Advances in
eISSN: 2377-4290


Case Report Volume 12 Issue 2
Assistant Professor, Department of Ophthalmology, Harran University School of Medicine, Turkey
Correspondence: Lokman Balyen, MD, Assistant Professor, Department of Ophthalmology, Harran University School of Medicine, Sanliurfa, Turkey, Tel 905058747473
Received: July 15, 2022 | Published: July 28, 2022
Citation: Balyen L. Maculopathy secondary to accidental laser beam exposure during alexandrite laser device repair. Adv Ophthalmol Vis Syst. 2022;12(2):45-47. DOI: 10.15406/aovs.2022.12.00416
Lasers have become widely used in various sectors such as industrial, military, social settings, and as well as cosmetic. Laser epilation is an increasingly popular method of hair removal. However, if not used with care, it can cause serious ophthalmological and psychological disorders; this may lead to job loss and economic loss. Eye injuries in the workplace are quite common worldwide, particularly in low-income and middle-income countries. The retina is the most vulnerable tissue to laser-related injury, which can lead to serious needless visual impairment. Therefore, precautions need to be taken to prevent such injuries, which could become a critical public health problem. This report relates to a 41-year-old female esthetician with unilateral maculopathy. An acute visual field defect occurred inadvertently with unplanned laser exposure while trying to repair Alexandrite laser device without any eye protection. Fundus examination, colour, red-free photography, fluorescein angiography (FFA) and optical coherence tomography (OCT) were performed. This report is important because it will raise awareness within both the medical and public sectors about the risks of misuse of laser epilation devices.
Keywords: Laser epilation, maculopathy, medical expenses, repair, job loss, economic loss
Unwanted hair has become a public health issue. Therefore, the use of lasers in the cosmetic setting has become widespread.1,2 However, inadvertent laser-induced eye complications have led to loss of labour productivity, economic loss to the affected individual, and to increased medical expenses. Furthermore, for the affected individual such accidents with lasers can lead to mental and psychological problems, low self-esteem and loss of self-confidence.1
During normal laser usage melanin in the hairs absorbs red and near-infrared light in the range from 600 to 1100 nanometers; this leads to photothermal damage of the hair follicles by the combination of long-pulsed ruby (694 nm), long-pulsed alexandrite (755 nm), long-pulsed diode (810 nm), long-pulsed Nd: YAG (1,064 nm), and intense pulsed light (IPL) (590–1200 nm).3 In the United States, there are more than 65,000 work-related eye injuries annually.4 However, the use of effective eye protection reduces injuries by more than 90 percent.4 This report is of a case of unilateral maculopathy developing while trying to repair Alexandrite laser device without proper eye protection.
A 41-year-old female aesthetician was admitted to our outpatient clinic with complaints of visual field defect, pain, and photophobia in the left eye. Approximately four days previously, while repairing the Alexandrite laser epilation device in the beauty centre, her left eye was exposed to a single, accidental direct discharge of energy from an Alexandrite laser epilation probe without using appropriate protective goggles. On ophthalmologic examination, the findings of the right eye were fully normal. In the left eye, the best-corrected visual acuity according to Snellen chart was 20/63. Fundus examination of the left eye revealed a yellowish spot in the central fovea (Figure 1). Red-free photography and fundus fluorescein angiography (FFA) revealed a hyperfluorescent appearance in the fovea (Figures 2&3). Optical coherence tomography (OCT) revealed intraretinal hyperreflective vertical structures extending to the external limiting membrane (ELM) under the foveal region. However, the retina pigment epithelium (RPE) and the inner segment/outer segment (IS/OS) junction or ellipsoid zone (EZ) were intact and there was no thinning or missing in the RPE, nor was there any thinning, missing, and dropping of the retinal layers. There was no intraretinal or subretinal fluid, nor was there tissue ischaemia or choroidal changes. In addition, there was no increase in signal transmission through the RPE/Bruch’s complex (Figure 4). She was treated with topical steroids, cyclopentolate, non-steroid anti-inflammatory eye drops, and systemic non-steroid anti-inflammatory drugs. She used these drugs for about 2 months; there was no change in visual acuity and fundus examination findings at 4 months or at subsequent observation at the outpatient clinic.
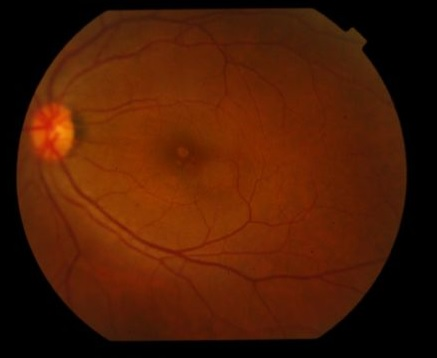
Figure 1 Colour fundus photography (CFP) demonstrating yellowish spot in the central fovea in the left eye.
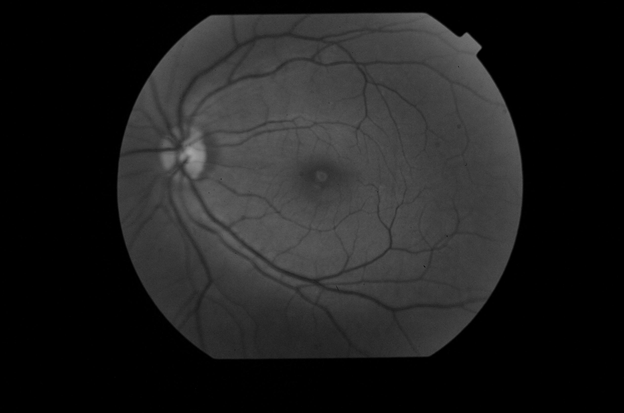
Figure 2 Red-free fundus photography demonstrating hyperfluorescent appearance in the fovea of the left eye.
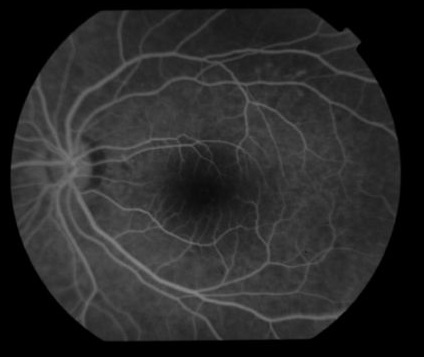
Figure 3 Fundus fluorescein angiography (FFA) demonstrating hyperfluorescent appearances in the fovea of the left eye, but there is no leakage.
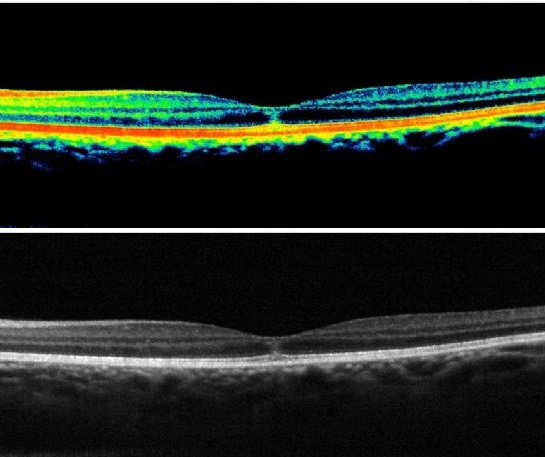
Figure 4 Optical coherence tomography (OCT) demonstrating intraretinal hyperreflective vertical structures extending to the external limiting membrane (ELM) under the foveal region of the left eye. The RPE and IS/OS band are entirely intact and intraretinal or subretinal fluid accumulation are not observed. There is no RPE band thinning or missing, nor is there thinning, missing, or dropping of the retinal layers. There is no tissue ischaemia or choroidal changes, nor is there any increased signal transmission through the RPE/Bruch’s complex.
Eye injuries in the workplace are quite common worldwide, particularly in low-income and middle-income countries.5 In particular, retinal injury after inadvertent laser exposure is becoming more common, this causes injury by photochemical, photomechanical and photothermal mechanisms.6 Laser epilation is an increasingly popular method of hair removal.7 There are severe potential complications resulting from laser hair removal procedures including corneal burns, iris atrophy, uveitis, pupillary distortion, posterior synechiae, cataract, as well as retinal burns. Lasers cause common symptoms such as pain, photophobia, conjunctival hyperaemia, blurred vision, and visual field defects.8 There is no doubt the retina is the most vulnerable tissue in the body to laser-related injury.9 The severity of retinal injury is associated with duration, wavelength and amount of laser exposure and the location of the lesion (i.e. the closeness of laser influence to the macula).
The foveal lesions generally lead to irreversible visual field defects, nevertheless parafoveal lesions that affect the fovea via inflammation and oedema may be reversible; however, perimacular and paracentral retinal burns may not cause visual acuity loss.9 In this case, the degree of macular injury was relatively limited due to the very short exposure duration. However, the damage had affected the visual acuity and the loss was irreversible because of the foveal localisation.10 have reported a case that presented with sudden loss of vision after inadvertent Alexandrite laser exposure during laser epilation without proper eye protection. Likewise, Anaya-Alaminos et al.11 have described a case of foveal injury due to an Alexandrite laser epilation procedure. Also, bilateral macular injury has been reported secondary to misuse of an Nd: YAG laser device.12 In this report, the person repairing the laser device was untrained and not an expert and did not wear protective goggles. Therefore, in the event of a breakdown of laser devices, it is essential that only trained service personnel repair them. In addition, beauty centres need to undergo very serious supervision, and have legal permission for operating. Consequently, this would increase the safety of patients, aestheticians and repairers.
Laser-induced ocular complications are likely to cause extremely serious irreversible tissue injury. It is very important to provide well-fitted, durable, protective goggles that are effective in preventing such dangerous exposures, and thus reduce the needless visual impairment and blindness. The increasing use of lasers in many cosmetic settings means that adequate and effective personnel protection is of utmost importance in beauty centres. In this perspective, the education of aestheticians, which raises the awareness of laser-induced hazards, is very important in the workplace setting. By this means, we can also prevent potential economic loss, loss of labour productivity and extreme medical expenses. It is important that medical staff, such as ophthalmologists and dermatologists, as well as the public is made aware of the risks associated with the use of lasers by non-medical personnel.
The author certifies that he has obtained appropriate patient consent form. In the form, the patient has her consent for her images and other clinical information to be reported in the journal. The patient understand that her name and initials will not be published and due efforts will be made to conceal her identity, but anonymity cannot be guaranteed.
None.
None.

©2022 Balyen. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.