Journal of
eISSN: 2379-6359


Research Article Volume 12 Issue 5
1Department of ENT and Head-Neck surgery, Sri Guru Ram Rai institute of Medical and Health Sciences, India
2Department of Pathology, Sri Guru Ram Rai institute of Medical and Health Sciences, India
Correspondence: Dr Apoorva Kumar Pandey (MS. ENT), Professor, Department of ENT and Head-Neck surgery, SGRR Institue of Medical & Health Sciences, Dehradun, 248001, Uttarakhand, India, Tel 0941132447, Fax 0135-2720151
Received: December 17, 2019 | Published: December 11, 2020
Citation: Pandey AK, Maithani T, Bhardwaj A. A case report of gingival tuberculosis:an Otolaryngologist’s perspective. J Otolaryngol ENT Res. 2020;12(5):172?174. DOI: 10.15406/joentr.2020.12.00478
Tuberculous infection of the oral cavity is an exceedingly rare clinical entity and it generally occurs secondary to pulmonary tuberculosis, with the gingival involvement as its only primary finding. Due to its rarity and atypical presentation this condition often gets misdiagnosed. We report here a case of secondary oral tuberculosis in a 44 year old male patient who presented with gingival involvement. The diagnosis was based on sputum examination, radiology of chest, montaux test and histopathology. Early diagnosis and prompt treatment is important for management of this clinical condition.
Keywords: oral tuberculosis (TB), gingiva, anti-tubercular therapy (ATT), mycobacteria
Tuberculosis is a chronic inflammatory granulomatous infection that most commonly affects lungs,but can involve almost any system of the human body. Oral lesions of Tuberculosis though unusual are evident in both the primary and secondary stages of this pathology. Farber et al reported that less than 0.1% of the cases whom they inspected, showed oral lesions.1 Tongue ulcer is the most common form of oral manifestation of tuberculosis followed by gingival involvement;2 other sites affected are the lip, cheek, soft palate, uvula, alveolar mucosa.3 Atypical clinical presentation, rare occurrence and increased chance of being overlooked or misdiagnosed result into a difficult and perplexing situation in diagnosing these lesions. The purpose of reporting this article is to have an insight into this clinical entity through an otolaryngologist’s perspective because most of these cases are examined and treated by dentists.
A 44 -year -old male was referred from the dental department to Otorhinolaryngology department with chief complaints of painless, progressive enlargement of gum and small granular lesionsonboth gumswith on and off bleeding episodes over thepast one year. There was no history of dental trauma or any dental surgery. He had been treated several times for this condition, but didn’t notice any improvement. Intra-oral examination revealed small papilliferous masses along both gingiva, in canine and molar regions, and adjacent vestibule. The gingivae were red, irregular, granular in appearance (Figure 1). It was painless to touch, but started bleeding on touch. He had a poor oral hygiene with dental caries. The rest of the ear nose throat examination was normal and there was no cervical lymphadenopathy. Panoramic X-ray (OPG) revealed multiple periapical abscesses (13,21,22,25,27), chronic generalized periodontitis and infected radicular cyst (26) (Figure 2). Blood counts revealed a slight increase in lymphocyte count and elevated erythrocyte sedimentation rate (ESR). A provisional diagnosis of inflammatory gingival enlargement was made andbiopsy under local anesthesia from multiple involvedsiteswas done. Biopsy revealed features consistent with tuberculosis, having many epitheloid cell granulomas with Langhans’ as well as a foreign body type of giant cell reaction and positive ZN staining for acid fast bacilli (Figure 3).

Figure 1 Clinical examination revealing appearance of gingivae as red, irregular, granular mass over lower and upper gingival.
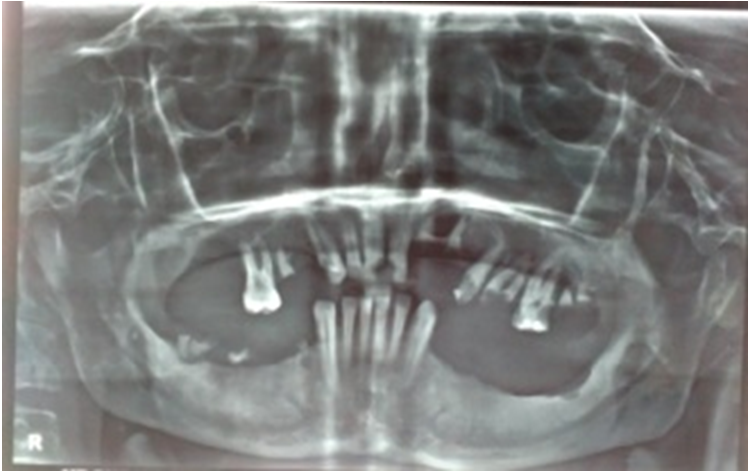
Figure 2 Panoramic X-ray (OPG) revealing multiple periapical abscesses (13,21,22,25,27), chronic generalized periodontitis and infected radicular cyst (26).

Figure 3 Biopsy revealed features consistent with tuberculosis having many epitheloid cell granulomas with Langhans’ as well as foreign body type of giant cell reaction and positive ZN staining for acid fast bacilli.
More specifically directed history, examination and investigations were done in lines of tuberculosis and further history taking revealed no cough or expectoration, hemoptysis, fever or lethargy, weight loss, evening rise of temperature, cervical lymphadenopathy or loss of appetite except weight loss of about 10 kg during the past 1 year. Chest finding on auscultation revealed bilateral coarse crepts and x-ray chest was suggestive of infiltrates in left upper and middle zone, along with a small cavity in the left upper zone. Infiltrates were also seen in the right upper zone along with a small cavity. Mantoux test was done and came out to be positive. Acid fast bacilli were detected in a sputum smear.Thus, the diagnosis of secondary gingival tuberculosis was established and anti-tubercular therapy was started with Isoniazid, Rifampicin, Pyrazinamide, and Ethambutol for initial 2 months followed by Isoniazid andRifampicin for next 4 months. The patient responded well to the ATT and is in regular follow-up.
In Indian population, the average prevalence of allforms of tuberculosis has been cited to be 5.05 per 1000, the prevalence ofsmear –positive cases is 2.27 per 1000 and the average annual incidence of smear –positive cases is 84 per million.4 It remains a major health problem in those parts of the world where HIV infection is prevalent. Increased susceptibility towards tuberculous infection in developing world emanates from various inter-related factors including poverty and poor living conditions, lack of awareness, in access to medical facilities, religious beliefs and economic constraints, available resources, malnutrition and finally treatment defaulters and therefore emergence of multidrug resistance. Among the world population, the Southeast Asian countries harbor 88% of world’s load of this dreaded entity.5
Gingival tuberculosis is caused by Mycobacterium tuberculosis, an acid fast bacillus, that is transmitted primarily via the respiratory route by inhalation of infected aerosolized droplets from a person having active disease. Occasionally it is caused by Mycobacterium bovis through ingestion of unpasteurized, infected cow’s milk or other atypical mycobacteria.6 Oraltuberculosis is rare and it is reported that only 0.05-5% of total tuberculosis cases may harbor oral manifestations.7 Oral tuberculosis can be primary or secondary. Primary gingival infection is more prevalent in children and adolescents than adults. It commonly manifests as a single painless indolent ulcer, which gradually advances from the gingival margin to the adjacent vestibule and is associated with caseation of dependent lymph nodes.2 Secondary tuberculous lesions are more frequent and are usually seen in adults. The most common sites involved are tongue, palate, lips, buccal mucosa, gingival and frenulum.8
Oral tuberculous lesions manifest as superficial non-healing ulcers, patches, gingival enlargement indurated soft tissue lesions, granular or papillary growths, lesions in jaw showing as tubercular osteomyelitis.9 The pathogenesis is generally self inoculation with infected sputum.10 although hematogenous spread can also occur. Intact oral mucosa offers resistance to invasion of tubercular bacilli. This protective function is increased due to thickness of oral mucosa, cleansing function of saliva, salivary enzymes, local pH, antibodies, all of them acting synergistically as barriers to micro-organisms.11 Besides, saliva also contains growth factors important for wound healing. Any violation in protective natural mechanismslike mucosal tears, acute or chronic inflammation may promote colonization of acid fast bacilli in the damaged region. Other predisposing factors are poor oral hygiene, extraction sockets, leukoplakia,12 local trauma, jaw fractures and irritation by clove oil, cyst and abscess.10
The differential diagnosis of gingival tuberculosis includes Wegener’s granulomatosis, sarcoidosis, syphilitic ulcer, actinomycosis, candidiasis, lymphoma, traumatic or aphthous ulcer. Clinical diagnosis of oral tuberculosis is arduous as the clinical course may exhibit atypically lacking constitutional features. A histopathologic examination revealing a granulomatous reaction and identification of the acid fast bacilli is necessary to establish the definite diagnosis and also to exclude the malignant changes. However, early identification for rapid diagnosis is warranted of M. tuberculosis in tissue specimens, as culture techniques lack sensitivity, pose technical difficulties, and demand a wait of 4-6 weeks for results.13 The cases where diagnosis requires tissue examination rather than detection of M. tuberculosis in body fluids, DNA amplification proves indispensable for detecting mycobacteria in formalin –fixed, paraffin embedded tissue specimens.14 Chest x-ray, mantoux test are done to rule out systemic tuberculosis. Anti tubercular therapy remains the mainstay of treatment.
Diagnosis of oral TB must be kept in mind when a chronic non healing ulcer, which is refractory to conservative management, is accompanied by above-mentioned varying clinical forms and predisposing risk factors. Tuberculosis persists as a potential occupational risk for health workers, particularly the dentists, otorhinolaryngologists and pulmonologists. Early suspicion and timely intervention prevent relentless progressive bone destruction.
None.
The author declares that there is no conflict of interest to disclose.
None.

©2020 Pandey, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.