MOJ
eISSN: 2381-179X


Case Report Volume 13 Issue 1
Student Research Committee, School of Medicine, Mazandaran University of Medical Sciences, Sari, Iran
Correspondence: Mehran Frouzanian, Student Research Committee, School of Medicine, Mazandaran University of Medical Sciences, Sari, Iran, Tel +989359397551
Received: January 25, 2023 | Published: March 23, 2023
Citation: Frouzanian M, Jafarpour H, Razavi A, et al. Multiple sclerosis and COVID-19 as two triggers of conjunctivitis: a case report. MOJ Clin Med Case Rep. 2023;13(1):17-19. DOI: 10.15406/mojcr.2023.13.00428
Introduction: Severe acute respiratory syndrome coronavirus, first identified in 2019, can present with atypical clinical features such as conjunctivitis. Furthermore, multiple sclerosis, the most common demyelinating disease, can present with ocular manifestations. Studies and reports regarding this issue still need to be included.
Case description: This article presented a rare case of eye redness and conjunctivitis in a COVID-19 patient with a previous history of multiple sclerosis. Symptoms occurred while the patient was complaining of pulmonary symptoms. Severe conjunctivitis was noticed during the physical examination. Levels of liver enzymes and inflammatory biomarkers were mild, and D-dimer levels were extremely elevated. The patient was hospitalized for five days and was prescribed empirical antibiotics and steroids, which showed improvement. Although COVID-19 with conjunctival symptoms is mostly self-limiting, interventions are based on the patient’s disease course. What was noticeable in this case is the concurrency of multiple sclerosis and COVID-19, which would be a significant trigger for conjunctivitis and hospitalization.
Conclusion: COVID-19 and multiple sclerosis could be risk factors for conjunctivitis, exacerbation of ocular symptoms, and higher hospitalization rates. Furthermore, conjunctivitis could be the sole clinical presentation of COVID-19, and it is primarily self-limiting and resolves within a few days. Therefore, close observation and monitoring should be taken by medical staff.
Keywords: COVID-19, conjunctivitis, ocular symptoms, multiple sclerosis
Coronavirus Disease 2019 (COVID-19), which is a newly identified and highly contagious infection that originated in China in late 2019,1 caused a catastrophic pandemic around the world and various negative impacts on many economies and global order.2 World Health Organization (WHO) declared it a pandemic in March 2020 due to its highly transmissible capability and danger. At the time of this writing,3 over 6 million deaths have been reported by WHO.4
In healthcare settings, good hygiene practices and awareness are critical in preventing the spread of COVID-19. Some measures that can be taken include: 1 Personal protective equipment (PPE): Healthcare workers should wear appropriate PPE, including masks, gloves, gowns, and face shields or goggles, to reduce the risk of transmission. 2 Hand hygiene: Frequent hand washing with soap and water for at least 20 seconds or use of alcohol-based hand sanitizers is important in preventing the spread of the virus. 3 Disinfection: Regular disinfection of surfaces and equipment, including door handles, bed rails, and medical equipment, can prevent the spread of the virus. 4 Social distancing: Maintaining a physical distance of at least six feet between individuals can help prevent transmission. 5 Screening: Healthcare facilities should screen patients and visitors for symptoms of COVID-19 before entering the premises to prevent the spread of the virus. 6 Education: Healthcare workers should receive education on COVID-19 prevention, including good hygiene practices and recognizing symptoms of the virus.5
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) comes from the Coronaviridae family and infects Angiotensin-converting enzyme 2 (ACE2)-expressing cells which are located in many organs and tissues throughout the body (bone marrow, oral and nasal mucosa, nasopharynx, spleen, skin, lungs, stomach, intestines, brain, kidney and liver).6 So, this variation in ACE2 receptor locations could allow SARS-CoV-2 to involve as many organs as possible.
In this paper, we present a case report of a young woman with a previous history of multiple sclerosis presenting acute conjunctivitis diagnosed with COVID-19 and the coincidence of numerous sclerosis and conjunctivitis which in this case is considerable. It is crucial for healthcare workers and personnel to be familiar with less common and atypical cases of COVID-19 and its different presentations, especially at the beginning of the illness, for a better prognosis.
A 36-year-old woman presented to our clinic with a sore throat, fever, and chills on February 22, 2022. She was suffering from complaints of left eye pain, swelling, warmth, and redness. Eye and conjunctiva examinations showed no double vision, no blurred vision, and had inflammation, swelling, and erythema in the left conjunctiva. The right eye examination was normal. The diagnosis of acute conjunctivitis was confirmed (Figure 1).
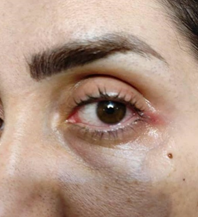
Figure 1 Image of the patient showing left eye redness and congestion demonstrating conjunctivitis, especially on lateral side of the eye.
The patient was a known case of multiple sclerosis (MS), which was diagnosed ten years ago with foot tingling symptoms and had not recurred since then, and she was not on disease-modifying therapies. She had no prior COVID-19 infection since the beginning of the pandemic and had receivedtwo2 doses of the Sinopharm BIBP COVID-19 vaccine. In addition, she has been using eyeglasses since she was an adolescent, and no history of diabetes mellites and hypertension, or any other significant underlying medical conditions was reported. Before hospital admission, she had not been using any specific drugs except acetaminophen and diphenhydramine. The patient appeared well on examination, and her blood pressure was 110/80 mmHg, temperature 36.8 °C, pulse 84 beats per minute, respiratory rate 18 breaths per minute, and oxygen saturation 97% when she was on nasal cannula. The body mass index (BMI) was 25.09 kilogram/meter 2. She did not use tobacco, drink alcohol, or illicit drug abuse.
This patient's ESR and CRP levels were elevated, which were consistent with acute inflammation. The D-dimer level was markedly, and Liver enzymes were mildly elevated. Other laboratory data were within normal limits. She was hospitalized after the symptoms worsened. Nasopharyngeal swabs were used for sampling, and SARS-CoV-2 nucleic acid was detected by reverse transcription-polymerase chain reaction test (RT-PCR). Lung CT scan was ordered and showed bilateral ground glass opacity involving approximately 30 percent of the lungs. Other system evaluations were normal, with no significant findings observed (table 1).
Variable |
During admission |
Reference range |
Hematocrit (%) |
39.8 |
41.0–53.0 |
Hemoglobin (g/dl) |
13.2 |
13.5–17.5 |
White-cell count (per μl) |
7000 |
4500–13,000 |
Differential count (%) |
||
Neutrophils |
62.7 |
40.0–62.0 |
Lymphocytes |
29.6 |
27.0–40.0 |
Platelet count (per μl) |
248,000 |
150,000–400,000 |
Sodium (mmol/liter) |
145 |
135–145 |
Potassium (mmol/liter) |
4 |
3.4–4.8 |
Phosphorus mg/dl |
3.1 |
2.8-4.5 |
Calcium (mg/dl) |
8.9 |
8.5–10.5 |
Urea nitrogen (mg/dl) |
19 |
24-Jun |
Creatinine (mg/dl) |
1 |
0.60–1.50 |
Alanine aminotransferase (U/liter) |
63 |
10–55 |
Aspartate aminotransferase (U/liter) |
45 |
10–40 |
Alkaline phosphatase (U/liter) |
252 |
44-147 |
Albumin (g/dl) |
4.7 |
3.3–5.0 |
Erythrocyte sedimentation rate (mm/hr) |
45 |
0-22 |
C-reactive protein (mg/liter) |
77.1 |
0-10 |
D-dimer (ng/ml) |
1450 |
0-500 |
Creatine phosphokinase (IU/liter) |
100 |
20-120 |
Table 1 Laboratory data
She received sulfacetamide, tetracycline, and betamethasone for acute conjunctivitis and COVID-19 treatment during her hospitalization. The patient appeared well on the last day of admission and was discharged after five days of hospitalization with complete recovery.
COVID-19 transmission is highly dependent on the interaction between the host cell ACE2 receptors and SARS-CoV-2 viral spike proteins, like the SARS-CoV, a previous member of the Coronaviridae family.7 So, the efficiency of this interaction is the critical factor for viral transmission. SARS-CoV2 enters the host cell via the ACE2 receptor and replicates within the cells. Transmembrane serine protease 2 (TMPRSS2) is an enzyme with serine protease activity, and SARS-CoV-2 utilizes ACE2 for the entry and uses TMPRSS2 to prime the spike protein. Willcox et al. found both ACE2 and TMPRSS2 in corneal epithelial and conjunctival cells, allowing the virus to gain access through this site.8 However, the ocular transmission route forms a small percentage of the daily and routine transmission of the virus. Furthermore, there are not enough studies to illustrate whether this method of viral transmission is related to the clinical manifestations of eye inflammation and conjunctivitis. ACE2 receptor is also found to be expressed in a wide range of different tissues and organs like the lung (type 2 pneumocytes), brain, kidney, colon and intestine, esophagus, heart, and thyroid,9 which could suggest why there are a wide variety of clinical manifestations of COVID-19 illness.
Previous studies have found that laboratory abnormalities can occur in COVID-19 patients. These include the elevation of inflammatory markers like ESR and CRP, liver enzymes, alkaline phosphatase, and D-dimer levels.10 Elevation of these markers is associated with a worse prognosis.11 Although this patient had some of these laboratory abnormalities, especially the D-dimer level, she did not have a complicated illness and was discharged home after five days of hospitalization. Another study found that COVID-19 patients who had ocular involvement had significantly high levels of CRP and ESR, probably due to the active inflammation and immune reaction12 consistent with our case. Layikh et al. found that there was no correlation between conjunctivitis and elevated levels of biochemical markers like D-dimer, WBC count, and CRP,13 unlike our case, which presented with markedly elevated D-dimer and mildly elevated CRP levels. Further evaluations are recommended if these biomarkers' elevation persists after the recovery from COVID-19. Although these biomarkers lack specificity or sensitivity in many cases, monitoring the levels of ESR and CRP is a beneficial tool for physicians to diagnose and manage a wide variety of inflammatory and pathological conditions.
SARS-CoV-2 can cause a wide range of ocular symptoms, from mild conjunctivitis and anterior uveitis to vision-threatening disorders such as retinitis.14 Multiple previous case studies have reported that conjunctivitis could be the only sign of SARS-CoV-2 infection, without any other typical manifestations of COVID-19 illness.15 Hence, physicians must consider conjunctivitis as an initial or possible sign of COVID-19 infection. Blurry vision in a case of conjunctivitis during COVID-19 infection is not shared and is very rare, similar to our case, and in a previous report of 35 patients with conjunctivitis, none of them presented this symptom.16 The role of conjunctivitis in diagnosing and treating COVID-19 patients is probably underrated. This factor can be utilized to predict the COVID-19 infection course. One study concluded that ocular involvement was associated with more viral load, longer COVID-19 disease courses, and extended hospitalization.17
A more severe ocular presentation of this virus is retinopathy. Gascon et al. reported a case of a 54-year-old male with retinopathy and acute vision loss associated with COVID-19 infection.18 Another report demonstrated a 40-year-old female with COVID-19 positive test, myalgia, and fever with significant vision loss.19 To prevent any further vision-threatening conditions, constantly monitoring COVID-19 patients with ocular manifestations is necessary. It is essential to consider that this patient’s history of multiple sclerosis may also be associated with her conjunctival manifestations and even exacerbated the condition.
Conjunctivitis is common among multiple sclerosis patients.20 It is possible that our patient's eye symptoms were due to his underlying disease, multiple sclerosis, and not COVID-19. However, it seems that the synchronicity of COVID-19 and multiple sclerosis have increased the risk of conjunctivitis. It is self-limiting, and most cases resolve in a few days. Treatment requires supportive therapy, although close monitoring and frequent eye examinations are necessary. We know that COVID-19 is found to be associated with the cytokine release and even inflammation seen in elevated levels of ESR and CRP, which would justify the use of steroids, as was done in this case.21
Conjunctivitis could present as the first clinical presentation of COVID-19 or anytime during the illness. Furthermore, COVID-19 and multiple sclerosis could be risk factors for conjunctivitis, exacerbation of ocular symptoms, and higher hospitalization rates. Conjunctivitis is primarily self-limiting and resolves within a few days. Therefore, close observation and monitoring should be taken by medical staff.
None.
As the manuscript is not a research study, we only have the patient consent for writing and other forms of publication. Also, the ethical approval for this case report has been exempted by our institution.
Written informed consent was obtained from the patient to publish this case report and accompanying image.
The manuscript is a case report, not considered formal research involving participants.
The authors report no conflicts of interest.

©2023 Frouzanian, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.