Journal of
eISSN: 2379-6359


Case Report Volume 15 Issue 3
Sri Guru Ram Rai Institute of Medical and Health Sciences, India
Correspondence: Apoorva Kumar Pandey MS (ENT), Professor Department of ENT and Head-Neck Surgery Sri Guru Ram Rai Institute of Medical and Health Sciences, Patel Nagar Dehradun, 248001, Uttarakhand, India, Tel +91 9411324477
Received: November 22, 2023 | Published: December 7, 2023
Citation: Pandey AK, Ahmed FAS, Bhardwaj A. Tuberculosis manifesting as bilateral acute parotid swelling with unilateral lower motor neuron facial palsy: an unusual presentation. J Otolaryngol ENT Res. 2023;15(3):97-99. DOI: 10.15406/joentr.2023.15.00536
A 41-year-old female presented to the otorhinolaryngology department with a history of painful swelling over the bilateral parotid region, low-grade fever for the past one month and progressively worsening left-side facial weakness for the last 15 days. She had received multiple courses of antibiotics elsewhere, which did not result in any improvement except pain. She had no past history of any comorbidities or any previous history of tuberculosis. Examination revealed that she had a non-tender, circumscribed, solitary, 3×3 cm size, firm swelling over the bilateral parotid region. Clinical signs of grade V facial nerve palsy (House and Brackmann classification) were noted. There was a severe grade left lower motor neuron facial nerve palsy (left side) seen. There was no cervical lymphadenopathy. The rest of the head and neck examination was unremarkable. Fine needle aspiration cytology (FNAC) from the most prominent part of the swelling was suggestive of granulomatous inflammation. The patient was initially treated with intravenous antibiotics, supportive care and started on antitubercular drugs (once the diagnosis was established) under the National Tuberculosis Eradication Program (NTEP) to which she responded well and after three months of therapy, her swelling and facial weakness improved significantly. In addition to reporting a completely rare kind of presentation, this paper reviews relevant literature and stresses the need for a high degree of suspicion for tuberculous parotitis in a patient with bilateral parotid swelling. The use of fine needle aspiration is important so that this curable condition can be diagnosed early and medically treated. In this way, surgical intervention can be avoided and further complications can be prevented.
Keywords: tuberculosis of the parotid gland, lower motor neuron facial palsy, anti-tubercular treatment (ATT), acid-fast bacilli (AFB)
Tuberculosis is a communicable pathological entity that usually affects the lungs but can involve extrapulmonary sites also. Out of all tuberculosis cases, extrapulmonary infections contribute about 25%, among which only 10% of cases have manifestations in the head and neck region.1,2 Salivary gland tuberculosis is a rare entity. Parotid gland tuberculosis is an uncommon event and bilateral tuberculous parotid affliction with facial nerve palsy is even more unusual and has been reported only six times in literature.1 Tubercular parotitis, being an infectious pathology, that usually presents with an increase in the gland size, and causes sialoadenitis of the gland.
Only a handful number of parotid gland tuberculosis have been mentioned in the literature. Tuberculosis of the parotid gland should be considered as a differential diagnosis in tumor cases where the pathologic swellings involve the parotid region bilaterally with/without facial nerve involvement. Prompt diagnosis and commencement of treatment are of crucial importance in preventing otological and possible intracranial involvement by the disease process. Only two hundred cases of tubercular parotitis have been cited in the medical literature yet, and the majority of those reported cases have mentioned unilateral involvement of the parotid gland, revealed from post-parotidectomy specimens.3 Here we are presenting such a unique case of bilateral tubercular parotitis co-existing with lower motor nuclear facial palsy in a female patient aged 41 years old.
A female patient, aged 41 years, presented to ENT outpatient department with complaints of bilateral painful swellings in the parotid region and low-grade fever for the past one month. There was no past history of any chronic illness, long-duration treatment, or addiction to tobacco or alcohol. On local examination of the pre-auricular regions, firm, mobile, and tender swellings were palpable on both sides. There was a swelling of size 3×2cm palpable on the left parotid region and a 2×1cm sized palpable swelling was present in the right pre-auricular region. There was no visible discharging sinus present on either side. Skin and temperature over swelling were found to be normal (Figure 1).
On further assessment, there was barely perceptible motion on gross appearance and asymmetry at rest was there. During motion, wrinkling was inconspicuous over the forehead on the left side, and incomplete closure of the left eye on maximal effort. There was also an absence of left nasolabial fold and drawing of the angle of the mouth on the right side (during smiling effort) for the last 15 days. Hence a probable clinical diagnosis of left-sided lower motor neuron facial nerve palsy [Grade V- Severe dysfunction (House-Brackmann Grading)] was assigned to this case (Figure 2). The rest of the examination was normal.
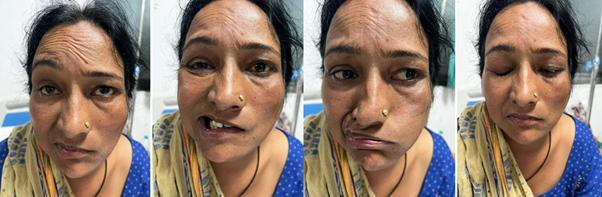
Figure 2 Left-sided lower motor neuron facial paralysis -grade V (severe dysfunction).
(a) Loss of wrinkling on frowning (b) On smiling effort (c) Blowing the face (d) Incomplete closure of the left eye. Loss of the nasolabial fold is evident in all figures (left to right).
Viral markers anti-HCV, anti-HBSAg, and anti-HIV were all non-reactive. Normal ESR (05mm/hr) and raised CRP levels (13mg/dl) were noted. All other routine hematological and biochemical reports were normal. Fine needle aspiration cytology was suggestive of granulomatous inflammation (Figure 3.1 - 3.4). Ziehl-Neelsen staining method showed no acid-fast bacilli (AFB).
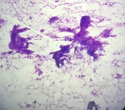
Figure 3.1 Smear shows clusters and sheets of ductal epithelial cells (parotid) embedded in a myxoid stroma (X40, MGG stain).
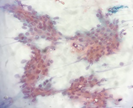
Figure 3.2 Smear shows sheets, clusters, and a few singly scattered round to oval ductal epithelial cells of the parotid gland. (X40, PAP stain).
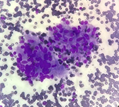
Figure 3.3 A cluster of well-formed epithelioid cell granuloma admixed with few lympho histiocytic clusters (X40, MGG stain).
Conservative treatment including intravenous antibiotics and steroid were started until the FNAC report came. Daily facial physiotherapy was also done. A chest physician’s opinion was taken with the FNAC report and they advised the patient to start ATT under NTEP. Added Tab benadon ½ tab once daily at night and repeat liver profile after 5 days. A neuro-physician opinion was also done in view of numbness and tingling sensation over the face and they advised an MRI head with CISS sequence to look for compression but the patient refused due to financial constraints. Afterwards, this patient was discharged in a satisfactory condition. She came for the follow-up after one month to OPD with improvement in facial nerve weakness (grade III- moderate dysfunction) and the size of swellings was also reduced (Figure 4).
As we already know, pulmonary involvement is the most common manifestation of the tuberculous infection but other parts of the body can also be involved. In developing countries, tuberculosis is a substantial cause of morbidities and mortalities, thus increasing the financial burden otherwise. Major salivary glands are rarely involved in tuberculosis and in addition, bilateral parotid involvement is an exceedingly uncommon event. Tubercular parotitis in a case was first mentioned in 1983 by C De Paoli.1 Tubercular infection of parotid develops clinically as a progressively increasing chronic swelling that evolves via three mechanisms; ascending mycobacterial infection from the oral cavity into the glandular duct or can involve lymph nodes via invasion of lymphatic channels or from extension of infection from a distant tubercular focus in lungs via hematogenous or lymphatic route.4 Generally, it develops as a secondary infection with its primary foci of infection in the lungs.
About 25% of cases diagnosed with tuberculous parotitis also harbor pulmonary infection.5 Pathologically tuberculosis of the parotid can manifest in two forms. The first, more common type, is the involvement of the intraglandular lymph node and the second is the glandular parenchymal involvement which is less common. The differential diagnoses of bilateral parotid swellings can be mumps, Sjogren’s syndrome, sarcoidosis, and carcinoma of the parotid gland. Tubercular infection of the parotid gland is usually diagnosed with the help of fine needle aspiration cytology which shows 81% sensitivity and a specificity ranging from 94 to 100%.2 Aspiration cytology of the parotid swellings reveals caseating granulomas of epithelioid cell clusters which is suggestive of tubercular infection.
Treatment should be instituted as early as possible to prevent complications such as xerostomia, dental caries, parotid abscess, post-aural fistula formation, septic thrombophlebitis and Frey’s syndrome, in case there be any delay in early commencement of the treatment. Anti-tubercular therapy forms the basis of the treatment of tubercular parotitis which includes a standard four-drug regimen given in the initial two months (intensive phase) succeeded by the two-drug regimen in the continuation phase for 4 months.
Parotid gland tuberculosis remains a relatively rare entity that manifests as bilateral swelling of the parotid gland along with possible lower motor neuron facial palsy. Sometimes making the diagnosis becomes an arduous and difficult task for clinicians for which they must exercise a high index of suspicion in uncertainty or even in interpretation of equivocal test results for tuberculosis. To make an early diagnosis a significant extent of suspicion aided with the judicious use of radiological and histopathological investigations is advisable. Antitubercular therapy (ATT) remains the mainstay of treatment and an early institution of drug therapy might help in preventing the wrath of debilitating complications.
None.
The authors declare that there are no conflicts of interest.

©2023 Pandey, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.