MOJ
eISSN: 2475-5494


Review Article Volume 8 Issue 1
Department of Morphological, Professor at Estácio Castanhal faculty, Brazil
Correspondence: Vanessa Novaes Barros, Department of Morphological, Professor at Estácio Castanhal faculty, Para, Brazil
Received: January 22, 2019 | Published: January 28, 2019
Citation: Barros VN. The heart cycle: review. MOJ Womens Health. 2019;8(1):66-69. DOI: 10.15406/mojwh.2019.08.00214
Cardiac cycle is the expression referring to the events related to the flow and blood pressure that occur from the beginning of a heart beat until the next beat. This events involves atrial and ventricle contraction, shots of autorrhythmic fibers, opening and closing valves, at the cellular level involves depolarization and calcium entry, coupling of contractile proteins such as actin and myosin and so many other events that must work in synergy for appropriate heart function. This article aims to synthetize most important events that are part of the heart cycle.
Keywords: heart cycle, flow, depolarization, calcium, autorrhythmic fibers, temperature, physiology
The heart is a pump that performs 72 beats per minute, equivalent to 1.2 Hertz, which each beat lasts around 0.830 ms (milliseconds) to boost the blood circulation that transports and distributes nutrients and oxygen, maintains the balance of fluids and body temperature as well as removes carbon dioxide and other metabolic byproducts from all cells of the body. Over a year, the heart beats around 38,843,300 times without taking into account the moments of stress and emotion in which the heart rate normally rises. Hence the importance of a system that works 24 hours a day, pumping about 200 million liters of blood (over a life of 70 years) to keep us alive.1 This work aims to synthesize the physiology of the cardiac cycle as well as to point out the main affections after a failure of this cycle.
The heart cycle
Cardiac events that occur at the beginning of each heartbeat until the beginning of the next are called the cardiac cycle. The heart is made up of two pumps in series: a blood supply to the lungs for gas exchange (expel carbon dioxide and oxygen) composed by atrium and right ventricle and another propels blood for all other tissues of the body (called circulation systemic) composed by atrium and left ventricle. The blood travels unidirectionally, due to the presence of valves inside the cardiac cavities which are: tricuspid valve, present at the intersection of the atrium with the right ventricle; mitral valve, present at the intersection of the atrium with the left ventricle; pulmonary valve, present at the intersection of the right ventricle with the pulmonary artery that leads the blood to be oxygenated in the lungs; and aortic valve, present at the intersection of the left ventricle with the aortic artery that carries the oxygenated blood to the systemic circulation. The control of the opening and closing of the valves is by pressure differences (Figure 1).2
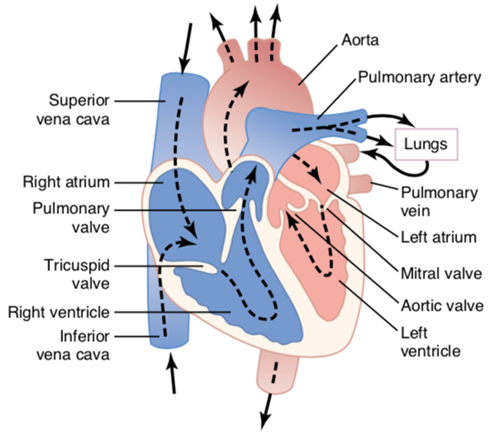
Like a pump, the heart works in two phases: systole and diastole. At systole the right ventricle contracts to eject the venous blood into the lungs so that they are oxygenated, and in the left ventricle contraction ejects oxygenated blood into the entire systemic circulation. This occurs with the closure of the atrioventricular valves (mitral and tricuspid) and opening of the pulmonary and aortic valves. The right ventricle contracts, increases the pressure inside that opens the pulmonary valve leading the blood from the right ventricle to the pulmonary artery. Contralaterally, the left ventricle contracts, increasing pressure by opening the aortic valve leading the blood from the left ventricle into the circulation. In the diastole the relaxation and decrease of pressure in the ventricles occurs, so that the tricuspid and mitral valves open and fill the ventricles with the blood coming from the atrial (Figure 2).2
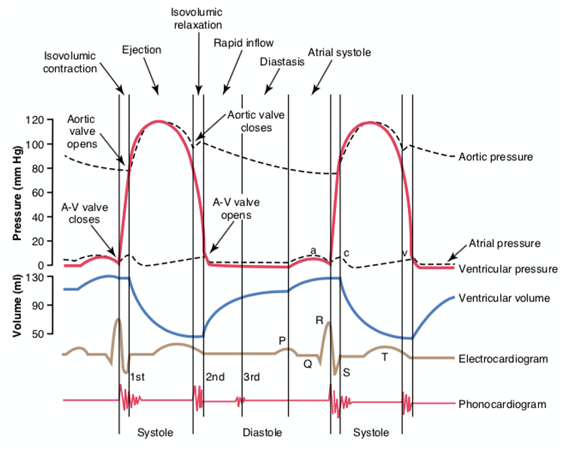
Usually problems with these valves causes valve prolapse; the most common is mitral valve prolapse because of the high pressure inside of the left ventricle. Mitral valve prolapse is defined for American Heart Association as a condition in which the two valve flaps of the mitral valve do not close smoothly or evenly, but instead bulge (prolapse) upward into the left atrium. When the heart pumps (contracts) part of one or both flaps collapse backward into the left atrium. In some cases, the prolapsed valve lets a small amount of blood leak backward through the valve, which may cause a heart murmur. The systole is divided into 3 phases: 1-isovolumetric contraction characterized by the closure of all valves, the ventricles contracts by increasing the pressure (8mmhg right ventricle and 80mmhg left ventricle) to the opening of the pulmonary and aortic valves, respectively. 2-maximum ventricular ejection fraction characterized by the ejection at high pressure (up to 120 mm Hg) of the blood volume to the pulmonary circulation and to the systemic circulation. 3 - Reduced ventricular ejection rate characterized by ejection at lower velocity and pressure, being progressively decreased until the aortic and pulmonary valves close.3
Diastole is divided into 4 phases: 1-isovolumetric relaxation characterized by relaxation of the ventricles without changing the blood volume inside (for a period of 0.03s to 0.06s), since all valves are closed at this time. 2-Rapid diastolic filling characterized by opening of the tricuspid and mitral valves and consequent filling of the ventricles with a slight pressure increase (about 5 mmhg). 3-Slow diastolic filling characterized by the slower flow of sage from the atria to the ventricles due to the slight increase in pressure in the ventricles. 4-atrial contraction, characterized by ventricular filling by contraction of the atria increasing pressure (4-6 mmhg AD and 7 to 8 mmhg AE) by preparing the ventricles for the onset of systole.3 About 70% of the blood volume flows directly from the atria to the ventricles without the atria contracting, the contraction of the atria contributes to the volume increase in the ventricles by only 25%. Therefore, it is said that the atria function as a priming pump. However, the heart can function without this additional 25% because it pumps about 300 to 400% more blood than is required for the body.4
During diastole, the ventricular filling reaches about 110 to 120 ml of blood volume. This volume is called the final diastolic volume. During systole, this volume decreases by about 70 ml, which is called systolic output. The remaining volume in each ventricle (from 40 to 50 ml) is called the final systolic volume. The fraction of the diastolic volume that is ejected is called the ejection fraction, usually equal to 60%. As a result, the increase in final diastolic volume and the decrease in the final systolic volume cause an increase in the systolic output. The amount of blood pumped per minute is called cardiac output.5
During cardiac cycle, atrial pressure variations are characterized by waves a, c, and v. The wave a is due to atrial contraction in the final diastolic phase. The wave c occurs at the beginning of the ventricular contraction, caused by the bulging of the A-V valves and by the small reflux of blood from the ventricles to the atria. The v-wave occurs at the end of systole, while the a-v valves are closed. It results from the slow flow of blood from the veins to the atria (Figure 2).6
Cardiac sounds are called sounds produced during the cardiac cycle. The first heart sound is produced by the closure of the atrioventricular (tricuspid and mitral) valves at the beginning of systole and the second heart sound is produced by the closing of the semilunar valves (aortic and pulmonary) during the onset of diastole (Figure 2). During a cardiac auscultation, the doctor is able to determine in which phase the abnormal sounds are happening, since sounds between the first and second sounds refers to the systole phase, sounds between the second and the first sound refers to the diastole phase.6 Another sound, the third one, is not normal and means that the person has a condition named arrhythmia. The electrocardiogram (ECG) shows waves that reflects the atrial and ventricular polarization and despolarization. After depolarisation of the atria (P wave on an electrocardiogram [ECG]), the atria contract compressing blood in the atrial chambers and push residual blood out into the ventricles. This signifies the last part of the ventricular resting phase (diastole) and the blood within the ventricles is referred to as the end diastolic volume (EDV). The atria then relax and then the electrical impulse is transmitted to the ventricles, which undergo depolarisation (QRS wave on an ECG). T wave refers to ventricular repolarization (Figure 3).
When the person is at rest, the heart pumps up to 6 liters per minute of blood, during exercise this volume can be increased 4 to 7 times. The basic mechanisms by which control of the volume pumped by the heart is regulated are: Intrinsic cardiac regulation of the pumping and regulation by the autonomic nervous system. The intrinsic regulation is due to the mechanism discovered at the end of the 19th century and the beginning of the 20th, called the Frank-Starling mechanism, that is, the larger the volume of blood reaching the heart, the more myocardium is distended during filling, in response to the volume of blood pumped and the contraction force for aorta. This happens due to the optimum interconnection of the actin and myosin filaments for generation of contraction force due to the distension of the muscle at the end of the diastole. Another intrinsic mechanism is distension of the right atrial wall that increases heart rate by 10 to 20%.1
Regarding the autonomic control of the heart, the pumping efficiency is controlled by sympathetic and parasympathetic (also called vagus) nerves that innervate the heart increasing to 100% or decreasing to 0 respectively. Sympathetic SN can increase the frequency from 70 to 200 beats per minute, as well as being able to increase the force of myocardial contraction. Parasympathetic nervous system can decrease heart rate and strength and even suppress heart rate for a few seconds by rapidly returning with a 20-40 min. Because there are many fibers in the atria and few fibers in the ventricles, the parasympathetic nervous system has more effect on the frequency than force of contraction. In general, inotropically positive factors are those that increase heart contractility, which includes: the sympathetic neurotransmitter, noradrenaline, adrenaline, calcium, beta1-agonist drugs, dobutamine, phosphodiesterase inhibitors (caffeine, glucagon, corticosteroids, insulin, angiotensin), drugs that increases intracellular calcium, and physiological effects such as Bowdish effect (described in 1871, homeometric self-regulation mechanism that allows the heart to adapt to changes in heart rate) and Anrep effect (described in 1912, related to variations in pressure developed).7
The heart has a specialized excitatory system formed by the sinoatrial node, which normal rhythmic impulse is generated; the intermodal pathways, which drives the impulse from the sinoatrial node to the atrioventricular node; atrioventricular node where the impulse coming from the atria delays until the arrival in the ventricles; the atrioventricular beam that drives the impulse in the ventricles and the Purkinje fibers that drives the impulse to all parts of the ventricles. This whole specialized system, especially the sinus node, has the capacity of self-excitation producing automatic rhythmic contraction of the heart. Purkinje fibers discharge at a frequency of 15-40 times per minute, the atrioventricular node 40-60 times/min in contrast to the sinoatrial node which discharges about 70-80 times per min, characterizing as our natural cardiac pacemaker (Figure 4). When the message from sinoatrial node doesn’t reach the ventricles happens a condition named atrioventricular block that is a type of heart block in which the conduction between atria and ventricles is impaired. The causes of this disease can be ischaemia, infarction, fibrosis or drugs.
The resting membrane potential of sinoatrial fibers is -55 to -60mV while ventricular muscle fiber is-85 to-90mV. The reason for lower negativity is in the fact that the sinoatrial fibers have potassium efflux channels. In addition, there are open channels for sodium intake as well, causing a continuous increase of the membrane potential even in the resting state. This differential membrane potential inactivates the rapid sodium channels, therefore, only the slow calcium and sodium channels can be activated to produce the action potential when the membrane potential rises to the threshold voltage of -40mV activating the calcium channels and sodium provoking the influx of positive charges into the cell that triggers the action potential. Within 100 to 150 milliseconds the calcium and sodium channels close, and the voltage-dependent potassium channels promote the output of the potassium channel reducing potential to basal levels. As it takes to close, excess of potassium output causes a hyperpolarization (-55 to -60mV), a process reversed by the entry of calcium into the ebbing channels which again raises the potential to-40mV.
The entire action potential of the sinoatrial node passes through the atrial muscle fibers and into the atrioventricular node. The pulse passing through the intermodal pathways reaches the atrioventricular node at 0.03s, however, the passage of this node to the atrioventricular bundle to the ventricles takes about 0.13s along with the initial delay in sinus sleep of 0.03s so that the momentum reaches the contractile muscle of the ventricles there is a delay of 0.16s. In the purkinje fibers, the action potential is extremely fast (velocity of 1.5 to 4 m/s), allowing almost immediate conduction of the cardiac impulse to all the ventricular musculature.6
As previously mentioned, the sinoatrial node, due to the higher frequency of shots, is the heart's natural pacemaker. However in abnormal situations other regions may acquire this task (called an ectopic pacemaker). In the case of a blockade of the conduction of the A-V bundles and node A-V, the atria continue to contract in the sinus node frequency, while the punkinje fibers begin to play the role of pacemaker. However, after a sudden block, the Purkinge fibers take about 5 to 20 seconds to initiate their intrinsic rhythmic impulses, at which time the individual faints due to inactivity of the ventricles and consequent lack of cerebral blood flow. This delayed resumption of heart rate is called Stokes-Adams syndrome. Vagal stimulation (parasympathetic) mainly in the sinoatrial and atrioventricular nodes causes decrease of frequency. The ACH released in the nodes binds to type 1 muscarinic receptors which, through the biochemical phospholipase C cascade, causes the opening of potassium channels, increasing the potassium permeability of the fibers , hyperpolarizing the cells (-65 to -75mV). On the other hand, the sympathetic stimulation provokes an increase in the frequency and the force of contraction by the mechanisms against the vagal. Norepinephrine binds to beta 1 receptors and, through the biochemical cascade of adenylyl cyclase, causes the opening of calcium channels, depolarizing the cell.
Recent studies published by the Institute of Biomedical Sciences of USP indicate that alcohol in moderate dose has cardioprotective effect due to the activation of a mitochondrial enzyme ALDH2, which helps to eliminate from the organism both toxic byproducts of alcohol metabolism and reactive molecules produced by the cardiac cells when these suffer some major damage (such as that caused by the heart attack, for example). The heart is a vital organ to stay alive. Similar mechanical pumps are invented and built to play the role of the heart in patients, but no mechanical pump can perform the role of the heart in a 100% satisfactory and long-lasting way. As much as we know about heart physiology more chance we have to discover treatments for heart diseases or how to avoid it.
None.
The author declares there are no conflicts of interest.

©2019 Barros. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.