MOJ
eISSN: 2381-179X


Case Report Volume 13 Issue 1
1Department of Neurosurgery (Omori), School of Medicine, Faculty of Medicine, Toho University, Japan
2Department of Neurosurgery, Saiseikai Yokohamashi Nanbu Hospital, Japan
Correspondence: Ryo Matsuzaki, Department of Neurosurgery (Omori), School of Medicine, Faculty of Medicine, Toho University, 6-11-1, Omori-nishi, Ota-Ku, Tokyo 143-8541, Japan, Tel +81-3-3762-4151
Received: February 11, 2023 | Published: February 22, 2023
Citation: Matsuzaki R, Noguchi Y, Aoki Y, et al. A case of endoscopic treatment of a symptomatic pineal cyst. MOJ Clin Med Case Rep. 2023;13(1):9-11. DOI: 10.15406/mojcr.2023.13.00426
Pineal cysts are frequently discovered by chance on magnetic resonance imaging (MRI) and are typically asymptomatic. However, hydrocephalus may develop and show symptoms when the cyst in the ventricles acts as an obstruction mechanism. We herein present a case involving a 52-year-old man with hydrocephalus due to the pineal cyst, who was effectively treated by an endoscope. He was transported by emergency with a chief complaint of impaired consciousness. At the time of admission, Glasgow coma Scale E4V4M6 was found, hydrocephalus with an Evans Index of about 0.3 was observed on the head computed tomography (CT), and a cystic lesion was observed on the pineal gland on the MRI During surgery, we tore the pineal cyst’s wall using forceps since it was blocking the aqueduct. Furthermore, an endoscopic third ventriculostomy was added in preparation for the recurrence of postoperative cerebral aqueduct obstruction. His awareness returned after the procedure, and he was released with no neurological damage. We believe that neuro endoscopic surgery is becoming the first choice for symptomatic pineal cysts because it is minimally invasive and safe.
Keywords: pineal cyst, hydrocephalus, endoscopic third ventriculostomy, aqueduct obstruction
MRI, magnetic resonance imaging; CT, computed tomography, ETV, endoscopic third ventriculostomy
The pineal cyst is a benign cyst that occurs in the pineal gland and has recently been found by MRI which occurs most often in women in their twenties.1 The pineal cyst is usually asymptomatic but rarely presents with symptoms such as headache, ocular motility disorder, fainting, and in some cases sudden death.1 As a treatment method, the effectiveness of neuro endoscopic surgery has been recognized as a new means to replace conventional craniotomy and stereotactic suction surgery. This time performed cyst-release surgery with a neuroendoscope and obtained good results, so we report it with a review of the literature.
A 52-year-old man with a headache and consciousness disturbance was taken to our hospital by ambulance. He had a history of thrombocythemia and was taking aspirin. At the time of the visit, his consciousness was GCSE4V4M6, and displayed an upward gaze disorder. Computed tomography (CT) at the first visit revealed ventricular enlargement and a cyst with calcification in the pineal gland. Additionally, ventricular enlargement was visible on MRI, and a pineal gland cystic lesion with a wall thickness of 15 mm was discovered. The signal inside the cyst was lower than that of the surrounding brain parenchyma and higher than that of the cerebrospinal fluid. The cyst wall was thin and smooth, and no septal structure or nodules were discovered inside, so we diagnosed a pineal cyst. The operation was performed under general anesthesia, trepanned on the right frontal mid-pupillary line and in front of the coronal suture, and a transparent sheath was placed and a flexible scope was inserted. The cerebral aqueduct intermittently became blocked as the cyst floated in time with the cerebrospinal fluid flow. With forceps, the cyst wall was ruptured, releasing a fluid with a pale yellowish serous content. When about half of the cyst wall was removed, it was validated that the cyst had originated from the pineal gland, and the cerebral aqueduct became observable, so we decided to finish the cyst wall removal. Furthermore, we conducted an endoscopic third ventriculostomy, and pulsatile movement of the third ventricular floor was observed. The operation improved the ocular motility disorder and consciousness disorder, and the ventricles shrank on CT. Postoperative MRI revealed that the cyst wall was discontinuous, and the stoma of the third ventricle was also verified. After the surgery, the postoperative course was uneventful and he was discharged on the 8th postoperative day without complications. Ventriculomegaly was not found. on MRI six months after the operation.
Pineal cysts were discovered in all age groups, and Al-Holou et al. observed pineal cysts 5 mm or larger in 478 (1%) of 48417 patients on MRI, of which 316 were female.2 He also states that there is little increase in size and that follow-up is not required for asymptomatic patients.2 Nevins et al. also followed 281 cases of pineal cysts, stating that no cases became symptomatic, and that follow-up could be completed only 12 months after the initial indication.3 Although the course is often benign, it can occasionally be symptomatic (Figure 1-5).4
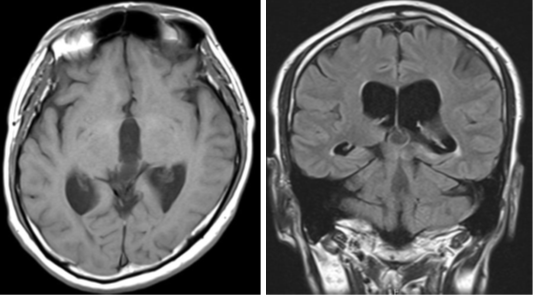
Figure 2 On magnetic resonance imaging, the cyst's signal inside the cyst was stronger than that of the CSF fluid and less strong than the surrounding brain parenchyma and higher than that of the cerebrospinal fluid.
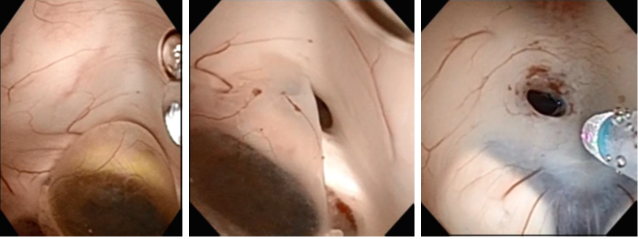
Figure 3 Endoscopic image before tearing the cyst (a) after tearing the cyst, (b) Endoscopic image of the third ventriculostomy.

Figure 5 Postoperative magnetic resonance imaging showed the perforated area of the cyst (arrow), and third ventricle (arrowhead).
Since the pineal gland is involved in hormone production, hormone secretion deficiency due to pineal gland dysfunction causes early puberty, hypogonadism, and diabetes insipidus.1 Although headache is the most prevalent symptom, Parinaud's syndrome from compression of the midbrain and hydrocephalus from obstruction of the cerebral aqueduct may also be present.1
VariousDifferent theories have been put forward regarding the mechanism of development, including remnants of the embryonic period, necrosis products due to ischemia, increase due to bleeding, and hormone involvement, all of which are controversial.5
CT displayed calcification along the wall in 25%–33%, and small lesions may be missed.1 A typical pineal cyst has a uniform, thin wall, and the content fluid reveals isointensity to hyperintensity on T1-weighted and T2-weighted images.1
According to Májovský et al., 21 symptomatic pineal cysts were surgically removed using a microscope, and 20 of them (95.2%) reported some improvement in their presenting symptoms.4
Also conducted craniotomy in 60 cases and showed improvement in symptoms in 59 cases.6 However, high invasiveness is a problem in craniotomy. Stereotactic puncture has a concern with its high recurrence rate. In recent years, neuroendoscopy has gained popularity as an alternate kind of therapy. With a neuroendoscope, the most suspicious part can be submitted as a sample while avoiding the part where blood vessels are abundant under visual inspection.7 The ability to execute ETV simultaneously is another benefit over previous surgical procedures.7
In this case, a pineal cyst obstructed the aqueduct, and the inlet to the aqueduct was detected by tearing it with forceps. At that point, the flow of CSF was already secured, but additional ETV was conducted. Fritsch et al. reported that 11.5% of patients with occlusive hydrocephalus caused by brain tumors or cysts had residual hydrocephalus after tumor removal, indicating that lesion cyst removal alone may not be sufficient.8
None.
The authors declare that there is no conflict of interest.

©2023 Matsuzaki, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.