Journal of
eISSN: 2373-4396


« Gentlemen, Rebels and Believers: the Radial Way1) »
In 2015, the trans-radial access (TRA) has been the default route in many countries for percutaneous coronary interventions (PCI) thanks to its well-established reputation as a safe procedure,2,3 the patient’s enhanced comfort and the reduced cost mainly due to shorter hospital stays. Credits are to be granted for this major move away from the trans-femoral approach to the anatomical properties of the radial artery itself4 and to a group of “rebels and believers” who spread the ”good news” since the mid-nineties.
But the victory of the TRA over the trans-femoral approach has had a cost for this splendid vessel: radial artery occlusion (RAO). RAO stays clinically silent in the vast majority of cases, due to the rich and complex hand vascularisation but its occurrence limits further use of this route for the patient. RAO is the direct consequence of a vascular injury: injury at the puncture step, at the time of insertion of a catheter (sheath or sheath less catheter) and finally at the hemostasis-compression step, after the intervention. Minimizing the degree of injury at each step will results in a lower RAO rate. There is no longer a need to make a case for the use of the TRA but TRA-PCI believers must now spread the word of acting gently.
Slender techniques5 are comprised of any technique that reduces trauma to the radial artery. One Slender approach is the miniaturization of trans-radial coronary access devices, an obvious but not unique way to minimize vascular damage. For most PCI operators, 6F are the default size for guiding catheters (GC): this size provides adequate backup support for routine PCIs and the lumen allows passage of current stents/intra coronary interventional devices. “6F sheath” designs products that accepts 6F catheters but they are in fact larger than 6Fs: their outer diameter (o.d.) is actually around 2.62mm (for the market’s leader) or more.
The Slender technique proponents saw a welcome move(6) in 2014 when the first 6F Glides heath Slender (GSS) hit the market: thanks to its thinner wall construction, this introducer allows passage of a working 6F GC but only a “virtual 5F” sheath enters the radial artery. In fact, the 6F GSS is a little bit larger than a normal 5F sheath (o.d. is actually 2.46mm and the normal o.d. of the 5F is 2.29mm). A few months ago, the same company released a 5F GSS (o.d. 2.13mm), equivalent to a virtual 4F sheath but allowing the use of 5F Guiding catheters, bringing us even closer to a true minimally invasive cardiology practice. The next step to further extend the slender attitude for TRA-PCI should be to convince our colleagues to move away from their 6F routine use for PCIs to a 5F by default technique (with 5F GSS). The only obstacle preventing most PCI-operators to switch from 6 to 5F-guided PCI when 5F sheaths have already existed for more than a decade is fear: fear to fail the PCI attempt. Operators are afraid of backup support failure and of adequate materials availability.
But devices indeed already exists: actual wires, stents and balloon catheters are perfectly suited for work into the inner diameter of current 5F GC. More than 85 % of TRA-PCI I perform are through 5F sized catheters, leaving 6 or 7F (sheath less) catheters for true bifurcation lesions (large branches), thrombi aspiration (this indication will vanish) and TRA-CTO-PCI. With a second “true” 0.014 (0.36mm) coronary wire along the stent-delivery catheter, the 5F GC (inner diameter (i.d.) 1.47mm) allows the positioning of a 4.0mm BMS (Pro-Kinetic Energy, biotronik AG, diameter of 1.10mm at the stent level) or of a 4.0mm DES (minimum GC i.d. required: 1.42mm for both Ultimaster™, Terumo® and Orsiro, Biotronik AG). A 4.5mm BMS (Pro-Kinetic Energy, Biotronik AG, diameter of 1.21mm at the level of the stent) can be placed through the same 5F GC (use of a second wire is not possible). I have easily delivered BVS stents less or equal to 3.0mm through a 5F GC. And fortunately, miniaturization will continue to grow6 and bring increasingly efficient tools/devices to the practice, thus reducing the need for large lumen catheter/sheath.
Adequate GC support is achievable using two different but not exclusive ways: I practice both. The first one is through work on the GC’s shape: most of the current GC shapes were designed when the femoral route was the rule. Some believers (Kiemeneij, Barbeau, Ikari and others) introduced a few dedicated and better suited shapes for the radial route. I personally drew new shapes to take advantage of the special anatomy of the radial route, especially at the level of the subclavian - innominate artery. These shapes, produced by special order (Medtronic inc. and Terumo®), were clinically tested and more than 300 PCI have been performed. Reports of my preliminary experience have been presented in 2013.7‒9
Nevertheless, manufacturers are reluctant to add another family of GC given their already extensive catalogue even though only a few different curves are required for the TRA-PCI routine procedures.
For many of our colleagues however, there is no other choice than to use currently available GCs. If they want to succeed equally well using 5F GC, they have to adopt a secondary way to obtain support by using backup improving techniques. These techniques are numerous and I will only present my most practical techniques here.
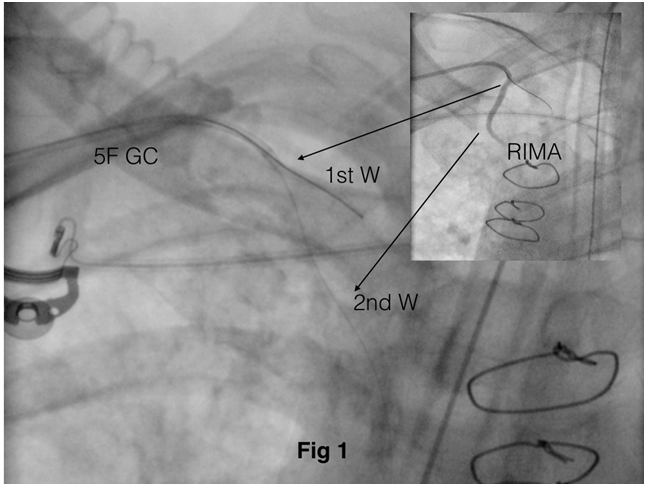
Figure 1 The use of two wires helps to stabilize a 5F GC for TRA-PCI through a RIMA graft (Anchor wiring).
To my daughter Pascal Dangoisse-Sénéchal and here coming baby for the careful proof reading.
Author declares there are no conflicts of interest.
None.

© . This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.