Advances in
eISSN: 2377-4290


Case Report Volume 3 Issue 3
Rome University La Sapienza, Italy
Correspondence: Maria Giulia Mutolo, Faculty of Medicine and Dentistry, Az Ospedaliera Sant Andrea Rome University La Sapienza Via di Grottarossa, 1037 00189 Roma, Italy, Tel 0039 3394083914
Received: October 23, 2015 | Published: November 13, 2015
Citation: Mutolo MG, Fabiani C, Pescosolido N. Neovascular glaucoma and diabetic macular edema in a patient with monolateral pseudoexfoliative glaucoma and type 2 diabetes: therapeutic effects of two-sided intravitreal triamcinolone acetonide treatment. Adv Ophthalmol Vis Syst. 2015;3(3):288-292 DOI: 10.15406/aovs.2015.03.00087
Background: To report on the safety and efficacy of intravitreal injections of triamcinolone acetonide in a patient with diabetic macular edema in the right eye and pseudoexfoliative glaucoma complicated by iris neovessels in the left eye.
Case presentation: Two intravitreal injections of triamcinolone acetonide were given (one per eye) in a 75 year-old caucasian male with macular edema in the right eye and neovascular glaucoma in the left eye. Changes in visual acuity, intraocular pressure, ophthalmoscopic examination of the anterior and posterior segment and flicker ERG response were regularly detected during a period of 6 months.
Conclusion: Bilateral visual acuity improvement was obtained after each injection and maintained for the whole observation period. Central retinal thickness in the right eye decreased after intravitreal injections of triamcinolone acetonide and remained stable until the last observation 6 months later. Iris neovessels in the left eye disappeared after the injection in the left eye. Flicker ERG implicit time in the right eye improved after intravitreal injections of triamcinolone acetonide, and remained stable in the left eye. No side effects of the treatment were observed. Intraocular pressure in the right eye remained within normal values without any intraocular pression-lowering drug, whereas it showed even some decrease in the left eye, despite the presence of glaucoma.
Keywords: neovascular glaucoma, diabetic macular edema, pseudoexfoliative glaucoma, triamcinolone acetonide, flicker ERG
DM, diabetes mellitus; DME, diabetic macular edema; NVG, neovascular glaucoma; NVs, angle neovessels; IVTA, intravitreal injections of triamcinolone acetonide; RE, right eye; LE, left eye; NCVA, non-corrected visual acuity; CF, count fingers; OCT, optical coherence tomography
Progressive ocular complications of diabetes mellitus (DM) result by the chronic exposure to high blood levels of glucose. Diabetic macular edema (DME) is the most common complication, and the cause of moderate to severe visual loss in diabetic patients. Furthermore, DM is the major etiologic factor for neovascular glaucoma (NVG) 1. The association of iris and angle neovessels (NVs) with DM becomes more frequent with the duration of the disease and inadequate blood sugar control.2 In the case here reported, the patient was affected by pseudoexfoliative glaucoma in his left eye, and by DME in the right eye. Intravitreal steroids are have been used in the management of both DME and NVG, due to their anti-inflammatory and anti angiogenic effects. Indeed, several studies reported the benefits of triamcinolone acetonide intravitreal injections (IVTA) in reducing DME and increasing visual acuity,3–6 alone or in association with laser treatment, and also like a useful additional tool in the management of neovascular glaucoma.7–9
A 75-year-old Caucasian male patient, with type II diabetes and hypertension (under oral therapy with hypoglycemic drugs) presented with DME in the right eye (RE) and iris and angle NVs in the left eye (LE). The patient had pseudoexfoliative glaucoma in the left eye and was on anti glaucoma treatment with an association of timolol and brimonidine plus brinzolamide. Non corrected visual acuity (NCVA) was 20/400 in the RE and count fingers (CF) in the LE. Intraocular pressure (IOP) was 18mmHg in the RE and 36mmHg in the LE. Figure 1 shows iris neovascularization of the left eye at slit lamp examination before and after IVTA treatment.
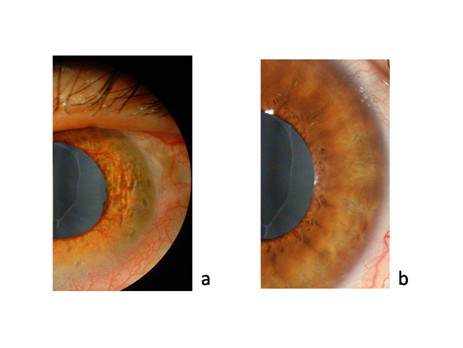
Figure 1 Morphological analysis of the left eye. A) Picture of the anterior segment soon before IVTA; B) Picture of the anterior segment two months after IVTA.
Figure 2 shows the optical coherence tomography (OCT) radial scan of the macula before and after IVTA treatment. Figure 3 shows the trend of macular thickness (a), flicker ERG implicit time (b) and IOP (c). Slit lamp examination of the RE anterior segment revealed moderate lens opacity while in the LE it showed iris and angle NVs, fixed mydriasis, pseudoexfoliation of lens capsule and mild lens opacity. The fundus examination of both eyes showed diabetic retinopathy with hemorrhages, microaneurysms, hard exudates and clinically significant macular edema in the RE with subfoveal and perifoveal hard exudates. Macular thickness measured with the OCT was 634 μm in the RE and 200μm in the LE. Flicker ERG implicit time was 36.64 ms in the RE and 42.15 ms in the LE.
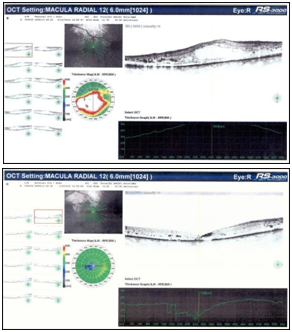
Figure 2 Morphological analysis of the right eye. A) OCT macular thickness soon before IVTA; B) OCT macular thickness 6 months after IVTA.
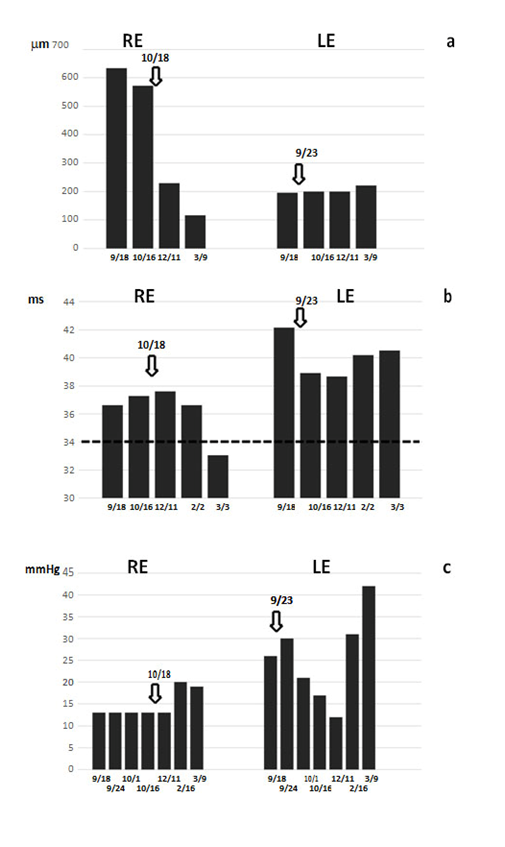
Figure 3 Trend analysis of relevant parameters during the 6 months of observation. A) Macular thickness at OCT; B) flicker ERG implicit time (the dotted line indicates the normality threshold level); C) IOP progression. The X axes report the dates of each evaluation. Arrows at the top indicate the date of IVTA treatment.
An IVTA was proposed for both eyes commencing with the LE. Therefore, a first injection of 4 mg (0.05 ml) triamcinolone acetonide (Taioftal ®, Sooft Italia S.p.A, IT) was performed in the LE. After one month, visual acuity was still CF, but iris and angle NVs were barely visible both at slit lamp examination and gonioscopy. IOP was reduced to 17mmHg and the fundus examination showed a marked reduction of the hard exudates. After two months follow-up, BCVA in the LE increased to 20/100 and no iris and angle NVs were detectable at slit lamp examination. IOP further decreased to 12 mmHg. Hard exudates were strongly decreased at fundoscopy, OCT macular thickness was 196μm and flicker ERG implicit time decreased to 38.50 ms. After six months follow-up, BCVA remained stable at 20/100 while IOP returned to 42 mmHg. Iris and angle NVs reappeared and were detectable both at slit lamp examination and gonioscopy. Fundus examination showed no reappearance of hard exudates, OCT macular thickness was stable at 221μm, whilst flicker ERG implicit time returned to 40.53 ms. 25 days after the IVTA in the LE, an injection of 4 mg (0,05 ml) triamcinolone acetonide (Taioftal ®) was given also in the RE. At one month follow- up NCVA was still 20/400, IOP was 13 mmHg and OCT macular thickness already decreased to 229μm. At fundus examination subfoveal and perifoveal hard exudates were reduced together with the entity of DME. Flicker ERG implicit time was 37.61 ms. Five months after treatment, visual acuity was improved to 20/100, IOP was 20 mmHg and fundus examination revealed a further reduction of the hard exudates and of the DME (macular thickness 116μm). Flicker ERG implicit time decreased to 33.07 ms.
This case illustrates the usefulness, safety and efficacy of intravitreal injections of triamcinolone acetonide in a patient with diabetic macular edema in the right eye and pseudoexfoliative glaucoma complicated by iris and angle neovessels in the left eye. During the 6 months observation period all the parameters under analysis were improving. Most notably, OCT showed a rapid important thinning of the macular area in the RE. Flicker ERG implicit time, as demonstrated in previous studies,10,11 is a quantifiable objective measurement of photoreceptor damage in different types of retinal diseases. In this case, its initial values were above the normality threshold of 34 ms10 in both eyes. After IVTA in the RE we observed a decrease of its value below the normality threshold (33.07 ms at 6 months) that was concomitant with the normalization of macular thickness at 116µm and a modest increase of visual acuity. In contrast, flicker ERG values in the glaucomatous LE remained stable, above the normality threshold, despite some improvement of the visual acuity.
In good agreement with the known literature,3–6,12 IVTA showed a good efficacy in both decreasing macular thickness in the RE and iris and angle NVsin the LE. No complications were observed during the whole 6 months observation period and the procedure resulted in rapid improvement of most of the symptoms. Furthermore, the steroidal treatment has shown to be effective in both the pathological conditions, and this is probably due to the inflammatory etiopathogenesis of both diseases. NVG, in fact, is a secondary ocular pathological condition resulting from a myriad of ocular and systemic conditions with retinal ischemia as a mediator in over 95% of cases. Inflammatory process maybe an important cause of iris neovascularization in subjects with NVG in addition to growth factors alone. In addition, DR manifests characteristics of both vasculopathy and chronic inflammatory diseases. Therefore, inhibition of the inflammatory process represents a therapeutic strategy valid for both diseases. The risks related to the intravitreal injection of steroids seem to be reasonable and well manageable. The IOP increase is higher in eyes with glaucoma and a high baseline IOP,13 although it appears to be manageable by anti glaucoma drugs.14 However, in this patient no further increase of IOP was observed, rather IOP in the both eyes even showed some decrease in the weeks following IVTA. Cataract progression is also known to occur as a consequence of steroid injection,15 but it requires longer times of observation, falling outside the observation time reported for this patient.
None.
The author declares there is no conflict of interest.

©2015 Mutolo, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.