
Perspective Volume 6 Issue 2
Femtosecond Assisted Lasik for Post PKP Myopic Astigmatism
Bahaa Al Din Jaber
Department of Cornea Refractive Surgery Bahaa Eye Clinic Jordon
Correspondence: Bahaa Al Din Jaber Department of Cornea Refractive Surgery Bahaa Eye Clinic Amman Jordan
Received: January 23, 2017 | Published: February 8, 2017
Citation: Jaber BAD (2017) Femtosecond Assisted Lasik for Post PKP Myopic Astigmatism. Adv Ophthalmol Vis Syst 6(2): 00175 DOI: 10.15406/aovs.2017.06.00175
Download PDF
Introduction
High residual refractive error can be a disappointing end point to an otherwise successful penetrating keratoplasty, it can prevent the patient attaining satisfactory visual acuity.
Causes of astigmatism post PKP
- Size and shape difference between donor and host
- Eccentric placement
- Scarring at graft host junction
- Asymmetric forces in the cornea resulting in altered shape
Astigmatic patterns
- According to ESCRS istanbul (Dr Rudy niujts)
- 4 to 5 D and anisometropia
- 30% shows > 5 D
- 25% regular
- 75% irregular
Vision correction options after keratoplasty
Non surgical
- Spectacles.
- Contact lenses
- Surgical
- PRK … (disadvantage) haze and scar.
- Corneal relaxing incision, wedge resection, along with ± compression sutures…….. (disadvantage) Wound dehiscence, corneal topographic changes, low predictability of the results, lack of internationally accepted nomograms.
- Lasik using microkeratome or femtosecond laser.
- Implantable contact lenses.
- ICRS
- Femtosecond laser–assisted
- Intrastromal corneal ring
- Segment implantation for high
- Astigmatism correction after
- Penetrating keratoplasty
- Carlos Lisa MD, Miriam García-Fernández MD, David Madrid-Costa PhD, Leonardo Torquetti MD, PhD, Jesús Merayo-Lloves MD, PhD, José Fernando Alfonso MD, PhD correspondence mail
Femtosecond laser
Ultra-short pulse duration (10-15 sec.) has the ability to deliver laser energy with minimal collateral damage to the adjacent tissue (1µm).
Femtosecond laser
- Mechanism of action
- Photo disruption
- FSL energy is absorbed by the tissue, resulting in plasma formation.
- This plasma of free electrons and ionized molecules rapidly expands, creating cavitation bubbles.
- The force of the cavitation bubble creation separates the tissue (Figure 1).
Femto laser
Why femto?
The only reliable and predictable way of creating the flap within the graft.
Why femto (cont’d)
- Reduced incidence of flap complications like buttonholes, free caps, irregular cuts etc.
- Control over flap diameter and thickness; side cut angle, hinge position and length.
- Increased precision with improved flap safety and better thickness predictability.
- Capability of cutting thinner flaps to accommodate thin corneas and high refractive errors.
Why femto (cont’d)
- Stronger flap adherence.
- Better contrast sensitivity.
- Decreased incidence of epithelial in growth.
- Extremely low incidence of graft wound dehiscence secondary to less increase in IOP required. (20 to 35 mm) compared to microkeratome (55 to 70).
- NB. The fibrotic edge of the graft was also an additional safety factor for us for the prevention of a possible transplant wound rupture.
Why femto (cont’d)
- Lesser incidence of dry eye due to higher epithelial stability.
- Lesser hemorrhage from limbal vessels.
- The ability to retreat immediately if there is incomplete FS laser ablation.
Why Femto?
- It is capable, to a certain extent, of passing through optically hazy media, such as an edematous cornea.
- The laser may be applied in multiple geometric patterns including vertical, spiral, or zigzag cuts.
- It can be focused anywhere within or behind the cornea.
Why Femto?
It is not a blade! (Figure 2).
Figure 2 It is not a blade!
Aim of the study
The purpose of this study is to determine the efficacy and stability of LASIK for the correction of post keratoplasty myopic astigmatism using a femtosecond laser for flap creation.
Study design
- Retrospective study, 40eyes of 35patients
- Time between PKP and femtosecond lasik 18 to 65months mean (41.5)
- Interval at least 8months after suture removal
- AGE: 25years TO 54years MEAN 39.5
- Follow up 1, 3 and 12months
Study design (Cont’d)
All patients were examined pre & post operatively for:
- UCVA
- BSCVA
- Autoreffraction and cycloreffaction(cyclo pre only),
- Corneal topography(TMS4),
- Corneal tomographhy (allegretto occulizer),
- IOP,
- ORA,
- And Pachymetry.
Study design (cont’d)
- Contraindications for refractive intervention include peripheral corneal vascularization, thin host tissue, wound ectasia and significant graft override or malapposition.
- The patient should have a minimal corneal thickness of at least 500μm.
- The possibility of graft rejection was considered and addressed by the use of topical steroids post operatively.
Pre op
- Pre op myopia -3.50 to -7.75D
- Pre op astigmatism -3.00 to -6.00D
- Pre op UCVA CF 3mtr to 0.30
- “The attempted spherical equivalent correction ranged between 60 to 90% of the measured pre op refraction.”
Post op
- Myopia -0.75 to -1.75 D
- Astigmatism -1.25 to -2.25
- UCVA 0.40 TO 0.90
Discussion
- In 3month follow up 75 to 92% reached the attempted correction (±1.00D).
- (Mean increase is 4lines) 3months.
- And in 1 year follow up all of the examined eyes (31 out of 40) gained at least 3lines on snellin acuity tests.
- No pt has lost one line of his original visual acuity.
- One eye exhibited peripheral flap epithelial in growth which didn’t require any flap re lifting.
Data analysis
Se pre op vs post op (Figures 3‒6).

Figure 3 Data Analysis: Se pre op vs post op.
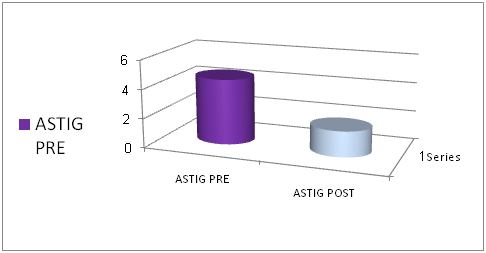
Figure 4 Data Analysis: astig pre vs astig post.
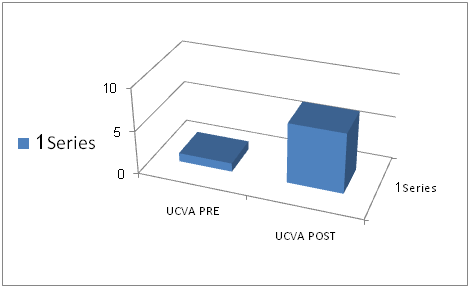
Figure 5 Data Analysis: UCVA pre vs UCVA post.
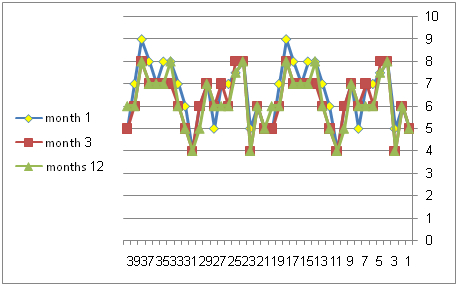
Figure 6 Effective procedure for pt with myopic astigmatism post PKP.
Conclusion
- Femto lasik is an effective procedure for pt with myopic astigmatism post PKP.
- It is also relatively a safe procedure with minimal complications regarding the surgery itself and the graft.
- However; more work should be done regarding the endothelial cell count and topographic changes over years.
Take home message
- Talk to the patient.
- Determine his needs, expectation
- Use the best and safest technology available to serve the best outcomes.
Acknowledgments
Conflicts of interest
The authors declare that there is no conflicts of interest.
Funding

©2017 Jaber. This is an open access article distributed under the terms of the,
which
permits unrestricted use, distribution, and build upon your work non-commercially.


