Advances in
eISSN: 2377-4290


Case Report Volume 12 Issue 1
Associate Professor, Department of Ophthalmology, IvanoFrankivsk national medical university, Ukraine
Correspondence: Nataliya Moyseyenko, Doctor of Medical Sciences, Associate Professor, Department of Ophthalmology, Ivano-Frankivsk national medical university, Ukraine, Tel 0677566341
Received: June 03, 2022 | Published: June 27, 2022
Citation: Moyseyenko N. Neurodegenerative diseases oculomotor manifestations. clinical cases. Adv Ophthalmol Vis Syst. 2022;12(1):19-21. DOI: 10.15406/aovs.2022.12.00411
Oculomotor manifestations (nystagmus and diplopia) do not lead to blindness. But the loss of cognitive properties in the background, such as ability recognition and reading, leads to irreparable social consequences. Therefore, improved methods of diagnostic oculomotor disorders will help reveal neurodegenerative disease in earlier stages. Moreover, their correction will prevent undesirable outcomes.
Clinical case 1- Partial Parinaue's syndrome, confirmed by MRI revealed multiple small degenerations in the area of the brain bridge (according to the localization indicated by Parinaue's syndrome - in the dorsal - medial part).
Clinical case 2- Pronounced vertical-rotational nystagmus of both eyes with greater amplitude in the lead positions. Viral encephalomyelitis.
In their form and nature, oculomotor disorders are a good indicator of the topic of damage to deep brain structures such as the trunk and bridge. Therefore, a more thorough study will help diagnose neurodegenerative injury in the early stages, treatment and prevent unwanted social consequences.
Keywords: oculomotor manifestations, nystagmus, neurodegenerative diseases, diplopia
Neurodegenerative diseases (NDDs) are a heterogeneous group characterized by progressive structural and functional degeneration of the central and peripheral nervous systems. Oculomotor manifestations (nystagmus and diplopia) due to NDD do not lead to blindness, but the cognitive properties are lost, and the recognizing and reading disability destroys social life. Vascular dementia, Alzheimer's, Parkinson's, and Huntington's diseases are common causes of morbidity and mortality worldwide, especially among the elderly.1 The oculomotor disorders are detected much earlier than other symptoms.2 That is why NDD could use as a potential biomarker. There is essential to clarify the pathophysiology of NDDs and to indefinite their premorbid markers to improve diagnostics in the early stage.
Parkinson's and Huntington's disease and dementia become due to neurodegenerative disorders. They may reflect motor and cognitive aspects of oculomotor behavior.3 The laboratory investigations of eye movements reveal the severity of the disease due to nuclear and synaptic lesions of the central neural system (CNS). Its topical interpretation helps to understand the location of the neurodegenerative area and value the effectiveness of therapy.
In addition, ocular movement disorders are typical in Parkinson's disease and differentiate its types.4 As a result, saccades' latency becomes slower. However, the deterioration of the visual control of movement shows the disease's progression.5 Also, the antisaccade complex reduces its efficacy (Figure 1) There inhibit reflex reactions and the formation of voluntary saccades.6
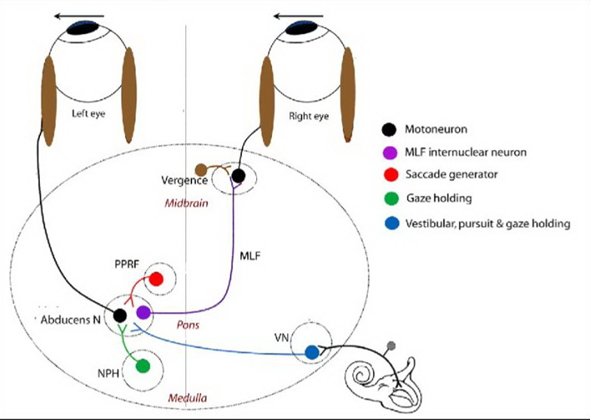
Figure 1 Antisaccade nerve complex.
Notes: A. look to the right, Б. initial position, B. look to the left, Г. convergence, Д. nystagmus at close range.
The internuclear ophthalmoplegia is common in multiple sclerosis (MS).7 Saccade eye movement changes relative to the clinical manifestations of MS.8 Therefore, there is impotent to improve the methods of diagnosing oculomotor disorders. That is why giving them topical analyses is essential. In addition, it is significant to investigate the neurodegenerative diseases' biomarkers.
The goal is to show two clinical cases with diplopia and nystagmus and give them CNS damage's topical interpretation.
The consultation of patients is based on the Department of Ophthalmology of Ivano-Frankivsk National University. It's done photo and video fixation. There were performed MRI of the brain and blood and cerebrospinal fluid immunological tests. All patients received informed consent for processing and personal data and used it for scientific purposes.
Clinical case 1- Patient B. is 30 years old. He complained about the concomitant horizontal double vision, which he suffered for over two years. He has suffered from polysinusitis for a long time. One year ago, he recovered after the maxillary and sphenoid sinuses surgery.
At the time of examination, the visual acuity of both eyes is 1.0. It was find bilateral convergent strabismus. Esophoria of both eyes was equal to 7 prisms. ptr. It was seen in the close distance nystagmus, (Figure 2) It was detected anisocoria (left pupil was more prominent), swollenness of direct and concomitant light pupillary reactions, but pupillary reactions for close distance were faster (Figure 3) RAPD was negative. It was detected slight retraction of the upper eyelid of the left eye. There was supported partial Parinaud's syndrome due to a unique combination of symptoms. Using MRI was found small multiple degenerations in the area of the midbrain. Following immunological tests of blood showed positive virus results. It could explain the reasons for neurodegeneration.

Figure 2 Oculomotor disorders in patient B.
Notes: A. Right site direct pupillary light reaction, Б. Left side swollenness of direct and concomitant light pupillary reactions, but pupillary reactions for close distance were faster, B. Reaction at close range is more active than light.
Clinical case 2- Woman O. 52 years old. Complaints of flickering in the eyes when looking into the distance. She suffered for over a year. As a result, the patient is forced to refuse to drive a car, and there is a question of ending her career, as she has difficulty working with a computer, an inability to read, and recently, loses the ability to recognize faces. On examination, her visual acuity was 1.0. She has a myopia of light degree. It was observed vertical-rotational nystagmus of both eyes in a larger amplitude in the lead positions. The immunological and virus examination of the cerebrospinal fluid was performed. The Epstein-Barr virus was detected. In conclusion, the diagnosis is viral encephalomyelitis.
There are two clinical cases with oculomotor disorders. Case 1 is characterized by a combination of bilateral convergent strabismus, nystagmus for close distance, dissociation of the pupillary light and close distance reactions, and retraction of the upper eyelid of the left eye in the downgaze. According to the literature, Parinaud's syndrome (Figure 4) includes a set of paralysis of the gaze upwards (the patient is absent), nystagmus of close-distance retraction, dissociation of the pupillary light and close distance reactions (B), and bilateral retraction of the upper eyelids.9,10 The search for the causes of disruption of the internuclear connections of the midbrain confirmed positive tests for viral infection.

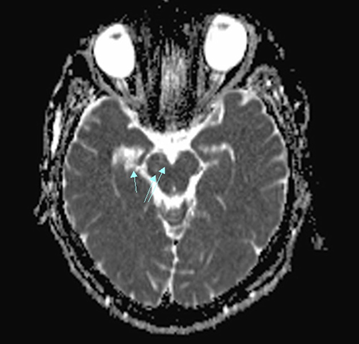
Figure 4 The localization of injuries in Parinau's syndrome.
Notes: A - scheme of the midbrain, B – MRI of lesions, 1 - dorsal midbrain syndrome, 2 - ventral midbrain syndrome, arrow – locals of the neurodegeneration.
There was used prismatic correction of diplopia to reduce his symptoms.
Case 2 was characterized by vertical nystagmus. There is a violation of the internuclear disconnections of the antisaccade complex in the midbrain. It is also common for Parkinson's disease or parkinsonism, which requires further study.
In their form and nature, oculomotor disorders are a good indicator of the topic of damage to deep brain structures such as the trunk and bridge. Therefore, more careful research will help diagnose neurodegenerative injury in the early stages, treatment and prevent unwanted social consequences.
None.
None.

©2022 Moyseyenko. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.