Journal of
eISSN: 2373-4426


Mini Review Volume 15 Issue 3
Instituto Nacional de Perinatologia, Mexico
Correspondence: Dr. Giovanna Ivette Zanatta Ramírez, Neonatologist with high specialization in neonatal critical care, Instituto Nacional de Perinatologia, Lomas – Virreyes, Mexico City, 11000, Mexico, Tel +525510486401
Received: October 23, 2025 | Published: December 11, 2025
Citation: Zanatta Ramirez GI, Candiani CL. Etiology of early and late neonatal sepsis at the national institute of pediatrics from 2015 to 2019. J Pediatr Neonatal Care. 2025;15(3):186-194. DOI: 10.15406/jpnc.2025.15.00606
Neonatal sepsis is an infectious disease caused mainly by Escherichia coli bacteria in developing countries.1 The term neonatal sepsis refers to a clinical syndrome described as a systemic inflammatory response syndrome, characterized by a systemic bacterial infection which is documented by bacterial isolation from a blood culture or cerebrospinal fluid culture resulting in the growth of the microorganism that caused the neonatal sepsis.1,2 Sepsis has high morbidity and mortality rates, which have serious consequences for the prognosis of the newborn. It is important to know the main factors related to this pathology, and determining the etiology allows us to standardize appropriate diagnostic procedures.
Despite the existence of literature reporting the main infectious agents causing early and late neonatal sepsis, it is necessary to update or confirm the data at the Institute. The objective of the following study was to identify the main etiologies in early and late neonatal sepsis.
We found that the most frequently identified etiological agent in patients with neonatal sepsis at the National Institute of Pediatrics is Escherichia coli in 14.7% of cases, followed by Staphylococcus aureus in 5.2% and Klebsiella pneumoniae in 4.3%. The most frequent etiological agents in isolated early neonatal sepsis are Escherichia coli (11%), Enterococcus faecalis (2.7%), and Staphylococcus aureus (1.38%). In late-onset neonatal sepsis, Escherichia coli accounts for 21.4%, Staphylococcus aureus for 11.9%, and Klebsiella pneumoniae for 11.9%.
This differs from two previous studies conducted at the National Institute of Pediatrics, one of which was carried out from 2008 to 2013, reported Staphylococcus epidermidis as the most frequently isolated etiological agent in late-onset neonatal sepsis, accounting for 26.9%, followed by Escherichia coli, Klebsiella pneumoniae, and Staphylococcus hominis, each accounting for 13.4%. Similarly, another series reported by the INP in 2003 found that the most frequent etiological agent was Klebsiella pneumoniae.3,4
Definition of the problem to be addressed
Neonatal sepsis is pathology of infectious etiology caused mainly in developing countries by the bacterium Escherichia coli. Neonatal sepsis has high morbidity and mortality rates, which have serious consequences for the prognosis of the newborn. Knowing the main factors related to this pathology and determining its etiology allows us to standardize appropriate behavior to initiate a diagnostic approach with timely treatment, and through this, take preventive measures and establish adequate management with the consequent prevention of complications; this reduces the high mortality rate.1
Background
The term neonatal sepsis refers to a clinical syndrome described as a systemic inflammatory response syndrome, characterized by a systemic bacterial infection which is documented by bacterial isolation from a blood culture or cerebrospinal fluid culture resulting in the growth of the microorganism that caused the neonatal sepsis. This pathology occurs in the first month of extrauterine life.2
Neonatal sepsis can be classified as early or late depending on the age of the newborn in days; the literature differs on the number of days used for classification. González Saldaña5 mentions in his book Pediatric Clinical Infectious Diseases that neonatal sepsis is divided into early and late, occurring within the first 72 hours (3 days) and after 72 hours, respectively,6 whereas Shane AL,7 divides it into early and late with a cutoff point of 7 days between the two.8
The prevalence of neonatal sepsis varies in different hospitals, depending on patient characteristics such as gestational age, birth weight, number and type of invasive procedures, whether the patient requires assisted ventilation, catheter placement, prematurity, perinatal history, chorioamnionitis, male sex, preeclampsia, perinatal hypoxia, prolonged rupture of amniotic membranes, maternal fever, and the immunodeficiency typical of the neonatal period.9,10
The incidence in Mexico has been reported as 4 to 15.4 cases per 1,000 live births; data from the United States of America (USA) mention incidence rates of 1-5 cases per 1,000 live births. A study was conducted at the National Institute of Pediatrics11 where Rodríguez Weber12 mentions that neonatal sepsis is the fourth leading cause of morbidity among newborns hospitalized at the institution and the third leading cause of death. The overall mortality rate of 44% is high when compared to national and international reports.13
The most frequently related etiological agents in early sepsis are colonizing or contaminating germs in the mother's vaginal canal,1 with Gram-negative bacteria being isolated most frequently, primarily enterobacteria such as Escherichia coli and Klebsiella pneumoniae, as well as Enterococcus spp. In developed countries, the etiology of neonatal sepsis is modified, with Gram-positive microorganisms replacing enterobacteria in first place. In some cases, the etiology is also caused by Gram-positive microorganisms such as Group B Streptococcus (Streptococcus agalactiae).13
The etiology of late-onset neonatal sepsis is mainly related to the type of hospital flora,1 with Klebsiella pneumoniae MDR (multidrug-resistant), Pseudomonas aeruginosa, Escherichia coli MDR (multidrug-resistant), Enterobacter cloacae, Staphylococcus epidermidis, Staphylococcus aureus, and Candida albicans being common in Mexico. The main route of transmission is associated with healthcare, as well as contact with the hands of healthcare workers or family members who visit patients, followed by the use of invasive medical devices such as mechanical ventilation, urinary catheters, and venous catheters, as well as the indiscriminate use of broad-spectrum antibiotics.13
History of the health problem
The definition of sepsis was first mentioned in adult patients in 1992 by the American College of Critical Care Medicine and the Society of Critical Care Medicine, who first mentioned the terms Systemic Inflammatory Response Syndrome (SIRS), severe sepsis, septic shock, and multiple organ failure syndrome (MOFS). In 2001, at the International Sepsis Definitions Conference, the definition of "sepsis" based on biological markers was proposed for the first time.5,6,14
In 2004, a consensus was reached for the first time to define the parameters of sepsis in pediatric and neonatal patients, defining neonatal sepsis as: "A clinical syndrome characterized by signs and symptoms of systemic infection, confirmed by positive blood cultures or cerebrospinal fluid (CSF) cultures for bacteria, fungi, or viruses, and occurring within the first 28 days of extrauterine life."5,6
According to the National Institute of Child Health and Human Development and Vermont Oxford Networks, neonatal sepsis is classified into early-onset neonatal sepsis and late-onset neonatal sepsis, taking into account the following:15
Epidemiology of early and late neonatal sepsis
Knowing the main microorganisms that cause infections in this age group is essential for every hospital. Active surveillance is necessary, especially of bacterial resistance patterns, in order to be able to act with initial empirical treatment, according to local epidemiology.13
This knowledge will facilitate the early and timely implementation of appropriate empirical antibiotic management.
The World Health Organization estimates that around 5,000 newborns die each year worldwide; 98% of these deaths occur in developing countries, and infection is the cause of 30-40% of these deaths. In industrialized countries such as the United States of America, the incidence of neonatal sepsis is reported to be between one and five cases per thousand live births.13
In Mexico and other developing countries, rates of 15 to 30 per 1,000 newborns are reported, with a fatality rate of between 25 and 30%, depending on the literature, since others have reported 4 to 15.4 cases per 1,000 live births. and in Mexico, bacterial sepsis in newborns (NB) is the second leading cause of death (12.3%) in patients between one and six days old.13
Statistics by age and sex
Newborns are at greater risk of infection and of developing this pathology due to their immunological immaturity, plus other risk factors that we will analyze later.
It has been observed that the patients most affected by neonatal sepsis are premature newborns or those with very low birth weight, mainly those exposed to maternal infections or with rupture of the amniotic membranes. The literature reports that Streptococcus agalactiae is the main microorganism isolated in these infections; however, in developing countries, the predominant bacteria are enterobacteria, specifically E. coli and K. pneumoniae.13,16
The study conducted at the INP with an 8-year follow-up (1992-2000) reports the following: among the general variables compared, gestational age [Md of 34 (27 to 42) vs. 38 (28 to 42) weeks, p 0.001], extrauterine age [Median of 48 (1-600) vs. 168 (1-696) hours, p 0.001], and birth weight [Median 2.1 (0.73 to 3.6) vs. 3.0 (1.26 to 4.0), p 0.001] were significantly lower in the group of deceased newborns, while the percentage of premature newborns was lower in this same group (58.8 vs. 27.7, p 0.001).1,8
Even though the mortality rate has decreased due to the use of antimicrobials, it is estimated that 2 to 3% of term neonates and 20 to 30% of preterm neonates will die from NTS, because virtually all very low birth weight neonates (< 1000 g) and approximately half of those born at term will require intensive care for the management of respiratory distress and hemodynamic support.1,9
Etiology of early and late-onset neonatal sepsis
The microorganisms involved in neonatal sepsis are diverse, with bacteria that are highly resistant to multiple antimicrobial regimens being of primary concern.
In microbiology, Gram-negative bacteria are those that do not stain dark blue or violet with Gram staining, but rather a faint pink color, hence the name Gram-negative. This characteristic is closely linked to the didermic structure of the cell envelope, as it has a double cell membrane (one external and the other cytoplasmic), which reflects a natural type of bacterial organization.17
Gram-negative bacteria are the most common causative agents of systemic infection, with 9 to 36 cases of sepsis reported per 100 discharges from tertiary hospitals and mortality rates ranging from 23% to 65%. In Mexico, neonatal sepsis is one of the leading causes of neonatal morbidity and mortality, especially when caused by Gram-negative bacteria.17,18
In microbiology, Gram-positive bacteria are those that stain dark blue or violet with Gram staining. This chemical characteristic is closely linked to the structure of the cell envelope, reflecting a natural type of bacterial organization.17
In Mexico and other Latin American countries, the microorganisms that predominate in early sepsis are mainly Gram-negative bacilli, Escherichia coli, and Klebsiella pneumoniae, while in late neonatal sepsis, Pseudomonas aeruginosa, Staphylococcus aureus, Staphylococcus epidermidis, and Candida spp. have been mainly isolated.
The etiology is primarily bacterial, as fungal and viral sepsis account for less than 1% of cases.17,18
In the latest study conducted at the National Institute of Pediatrics from 1992 to 2000, the following causative microorganisms were reported (Table 1):
Risk factors for early and late neonatal sepsis
Early neonatal sepsis is commonly associated with premature and prolonged (more than 18 hours) rupture of membranes, chorioamnionitis, colonization of the genital tract with Group B Streptococcus, urinary tract infection, gestational age less than 37 weeks, intrauterine growth restriction, birth asphyxia, and male sex, which may be related to X-linked immunoregulatory genes.13,17
Anaya-Prado2 states in his article Neonatal sepsis and associated factors that newborns who will develop NTS have factors directly associated with pregnancy and childbirth. These include gestational age, maternal colonization by group B Streptococcus (GBS) of the genital and urinary tract, maternal urosepsis, premature or prolonged rupture of membranes, maternal peripartum infection, traumatic or septic delivery, male sex of the newborn, low birth weight, an Apgar score of less than 7 at five minutes, hypothermia of the newborn, and the presence of chorioamnionitis.2
The strongest positive predictive risk factor for developing NTS is low gestational age. A review from 1992 to 2000 reported an overall incidence of 0.77 per 1,000 live births. Although low gestational age is related to and interacts with low birth weight, it is concluded that the increased risk is more related to low gestational age than to birth weight.1,8
In developing countries, access to health services and sociocultural level are additional factors. Other risk determinants include a history of immunodeficiencies and certain metabolic disorders, such as galactosemia.18
Pathophysiology
In the pathophysiology of sepsis, the response seems to depend on the strain of T lymphocyte that is stimulated: without that Th1 lymphocyte, the predominant response is SIRS; if the response is led by the Th2 lymphocyte, the predominant response will be CARS (compensatory anti-inflammatory response syndrome); but if there is a balance between the inflammatory and anti-inflammatory components, the predominant response will be MARS (mixed antagonistic response syndrome).8,17
This means that the infectious component may be present even in the absence of the classic signs of systemic inflammatory response that we know, but that they can cause confusion due to their inadequate specificity. That is why we must familiarize ourselves with the other two concepts. Now, any of these three components (SIRS, CARS, MARS) and their manifestation in the patient are directly related to the infecting microorganism and the host.17
The body's response to infection when triggering the release of different inflammatory mediators is to maintain homeostasis, i.e., a balance between CARS and SIRS, but this rarely happens. In most cases, the systemic inflammatory response predominates, and if it cannot be effectively controlled, the cardiovascular system is affected and shock occurs, triggering multiple organ dysfunction syndrome. Conversely, if CARS predominates, the characteristic feature is suppression of the immune system with induction of apoptosis or programmed cell death.17,18
In sepsis, the pathophysiological explanation remains extremely complex. Proinflammatory, anti-inflammatory, cellular, coagulation, and microcirculation components are involved, which can potentially lead to multiple organ dysfunction and, if not adequately supported and managed, to death. In the concept of host predisposition and response to infection, genetic polymorphism and the role of immunogenetics had already been identified as factors that predispose to the presence of severe sepsis, septic shock, and multiple organ dysfunction.17
The initial reaction to an infectious event begins when the immune system detects and isolates a potentially infectious antigen and triggers a generalized pro- and anti-inflammatory cellular and humoral response, in which the first cells to be activated are neutrophils, monocytes, and macrophages.5,18
This phenomenon occurs in the first few hours, and the interaction of these cells, by releasing their various inflammatory components, causes endothelial disruption and the release of substances into the plasma. A secondary inflammatory process then develops, in which cytokines (interleukins) and components of the arachidonic acid inflammatory cascade play a major role.8,17
Other substances derived from endothelial dysfunction, such as nitric oxide, also contribute to the various manifestations of microcirculatory failure that explain the organ dysfunction associated with sepsis.8,17
The activated and dysfunctional endothelium activates platelets, amplifies the coagulation cascade, and activates the complement. It is clear, then, that the endothelium is the platform for this entire scenario. This organ loses its integrity significantly, generalized microthrombosis develops, there is an increase in systemic short-circuiting, tissue oxygen supply is reduced, and if optimal management is not provided to avoid the various complications arising from endothelial dysfunction, there is a blockage of the respiratory chain, generating cytopathic hypoxia, and the much-feared mitochondrial microcirculatory distress syndrome appears.8,17,18
Clinical diagnosis
The diagnosis of neonatal sepsis based solely on clinical criteria is difficult to establish. However, prior risk assessment makes the management of newborns at risk of sepsis more effective.
Early and timely diagnosis of neonatal sepsis is not easy because the clinical manifestations are nonspecific and may be related to other pathologies observed in neonates, mainly in the premature group.
The clinical picture can progress rapidly to more advanced stages, so the physician must conduct a very thorough interview with the mother and a comprehensive physical examination.
Clinical suspicion is the main factor in reaching a diagnosis of neonatal sepsis, which should ideally be confirmed by positive cultures in blood, urine, cerebrospinal fluid, or other normally sterile sites, in order to arrive at the correct diagnosis and thus structure the approach and confirm the diagnosis by isolating a pathogenic microorganism in the blood.12
Since the clinical presentation of neonatal sepsis is nonspecific and, in some cases, especially in premature infants, may initially be asymptomatic, the diagnostic suspicion can be based on the presence of risk factors for infection.
Rodríguez-Weber12 mentions in his study conducted at the National Institute of Pediatrics from 199211 to 2000 that among the clinical variables studied, respiratory distress, hypotension, prolonged capillary refill, oliguria, history of dysthermia, and abdominal distension showed highly significant differences between the groups (p<0.01); dehydration, tachycardia, edema, and the presence of diarrhea showed significant differences (0.01 ≤p < 0.05), while cyanosis, pallor, and refusal to eat showed a tendency toward significant differences (0.05 ≤p < 0.10).12
The warning signs identified by the World Health Organization are as follows: convulsions, refusal to feed, respiratory distress, hypoactivity, and polypnea.3,7
Attempts have been made to document clinical variables for the timely diagnosis of sepsis; for example, Haque et al.,4 have proposed definitions of neonatal sepsis based on clinical variables: temperature instability, heart rate greater than 1 standard deviation for age (<100 or >180 beats per minute); respiratory rate (>60 breaths per minute); moaning or desaturation; lethargy or altered alertness, food intolerance, and hypoglycemia.1,9
The neonatal sepsis guidelines published by the Federico Gómez Children's Hospital in Mexico mention that the clinical manifestations are nonspecific and vary greatly depending on the severity of presentation. Some of the main ones are: dysthermia, respiratory distress, jaundice, apnea (more common in premature infants), abdominal distension, hepatomegaly, lethargy, bleeding, hypoactivity, pallor, oliguria, cyanosis, marbled skin, seizures, irritability, splenomegaly, vomiting, diarrhea, arterial hypotension, petechiae or ecchymosis, thrombocytopenia, and acidosis.14
Finally, the CENETEC Clinical Practice Guidelines, when applying clinical prediction models to initiate empirical antibiotic treatment, mention relevant data such as: feeding difficulties, seizures, fever, hypoactivity, tachypnea, severe thoracoabdominal dissociation, moaning, cyanosis, bulging fontanelle, capillary refill time greater than 3 seconds, marbled appearance, weak peripheral pulses, jaundice, vomiting, abdominal distension, periumbilical erythema or omphalitis, generalized flaccidity or hypertonia, and decreased urine output as reported by the mother.6
Differential diagnosis
One of the biggest challenges in managing neonatal sepsis is making a correct diagnosis. Unlike older patients, newborns present with nonspecific clinical signs of infection.
Many complications of prematurity, such as respiratory distress syndrome or congenital heart defects, can present similarly to neonatal sepsis and are sometimes clinically indistinguishable.
Although there is no specific diagnosis, dehydration, neonatal jaundice, apnea, congenital heart disease, and inborn errors of metabolism should be ruled out when evaluating the newborn. Depending on the patient's history and the time of evolution, as well as the number of days of extrauterine life, the diagnosis of neonatal sepsis should be considered first.7,9
Problem statement
Despite the existence of literature reporting the main infectious agents causing early and late neonatal sepsis, it is necessary to update or confirm the data at the Institute. Therefore, the following research project would provide us with this information for the years 2015 to 2019. At the same time as identifying the main causative agents, we must establish empirical treatment for our patients, since both early and late neonatal sepsis have a poor prognosis if not detected and treated in a timely manner.
This research project can be extended to determine the sensitivity of these same agents to different antimicrobials, as reported by the National Institute of Pediatrics, and to establish empirical treatment guidelines.
In the long term, this information will be very useful, as the results obtained can be applied to children diagnosed with early or late neonatal sepsis.
Research question
What is the etiology of early and late neonatal sepsis in the Neonatology Department of the National Institute of Pediatrics?
Justification
Objectives
General objective
To determine the infectious agents causing early and late neonatal sepsis in newborns discharged from the Neonatology Department of the National Institute of Pediatrics between 2015 and 2019.
Specific objective
To determine the etiology of neonatal sepsis up to 24 to 72 hours after birth at the National Institute of Pediatrics
To determine the etiology of neonatal sepsis after 72 hours of birth at the National Institute of Pediatrics
Research classification (type of study): Observational, retrospective, retroelective, and descriptive.
Population universe
Records of newborns diagnosed with neonatal sepsis upon discharge.
Eligible population
Newborns discharged from the Neonatology Department between January 1, 2015, and December 31, 2019.
Inclusion criteria
Exclusion criteria
Method
The clinical archive will be asked to provide a list of the files of patients discharged from the Neonatology Service and the Infectious Diseases Department with a diagnosis of neonatal sepsis (P36). The list will be completed with electronic statistics from the Neonatology Service itself. The files will be located in the clinical archive and checked to ensure they contain the required data. The form designed for this purpose will be filled out, obtaining demographic, clinical, bacteriological, and patient evolution data. The data will then be compiled in an Excel spreadsheet for processing.
Sample size
The clinical archive was asked to provide a list of the files of patients discharged from the Neonatology service and the Infectious Diseases Department with a diagnosis of Neonatal Sepsis (P36). Newborns discharged from the Neonatology service from January 1, 2015, to December 31, 2019.
Sample calculation
A convenience sample was taken that included all locatable cases of newborns discharged from the Neonatology Service of the National Institute of Pediatrics from January 1, 2015, to December 31, 2019.
Statistical analysis
In the first phase, a database was created in Excel. This was then exported to the statistical program SPSS Version 21, which was used to analyze the information. The results of the study were presented in tables, charts, or graphs.
Ethical considerations
The study was retrospective, and given the type of study, it does not require informed consent. Patient information will be kept confidential, and their identities will not be disclosed. No individual data will be included.
As this study was limited to a population of discharges from the Neonatology Department during a specific period, the sample was taken for convenience from all newborns treated at the National Institute of Pediatrics between January 1, 2015, and December 31, 2019, with a discharge diagnosis of neonatal sepsis (ICD-10-P36). A total of 126 records were found, of which 12 were excluded because they did not correspond to the diagnosis of neonatal sepsis, in addition to some being duplicates or not meeting the inclusion criteria. Only 114 met the diagnostic criteria for neonatal sepsis.
A total of 114 neonates diagnosed with neonatal sepsis were included in this analysis. Sixty-six cases occurred in the first 72 hours of life, and 48 cases occurred after the first 72 hours of extrauterine life up to 28 days. Isolation and identification were achieved in 47 cases, which were included in the study.
In the population group studied, the male-to-female ratio was 1.4:1, with 68 male cases and 46 female cases. This is consistent with the literature, as it has been reported more frequently in males (Figure 1).
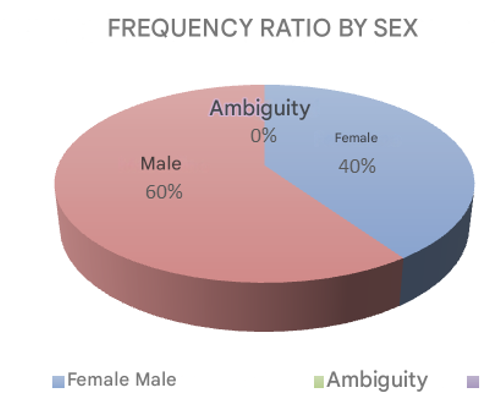
Figure 1 The frequency of neonatal sepsis by gender at the National Institute of Pediatrics from 2015 to 2019 is shown.
The average age of onset of neonatal sepsis is 5.9±8 days. Regarding the classification of neonatal sepsis as early or late, of the 114 patients, 71 were less than 72 hours old, corresponding to early neonatal sepsis, and 43 were older than 72 hours, corresponding to late neonatal sepsis. The minimum age was 24 hours and the maximum was 27 days (Figure 2).
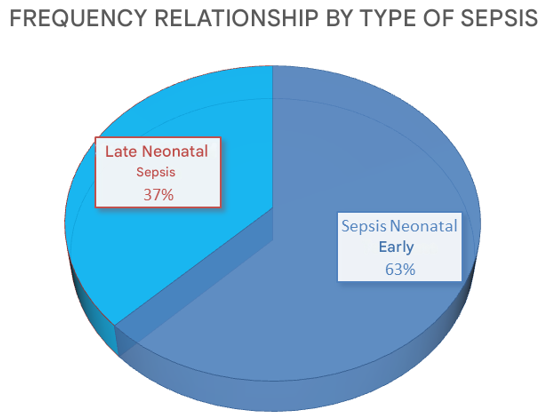
Figure 1 Frequency ratio of early and late neonatal sepsis at the National Institute of Pediatrics from 2015 to 2019.
The ratio of cases by gestational age, between preterm and term, obtained a median of 35 weeks of gestational age with a minimum value of 25 SDG and a maximum value of 42 weeks, with 64 cases of preterm patients (less than 37 SDG), and 50 term cases (from 37 SDG to 42 SDG). The average was 34 SDG, with a standard deviation of 3.1 (Figure 3).

Figure 3 Relationship by gestational age in patients with neonatal sepsis at the National Institute of Pediatrics from 2015 to 2019.
Upon arrival, patients were assessed to determine whether they had any primary disease, the most common of which were as follows: 60 cases arrived with an initial diagnosis of prematurity (52.6%), of which 35 also presented with neonatal sepsis from the outset (30.7%). Acute respiratory distress syndrome 18 patients (15.6%), hyperbilirubinemia (12%), and congenital heart disease 0.52% (Figure 4).
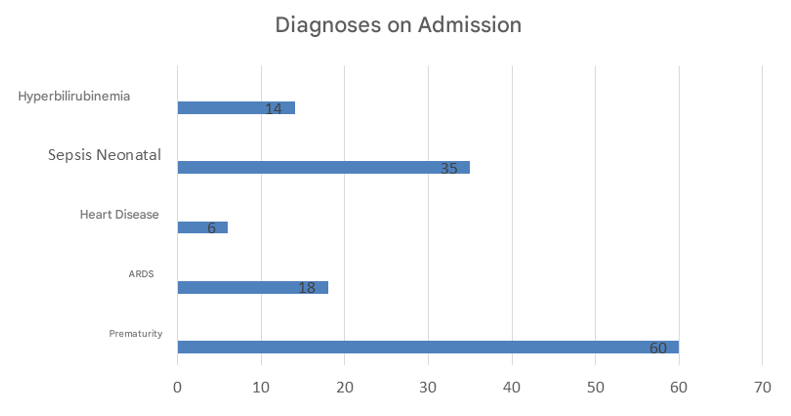
Figure 4 Most frequent admission diagnoses in neonates with neonatal sepsis at the National Institute of Pediatrics from 2015 to 2019.
The average birth weight was 2912 grams, with a standard deviation of +989 g, a minimum of 636 grams, and a maximum of 4230 grams.
Of the 114 patients who met the criteria for neonatal sepsis, there were 49 cases with positive blood culture results, meaning that the etiological agent was isolated and identified. Three of them did not have blood cultures, and 62 cases had negative blood culture results or no growth was found (Figure 5).
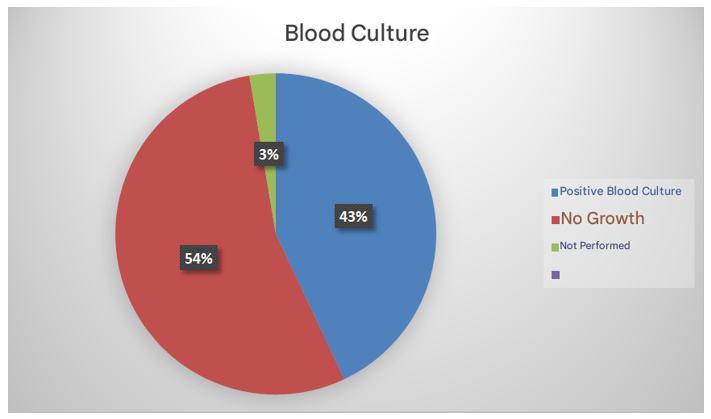
Figure 5 Cases of neonatal sepsis in newborns who underwent blood culture at the National Institute of Pediatrics from 2015 to 2019 are presented.
The most common etiological agents in neonatal sepsis are (Table 1): Escherichia coli 14.7% (17 cases), Staphylococcus aureus 5.2% (6 cases), Klebsiella pneumoniae 4.3% (5 cases), Staphylococcus hominis 3.4% (4 cases), Candida albicans 3.4% (4 cases), Acinetobacter baumannii 2.6% (3 cases), Enterococcus faecalis 1.7% (2 cases), Enterobacter cloacae 1.7% (2 cases), Pseudomonas aeruginosa 1.7% (2 cases), Staphylococcus epidermidis 0.86% (1 case), Klebsiella oxytoca 0.86% (1 case), Staphylococcus pausteri 0.86% (1 case), Enterococcus faecium 0.86% (1 case), Stenotrophomonas maltophilia 0.86% (1 case) (Figure 6).
|
Causative agent |
% isolation in living patients (n=65) |
% isolation in deceased patients (n=51) |
|
E. coli |
3 |
6 |
|
E. cloacae |
8 |
4 |
|
K, pneumoniae |
12 |
53 |
|
S. aureus |
11 |
4 |
|
S. epidermidis |
30 |
8 |
|
No isolation |
36 |
25 |
|
Total |
100 |
100 |
Table 1 Microorganisms causing neonatal sepsis at the National Institute of Pediatrics from 1992 to 2000
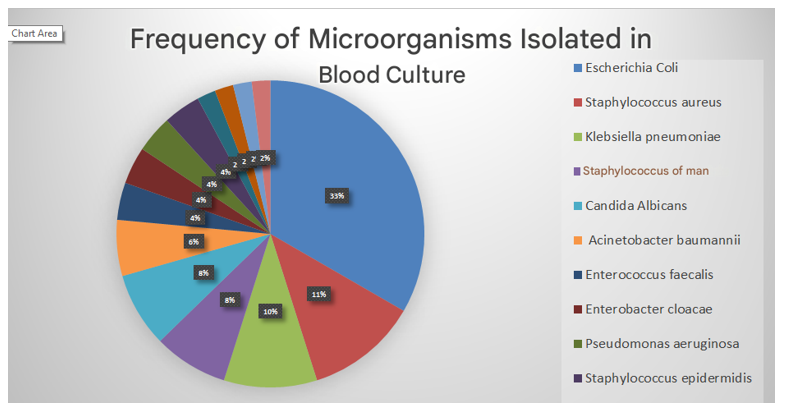
Figure 6 Frequency of microorganisms isolated in blood cultures at the National Institute of Pediatrics from 2015 to 2019.
Of the 114 cases included in this study, the following statistical analysis of the variables described above was performed (Table 2).
|
Microorganism isolated in patients with neonatal sepsis at the INP |
Number of cases |
Percentage
|
|
Escherichia coli |
17 |
14.9 |
|
Staphylococcus aureus |
6 |
5.26 |
|
Klebsiella pneumoniae |
5 |
4.38% |
|
Staphylococcus hominis |
4 |
3.5 |
|
Candida Albicans |
4 |
3.5 |
|
Acinetobacter baumannii |
3 |
2.6 |
|
Enterococcus faecalis |
2 |
1.7% |
|
Enterobacter cloacae |
2 |
1.7% |
|
Pseudomonas aeruginosa |
2 |
1.7% |
|
Staphylococcus epidermidis |
1 |
0.87 |
|
Klebsiella oxytoca |
1 |
0.87 |
|
Staphylococcus pausteri |
1 |
0.87 |
|
Enterococcus faecium |
1 |
0.87 |
|
Stenotrophomonas maltophilia |
1 |
0.87% |
Table 2 Frequency of microorganisms isolated in blood cultures
In cases of early and late neonatal sepsis, the isolated germs and their frequency are shown in the following Tables 3–5.
|
Microorganism isolated in patients with early neonatal sepsis at the INP |
Number of cases |
Percentage
|
|
Escherichia coli |
8 |
11 |
|
Staphylococcus aureus |
1 |
1.38 |
|
Klebsiella pneumoniae |
0 |
0 |
|
Staphylococcus hominis |
1 |
1.38% |
|
Candida Albicans |
1 |
1.38% |
|
Acinetobacter baumannii |
0 |
0 |
|
Enterococcus faecalis |
2 |
2.7% |
|
Enterobacter cloacae |
1 |
1.38% |
|
Pseudomonas aeruginosa |
1 |
1.38% |
|
Staphylococcus epidermidis |
1 |
1.38% |
|
Klebsiella oxytoca |
1 |
1.38 |
|
Staphylococcus pausteri |
1 |
1.38 |
|
Enterococcus faecium |
1 |
1.38 |
|
Stenotrophomonas maltophilia |
0 |
0 |
Table 3 Distribution of microorganisms isolated from patients with early-onset neonatal sepsis at the INP
|
Microorganism isolated in patients with late-onset neonatal sepsis at the INP |
Number of cases |
Percentage
|
|
Escherichia coli |
9 |
21.4 |
|
Staphylococcus aureus |
5 |
11.9% |
|
Klebsiella pneumoniae |
5 |
11.9% |
|
Staphylococcus hominis |
3 |
7.14% |
|
Candida albicans |
3 |
7.14% |
|
Acinetobacter baumannii |
3 |
7.14% |
|
Enterococcus faecalis |
0 |
0 |
|
Enterobacter cloacae |
1 |
2.38% |
|
Pseudomonas aeruginosa |
1 |
2.38% |
|
Staphylococcus epidermidis |
0 |
0 |
|
Klebsiella oxytoca |
0 |
0 |
|
Staphylococcus pausteri |
0 |
0 |
|
Enterococcus faecium |
0 |
0 |
|
Stenotrophomonas maltophilia |
1 |
2.38 |
Table 4 Distribution of microorganisms isolated from patients with late-onset neonatal sepsis at the INP
|
Method |
Number of cases in which it was performed |
Percentage |
|
Blood culture |
112 |
98 |
|
Stool culture |
1 |
0.87 |
|
Urine culture |
49 |
42.9 |
|
CSF culture |
8 |
7 |
|
Secretion culture |
35 |
30.7 |
|
Catheter culture |
60 |
52.6 |
Table 5 Diagnostic methods performed in neonates evaluated for sepsis at the INP
Among the associated factors investigated in the study, it was found that of the 114 patients, 61 had endotracheal intubation (53.5% of cases). Patients with central venous catheter placement accounted for 75 cases, corresponding to 65.7%. Orogastric tube placement was performed in 42.9% (49 cases), and patients had a history of previous surgery, corresponding to 25 cases (21.9%). Fifty cases (43.8%) received parenteral nutrition.
Of the main infectious foci in the study, it was found that of the 114 cases, 51 had pneumonia during their hospital stay (44.7%). Nine cases had diarrhea (7.89%), nine cases had urinary tract infections (7.89%), three cases had meningitis (2.63%), one case had arthritis (0.87%), one case had cellulitis (1.7%), five cases had omphalitis (4.38%), and 26 cases had other mainly abdominal sources (22.8%).
Laboratory studies found in patients showed that 22 patients had white blood cell counts within normal values, 54 cases had leukocytosis (>14,000), and 37 cases had leukopenia (<5000). Platelet counts were within the normal range for age in 51 cases, >500,000 in 11 cases, and <100,000 in 51 cases. Only 3 patients underwent lumbar puncture, which was reported as pathological in these cases. Only one of the 114 patients underwent rotaforesis and serology for any TORCH spectrum, which was reported as positive in 10 patients, while in 87 patients, it was not performed.
The average length of hospital stay was 20 days, with a minimum of 2 days and a maximum of 188 days. Hospital stays were not exclusively due to neonatal sepsis, but also to other clinical conditions of the patient. The median length of stay was 22 days.
Of the total number of patients with neonatal sepsis, 16.6% died (19 cases), while 95 cases (83.3%) improved. Of the 19 cases that died, 3 were diagnosed with late neonatal sepsis (2.63%), and 16 cases with early neonatal sepsis (14%). The direct cause of death was neonatal sepsis.
Neonatal sepsis is increasingly common in neonatal intensive care units due to the higher survival rate of premature patients, associated with a significant increase in invasive procedures. Therefore, early identification and treatment according to the etiological agent of each hospital is required to improve the prognosis and survival of patients. Nosocomial neonatal sepsis is also a significant problem that has been increasing due to long hospital stays, especially in low birth weight and premature infants.
A study conducted at the National Institute of Pediatrics in 2003 by Dr. Rodriguez Weber reports that neonatal sepsis is the fourth leading cause of morbidity in hospitalized neonates and the third leading cause of mortality.3
In the present study, the percentage of early neonatal sepsis was 63%, i.e., cases identified with neonatal sepsis before 72 hours of life, and after the first 72 hours of life, 36.5% were found to be late neonatal sepsis. In Mexico and other developing countries, rates of 15 to 30 per 1,000 live births are reported, with a mortality rate of 25 to 30% reported by the Federico Gómez Children's Hospital of Mexico.13
In our study, lower figures were found, documented at 16.6%.
This is because it has been found that in developing countries, access to health services and sociocultural level are high-risk factors added to the diagnosis of neonatal sepsis.
The frequency of microorganisms related to early and late neonatal sepsis varies according to the series studied.
Newborns suffering from early and late neonatal sepsis generally have clinical conditions that require invasive diagnostic and therapeutic procedures, such as ventilatory support, prolonged hospitalizations, surgical procedures, use of central venous catheters, as well as providing caloric and nutritional support, such as parenteral nutrition and management in the neonatal intensive care unit.
The etiological agents related to early and late neonatal sepsis are mainly nosocomial pathogens, which explains the variability of results in different series reported in the international literature.
However, Klebsiella pneumoniae and Staphylococcus aureus were found to be frequent etiological agents in both this study and international reports. The most frequently reported in this study were Escherichia coli and Staphylococcus aureus, followed by Klebsiella pneumoniae in both early and late neonatal sepsis.
In order to increase the effectiveness of antimicrobial coverage in the neonatal intensive care unit, it is necessary to know the frequency of isolates so that, prior to reporting blood cultures, an empirical antimicrobial regimen can be established based on the reported prevalence and the experience of each hospital, always taking into account the pattern of resistance and sensitivity. In nosocomial sepsis, treatment should be aimed at combating the microorganisms present in each institution.
In the present study conducted at the National Institute of Pediatrics with a clinical diagnosis of neonatal sepsis, in 42.9% of cases the diagnosis was confirmed by a positive blood culture, which is considered the gold standard for diagnosis only in 2.6% of cases was a blood culture not performed to isolate the etiological agent or confirm the diagnosis, and in 54.3% of cases, a blood culture was performed but the agent could not be isolated. This is consistent with what is reported in the literature, since in more than 50% of cases, empirical antimicrobial therapy is initiated without isolation by blood culture for neonatal sepsis, which in most cases, due to the lack of isolation, leads to the addition of a second or third antimicrobial due to poor evolution.
Having a low number of positive blood cultures means that in most cases the treating physician does not know the etiological agent of sepsis in the neonatal period, so it is advisable to initiate management not only empirically, but also according to the etiology of each hospital, which should be modified as soon as growth or isolation is achieved.
The most frequently identified etiological agent in patients with neonatal sepsis at the National Institute of Pediatrics is Escherichia coli at 14.7%, followed by Staphylococcus aureus at 5.2% and Klebsiella pneumoniae at 4.3%. The most frequent etiological agents in early neonatal sepsis isolates are Escherichia coli (11%), Enterococcus faecalis (2.7%), and Staphylococcus aureus (1.38%); and in late-onset neonatal sepsis, Escherichia coli (21.4%), Staphylococcus aureus (11.9%), and Klebsiella pneumoniae (11.9%).
This differs from two previous studies conducted at the National Institute of Pediatrics, one of which was carried out from 2008 to 2013, reported Staphylococcus epidermidis as the most frequently isolated etiological agent in late-onset neonatal sepsis, accounting for 26.9%, followed by Escherichia coli, Klebsiella pneumoniae, and Staphylococcus hominis, each accounting for 13.4%. Similarly, another series reported by the INP in 2003 found that the most frequent etiological agent was Klebsiella pneumoniae.3,4
The trend in identified etiological agents differs in different hospitals in Mexico and the United States. In different hospitals in Mexico, Staphylococcus aureus has been found to be the most frequent agent, and coagulase-negative staphylococcus was the most commonly isolated germ in neonates with sepsis at the Children's Hospital of Mexico in 2003. No more recent reports are available. Group B Streptococcus is the most frequent etiological agent in the United States and Europe.14
Khalid et al.,4 in a study conducted in 2010, comment that neonates generally begin to be colonized during the first 48 hours of life by Gram-positive, Gram-negative, and Candida species microorganisms, and in late-onset neonatal sepsis, the most frequent microorganisms are Staphylococcus, Serratia, and Citrobacter.
In the present study, it was found that in the population group studied, the male:female ratio was 1.4:1, with 68 male cases and 46 female cases. This is consistent with the literature, as it has been reported more frequently in males, which has been considered a risk factor for nosocomial sepsis. There was also an increase in mortality in male patients compared to female patients.
With regard to gestational age, 57% of cases were preterm and 43% were term, in accordance with the literature, where gestational age is considered a risk factor for neonatal sepsis. Studies published by the National Institute of Pediatrics have shown a significant increase in these figures due to the fact that life expectancy in premature infants has increased significantly. The results obtained are as expected because premature patients are at greater risk of acquiring infections due to their increased susceptibility to them, as well as prolonged hospital stays.
On this occasion, the diagnosis of early neonatal sepsis differed from the previous series conducted from 2008 to 2013, in which the most frequent diagnosis was late neonatal sepsis with 37%, with 30.7% of cases of nosocomial neonatal sepsis, which at that time was related to the fact that our hospital does not have a toco-surgery area and the neonates treated come from the community or are referred from another hospital. However, in the current study, early neonatal sepsis was found more frequently in 63% of patients and late neonatal sepsis in 37%. This may be related to a higher number of transfers of premature patients.
In terms of reported mortality, it was higher in males, with 8.6% and 91.4% dying. They showed improvement, of which 15% were diagnosed with late-onset neonatal sepsis and 85% with early-onset neonatal sepsis, which is consistent with the literature because gestational age is a risk factor.
It would be important to perform postmortem studies because the patients had more than one diagnosis as the cause of death, so exhaustive studies should be carried out to determine whether the actual cause of death was neonatal sepsis. The pathogen most frequently identified in the group of neonates who died is Escherichia coli BLEE.
This study concludes that the etiology has changed over time and with the increase in premature patients at the institution, which on this occasion was associated with an increase in these patients. The increase in the frequency of early neonatal sepsis stands out as a risk factor.
Microbiology changed from 2015 to 2019, as the most frequently isolated agent was Escherichia coli, followed by Staphylococcus aureus and Klebsiella pneumoniae, with no distinction between early and late sepsis. It was found that the most frequently isolated agent in early neonatal sepsis is Escherichia coli, followed by Staphylococcus aureus and Enterococcus faecalis, and in late neonatal sepsis, Escherichia coli, Staphylococcus aureus, and Klebsiella pneumoniae.
It is important to perform blood cultures on all newborns who meet the clinical diagnosis of neonatal sepsis, as this is the gold standard for providing better management of these patients and for being able to prescribe a specific antimicrobial regimen for the agent in question.19–21
None.
This work did not receive external funding.
The author declares no conflict of interest.

©2025 Zanatta, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.