Journal of
eISSN: 2379-6359


Mini Review Volume 10 Issue 1
1Department of Ophthalmology Regional Eye Hospital, India
2Department of Radiology Surya Diagnostics, India
3Department of Neurology Vinayaka Neuro Multispecialty Centre, India
Correspondence: Anirudda Deshpande, Department of Neurology Vinayaka Neuro Multispecialty Centre Warangal Telangana, India, Tel +91-8106812222
Received: December 06, 2017 | Published: January 5, 2018
Citation: Khardenavis S, Karthik DK, Deshpande A (2018) Septo-Optic Dysplasia: A Mini Review. J Otolaryngol ENT Res 10(1): 00299. DOI: 10.15406/joentr.2018.10.00299
Septo-optic dysplasia (SOD) is an unusual medical condition affecting multiple systems of the human body especially the central nervous system, endocrinal, ophthalmological as well as rhinological apparatus. The important components of SOD are a combination of optic nerve hypoplasia (ONH), olfactory tract hypoplasia (OTH), pituitary gland hypoplasia, corpus callosum dysgenesis and absence of septum pellucidum. Etiology of SOD is not certain. It has been postulated to be associated with certain genetic mutations (which also may give rise to lobar holoprosencephaly).There is some evidence to suggest that intrauterine insults also have a role to play. Genetic mutations in the HESX1 gene have also been implicated as one of the important etiology.
Keywords: de-morsier’s syndrome, septo-optic dysplasia, olfactory tract hypoplasia
SOD, septo-optic dysplasia; OAH, optic nerve hypoplasia; OTH, olfactory tract hypoplasia; CNS, central nervous system; HPA, hypothalamic-pituitary axis; MRI, magnetic resonance imaging
De-Morsier’s syndrome or Septo-optic dysplasia is a rare medical disorder which is strongly associated with CNS, Ophthalmological manifestations. However, in minority of patients, this condition presents with olfactory tract hypoplasia. The CNS abnormalities include abnormalities of the hypothalamic-pituitary axis, hypoplasia of the optic nerve. Often, absence of septum pellucidum is seen along with thinned out corpus callosum.
SOD was first described by de-Morsier in 1956, after necropsy of a patient showed septum pellucidum agenesis and ONH. Later on in 1970, Hoyt and his team put forth the possibility of hormonal insufficiency in patients with SOD.1
It was noted that mutant mice, in whom if the novel homeobox gene Hesx 1 if disrupted manifests with the phenotype resembling SOD. Certain SOX2 mutations are associated with severe bilateral eye abnormality and defects of corpus callosum.2
SOD is not a specific entity but a spectrum of clinical manifestations. The wide range of phenotypic variability as seen in SOD patients can probably be attributed to the interaction between the environmental and genetic factors. Infants with SOD usually present very early in their life with features of jaundice, neonatal hypoglycemia, failure to thrive, seizures, unusually small size of their genital organs and delayed developmental milestones. These patients may also have strabismus, diminished vision due to optic nerve and refractive errors. There is increased incidence of mental retardation, abnormal behavior, cerebral palsy.3
Bilateral ONH may be regarded as the hallmark of SOD, although it may be seen unilaterally as well. Some of the useful predictors of long term visual outcome are initial acuity of vision, visual evoked potentials and optic disc size.4
Endocrinal abnormality, especially the dysfunction of the HPA is an important feature of SOD. It may be due to pituitary gland malformation and/or hormonal insufficiency of the pituitary.5 The deficiency of the pituitary hormone may manifest as episodes of hypoglycemia, failure to thrive, hypothyroidism or diabetes insipid us. Some studies also show deficiency of growth hormone.6
The radiological diagnosis of SOD is best established by Magnetic Resonance Imaging (MRI) of Brain. It identifies the hypoplasia of olfactory bulb, optic nerve and optic chiasma and certain malformations in the brain present congenitally.7 Some of the malformations of the brain are schizencephaly, absent septum pellucidum, abnormal ventricles8 (Figure 1-4).
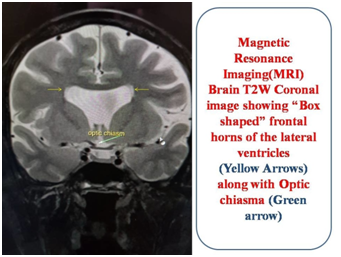
Figure 2 Shows MRI Brain T2W coronal view showing the “Box type” abnormal shape of the ventricles (yellow arrows). Optic chiasma is also seen (green arrows)
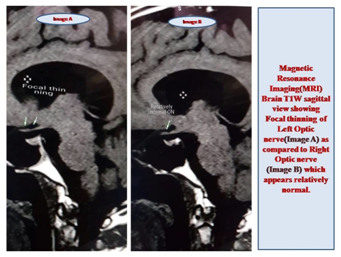
Figure 4 Image A shows MRI Brain T1W sagittal view showing focal thinning of left optic nerve as compared to the right optic nerve (Image B), which seems to be relatively spared.
Patients with SOD need to be followed up atleast once in six months to evaluate for hormonal insufficiencies, ophthalmological and Otolaryngology evaluation. Genetic counseling is an important in patients of SOD.9
Due to its multi-factorial and heterogenous nature, SOD still remains a diagnostic challenge despite the best of genetic studies and neuroimaging modalities. One should have a high index of suspicion when the patient has midline CNS defects, optic or olfactory nerve hypoplasia and signs of HPA dysfunction.
I would like to thank my parents Dr. Jayant Khardenavis, Dr. Veena Khardenavis, my brother Dr. Vikram Khardenavis & my in laws Mr. Jaikrishna Deshpande & Mrs. Kanchan Deshpande for supporting and motivating me.
Author declares there are no conflicts of interest.
None.

©2018 Khardenavis, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.