MOJ
eISSN: 2475-5494


Research Article Volume 11 Issue 2
1Students of the Biomedicine Course- Faculty of Biomedical Sciences of Espírito Santo, Brazil
2Professor of the Biomedicine Course- Faculty of Biomedical Sciences of Espírito Santo, Brazil
Correspondence: Afrânio Côgo Destefani, Professor of the Biomedicine Course- Faculty of Biomedical Sciences of Espírito Santo, Cariacica/ES, Brazil
Received: December 09, 2022 | Published: December 22, 2022
Citation: Aguilar AC, Silva M, Rodrigues RO, et al. Evaluation of the use of micro needling associated with the drug delivery system for the treatment of Melasma. MOJ Women’s Health. 2022;11(2):59-61. DOI: 10.15406/mojwh.2022.11.00306
Melasma is a chronic and unsightly dermal pathology responsible for a high demand for aesthetic treatments. It can be caused by excess melanin in the epidermis, commonly exhibiting symmetrically distributed brown or gray macules, with a predilection for the face. It is more common in women than men, usually begins between the ages of 20 and 40, and can lead to considerable embarrassment and distress. The present work aims to evaluate the effectiveness of microneedling associated with drug delivery in the treatment of this dysfunction. This is a narrative bibliographical review whose research was carried out from the descriptors “Melasma”, “microneedling”, “drug delivery system” and “treatment”. The Boolean operator "AND" was used in the PubMed and Scielo databases; including works in Portuguese and English published in the last 10 years, excluding bibliographic reviews. Isolated microneedling can lighten skin spots in patients with recalcitrant melasma. The trauma caused by the procedure should be modest and the use of whitening actives and sunscreen after the procedure becomes mandatory. Despite some proposed theories, the exact mechanism of skin lightening is still not well established. The effect of the technique drug delivery system tends to flexible results. The findings of this review confirm positive results, especially when associated with whitening actives, which considerably increase skin rejuvenation, the treatment of scars and hyperchromia (melasma). New controlled studies are needed to clarify the mechanism of action of microneedling in melasma.
Keywords: melasma, microneedling, drug delivery system and treatment
Melasma is a chronic pathology caused by increased production of melanin in the epidermis where it appears more frequently in the form of brown to gray macules, symmetrically distributed as reticulated spots tending to the face, in some more unusual cases it may appear in other regions of the body, being classified into four subtypes in relation to the depth of melasma: epidermal, dermal, mixed or undetermined.1
It should be noted that melasma is a chronic and unsightly pathology, responsible for a high demand in clinics for aesthetic treatments to resolve this dysfunction. This can be explained by the fact that in some cases it is considered a problem that affects self-esteem and emotions, generating greater problems, compromising the individual's social life due to dissatisfaction with appearance,2 although the pathology is predominant in females of childbearing age, it can affect all types of skin.3
Treatments with topical and oral depigmentants and antioxidants, chemical peelings, microneedling and the Q-Swchited 1064 laser are used to alleviate the effects caused on the epidermis resulting from melasma.4 Microneedling emerged in Germany in the 1990s, but was not known until 2006. It is a device with rollers coated with thin surgical stainless steel or titanium needles of various lengths.5
The procedure using microneedling has advantages such as stimulating collagen without promoting ablative effects on the skin. Healing takes place in a short period of time and there is little chance of side effects compared to other ablation techniques as it makes the skin denser and more resistant.
Compared to other technologies available on the market, the technique has an affordable cost with low cost when compared to other treatments, since the disadvantages are related to specialized training and specific training, because, depending on the depth of the needle, time is needed greater recovery; therefore, to avoid false expectations of the final result, a careful evaluation by the professional is necessary.6,7
The objective of this study was to evaluate the application of microneedling in relation to drug delivery systems for the treatment of melasma, explain the facial dysfunction resulting from the pathology, and explain the microneedling technique and its importance in facial aesthetics and its results.
This is a narrative bibliographic review built from the search for articles in the PubMed and Scielo databases, on the theme of evaluating the benefits of microneedling associated with the drug delivery system.
Articles in Portuguese and English that comprised a time span of 10 years (2011 to 2021) were used. The Boolean operator “AND” was used for the following keywords “Melasma”, “microneedling”, “drug delivery system” and “treatment”. Bibliographic reviews were excluded.
The five phases described by Arksey and O'Malley followed, which consisted of: (1) identifying the research question; (2) identify relevant studies; (3) select the studies; (4) data organization; and (5) collate, summarize, and report the results.
After screening the databases, four articles were found. However, when applying the inclusion criteria, they did not meet the methodological requirements of this review work.
However, in order to enrich the debate, we observed that by inserting the word microneedle in the search terms, we obtained a literary base that we will discuss below.
According to Saraiva, et al.3,4 melasma is still a dermatological challenge, especially due to its recurrence and particularity causing aesthetic damage to the patient, therefore, the search for new therapeutic modalities and active associations seek to enhance the beneficial effects and minimize undesirable systemic effects, maintaining efficacy and security. This effect, Pitassi, et al.8 describe the use of tranexamic acid, hydroquinone, sofora-alpha rucinol and ascorbic acid in the whitening technique of microneedling associated with drug delivery in patients with recalcitrant melasma. According to Kalil et al.9 this technique can contribute to skin rejuvenation, the treatment of scars and hyperchromia (melasma). Saraiva, et al.3,4 aims to induce the remodeling process including neocollagenesis and neoelastogenesis, leaving the epidermis considerably intact, proving to be effective in reducing the melanic pigmentation of the epidermal tissue. Leading to increased skin permeability for 48 hours, this time can be extended with occlusion, which delays the restoration of the stratum corneum, considering that the substances are water-repellent and anhydrous in nature. The synthesis of melanin through the combination of actives and mechanisms of action, can contribute to the whitening of the hands and face.9 A similar result was observed by Kalil et al.9 Among the numerous studies carried out, the one by Aust et al.10 who presented, after eight weeks of microneedling associated with vitamins A and C, obtained an increase of 140% in the thickness of the epidermis when compared to the use of the isolated antioxidant that the increase was of 22%. According to Kalil et al.,9 has several factors that affect skin permeability to ionization, concentration, liposomes or nanoparticles that are linked to drug properties. In addition to the hydrophobic characteristics of the vehicle.
El-domyati et al.,11 studied the effect of facial rejuvenation with 1 mm needles in 10 patients who received 6 sessions of microneedling, with an interval of two weeks between sessions of papillary dermis. After the course of treatment, the patient developed erythema and edema, which subsided after two days.
Budamakuntla et al.,12 good results were also obtained with the use of microneedling associated with tranexamic acid (whitening) with drug delivery in patients with moderate to severe melasma compared to topical treatment alone. The same asserts Lima et al.,6,7 studies carried out in patients with melasma who underwent two sessions of microneedling, with 1.5mm needles with an interval of 30 days, however, in this study there was an association of Kligman's triple formula (Triluma®) and broad spectrum photoprotector (Figure 1). The improvement of melasma in all participants was visible, considering the better quality in the smoothness, texture and brightness of the skin, increase in the thickness of the epithelium, decrease of melanin in the epidermis and increase in the density of collagen in the superficial dermis, as observed in the microscopy of Figure 2.
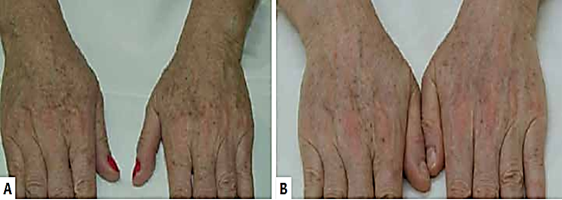
Figure 1 Hands before (A) and 30 days after (B) the last microneedling session with a 1.5mm roller. In addition to whitening the region, it is possible to observe an improvement in the texture and quality of the skin.9

Figure 2 A-B: Pre-treatment biopsy of a patient with phototype II. In this image, histology shows a significant number of melanocytes in the basal layer of the skin. Images were stained with Hematoxylin & Eosin (original magnification 40x);
C-D: Histological analysis three months after treatment suggests a reduction in the number of melanocytes with improvement in skin pigmentation in the areas treated with microneedling. The melanin reduction seems to be relatively homogeneous in the evaluated epidermal extension (original magnification).8
Braghiroli, C. S., & Conrado, L. A,13 describe the advantage of microneedling as being tolerable by patients, the possibility of increasing the transepidermal distribution of drugs through drug delivery, practicality and safety in use in higher phototypes.
Pitassi, et al.,8 understands as an advantage the stimulation of the body's own regenerative mechanisms, percutaneous induction of collagen with microneedles resulting in the partial breakdown of the skin barrier and the release of cytokines such as interleukin 1-alpha, interleukin 8, interleukin 6. After injury, a matrix of fibronectin forms and collagen begins to be deposited, initially consisting of type III collagen, which is later replaced by type I collagen.
Despite several advantages AGOSTINHO et al.,14 reports that melasma is a chronic condition that is often resistant to treatment. Despite the multiple treatment options, complete control of the pathology and long-term remission remain a challenge.
It is known that the combined use of microneedling with drug delivery increases the chance of treatment success, being a promising technique for recalcitrant melasma, but its mechanism of action as a bleaching agent has not yet been fully elucidated.
Studies carried out based on this research point out that the use of the microneedling technique combined with drug delivery tends to have satisfactory results in lightening the pathology, in addition to skin rejuvenation.
Many studies have shown that the tolerability of the procedure is safe and recovery is fast, considering that it is safe to perform in any phototype. It’s understands that the technique is promising, safe and effective, the treatments still remain challenging because it is a chronic and resistant pathology.
Consequently, the effect of the effective drug delivery system technique and the findings of this review confirm positive results, especially when associated with whitening actives, considerably increasing the whitening of hyperchromias caused by melasma. However, there is a need to enrich the literature with more research on the subject, to develop strong techniques for eliminating melasma.
None.
The authors have no conflict of interests related to this study.

©2022 Aguilar, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.