.5
Therapies linked to smoking cessation are always important.
Smoking is characterized as a complex disease and its control requires the integration of several approaches, including pharmacological, psychological, mass communication and economic approaches, among others. Cognitive-behavioral therapy (CBT) is a fundamental part associated with other therapeutic methodologies.5 The use of CBT helps smokers change their tobacco consumption behavior, avoiding situations linked to relapses. Brazil provides smoking cessation treatment through the Unified Health System (SUS), which consists of structured therapeutic counseling with an intensive approach accompanied by drug treatment with nicotine replacement therapy (NRT): patch, gum associated with bupropion.5,6 The public policies provided for in SUS (Sistema Único de Saúde - Unified Health System) also include integrative and complementary health practices. In our service, CBT has always been part of the therapeutic measures in the outpatient clinic and during the pandemic period, CBT for smoking cessation was initiated via video telemedicine, comprising four sessions, one per week lasting approximately 120 minutes, with a multidisciplinary team with the other drug therapies being maintained, as recommended in the national guidelines included in Joint Ordinance No. 10.5 Our group telemedicine monitoring service is offered to all patients at the first consultation, and the patient makes the choice. It consists of providing information about the risks of smoking and the benefits of quitting and encouraging self-control or self-care so that individuals can manage the cycle of addiction.
Telemedicine throughout our hospital complex began with a tele-respiratory ICU project in March 2020. This project remains successful.7 Telemedicine has been seen as an important tool to address the challenges of universal health systems.8 It is characterized as the use of information and communication technologies for the delivery of health services, especially when distance is a critical factor in access to the health service provider.9 The concept of telemedicine and associated services are already well established and proven to help society.10 Studies show that live telemedicine is well accepted for the management of tobacco use disorders.11 A study also shows that the telemedicine approach is not inferior to the face-to-face approach in addressing smoking cessation.12
The COVID-19 pandemic has accelerated the implementation of real-time telemedicine, and in parallel, research has been conducted to test its effectiveness. Videoconferencing and telephone-based interventions are supported by robust evidence for at-risk alcohol, use and alcohol use disorder, tobacco use disorder, and opioid use disorder.
What we have in terms of innovation: knowing the use of telemedicine as a tool – in CBT in smoking treatment in a reference outpatient service that works in the training of medical residents in pulmonology. Our service has 3,780 registered patients who have sought treatment to quit smoking since 2000. Considering the “offers” of treatment methodologies and results presented in studies,13 we consider it essential to discuss different methodologies.
Objective
To analyze the use of telemedicine in CBT and smoking cessation in a Pulmonology service and describe the sociodemographic profile of patients who participated in the telemedicine CBT groups.
Descriptive study, where data from patients in the Pulmonology Division of a teaching hospital were analyzed. Data from smoking patients over 18 years of age who participated in group meetings to videoconferencing were analyzed. Nicotine addiction treatment groups for telemedicine are made up of four structured sessions that address cognitive and behavioral techniques on nicotine dependence with participation of a multidisciplinary team. Ten places are offered per month. Participants are included in the group based on an in-person assessment at the institution's pulmonology outpatient clinic. Patients included in the program between 2021 and 2023, who opted to participate in a group and agreed to the study's privacy policy, providing a free and informed consent form, were included as participants. The first session involves guidance and motivational practices. After the second session, medications are started according to the clinical picture and include: Bupropion 150 mg or 300 mg per day and/or nicotine patches of 7, 14 or 21 mg that can be associated with chewing gum. All patients used some type of medication, either in combination or alone. Sessions 3 and 4 consist of monitoring the strategies defined by each patient, clarifications and motivational/behavioral activities. All 154 patients who opted for group monitoring were included. The data analyzed were frequency in four weekly sessions, age, sex, color/race, reduction in the number of cigarettes and smoking cessation. Statistical analysis, continuous variables are presented as mean ± SD or median (IQR), depending on the distribution. Categorical variables are presented as numbers and percentages. The development of group care via telemedicine is carried out through the zoom platform, on a computer in our service and each patient participates through their cell phone, in a collective digital space. All patients participate in prior training and register consent forms.
From May 2021 to March 2023, 306 people over 18 years of age sought our outpatient smoking cessation service. Of these, 154 (50.3%) chose to initially be followed up via telemedicine and these cases were registered and analyzed here. 62% attended in 2022 (Figure 1).
Of the total in the group, 120 (78%) were women (Table 1). The average age was 54 years (+/- 9.6). Regarding self-declared color/ethnicity, 81 (53%) were white, 66 (43%) were black, 7 (4%) were yellow (Table 1). The Fagerstrom test shows that 63% have 5 or more points (Table 2).
|
Gender (women) |
120 (78,0 %) |
|
Age (yo) |
54.0 ± 9.6 |
|
Color/race |
White = 81 (52,6%) Black = 66 (42,9%) Yellow = 3 (2,0%) No date = 4 (2,5%) |
|
Tobacco load |
≤20 = 36 (23,0%) >20 = 117 (76,0%) No date = 1 (1,0%) |
Table 1 Sociodemographic and characteristics of tobacco load (pack-years) of the participants
|
Fagerstrom test |
Number |
% |
|
≤ 4 points |
57 |
37,0 |
|
5 points |
17 |
11,0 |
|
≥ 6 points |
79 |
52,0 |
|
No dates |
1 |
1,0 |
Table 2 Result of Fagerstrom test
In the analysis of attendance by session, we found that 121 (78%) people attended the 1st session, 108 (70%) the 2nd session, 97 (63%) the 3rd session, 98 (64%) the 4th session. 83 (54%) people attended all 4 sessions. Calculating the adherence rate considering the number of participants in the first session (121) in relation to fourth session (98), we found an adherence rate of 81%.
Regarding the result of quitting smoking with 154 participants, considering the number of people present in each session, we analyzed each session separately. 65,6 % stopped within one month, with 8 (6,6%) people stopping smoking after the 1st session (total of 121 participants), 7 ( 6,5%) after the 2nd session (total de 108 participants), 22 (22,7%) people after the 3rd session (total 97 participants) and 29 (29,6%) people in the 4th session (total 98 participants) (Figure 2). We also analyzed the item reduction of ≥ 50% of the initial number of cigarettes by session. 70,5% reduced, with 15 (12,4%) of the participants reducing ≥ 50% in the 1st session, 24 (22,2%) people had reduced by ≥ 50% in the second session, 20 (22,7%) in the 3rd and 15 (15,3%) in the 4th session. (Figure 2).
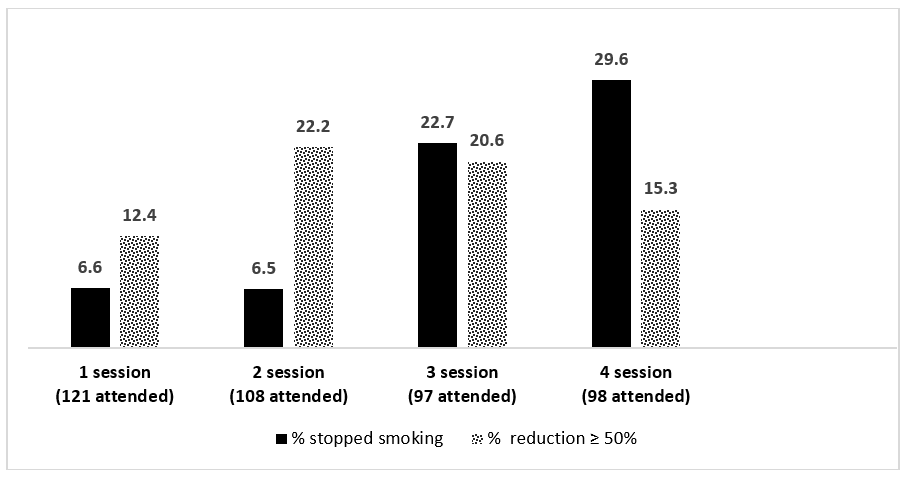
Figure 2 % of patients that stopped smoking by session, and % of reduction ≥ 50%. Period: 2021-2023.
According to our methodology, the use of medications begins after the second session.
At the end of the collective analysis of all sessions, we found that of the 154 participants, 66 (42.9%) stopped smoking, 74 (48.1%) reduced smoking ≥ 50% and 14 (9.1%) did not have final information due to absences or had difficulty participating (Figure 3).
Our study found that of the 154 participants, 90.9% had a significant impact on smoking cessation within one month.42,9% stopped smoking and 48,1 % reduced their initial number of cigarettes by ≥ 50%. When we analyze each session separately by the number of participants We found 65,6 % of participants stopped. Women were the majority of our patients in the group.
Data from the National Cancer Institute (INCA)14 indicate that in Brazil, women have been the majority in nicotine addiction treatment services since 2018, with 55% in 2021 and 2020, compared to 58% in 2019 and 57% in 2018. In national surveys, women are already the majority in nicotine addiction treatment services. The data found in our study indicates that women were also the most frequent in seeking CBT treatment via telemedicine (74%), as well as some studies found. A review involving 15 studies15 with the aim of describing the research that applied the Smoking Cessation Program in Brazil, identified, regarding the characterization of the samples, the predominance of female participants (51% to 73% and age range between 40 and 59 years).
A New York City study evaluating telehealth treatment during the COVID-19 outbreak for tobacco-dependent cancer patients found that 62% of participants were women.16 China has the highest number of smokers on the planet. A Chinese study17 that evaluated telephone monitoring of smoking cessation treatment found that almost all patients were male (97.4%, 335/344). Research in this country indicates that only 2% of smokers are women. A follow-up study in Japan13 found that 94% were men.
Studies indicate that the age range of those seeking treatment may be associated with the emergence of health consequences resulting from smoking. In Brazil, the prevalence of smoking peaks between 50 and 54 years of age for both genders.13
The average age of the population in our study was 54.00 (+/- 9.57), indicating a search for an elderly population. A study carried out in China with telephone counseling in a population aged 18 to 80 years old found 45.63 (±12.34 years) (17). A retrospective cohort study in Japan, carried out between August 2018 and October 2020, found an average age of 42.40±9.8 years.13
In the analysis regarding color/ethnicity, we found in our study that the white population is more frequent at 53%, as in some studies16 where it was identified that 78% were white.
In the analysis of attendance by session, we found that attendance rates for sessions were above 50%, where 60% attended the 1st session, 59% attended the 2nd session, and 54% attended all 4 sessions. A study that compared cessation rates between the two groups at 1, 2, 4, 8, and 12 weeks identified that smokers who attended telephone consultations had significantly lower quit rates at all follow-ups, compared to those who attended face-to-face consultations.18
Our adherence rate was 81%. A study that analyzed 15 Brazilian studies found adherence to treatment of 33% to 100%.19 Studies using telemedicine to treat tobacco users concluded that large-scale public health interventions delivered through telemedicine should be targeted at tobacco users living in rural areas.20
The outcome of quitting smoking or reducing the number of cigarettes by 50% or more were analyzed in our study. We emphasize that the use of medication usually begins after the second session. They are provided free of charge and vary according to the individual profile of each patient. Regarding the outcome of quitting smoking, out of a total of 154 participants, 8 (5,2%) people quit smoking after the 1st session, 4,5% after the 2nd session, 22 (14,1%) people after the 3rd session and 29 (18,0%) people in the 4th session. A study21 that analyzed the smoking cessation rate and factors affecting the success of smoking cessation in a smoking cessation clinic with telephone monitoring found that of the 344 patients, 16.3% stopped within 1 week, 26.5% within 1 month, 27.6% within 3 months and 31.7% within 6 months. One of the predictive factors for stopping at 6 months was telephone monitoring, age 60 or older, immediate cessation and previous attempts. We also analyzed the item reducing the initial number of cigarettes by 50% or more, 9,7% of participants reduced by 50% in the 1st session, 24 (16%) people had reduced by 50% in the second session, 13% in the 3rd and 9,7% in the 4th session. In a study22 where data were collected via telehealth and in-person primary care consultations for adult patient’s ≥18 years old, they observed that in the period from March 2020 to May 2020, monthly tobacco assessment rates decreased by 50% and increased from June 2020 to May 2021, but remained 33.5% lower than pre-pandemic levels. Authors concluded that using telehealth to collect information about smoking history and provide smoking cessation treatment can be effective.
Studies demonstrated the feasibility of using asynchronous counseling in smoking cessation.23
Our service is also aimed at training resident doctors, so it is essential that they have experience in smoking cessation programs. Ottawa study for Smoking Cessation used an “organizational change” approach and demonstrated that training primary care physicians in smoking cessation increases the rate of tobacco treatment, with the role of physicians in prioritizing smoking cessation being essential in all settings.23 Initial data from this population show promising results that encourage the expansion of our multidisciplinary team, highlighting telemedicine with CBT as an important tool for quitting smoking and reducing cigarette consumption.
Many studies talk about the importance of cessation counselling, brief advice with use of varenicline or other and each probably help more people to quit smokeless tobacco use than minimal or no support, or placebo.24–26 The main limitation of our study is the difficulty some patients have in accessing the system and attending all sessions.
Brazil has been internationally recognized for its actions in the areas of regulation, education, prevention and governance for tobacco control. Thinking about strategies that use telemedicine can improve actions. Telemedicine with CBT was important for smoking cessation and reduction in the 4-week period and can be an important tool in smoking cessation.
The authors would like to thank all the staff involved in the teleconsultation for smoking cessation at InCor - HCFMUSP and the professionals who participated in the sessions during this period especially: Dr. Stella Regina Martins, Shirlene Aparecida Lopes, Talita Cepas Lobo and the resident’s doctors
The author declare that there is no conflict of interest.

©2026 Nery, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.