Journal of
eISSN: 2379-6359


Review Article Volume 15 Issue 1
Otorhinolaryngology Service of the Güemes Sanatorium, CABA, Argentina
Correspondence: Alan Gilpin, Otorhinolaryngology Service of the Güemes Sanatorium, CABA, Argentina
Received: January 12, 2023 | Published: March 20, 2023
Citation: Gilpin A. Use of botulinum toxin in patients with bruxism.J Otolaryngol ENT Res. 2023;15(1):38-42. DOI: 10.15406/joentr.2023.15.00525
botulinum, carotid, bruxism, prognosis, trigeminal nerve
Bruxism is a pathology that affects millions of people around the world and whose prevalence is increasing annually. In addition to the significant health costs that it demands, temporomandibular joint (TMJ) disorders cause great consequences not only of a physical nature, but also psychological and emotional, affecting the person's social and family environment.
That is why different branches of medicine such as Dentistry, Neurology, Physiatry, Maxillofacial, Otorhinolaryngology, among others, began hard work several years ago in search of an effective approach that allows patients to improve their quality of life and so you can carry out your daily activities. Among the possible therapeutic measures is the injection of botulinum toxin (TB) whose evidence, still scant, seems to show a hopeful path.
The objective of this monograph is to introduce bruxism and the use of BT for its treatment.
Anatomical landmarks of the masseter muscle
The TMJ is an anatomical structure composed mainly of bone, muscle and ligamentous tissue that carry out important movements of the jaw. Within the muscular structures we will focus on the masseter muscle (MM) since it is one of the protagonists in the use of TB as a treatment.
The MM is a short, thick, rectangular masticatory muscle of the craniomandibular type located in the middle third of the face, specifically in the parotid-masseteric region, whose functions are mandibular elevation and protrusion, and to provide support to the TMJ joint capsule. . It is made up of 2 fascicles, one superficial and more voluminous, whose origin is at the lower edge of the anterior 2/3 of the zygomatic arch, inserting it in the angle of the mandible and in the lower and lateral area of the mandibular ramus; and in turn a deep portion originating in the medial, inferior and posterior border of the zygomatic arch with its insertion in the supero-lateral area of the mandibular ramus and in the coronoid process Figure 1.1
It should be noted that MM is related to
Laterally and posteriorly through its fascia with the anterior prolongation of the parotid gland and its respective excretory duct, in addition to different vascular, nervous and muscular structures such as the facial artery, the zygomatic major and minor muscles, risorium and platysma. Medially, through its deep portion, with the lateral face of the mandibular ramus, where the muscle is superiorly related to the mandibular notch (where the nerve and masseteric artery access); in the middle zone it is related to both the coronoid process of the mandible and the terminal tendon of the temporalis muscle and the adipose body of the cheek. Anteriorly, only with the adipose body of the cheek, tissue that separates it from the buccinator muscle and from the facial vessels. Posteriorly with the TMJ and with part of the parotid cell.
Regarding innervation, the protagonist is the mandibular branch (V3) of the trigeminal nerve (V).2 The mandibular nerve passes from the middle cranial fossa through the foramen ovale towards the infratemporal fossa, where it immediately divides into an anterior trunk from which The temporomaseterine trunk detaches, giving rise to the masseteric nerve, which accesses the MM through the mandibular notch.3
Regarding irrigation, it depends on the facial artery, superficial temporal artery and maxillary artery. Their respective paths are briefly described below:
The facial artery is detached from the anterior face of the external carotid artery, one of its collateral branches is the inferior masseteric artery, which arises a little above the lower edge of the mandible. From here it runs obliquely superiorly and posteriorly along the lateral aspect of the masseter muscle, where it ends.
The superficial temporal artery, terminal branch of the external carotid, arises at the level of the neck of the condylar process of the mandible. From this the transverse artery of the face is detached, which in turn is divided into 2 branches; the superficial branch that runs along the lateral aspect of the masseter muscle between the parotid duct and the zygomatic arch, which gives some ascending and descending branches for the muscle; and on the other hand, the deep branch or deep masseteric artery, which perforates the masseter near its posterior edge and runs between the superficial and deep fascicles of the muscle.
The maxillary artery -terminal branch of the external carotid-; gives 15 branches in total. Of these, the one in charge of irrigation of the MM is the masseteric artery, which is the one that mainly provides irrigation to said muscle. The masseteric artery passes through the mandibular notch, reaching the deep face of the masseter, thus distributing throughout the muscle.1
Generalities of botulinum toxin
At the end of the 18th century, botulism caused a large number of deaths in Europe due to poor sanitary controls as a result of the aftermath of the War commanded by Napoleon. In 1811 the Department of Internal Affairs of the Kingdom of Wurttemberg defined "sausage poisoning" thus beginning numerous studies and giving the term "botulus" to the disease (sausage in Latin).
It was thus that in 1822 the German Justinus Kerner "Wurst" (German term for sausage) wrote the first complete monograph on the "fat toxin" of Aryan sausages-based on experiments carried out on himself and animals-where he described the neurological symptoms produced of interruption of motor signal transmission. On that occasion, he took the opportunity to propose that this substance be used for therapeutic purposes as a movement disorder and/or hypersecretion of body fluids. However, it was necessary to wait for the microbiologist Figure 2 Emile Pierre van Ermengem under the guidance of Robert Koch - at the end of the 19th century, to demonstrate that botulism corresponds to the presence of a toxin found in food, whose producing bacterium was called Clostridium. Botulinum. Subsequently, the toxin was used for war (fortunately without success) and therapeutic purposes where the pharmaceutical company Allergan Inc. takes a leading role buying the rights to the patent and calling the drug "Botox". In the current market, the most recognized brands worldwide are: Botox™ (Allergan USA) and Dysport™ (Speywood England).4

Figure 2 Holding the contraction we will proceed to identify the region of greatest procidence of the muscle (green dot) which will be the epicenter of our work triangle.
Currently it is stated that Clostridium botulinum is a gram-positive anaerobic bacterium that presents 7 serotypes (A, B, C, D, E, F and G) which produce a unique form of neurotoxin. The latter is a high molecular weight protein of 150,000 daltons with non-covalent proteins which protect it from digestive enzymes, requiring exposure to 80ºC for at least one minute for its destruction. All neurotoxins have the same mode of action, interfering with the transmission of the nerve impulse, thus inhibiting the release of the neurotransmitter acetylcholine from the nerve terminals towards the neuromuscular junction. Said interception is reversible, which will depend on the delay in the neo formation of new terminals that will replace those affected.
These discoveries promoted and encouraged the use of TB within different fields of Medicine such as Aesthetics, Ophthalmology, Traumatology, Endocrinology, Neurology, Dentistry and Otorhinolaryngology. In the latter, it is of great importance in the treatment of facial pain secondary to TMJ involvement due to bruxism.
Bruxism: definition, diagnosis and treatment
Bruxism is an oral condition of great interest to health professionals and researchers due to its high prevalence worldwide. Over time, different ways were defined to describe this pathology. Among them, the definitions proposed by the Glossary of Dental Terminology (GPT-8), the American Academy of Sleep Medicine, the 2nd. Edition of the International Classification of Sleep Disorders (ICSD-2) and the 4th. Edition of the Oro facial Pain Guide (OFPG-4). Rescuing the main characteristics of each of them, we could define bruxism as a repetitive activity of the jaw muscles characterized by clenching or grinding the teeth, accompanied or not by mandibular protrusion.5
Depending on the bibliography, it is estimated that the prevalence is between 8-70%, with no significant differences according to gender and an inversely proportional relationship to the age of the patient. It should be noted that this entity is also present in children and adolescents in a notable way, with a prevalence that reaches 40%.6
Among the possible etiologies, different theories and positions are proposed6,7 biological factors (such as dopamine, sleep arousals, central nervous system disorders, craniofacial alterations, genetic predisposition, etc).psychological factors (anxiety disorder, stress, depression). Exogenous factors (smoking, alcohol, caffeine, IRSS, cocaine, among others).
The diagnostic capacity of this disorder varies according to the resources available to the professional. The most widely used -and at the same time with less specificity and diagnostic sensitivity- are the questionnaires and the physical examination. Increasing in complexity, electromyography (EMG) is often used to finish with the current Gold standard, polysomnography (PSG).5,6
Regarding the treatment, we must take into account that the complexity of the patient is important, since the symptoms that he presents are usually exacerbated by the strong psychological-emotional component that the same pathology demands, added to the chronic disorder of the picture, for which the multidisciplinary approach should be the cornerstone of treatment. Among the measures, sleep hygiene techniques, dental containment splint, mandibular advancement devices and electrical stimulation are proposed. In the pharmacological field, clonidine, muscle relaxants and BT injection are used in the presence of masseteric hypertrophy.7 In a schematic way, it could be said that the treatment for bruxism is based on compliance with the “four Ps”8–10
Use of botulinum toxin in patients with bruxism
Literature review and mode of application
In recent years, many professionals, especially of Asian origin, have devoted themselves to the study of the use ofTBin patients with TMJ pathology. It should be noted that the companies that offer the drug do not mention its use in MM and temporarily in any section of the leaflet in order to treat bruxism. That is why today, different branches of medicine are determined to produce countless research papers in order to determine its effectiveness. Below we will name some of the most outstanding authors in the field of the last decade and their most significant contributions:
Patel et al.,11 in their systematic review (SR) of 11 studies, concludes that the use of T BIt would help to reduce pain levels and the number of bruxism events verified by EMG. He also comments that several of the patients had already failed with other more conservative treatments, so the possible results would be more encouraging if it is used as the first line. Within the limitations, he accuses that the included studies do not present a systematization in the placement of T Band the follow up was limited -with an average of 6 months-.
Fedorowick et al.,12 in accordance with the Cochrane Review system, proposed to recruit Randomized Controlled Clinical Trials and Controlled Clinical Trials where the use of BT is compared with placebo in patients with masseter hypertrophy. Unfortunately, the SR did not return any studies that met the inclusion criteria; which demarcated the need to carry out research studies of high scientific quality.
Sendra et al.,13 conducted a SR that included 6 randomized studies and 4 case series. Despite emphasizing that there is no established protocol for treatment (units to be injected, intervals, and points of application) and the follow-up time was not long, he concluded that the use of type A TB is effective in the symptomatic treatment of adult patients. with bruxism. Cheng et al.14 He included 6 studies (148 patients) in his meta-analysis. Where the use of BT was compared with placebo, and a statistically significant improvement was evidenced in the variables "Pain at rest (PR)", "Self-assessment by patients (SA)" and "Number of bruxism events (NBE)", This was not the case with the variable "Pain at chewing (`PC)" where no statistically significant differences were found). Within the limitations, he comments that the sampling Figure 3 was small and that the control group should not be a placebo since the patients generally already have some treatment established. De la Torre et al.,15 cited 5 studies in their SR (3 randomized controlled studies and 2 randomized uncontrolled studies) finding a statistically significant improvement in mandibular stiffness based on subjective evaluations while, on objective evaluations (EMG and PSG ), found no statistically relevant differences, thus concluding with contrasting results.
Long H et al.,16 conducted a SR of 4 studies (2 randomized controlled and 2 case-control) where evidence that after BT injection there is a decrease in bruxism events objectified by EMG and facial pain based on self-assessment of the patient when compared with the placebo group (injection with saline solution). However, these differences were not found to be statistically significant when compared with patients treated with oral retention plates.
Regarding the adverse events of BT injection, several studies13–19 have described a wide variety of them. In order of frequency they are: pruritus and erythema (with a recovery time of 48 to 72 hours), hematoma at the puncture site (remission between the first and second week); headache (self-limited after 4 days in 95% of cases), loss of chewing force, paradoxical pocking (product of compensation and hypertrophy of untreated superficial muscle fibers) and facial asymmetries/unaestheticism. The latter are observed after the seventh day and their resolution will depend on the effect of the BT on the muscle (30-90 days).
Taking into account the detailed evidence, we will proceed to detail a possible method of application of TB in the MM:
A thorough history-taking is of the utmost importance in order to prevent certain unwanted events or detect contraindications: pregnancy and/or lactation, allergy to albumin, Myasthenia Gravis, Polyneuropathies, collagenopathies and autoimmune diseases, surgical interventions Figure 4 in the region to be treated, amount of TB dose previously injected and brand used, among others. A bright environment is recommended to be able to visualize the facial features adequately. We will proceed to carry out a photographic record of the patient prior to the treatment and 2 weeks after the treatment. The patient will be asked to exert force on the MM to demonstrate its anterior, posterior, upper, and lower limit (green trace). It should be noted that the anterior limit of the MM coincides with the exit of the Facial Artery (curved red line), which we must avoid during the procedure.
Holding the contraction we will proceed to identify the region of greatest procidence of the muscle (green dot) which will be the epicenter of our work triangle. Then we will take into account our upper working limit (linear red line) which is obtained by projecting a line from the tragus Figure 5 to the ipsilateral labial commissure, since above this area is the Risorio de Santorini muscle – in charge of the smile in facial gesticulation. After that, we are able to make our safety triangle (the distance between the epicenter and its edges must be between 0.7-1.0 cm.)
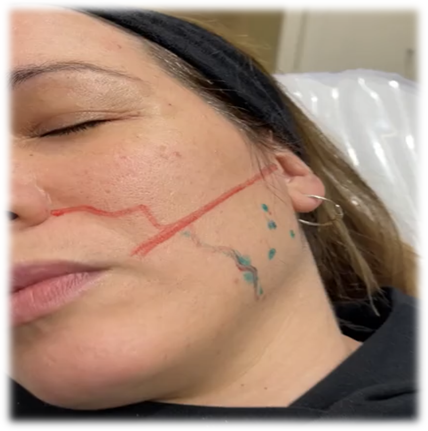
Figure 5 A 1ml tuberculin syringe with a 13mm needle will be used, the dilution used will be 2ml of physiological solution for 1 ampoule of TB Botox.
A 1ml tuberculin Figure 6 syringe with a 13mm needle will be used, the dilution used will be 2ml of physiological solution for 1 ampoule of TB Botox™. TB will be placed on the 3 edges of the triangle obtained. We will use 25U of TB Botox™ in each muscle (50U in total).
Bruxism is an entity whose prevalence and incidence are in sharp rise worldwide and is responsible for numerous physical, psychological and economic consequences. This repercussion has motivated the health field to improve its approach and therapeutic management. Currently, the knowledge of the pathology related to the TMJ has been clarified while others still continue to be a matter of debate.
Among the latter is the use of TB as a treatment for bruxism. In the grounds in favor of its application, it is emphasized that BT has 2 synergistic mechanisms to provide analgesia: On the one hand, it has antinociceptive effects, since it prevents the release of neurotransmitters related to the expression of pain, and on the other, it promotes the MM to enter a relaxation phase, which prevents its contraction, hypertrophy, and hypertonia of the muscles associated with TMJ14. However, several authors maintain that the application of BT does not significantly reduce the episodes due to the physiology of bruxism itself, where it is stated that the episodes are under the influence of the ascending reticular system of the brainstem -which contributes to the activity of networks cardiac autonomic and motor neuronal disorders-, which would explain that the proposed treatment would only influence the “final phase” of the episode without acting on its genesis.15 For these reasons, In addition to the poor quality and methodological rigor of the studies carried out to date, BT is within the therapeutic arsenal to offer to patients knowing its limitations and scope. For this reason, the multidisciplinary approach and the doctor-patient relationship are extremely important in order to be able to discuss their pathology, treatment expectations and prognosis.
None.
Authors declare no conflict of interests.
None.

©2023 Gilpin. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.