Journal of
eISSN: 2379-6359


Case Report Volume 8 Issue 6
University of Khartoum Faculty of Dentistry, Sudan
Correspondence: Amal H Abuaffan University of Khartoum Faculty of Dentistry, Sudan
Received: June 24, 2017 | Published: October 16, 2017
Citation: Altayeb TM, Eltohami YI, Abuaffan AH (2017) Diffuse Large B cell Lymphoma: Case Report. J Otolaryngol ENT Res 8(6): 00268. DOI: 10.15406/joentr.2017.08.00268
Lymphoma is malignant neoplasm arising from lymphocyte, it is a type of cancer that affects the immune system - specifically, it is a cancer of immune cells called lymphocytes, a type of white blood cell. It affects mainly young adults. African Burkett’s lymphoma affects children before the age of 12-13years old and more among males than females.1 There are two main types of lymphoma; Hodgkin's or non-Hodgkin.
Hodgkin’s lymphoma
Hodgkin’s lymphoma is a cancer of the blood and bone marrow is one of the most curable forms of cancer. The disease was called Hodgkin's disease until it was officially renamed Hodgkin lymphoma in the late 20th century
Clinical feature: Bimodal distribution (late adolescence and old age), enlarged rubbery lymph nodes, often in the neck, fever, purities, weight loss and night sweet, hepatosplenomegaly, oral lesions are rare.
Non-hodgkin lymphoma
Non-Hodgkin lymphoma (NHL), it affects the lymphatic system generally develops in the lymph nodes and lymphatic tissues. In some cases, NHL involves bone marrow and blood. It either indolent (slow growing) or aggressive (fast growing). It was predisposed by: HIV, Immune suppression, Autoimmune Disease.
Clinical feature: Oral lesions include lumps or ulcers intra orally on maxillary gingival or with bony deposits; pain, anesthesia, and swelling, loosening of teeth or pathological fracture.2 Lymphoma is definitively diagnosed by a lymph node biopsy, meaning a partial or total excision of a lymph node examined under the microscope. CT scan or PET scan imaging modalities are used to stage a cancer.3
After lymphoma is diagnosed, a variety of tests may be carried out to look for specific features characteristic of different types of lymphoma. These include: Immunophenotyping, Flow cytometry, fluorescence in situ hybridization testing.4
Classification
The classification of a lymphoma can affect treatment and prognosis. Classification systems generally classify lymphoma according to:
The WHO classification is based upon the foundations laid within the "revised European-American lymphoma classification" (REAL). This system groups lymphomas by cell type i.e. the normal cell type that most resembles the tumor and defining phenotypic, molecular, or cytogenetic characteristics. Most of the aggressive lymphomas respond well to treatment and are curable. The prognosis, therefore, depends on the correct diagnosis and classification of the disease, which is established after examination of a biopsy by a pathologist generally a hematopathologist.5,6
Treatment
Prognoses and treatments are different for HL and between all the different forms of NHL and also depend on the grade of tumour, referring to how quickly a cancer replicates. Paradoxically, high-grade lymphomas are more readily treated and have better prognoses.
Low-grade lymphomas
Many low-grade lymphomas remain indolent for many years. Treatment of the non symptomatic patient is often avoided. In these forms of lymphoma, such as follicular lymphoma, watchful waiting is often the initial course of action. This is carried out because the harms and risks of treatment outweigh the benefits. Some centers advocate the use of single agent rituximab in the treatment of follicular lymphoma rather than the wait and watch approach. Treatment for these types of lymphoma typically consists of aggressive chemotherapy, including the CHOP or R-CHOP regimen. Most relapses occur within the first two years, and the relapse risk drops significantly thereafter.
Hodgkin lymphoma typically is treated with radiotherapy alone, as long as it is localized. Advanced Hodgkin disease requires systemic chemotherapy, sometimes combined with radiotherapy.5
Prognosis: Five-year relative survival by stage at diagnosis for Localized (confined to primary site) is 82.3%.7
Case scenario
A 6-year-old female presented with a 4weeks history of pain and swelling in her left arm associated with fatigability, weight loss, night fever and sweating.
On examination
Generally the pt looks will, not jaundiced, not cyanosed, not pale. Head examination, revealed no abnormality. Neck examination, by inspection there is supraclavicular ovoid single swelling (Figure 1).
By palpation
The swelling is firm not tender' fixed to underlying structure' about 4 by 5cm in diameter' with well defined borders overlying skin is intact with normal color smooth surface with no scar and normal temperature, not pulsating, trans illumination test not applicable, other cervical lymph node is palpable but not tender. The remaining systemic examination was not significant.
Laboratory test reveal that the peripheral blood count was unremarkable (hemoglobin 136g/l, red blood cell count 8.9x, white blood cell count 3.05x, and platelet count 230x). The peripheral blood smear revealed no immature cells (41% neutrophils, 46% lymphocytes). Liver and renal functional tests, bilirubin and electrolytes were normal. ESR was 35(normal 5-20). Mantoux test was reactive (10mm).The remaining laboratory tests were all within the normal limits.
Imaging
Normal computed tomography (CT brain) was obtained (Figure 2).
CT of neck find left neck base shows subcutaneous soft mass size 5.2×4.9cm, extending into the sub-clavicles and left apical lung. The mass of regular outline mixed textures mild enhancing after I.V contrast with necrotic non-enhancing area seen. Bilateral cervical enlarged LN seen.
Radiographic Conclusion was Left Neck Base Mass with Cervical Lymph adenopathy features suggestions of Lymphoma for fine niddle aspiration cytology (Figure 3 & 4).
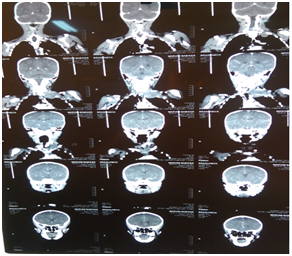
Figure 3 Coronal veiw of c.t neck reveal left side neck mass extending to subclavicular and apical part of left lung.
Fine Niddle Aspiration Cytology (FNAC) result in cellular deposits and heterogeneous lymphocytes and with mononuclear cells with primitive nuclei and deep basophilic cytoplasm and they conclude that the picture is strongly suggestive for secondary deposits. lncisional biopsy was taken under general anesthesia and the Pathological evaluation was: features of malignant infiltrative neoplasm suggestive of diffuse large cell lymphoma and immune histochemistry for CD20 '3 - CK needed to confirm diagnosis.
DLBCL is a high-grade non-Hodgkin lymphoma that has developed from B cells. It is called ‘diffuse large B-cell lymphoma’ because when it is examined under a microscope the cancerous lymphocytes are abnormally large and they are spread diffusely throughout the biopsy specimen rather than being found in clusters.
It is the most common type of non-Hodgkin lymphoma among adults.8" With an annual incidence of 7-8 cases per 100,000 people per year.
Cancer occurs primarily in older individuals, with a median age of diagnosis at approximately 70years of age, with male predilections.9 In comparison to this case which is 6years old female.
The first sign of this illness is typically the observation of a rapidly growing ma
ss, sometimes associated with fever, weight loss, and night sweats.10 Causes of diffuse large B cell lympboma (DLBCL) is not well understood but immunodeficiency like Epstein bar virus may be a contributing factor of development of subtype of disease.11
Diagnosis of diffuse large B cell lympboma (DLBCL) made by removing a portion of the tumor through a biopsy, and then examining this tissue using a microscope. Usually a hematopathologist makes this diagnosis.
Treatment: Usual treatment for each of these is chemotherapy, R-CHOP is a combination of one monoclonal antibody (rituximab), three chemotherapy agents (cyclophosphamide, doxorubicin, vincristine), and one steroid (prednisone). Through these treatments, more than half of patients with DLBCL can be cured.
Radiation therapy is often part of the treatment for DLBCL.
Diffuse large B cell lymphoma is the most common type of non Hodgkin lymphoma that require aggressive treatment thought combination chemotherapy and radiation. The germinal center subtype has the best prognosis, with 66.6% of treated patients surviving more than five years. It was a case of recurrence 2years after first treatment.
Author declares there are no conflicts of interest.
None.
None.

©2017 Altayeb, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.