eISSN: 2378-3176


Research Article Volume 4 Issue 6
1Neurourology Unit, Rambam Health Care Campus, Israel
2Pain Research Unit, Rambam Health Care Campus, Israel
3The Ruth and Bruce Rappaport Faculty of Medicine, Technion-Israel Institute of Technology, Israel
4Department of Statistics, Rambam Health Care Campus, Israel
Correspondence: Ilan Gruenwald, Neurourology Unit, Rambam Health Care Campus, 12 Haaliya st, P.O.B 9602, Haifa 3109601, Israel, Tel 972-54-4-474341, Fax 972-4-8542883
Received: February 19, 2017 | Published: May 29, 2017
Citation: Gruenwald I, Adler MT, Haddad MM, Leiba MR, Eisenberg E (2017) Sexual Dysfunction in Patients with Chronic Pain. Urol Nephrol Open Access J 4(6): 00147. DOI: 10.15406/unoaj.2017.04.00147
Objective: Restricted normal activities associated with chronic pain are well documented. In contrast, there is a paucity of reports regarding the association between chronic pain patients and their sexual function. The aim of the present “snapshot” study was to evaluate the prevalence and severity of sexual dysfunction (SD) in a cohort of patients suffering from chronic pain.
Methods: 709 patients with chronic pain completed questionnaires assessing demographics, pain-intensity, disability and severity of their SD. A subgroup also completed questionnaires relating to depression and anxiety as well as specific gender-related SD questionnaires.
Results: 404 patients (58%) reported pain related SD. No differences in demographic parameters were found between those with and without SD. In contrast, patients with SD exhibited significantly higher scores in pain intensity (VAS), Short-form McGill Pain questionnaire and the Oswestry Disability Index. Patients with SD also consumed significantly higher doses of pain medications. On both numerical and categorical self-report scales of SD severity, women scored slightly but significantly higher than men. A significant correlation was found between pain intensity and SD severity (Pearson's test: r=0.349; p<0.001). The questionnaires completed by a sub-group of patients with SD revealed a mild degree of depression, a moderate anxiety level and a moderate degree of SD in both genders.
Conclusion: A significant number of patients with chronic pain suffer from moderate to severe SD, which correlates with pain intensity. These findings are congruent with previous reports and highlight the importance of increased awareness to SD in patients with chronic pain.
Keywords: chronic pain, disability, sexual dysfunction
Chronic pain is associated with significant disability in various domains of daily activity, which has been consistently documented in the medical literature.1,2,3 In contrast, there is a relative paucity of reports (especially in the pain literature) regarding the prevalence and severity of sexual dysfunction (SD) in patients with chronic pain, which may be due to various reasons. First, both patients and their caregivers may feel embarrassed to discuss SD, as indicated in a recent study in which 66% of the patients with chronic low back pain noted that they have never discussed the subject with their healthcare providers even though the prevalence of SD was 81%.4 Second, although SD is frequently assessed in studies on chronic pain by using disability questionnaires such as the Pain Disability Index (PDI)5 or the Oswestry Disability Index (ODI),6 in most studies, only the total scores of those questionnaires are reported, overlooking the prevalence and severity of specific domains such as SD.
One specific population of patients with chronic pain seems exceptional in this regard. These are patients with chronic pelvic pain in whom SD has been studied extensively.7,8 Yet, published literature on patients with other forms of chronic pain points to high prevalence of SD9‒12 More recently higher levels of SD were found in 166 women with chronic widespread pain compared to healthy women.13 Another recent study on a large population of Iranian patients with chronic low back pain, showed a twice as high prevalence of SD compared to healthy controls (women 71.1% versus 36.8%; men 59.5% versus 24.5%, respectively).14 Higher prevalence of SD was also reported in male patients with migraine and tension type headaches15 and in women with primary headaches.16
Many factors have been identified as potential contributors to SD in patients with chronic pain. They include physical limitations, actual pain or fear of pain during sexual activity,17 depression and other psychosocial factors.9,11 A higher prevalence of SD was reported in patients with chronic pain who had greater disability and depression, shorter pain duration, and infrequent use of coping self-statements. Adverse effects of medications, which are used frequently for the management of chronic pain, can also alter sexual function.18‒22 The present study was aimed to validate previous published knowledge on this topic by conducting a survey on the prevalence and severity of pain-related SD in a large population of patients with chronic pain who were referred to a tertiary ambulatory care pain clinic in Israel. We hypothesized that SD will indeed be prevalent among these patients and that patients with chronic pain and SD will exhibit higher levels of pain intensity, disability in additional functional domains and will consume more medications than those without SD.
The Rambam Health Care Campus Ethical Committee approved the study and a written informed consent for participation in the study was obtained from all participants. The study population consisted of patients who were referred to the Institute of Pain Medicine at Rambam Health Care Campus in Haifa, Israel, a tertiary referral center, for the management of their chronic pain. As part of a routine preliminary assessment, the following questionnaires were mailed to all referred patients: I. Ademographic questionnaire; II. The Visual Analogue Scale (VAS) and the Short-form McGill Pain questionnaire (SF-MPQ)23 for assessing pain intensity and qualities; III. The Ostwestry Disability Index (ODI)6 for quantifying pain related disability. An additional page was attached to the questionnaires with a short explanation on the study and making it clearly optional for the patients who are willing to participate to indicate whether or not pain has affected their sexual functioning. Patients were advised that by answering this question they give their consent to participate in the study. Those that consented were then requested to self-assess the severity of their pain-related SD on a 0-100 numerical scale (where 0 represents no SD and 100 represents complete SD) and on a five point categorical pain scale (0=no SD; 1=mild SD; 2=moderate SD; 3=severe SD and 4=complete SD). These measures are based on the "sexual behavior" scale of the Pain Disability Index.24
For the purpose of this study SD was defined as difficulty experienced by the patient or by both the patient and his/her partner during any stage of a normal sexual activity. Patients were instructed not to answer the question and to leave these scales untouched if they wished to decline participation. Patients who completed the SD scales were then requested to complete additional questionnaires including I. The Beck Depression Inventory II (BDI)25 II. The Beck Anxiety Inventory (BAI).26 These questionnaires were used for assessing levels of depression and anxiety, respectively; III. The Female Sexual Function Index (FSFI)27 for women; IV. The International Index of Erectile Function (IIEF-EF)28 questionnaire for men. Statistical analyses consisted of Chi Square and T-Test for comparisons between different sub-groups within the cohort and Pearson's coefficient test for correlations between various parameters (demographic and pain) and SD.
Initial questionnaires
One thousand and fifty-nine patients (men = 542; 52%) who were referred to the Pain Clinic at Rambam Health Care Campus, Haifa, Israel for the treatment of chronic pain were offered to participate in this study. Seven-hundred and nine patients agreed to provide information regarding their sexual function in relation to their pain (67% response rate; Figure 1). The response rate was higher among approached men (79.1%) than women (54.1%). Four-hundred and four patients (58% of the responders) reported that pain had affected their sexual function. Two-hundred and forty-nine of them (61.6%) were men and 155 (38.4%) were women. A comparison of the demographic data of the patients with reported pain-related SD (n=404) to those with chronic pain but without pain-related SD (n=305) did not reveal any significant differences interims of age, gender, weight, years of marriage, and level of education (Table 1).
Parameter |
All patients |
With SD |
Without SD |
p-value* |
Mean Age (years) |
44±13 (45) |
45±13 (45) |
44±14 (45) |
P=0.37 |
Gender |
429 (61%) |
249 (58%) |
180 (42%) |
P=1.00 |
Mean weight (kg) |
79±16 (78) |
80±17 (80) |
77±15 (75) |
P=0.07 |
Mean Marriage (years) |
23±12 (23) |
22±12 (22) |
23±14 (24) |
P=0.48 |
Education, n(%) |
40 (7%) |
29 (9%) |
11 (5%) |
P=0.18 |
Table 1 Comparison of demographic data between patients who reported SD and those who denied having SD
*Comparison between patients with and without SD
Data is presented as mean ± standard deviation (median) or number (percentage).
In contrast to the demographic findings, significant differences between these two patient groups were found in a number of clinical parameters, including pain intensity (VAS and SF-MPQ), disability measured by the ODI and consumption of all types of analgesic medications (Table 2). All these parameters scored higher in the group with pain-related SD as compared to the group without pain-related SD. Three-hundred and thirty nine patients (207 men and 132 women) of the 404 patients who reported pain-related SD, provided information on the magnitude to which pain affected their sexual function. High scores of SD were reported on both the 0-100 (0= no SD; 100= complete SD) numerical scale (mean±SD = 70±24) and on the five points (no SD=0; mild SD=1; moderate SD=2; severe SD=3; complete SD=4) categorical scale (2.9±0.9) of SD. Notably, sexual function was significantly more severely impaired among women as compared to men (74±24 vs. 68±23; p=0.024 and 3.1±0.9 vs. 2.8±0.9; p=0.016,respectively). Pearson's test showed a significant linear correlation (r=0.349; p<0.001) between pain intensity and the degree of SD (both measured on 0-100 VAS) (Figure 2).
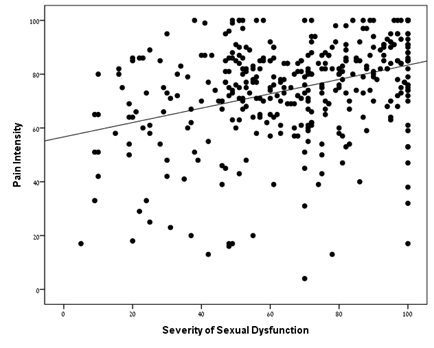
Figure 2 Correlation between pain intensity and the degree of sexual dysfunction (both measured on 0-100 VAS).
Pearson's test showed a significant linear correlation (r=0.349; p<0.001) between pain intensity and the degree of SD (both measured on 0-100 VAS).
|
All Patients |
With SD |
Without SD |
p-value* |
Pain Intensity (VAS) |
68±25 (71) |
70±23 (72) |
50±27 (47) |
p<0.001 |
Mean SF-MPQ score |
14.7±9.9 (12) |
16.5±10 (15) |
12.3±8 (10) |
p<0.001 |
Mean ODI score |
20.5±9.3 (21) |
23.5 ± 8.6 (24) |
16.4 ±8.5 (15) |
p<0.001 |
Use of opioidsn(%) |
216 (31%) |
160 (40%) |
56 (19%) |
p<0.001 |
Use of Antidepressants n(%) |
71 (10%) |
49 (12%) |
22 (7.5%) |
p=0.043 |
Use of Aticonvulsants n(%) |
59 (8.5%) |
45 (11.3%) |
14 (4.8%) |
p=0.002 |
Use of non-opioid Analgesics, n(%) |
460 (66.3%) |
285 (71.3%) |
175 (59.5%) |
p=0.002 |
Table 2 Pain, disability and use of medications by patients with and without SD
*Comparison between patients with and without SD
Data is presented as mean ± standard deviation (median) or number (percentage).
In contrast, no significant correlations were found between any of the other demographic parameters (age, weight, years of marriage) or any other pain scores (verbal pain intensity score, SF-MPQ score) and the severity of SD.
Indepth questionnaires
A subgroup of 134 patients (93 men) of the 404 patients with SD (33%) agreed to complete additional questionnaires aimed to assess the degrees of their depression, anxiety and SD. These questionnaires indicated a mild degree of depression (BDI:16±10 mean±SD; median 15) and a moderate degree of anxiety (BAI:17.1±15; median 13) (Table 3). The severity of SD, measured by the gender specific questionnaires, showed the following: Women scored 15.1±8.4 (median = 17) on the FSFI, whereas men scored 15.3±5.3 (median = 16 ) on the IIEF-EF, indicating moderate SD in both genders.
|
Total |
Men |
Women |
P-value* |
BDI |
16±10 |
15.6±10.5 |
17.4±9.9 |
P=0.34 |
BAI (Anxiety) |
17.1 ± 15 |
16.3±14.6 |
19.1±15.3 |
P=0.35 |
Sexual Dysfunction: |
- |
15.3±5.3 |
15.1±8.4 |
- |
Table 3 Levels of depression, anxiety and SD in a subgroup of 134 patients with SD
*Comparison between genders
Data is presented as mean ± standard deviation.
The first notable finding in the present study was that as many as 67% of the patients who were contacted by mail agreed to provide information about their pain-related sexual function. This is a similar to another mailed questionnaire-based study on post-coronary artery bypass graft (CABG) pain, from our institution, where the response rate was 71%.29 This relatively high response rate is encouraging, given the delicacy of the studied topic (SD) and the fact that this study was part of the first contact between our pain center and these patients. This high response rate probably reflects the distress and the difficulties that exist regarding sexual activity in this group of patients and for the investigators it created a fairly large data-base, a fact that typically contributes to the validity of the study findings.
In agreement with previous studies,9‒15 we found that a high percentage of patients with chronic pain reported having SD (58%). An emphasis should be put on the fact that our patients were inquired specifically about SD related to their pain. Unexpectedly, no differences were found in any of the demographic parameters between those with and without SD. These include factors which generally contribute to SD such as age,30 years of marriage11 or level of education.31 A striking finding is the relatively young age of the studied population (mean of 44 years), yet the reported prevalence of SD in these patients was almost double than that found in age-matched healthy subjects.30 Taking these findings together with the relatively large patient population, suggests that the presence of chronic pain is indeed strongly associated with SD. Based on this, we hypothesize that chronic pain per-se had such a robust negative effect on sexual function that the other factors, which typically contribute to SD, became negligible. This however needs further investigation.
Despite the fact that chronic pain is more prevalent among women than men,32 the total number of questionnaires sent to men and to women was almost identical. Still, the response rate (number of patients answering the question about pain-related SD) was higher among men than women (79.1% versus 54.1%). This may indicate that the former are more prone to discuss sexual-function related issues. It may also imply that SD has a much stronger negative effect on men than on women and they either need to express this or are seeking help. At the same time it is important to emphasize that among the responders, the proportion of men and women reporting SD was almost identical. Furthermore, the self-reported severity of SD (both numerical and verbal) was statistically higher in women than in men, but these differences were small and therefore seem to be clinically insignificant. Thus, taken together, the results of the present cohort suggest more or less similar prevalence and severity of SD among patients with chronic pain, regardless of their gender. Notably, these results are not entirely in line with those of another study showing higher prevalence of SD among women, either healthy or with chronic low back pain, than among men with congruent conditions.14 Yet, in another recent report of 100 patients with chronic low back pain a higher prevalence of SD was found in men than in women.4 Thus, gender differences in the prevalence of SD among patients with chronic pain seem to vary between studies.
Although various medical and mental conditions, such as diabetes mellitus, hypertension, cardiovascular disease32 and depression9,11 are recognized as risk factors for SD, chronic pain is not typically regarded as one of them. The higher levels of pain reported by patients with SD as compared to those who did not report SD in the present study may suggest that chronic pain could also be considered a risk factor for SD, as suggested by others.9‒16 This is strongly supported by the significant correlation between the VAS scores of pain intensity and severity of SD found in the present study. Another potential contributor to interference with normal sexual function is the use of medications such as antidepressants21,22 and opioids.18,19,20,33 In the present study, all four classes of medications (non-opioids, opioids, antidepressants and anticonvulsants) had been used in significantly higher percentages of patients with SD than by those who did not report SD. This finding may suggest that these medications, by themselves, have contributed to SD. However, since many of the patients were taking mixtures of different medications at various doses, we have not been able to formulate a standardization of their medication intake. Therefore, a formal statistical analysis aimed to establish correlative relationships between the use of these medications and SD could not be performed.
A recent systematic review and meta-analysis aimed to identify and examine the extent to which putative mediators explain the effect of pain on disability in patients with lower back or neck pain. The authors suggest that factors such as self-efficacy, psychological distress, and fear significantly mediate the relationship between pain and disability.3 In our study, two psychological distresses have been tested: depression and anxiety. Although depression commonly coexists in patients with chronic pain,1 and is a recognized cause of SD,9,11 surprisingly, the in-depth questionnaire showed, on average, only a low level of depression among these patients. We don't have a clear explanation for this finding by itself. However, the fact that on average, only mild depression was found in that group of patients limits the likelihood that depression was a significant contributor to their SD. The average level of anxiety was higher, in the moderate range, suggesting that anxiety is a possible contributor to SD in these patients. Congruently, the results of a recent study points to a strong association between an anxiety negative trait-affect and sexual functioning in women with sexual problems.34,35
Two shortcomings of this study should be noted. First, of all demographic and clinical parameters tested, pain intensity was the only one which showed a significant correlation with SD. As such, we have not performed any regression analyses and the degree to which each of those parameters contributed to the SD could not be determined in the present study. Second, the potential impact of the SD on the quality of life (QoL) of patients with chronic pain is an important issue which has not been addressed in the present study. It has been investigated in a pilot study on 41 patients with chronic pain, which found that although SD was prevalent, patients perceived it less important than other factors in terms of the degree to which it affected their QoL.11 Based on this finding, one may get the impression that SD in patients with chronic pain has only marginal importance and therefore requires only minimal diagnostic and therapeutic attention, if at all. However, drawing firm conclusions about this issue from a single, small sample sized study would probably be incorrect. Several limitations of this study should be mentioned. First, the patients referred to the Pain Clinic at Rambam health Care Campus, are those who suffer the most severe, chronic and persistent pain and therefore may not represent the 'typical' population of patients with chronic pain. Second, only 33% of the patients with SD agreed to complete the in depth questionnaires, a fact which may have created a bias. This relatively low response rate could be a result of patients' embarrassment and discomfort to expose intimate issues related to SD with the clinic staff.
A significant number of patients with chronic pain suffer from moderate to severe SD. Pain intensity correlates with SD severity. These findings highlight the importance of increasing awareness of SD in patients with chronic pain.
None.
None.

©2017 Gruenwald, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.