eISSN: 2378-3176


Case Report Volume 12 Issue 1
1Department of Urology, Sidi Mohamed Benabdellah Fez, Morocco
2Department of Radiology, Sidi Mohamed Benabdellah Fez, Morocco
Correspondence: Malki Mohamed Amine, Department of Urology, Sidi Mohamed Benabdellah Fez, Morocco, Tel +2126000956067
Received: February 29, 2024 | Published: March 18, 2024
Citation: Amine MM, Asmae S, Bouh KS, et al. Challenges in diagnosing and treating urachal abscess in adults. Urol Nephrol Open Access J. 2024;12(1):12-14. DOI: 10.15406/unoaj.2024.12.00347
Urachal abscess, a rare condition from fetal allantoic canal remnants, presents diagnostic challenges. We report a case in a 40-year-old man, emphasizing clinical, diagnostic, and therapeutic nuances. Imaging aids diagnosis, with prompt surgical intervention following antibiotic therapy. Early recognition is vital to prevent complications. Multidisciplinary management improves outcomes.
Keywords: emphasizing clinical, therapeutic nuances, fetal allantoic canal, leucocytosis
Urachal abscess is a rare condition resulting from incomplete obliteration of the fetal allantoic canal.1 Since the first description by Cabrioles in 1550, few cases of urachal sinuses have been reported in the medical literature, high lighting the rarity of this pathology in adults. Typical symptoms include umbilical discharge, but diagnosis remains difficult due to clinical variability. In this study, we present a case report of urachal abscess in an adult, highlighting the clinical, diagnostic and therapeutic characteristics.
A 40-year-old man, with no relevant medical history, presented with persistent fever for three days, abdominal pain and purulent umbilical discharge, without associated digestive or urinary symptoms. On physical examination, the patient had an initial temperature of 38.9°C, purulent umbilical discharge with erythema and a tender umbilical masse Figure 1. Laboratory tests showed a significant leucocytosis at 16,000/mm3 and elevated C-reactive protein (122 mg/L), while urine analysis and renal function were within normal. Culture of the umbilical discharge revealed the presence of Klebsiella pneumoniae, while blood culture was negative. Abdominal ultrasound showed an echogenic retro-umbilical collection, and computed tomography confirmed the diagnosis of infected urachal sinus, heterogeneous collection, stone formation and gas comminated with the umbilicus Figure 2. The patient was initially treated with broad-spectrum intravenous antibiotics. Subsequently, a complete excision of the fistulous tract en bloc of the urachus with creation of a bladder cuff was performed Figure 3. The postoperative course was uneventful, and histological examination revealed no signs of malignancy.
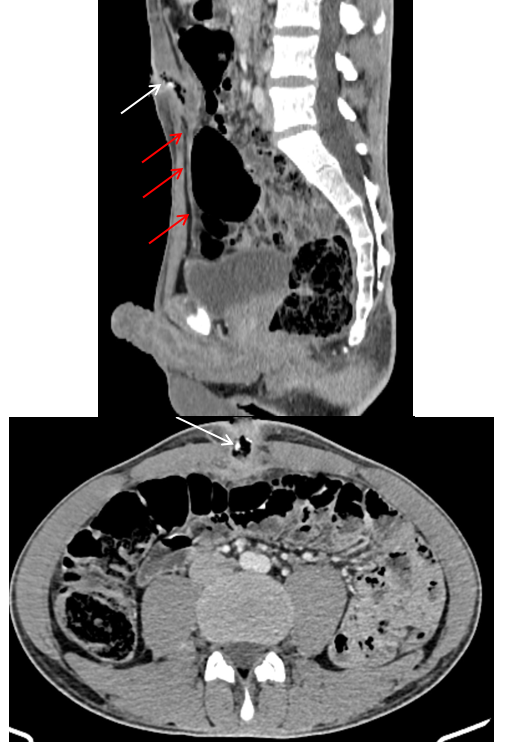
Figure 2 Enhanced abdominal CT scan, in sagittal and axial views, showing a well-defined tubular collection, along the midline, with regular contours, and thick walls. It contains calcifications and air. The collection is a non-communicating dilatation of the urachus (red arrows) at the umbilical end, which is fistulised to the anterior abdominal wall. It measures 40 x 22 mm. The diagnosis was infected urachal sinus.
The urachus is a fibrous remnant of the allantois, a tubular canal between the bladder and the umbilicus through which urine exits the fetus during pregnancy. It generally involutes before birth. Failure of this process leads to a fully or semi-permanent urachal tract,2 and possible formation of the following urachal remnant anomalies - urachal sinus, urachal cyst and vesi coached verticulum.3 Among the mentioned structures, the urachal cyst is most common. Histologically, it consists of three layers: an inner modified transitional epithelial layer similar to urothelium, an intermediate layer of fibrous connective tissue, and an outer layer of smooth muscle continuing with the detrusor of the bladder.4 Clinical manifestations are diverse being asymptomatic and symptoms as infectious or painful complications. In children and adolescents, diagnosis is most often made (62% of cases), while it can be incidental in adults, often after years of atypical symptoms.5
Vesicoumbilical fistulas are generally diagnosed at birth, with urine drainage through the umbilicus or delayed cord stump detachment. Manifestations of urachal sinus include purulent umbilical discharges - commonly isolated microorganisms include Escherichia coli, Enterococcus faecium, Proteus, Streptococcus viridans and Fusobacterium-, erythematous or granulomatous peri-umbilical lesions, sometimes accompanied by fever.6
Urachal diverticula can cause residual post-voiding, two-phase voiding, urinary tract infections or lithiasic complications. Urachal cysts, often asymptomatic, can manifest with non-specific urinary symptoms such as dysuria, pollakiuria or hematuria.7 Suppurations of urachal cysts are common and can lead to severe complications such as peritonitis or Retzius space abscesses.8 Atypical abdominal symptoms can also be caused by intra-cystic infections, hemorrhages or lithiasis. Although rare, fistulisation to the digestive tract can occur, particularly in patients with Meckel's diverticulum.9 While the inner layer of the urachus is mainly composed of transitional cells, adenocarcinoma (mainly mucinous) is the predominant histological type at 69% and 15% are non-mucus secreting and 16% are transitional or squamous cell carcinomas. Very rarely, it could be a sarcoma.10,11 Two theories are proposed for this tumour: the dysplastic and the metaplastic theory. The dysplastic theory suggests the possibility that urachal tumours develop from native digestive germ cells incorporated during embryonic development. The metaplastic theory involves the participation of irritating factors such as infection and reflux in urachal remnants. Imaging plays a crucial role in diagnosing urachal pathologies, as they are generally not accessible to clinical or endoscopic examination. Cystography and fistulography can be useful for diagnosis.12 Cysts and diverticula are diagnosed by ultrasound, showing an anechoic mass on the midline, near the bladder and behind the rectus sheath. Abdominal and pelvic CT scan is the reference examination for diagnosis, allowing visualization of cystic masses in the prevesical space and detailing the wall appearance. Sinuses appear as thickening along the urachal tract near the umbilical area.13,14
The therapeutic approach in our case was antibiotic therapy as first step and then resection of the urachus and its bladder implantation base. Drainage alone is not recommended15 duo to the risk of degeneration on residual tissue. The treatment of reference is complete excision of the fistulous tract. It must remove en bloc the urachus, the lateral umbilical ligaments and a bladder cuff, in this case, through a median sub umbilical incision.16 In conclusion, urachal abscess remains a rare but important condition in urological practice, requiring an understanding of its pathogenesis. Advances in understanding the embryology of the urachal remnant, as well as improvements in surgical techniques and appropriate use of antibiotics, are essential to improve clinical outcomes in patients with urachal abscess.
None.
The authors declares that there are no conflicts of interest.

©2024 Amine, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.