Journal of
eISSN: 2471-1381


Case Report Volume 3 Issue 5
1Department of Radiology, Webimagem, Brazil
2Department of Radiology, Hospital São Camilo, Brazil
Correspondence: Marcio Luis Duarte, Webimagem, Avenida Marques de Sao Vicente 446, Sao Paulo, Sao Paulo, Brazil, Tel 55xx13981112799
Received: October 24, 2017 | Published: November 15, 2017
Citation: Duarte ML, Traple FAL, Dantas TN, et al. Thrombosed vascular incarcerated umbilical hernia-an unusual complication of chronic liver diseases. J Liver Res Disord Ther. 2017;3(5):128-129. DOI: 10.15406/jlrdt.2017.03.00070
Umbilical hernias are common in patients with chronic liver disease, caused by increased intra-abdominal pressure. In some patients the hernia contents can be the dilated paraumbilical vein. Complications are ulceration of the skin and vascular rupture, with high mortality. It can also occur thrombosis of paraumbilical herniated vein. Imaging tests are essential for the diagnosis of the contents of the sac in order to assist the treatment. Hepatocellular carcinoma is the most common primary tumor of the liver. Affects three times more men than women. The main risk factor is chronic liver disease. The imaging methods are essential for early diagnosis and to decrease morbidity and mortality. The authors report a case of a Thrombosed vascular incarcerated umbilical hernia with an MRI and ultrasound imaging tests diagnosis.
Keywords: liver diseases, carcinoma, umbilical, ultrasonography, magnetic resonance imaging
CT, computed tomography; MRI, magnetic resonance imaging; ICU, intensive care unit
Hepatocellular carcinoma is the most common primary tumor of the liver. Affects three times more men than women.1,2 The main risk factor is chronic liver disease. The imaging methods are essential for early diagnosis and to decrease morbidity and mortality.
The umbilical vein becomes the teres ligament after birth. In portal hypertension, collateral veins can rechannel the umbilical vein, forming a portosystemic shunt, called paraumbilical vein. The collateralization of the portal system with paraumbilical vein, periumbilical veins of the anterior abdominal wall and the superficial and deep epigastric veins, forming a network of dilated veins in the abdominal wall (aspect called “caput medusa”) in patients with chronic liver disease and portal hypertension is known as Cruveilhier-Baumgarten syndrome.2,3
59 years old man with confusion, dyspnea and abdominal pain for 02 days. History of hepatocellular carcinoma awaiting liver transplantation. CT scan performed 07 months earlier shows chronic liver disease with hepatic nodules, splenomegaly, dilatation of portal, splenic and superior mesenteric veins, and collateral circulation in the topography of gastric, splenic and perisplenic veins. There is recanalization of the paraumbilical vein that insinuates through the umbilical hernia with fat content.
MRI performed 04 months after the CT scan shows signs of chronic liver disease with juxtaposing hepatic nodules with peripheral enhancement, associated to satellite nodules and splenomegaly; increased caliber of portal, splenic and superior mesenteric veins, with recanalization of paraumbilical vein, inferring portal hypertension (Figure 1).
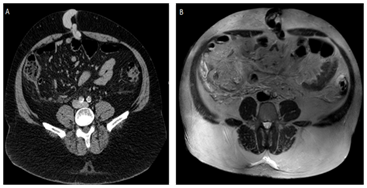
Figure 1 In A, Axial CT scans with contrast and in B, MRI without contrast in the axial T2 plane shows recanalization of paraumbilical vein insinuating through the umbilical hernia.
Ultrasound performed in attendance reveals ascites, signs of chronic liver disease and portal hypertension, such as splenomegaly, dilated splenic and portal veins, and recanalization paraumbilical vein that presents with herniated fat content. This vascular herniated segment presents thrombosed (Figure 2). After the ultrasound, the umbilical hernia was reduced manually, and patient was removed to the ICU.
The umbilical vein is echogenic and becomes anechoic after recanalization, producing the appearance of “bull's eye" in the transverse plane of ultrasound and with a vascular channel larger than three millimeters in diameter is a specific sign of portal hypertension.4 If there is herniation of paraumbilical vein, Doppler ultrasound shows the paraumbilical vein protruding through the umbilical channel during the Valsalva maneuver.5
CT scan demonstrates dilated and tortuous paraumbilical vein, coming from the left branch of the portal vein, which runs through the falciform ligament toward the belly button, forming a network of periumbilical dilated veins-the blood possibly drains into the systemic circulation through the superficial and deep epigastric veins, reaching the external iliac vein.5
Umbilical hernias are common in patients with chronic liver disease, caused by increased intra-abdominal pressure. In some patients the hernia contents can be the dilated paraumbilical vein.6Complications are ulceration of the skin and vascular rupture, with high mortality. It can also occur thrombosis of paraumbilical herniated vein. Imaging tests are essential for the diagnosis of the contents of the sac in order to assist the treatment.6
None.
The authors declare that there is no conflict of interests regarding the publication of this paper.
The written informed consent of the patient was obtained, for the publication of her case.

©2017 Duarte, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.