Journal of
eISSN: 2373-4345


Clinical Report Volume 10 Issue 6
1Department of Restorative Dentistry, Federal University of Minas Gerais (UFMG), Belo Horizonte, MG, Brazil
2Department of Biomaterials and Oral Biology, University of São Paulo (USP), Sao Paulo, SP, Brazil
3Department of Biomaterials and Oral Biology, University of São Paulo (USP), Sao Paulo, SP, Brazil
Correspondence: Carolina Bosso André, Department of Restorative Dentistry, Federal University of Minas Gerais (UFMG), Belo Horizonte, MG, Brazil, Tel 55 31 34092437
Received: November 15, 2019 | Published: November 27, 2019
Citation: André CB, Fronza BM, Giannini M. Re-intervention on a restored fractured central incisor after one year of restoration replacement: from direct to indirect approach. J Dent Health Oral Disord Ther. 2019;10(6):324-329. DOI: 10.15406/jdhodt.2019.10.00506
This clinical report elucidates both uses of direct and indirect restoration techniques, in which a failure of the direct resin restoration after one year by tooth discoloration relapse was detected, and a ceramic veneer restoration was the final elected treatment. A poor marginal adaptation and mismatching color of a class IV resin composite restoration was observed, which was placed due to a traumatic dental injury, in which part of the enamel and dentin was lost but without tooth vitality impairment. Tooth bleaching was performed combining home and in-office bleaching techniques, followed by restoration replacement with resin composite in order to improve the dental esthetic. After one year of follow up, it was observed that the restored tooth was darker and the resin shade mismatch the tooth color, showing an evident restoration margin. In attempt to achieve a long lasting treatment, substitution of the direct composite by an indirect restoration was selected, using a unit ceramic veneer restoration, and followed up for four years. Conservative approaches should be the choice treatment in restorative dentistry, however the re-incidence of discolored tooth or the restoration material degradation must be taken into consideration before indicating a direct or indirect restoration.
Keywords: resin composite, laminate veneers, tooth bleaching, dental esthetic, dental trauma
Traumatic dental injuries are common cases reported in Dentistry and may result in damage of hard dental tissues, pulpal complex, and periradicular structures. The anterior tooth, involving enamel and dentin, is the most frequent tooth affected, in which the coral fractures represents 65-75% of all dental traumas.1‒3 According to a review, for the permanent dentition the crown fractures without pulp exposure is the most common injury described in most studies.4 Also, the maxillary central incisor is the most frequently affect teeth.4,5 One of the post-traumatic complications, with and without pulp exposure, is the tooth discoloration caused by intrapulpal hemorrhage, in which the bloody degradation byproducts (such as hemosiderin, hemine, hematin and hematoidin) penetrates into the dentinal tubules staining the dentin structure.6,7 Yellow discoloration can also be correlated to pulp obliteration, another dental trauma sequel.6 The darker color, in these cases, is related to the decrease in translucence due to a greater thickness of dentin that were deposited as a response to the trauma.8,9 In cases where no pulp necrosis or signs of infection is detected, by radiographic evaluation, clinical examination and clinical signs and symptoms, the recommendation is to follow the patient without any endodontic intervention.8
A conservative intervention regarding discolored teeth by dental trauma, with no endodontic intervention, is the tooth external bleaching followed by resin composite restoration to reestablish function and esthetics when dental hard tissues are partially lost. When combined dental adhesives with direct resin placement, the treatment can be very conservative, because no previous preparation by removing sound tissue is necessary, which is a significant advantage of resin composite restorations that allow minimal intervention approach.10 However, for a successful restoration with greater longevity, the correct technique for each restorative material has to be applied. The long-term survival of the restoration is not only material-dependent,11 the time of acid etching for each substrate, proper acid removal, dentin humidity control, material placement and adequate polymerization are some critical steps that practitioners need to be cautions in order to achieve reliant and long-lasting treatments.12‒15 Besides that, some factors not related to the practitioner can also lead to restoration failure, as the re-incidence of tooth discoloration.16
When the material properties are taken into consideration, the use of ceramics veneers has some advantages. Ceramic materials presents high color stability, gloss maintenance, wear resistance, ability to mimic the restoration with the homologous tooth by using different types of pigments, and the possibility to cover the restoration margin, which gives a greater esthetics compared to direct resin composite restorations.17‒19 However, an indirect restoration, even if minimal, usually requires tooth preparation involving sound tissue.20 This clinical report elucidates both use of direct and indirect restoration techniques, in which a failure of the direct resin restoration after one year by the tooth discoloration relapse was detected, and a ceramic veneer restoration was the final elected treatment.
A female patient, twenty years old complaining about the esthetic involving her left maxillary central incisor tooth sought for restorative treatment. A poor marginal adaptation and mismatching color of the resin composite class IV restoration was observed, which was placed due to a traumatic dental injury, in which part of the enamel and dentin was lost but without tooth vitality impairment. During clinical inspection, it was noticed that this central incisor was darker than the other teeth and the restoration was too translucent (gray expect), with no signals of resin stratification to mask and give naturalness to the restoration (Figure 1). Radiography acquisition was taken and new endodontic tests were performed to ensure that the pulp tooth was still vital. A dystrophic calcification of the pulp chamber was observed, but without any periapical alterations, by the radiography image (Figure 2). The pulpal response was positive to the tests and no pulp necrosis or signs of infection were detected.
In attempt to homogenize the teeth color, external tooth bleaching was indicated, and for that, the initial shade (A2) was identified and a home bleaching and an in-office bleaching were used as combined treatment. The home bleaching (Whitness Perfect 10% –FGM Produtos Odontológicos Ltda.) was carried out for 2 weeks and the in-office bleaching (Polla Office–SDI Limited) was applied twice, in which the first application ranged from second pre-molar to second pre-molar (superior and inferior), and the second time it was applied just on the superior left central incisor and canines. The final shade obtained after these procedures was A1 to the left central incisor and canines, and a lighter shade was obtained for the other teeth (Figure 4).
The resin restoration was replaced after two weeks, to prevent bleaching sub products to interfere in the bonding process. In order to facilitate the incisal reconstruction, an addition silicon impression material was used to obtain a barrier (Aquasil EasyMix Putty – Dentsply Sirona), coping the initial palatal and incisal anatomy restoration. Thereafter the old restoration was removed with a spherical diamond bur, leaving the margins in enamel, and a bevel was done on all buccal surface, obtaining a small area with enamel in progressive depth to disguise the restoration margin (class IV). Restorations with margins in enamel are preferred to those with margins in dentin, due to greater bonding mechanism to enamel. All the restoration steps were done using rubber dam isolation to control saliva contamination and to avoid deglutition of restorative waste. Following the restoration procedure, the tooth was etched with 37% phosphoric acid for 30s in enamel and 15s in dentin and, after the acid gel rinsing (30s) and dentin moist control with absorbent paper, a single bottle adhesive (etch-and-rise: Gluma Confort Bond - Heraeus Kulzer) was applied twice with gentle air blow to evaporate the water and organic solvent. The adhesive was then light-cured using Radii-Cal (SDI Limited – Radiant exposure: 17 J/cm2). The light tip was placed as close as possible to the restoration to achieve an adequate degree of conversion of the resin material.
Four resin composite shades were utilized to reconstruct the incisal (Estelite Omega–Tokuyama Dental), matching the dentin, enamel, the incisal white halo and the translucence area. A thin layer of enamel resin shade (EB1) was placed at the silicon template, in the same area to be reconstructed, and this set of barrier and resin was adapted to the teeth and light-cured (Figure 4). After that, the dentin resin shade (DA2) was placed on top of this first increment and the dental mamelons were carved to give a natural aspect for restoration. The white halo was obtained placing a line of white shade resin (BL1) to the very end of the incisal portion, and to obtain translucence in this area, a translucent shade (Trans) was placed covering the area between the white shade and the dentin shade. To mimic the white spots found at the homologous central tooth, a white pigment (GC Corporation) was placed over the translucent resin reproducing the white lines observed in the homolog tooth (Figure 5). Covering all shades used, another thin layer of enamel resin composite was placed to finalize the restoration stratification. Each increment was light-cured separately with the same light-curing unit and its tip was positioned as close as possible to the increment. After removing the rubber dam, the occlusal contact was verified and the finishing and polishing was performed following these steps: excess removal with multi-blade tungsten bur and interproximal resin sandpaper, polished with enhance (Dentsply Sirona), extra thin Sof-Lex (3M), silicon carbide (Ivoclar Vivadent) and a diamond paste (Poli I and II - Kota) with felt (Kota).
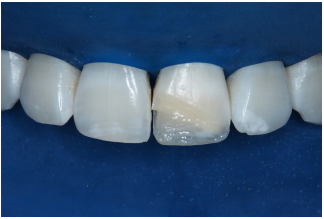
Figure 5 Resin composite restorations with incisal white halo and white pigment to mimic the white spots.
The appearance of the restoration right after the polishing procedure is shown on Figure 6. The patient was glad with the final result although a thin yellow dark line was still present. However, after one year of follow up, the patient returned presenting recurrent staining of the traumatized central incisor, which was darker than the resin restoration and the margin was more evident than the beginning, not matching the resin shade with the tooth color anymore Figure 7. For this reason, the patient agreed on removing the composite restoration and replacing it with an indirect restoration to avoid the recurrent bleaching treatment that would be required periodically. Ceramic veneer would achieve the desired esthetic, due to the better characterization and coverage of the fracture margin, which now would be placed near the gingival area.
A ceramic veneer preparation was performed maintaining margins mostly in enamel, and conserving part of the composite restoration, which was partially kept to give better palatal support (Figure 8). The amount of removed hard tissue was verified with a silicon barrier (obtained from the wax-up) to check if the thickness of the ceramic material would be able cover the discolored tooth. The prepared tooth and adjacent teeth were molded with addition silicon impression material (3M), using two dental retracting cords (Ultrapak–Ultradent Products Inc.) at the aim tooth, #000 over #00. Only the #00 cord was removed before the molding. The retraction cord facilitates the gingival finish lines molding. A resin composite provisional restoration was then temporary cemented.
The ceramic veneer was manufactured in a dental laboratory, choosing the color by the homologous central tooth and replicating the characterization found at the same tooth using lithium dissilacate ceramic (e-max CAD–Ivoclar Vivadent) and pigments. At this time, not only the white spots were mimic but also the fracture line found in the homologous central incisor. After testing the marginal adaptation, the color matching tested with the try-in cements (RelyX Veneer – 3M), and receiving the approval from the patient, the ceramic veneer was cemented. For that, a modified isolation was placed and, the prepared tooth was etched (30 s enamel and 15 s dentin–37% phosphoric acid) and a thin adhesive layer (Adper Single Bond–3M) was applied and light activated. The ceramic veneer was also etched (FGM), but with 9.6% hydrofluoric acid, the debris arising from the acidic treatment were removed in ultrasonic bath, dried and a silane layer was applied, as well as a layer of adhesive (bond–Clearfil SE Bond, Kuraray Noritake Dental Inc.), not light cured, in the internal part of the veneer ceramic. The choice of not light-curing the adhesive applied on the veneer, before cementation, was to avoid the misfit of the veneer.
Following the cementation steps, the resin cement Rely-X Veneer (TR color–3M) was applied over the adhesive-coated tooth and the ceramic veneer was placed in position with hand-pressure. The excess of resin cement was removed using a resin spatula and just than the hole set was light cured (34 J/cm2 at each surface). The final result was again approved by the patient and fulfilled the function and esthetic goals (Figure 9). After 4 years of cementation, the ceramic veneer does not show any signal of discoloration or cracks, and the gingival margin has a healthy aspect with no gingival recession (Figure 10).
Independent of the adhesive chosen, the adhesion mechanism is essential for both direct and indirect resin restoration techniques. However, the direct resin restoration offers a more conservative approach in oral rehabilitation, preserving the existing tooth structure.21 Today, the resin composites present different shades and pigments that allow the practitioner to stratify the resin to mimic the restoration to the sound tooth, giving a natural aspect of the restoration and being imperceptible.22‒24
However, even after a successful direct resin restoration placement, some factors can lead to restoration failure. These failures can be related to the material itself, as loss of gloss, pigmentation, margin evidence, wear and/or fracture,16,25,26 or due to uncontrollable reasons, as the relapse of tooth discoloration.16,24 In small to moderate-sized restorations the successful long-term performance (10+ years) of dental composite are described in clinical studies.26 Ferracane JL10 also relates two studies with overall success rates of 75% and 64%, one a 17 year and other a 22 year study, respectively, both hybrid composites placed in class I and II cavities under rubber dam. And, the predominant failures are due to secondary caries development or resin composite fractures.25,26
In literature, the recurrence of discoloration of single tooth relies on non-vital bleached teeth, no information regarding relapse in discoloration by pulp obliteration after bleaching is found. The recurrence of discoloration in bleached endodontically treated teeth is relatively high; some authors indicate a percentage of around 50% in relapse of tooth discoloration.27,28 No ideal protocol to overcame tooth relapse of discoloration is proposed, however in both cases alternative treatments over bleaching can be suggested, as direct or indirect resin composite veneers or ceramic veneers. Also, multiple bleaching treatments (periodically) can be indicated. The disadvantages regarding periodical bleaching regards on multiple chair sessions, lack of long-term color stability (after dental trauma), enamel alterations, and in same case post-operative sensitivity.28‒30 Nonetheless, all treatments options should be clarified to the patient regarding the advantages and disadvantages, and fulfill both patient and dentist expectations. Also, the practitioner need to have in mind that there are factors that cannot be controlled, resulting in failures in which a re-intervention may be necessary to restore function and esthetics to patients with loss of dental hard tissues due to traumatic dental injuries.
In cases of tooth discoloration relapse, the choice of an indirect restoration must be taking into consideration, as this type of restoration could give a greater longevity and long-term esthetic (gloss and color stability),31 but at the same time is not as conservative as a direct restoration.20 The indirect esthetic restoration has become increasingly popular and the ceramic veneers are considered an alternative to full coverage and enhances the esthetic appearance of anterior teeth.32 Also, the veneer restoration may be a minimal intervention approach, compared to indirect restorations crown,33 depending on the amount of dental tissues removed. A recent study, with follow up of ten years, compared indirect resin composites veneers with ceramic veneers, and better performance was observed for ceramic veneers, considering survival rate and quality of the long-term restorations.19 The authors reported greater differences on surface degradation and reduced gloss retention of the indirect resin composite; on the contrary, ceramic veneers presented smooth surface gloss retention after the ten years follow up.19
Conservative approaches should be the choice treatment in restorative dentistry; however the re-incidence of discolored tooth or the restoration material degradation must be taken into consideration before indicating a direct or indirect restoration, to avoid multiples treatment and to fulfill function and the patient esthetic claim.
The authors of this article certify that they have no proprietary, financial, or other personal interest of any nature or kind in any product, service, and/or company that is presented in this article. The letter of consent signed by the patient was obtained and is held by the authors.
None.
None.
The authors declare that there are no conflicts of interest.

©2019 André, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.