MOJ
eISSN: 2381-179X


Groin contracture is a common complication of burn and causes functional disability by restricting extension and abduction of hip. As the normal resting position of groin region is in flexion, these contractures are difficult to prevent. They also remain a difficult problem to treat as they recur frequently and multiple operations are often required. The goal of management of groin contracture is to provide maximum release with minimum or no local anatomic distortion. Various surgical techniques that have been used include skin grafting, Z plasties (single and multiple), fasciocutaneous and myocutaneous flaps. In this article we describe a novel perforator-based fasciocutaneous flap for the management of groin contracture and describe the anatomical basis of the flap.
A 16-year-old girl presented with bilateral scar contracture of her groins. She had sustained a flame burn six years back and received only rudimentary medical care for her acute burn injuries. On examination, she had difficulty in abducting and extending her hips. Her inguinal regions and anterior thighs were extensively scarred bilaterally (Figure 1).
The contractures were released up to the healthy subcutaneous fat. This created wide defects in both the groins. The right side was addressed first. Doppler examination revealed a number of perforators in the upper third of medial thigh. A 12cmx6cm flap was drawn on the medial thigh based on a dominant perforator about 5cm below the inguinal ligament (Figure 2). The lateral margin of the flap was incised first and the gracilis identified. The flap was dissected medially in the subfascial plane till the medial border of gracilis was reached. Here a vertical row of perforators were identified. The medial margin of the flap was then incised and dissection proceeded up to the aforesaid perforators. The flap was based on a single perforator located about 5cm below the pubic tubercle, and the rest of the perforators were legated (Figure 3). The flap was rotated into the defect and the donor site closed primarily. A similar procedure was adopted to resurface the left groin defect, where the dimensions of the flap were 15cmx8cm (Figure 4).
The flaps survived on both sides without any complication, and there was no donor site morbidity. The functional results are satisfactory at one year follow up (Figure 5) and there has been no contracture recurrence to date.
The medial aspect of the thigh is supplied by a series of cutaneous arteries. .Approximately 90percent of the upper medial thigh perforators originate from the medial femoral circumflex artery, and the other 10percent from the first profunda perforator or directly from the femoral artery. They arise from the deep plane and pass between the adductor longus and gracilis and divide into several divergent branches Detailed1,2 anatomical study of the medial thigh region by Peek et al.,3 have demonstrated these perforators are septocutaneous in 84 percent cases and musculocutaneous in the rest. Our flap is based on one such septocutaneous perforator which is constantly present about 5cm below the pubic tubercle.
Various procedures have been described for the reconstruction of post-burn groin contractures. Skin grafting, albeit being the most common procedure, is usually unreliable due to significant risk of contracture recurrence, and also requires prolonged splinting and immobilization. Z-plasties (single, multiple e.g. seven flap pasty) and local transposition flaps are only suitable for linear band contractures.4 The musculocutaneous flaps, e.g., gracilis and rectus abdomens, have the disadvantages of excessive bulk as well as higher risk of donor site morbidity. Hence, local fasciocutaneous flaps are preferred for release of groin contractures, the choice of which depends upon the extent of skin scarring in the adjacent thigh area. However, only two such flaps have been described in literature. The anteromedial thigh fasciocutaneous flap described by Baek5 has been used by Hayashi and Maruyama6 for reconstruction of soft tissue defects of groin.5,6 This flap is based on a branch of the superficial femoral artery passing round the supero-medial border of sartorius in the apex of the femoral triangle.7 However, the anteromedial thigh flap is not suitable in the presence of the extensive burn scarring of the anterior or anteromedial thigh skin1 as in our case.
The medial thigh fasciocutaneous flap is a transposition flap described by Wang et al.,7 based on the presence of a communicating suprafascial vascular plexus in the medial thigh. Turley et al.,4 reported lateral transposition of the same flap to release post-burn groin contractures. The flap described in the present article is a novel fasciocutaneous island flap having a unique vascular basis different from the flaps previously described. Our flap is based on a dominant septocutaneous perforator in the inner medial thigh, located about 5 cm below the pubic tubercle at the medial border of gracilis. The perforator was found in the same location bilaterally with the help of Doppler, thus enabling a single-stage reconstruction of groin contracture on both sides, with satisfactory functional outcome. Colour Doppler examination in healthy volunteers also revealed the presence of a perforator in the above location (Figure 6).
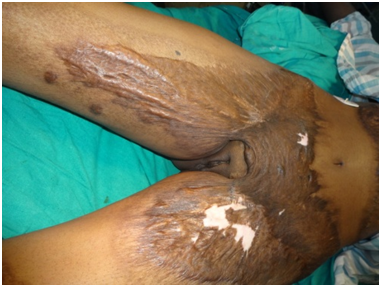
Figure 6 Colour Doppler examination in healthy volunteer showing the perforator at the medial border of gracilis about 5 cm below the pubic tubercle.
Hallock8 and Peek et al.,3 have described a free perforator flap based on single or multiple musculocutaneous perforators from the dominant pedicle of the gracilis muscle,7,8 Eom et al.9 have also described a horizontally oriented free medial thigh flap for resurfacing of lower extremity defects. However there is no previous report of a vertically oriented flap based on a single septocutaneous perforator between the gracilis and the adductor longus muscles as described in the present article, and neither has such a flap been used for reconstruction of groin contracture.
The advantages of our flap are as follows:
The authors conclude that the novel perforator-based fasciocutaneous flap described in this article is simple, easy to rise, with minimum morbidity, and could be a useful addition to the procedures available for reconstruction of extensive post-burn groin contractures.
None.
The author declares no conflict of interest.

© . This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.