Journal of
eISSN: 2373-6437


Mini Review Volume 17 Issue 3
1Critical Care Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
2Pharmacy Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
3Airport Management, Sydney Kingsford Smith Airport, NSW, Australia
4Pulmonary Hypertension Department, KFMMC, Dhahran, Saudi Arabia
5ER Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
6CQI Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
7Respiratory Care Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
8Cardiology Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
Correspondence: Khaled Sewify, Critical Care Department, KFMMC, Dhahran, Kingdom of Saudi Arabia
Received: July 07, 2025 | Published: July 21, 2025
Citation: Sewify K, Elsayed A, Elmasry D, et al. The pulmonary embolism response team revolution: transforming PE management through multidisciplinary pathways. J Anesth Crit Care Open Acces. 2025;17(2):91-4. DOI: 10.15406/jaccoa.2025.17.00626
Pulmonary embolism (PE) is a life-threatening cardiovascular emergency requiring rapid, coordinated, and multidisciplinary care. A Pulmonary Embolism Response Team (PERT) model provides a framework for evidence-based, timely diagnosis and treatment of PE. This article describes the development of a standardized clinical pathway supported by risk stratification tools, advanced imaging, and a collaborative team activation protocol. The PERT pathway enables streamlined, consistent, and safe management of acute PE, improving patient outcomes while ensuring optimal resource use.
Abbreviations: BMI,body mass index; BP, blood pressure; BNP, brain natriuretic peptide; CT, computed tomography; DVT, deep vein thrombosis; PE, pulmonary embolism. NOACs,New Oral Anticoagulants.
Acute pulmonary embolism remains a leading cardiovascular emergency with significant morbidity and mortality worldwide. Its variable and often subtle clinical presentation may delay diagnosis, complicate management, and increase mortality rates.1 Drawing inspiration from a structured multidisciplinary nutrition pathway previously implemented at our institution,2 we developed standardized protocols supported by rapid multidisciplinary consultation are crucial to improve clinical outcomes in PE management. The Pulmonary Embolism Response Team (PERT) is a coordinated, interprofessional framework intended to accelerate care decisions, leverage risk stratification, and improve therapeutic interventions.3 By incorporating validated clinical tools, diagnostic algorithms, and structured communication processes, a PERT pathway offers a practical model to enhance the safety, timeliness, and quality of PE care.4
Pathway framework and screening protocol
A PERT-based pathway (as shown in Figure 1) begins with early clinical suspicion and initial diagnostic work-up, which includes:
Patients are then stratified using the Simplified Revised Geneva Score (Table 1).
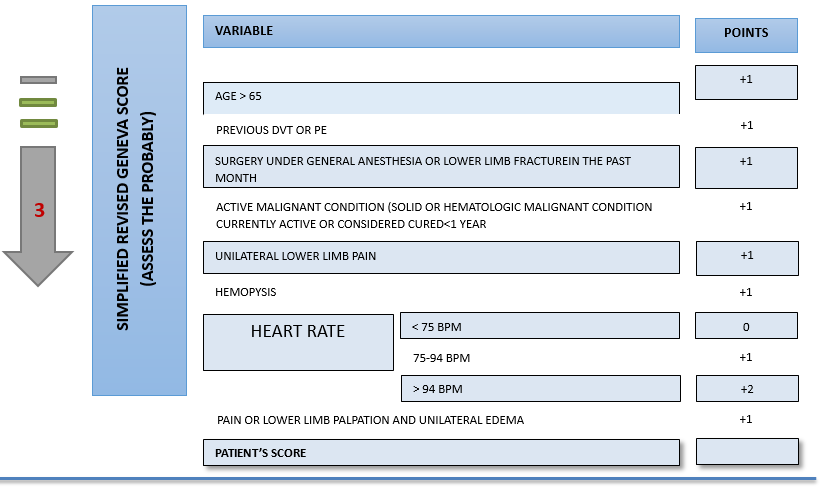

Table 1 Simplified Revised Geneva Score: patient scoring 0 to 2 are low risk (or PE unlikely), and patient ≥ 3 are high risk (or PE likely). Adapted from1
Ascore of:
For low-risk patients with negative D-dimer, PE is ruled out. In high-risk or positive D-dimer patients, advanced imaging is indicated with CT pulmonary angiography (CTPA) as first-line, and ventilation-perfusion (V/Q) scanning if CTPA is contraindicated.1
Risk stratification and escalation
Following confirmation of PE, bleeding risk is evaluated using the HAS-BLED score (Table 4) to guide anticoagulation safety³. Prognostic risk is then categorized using:
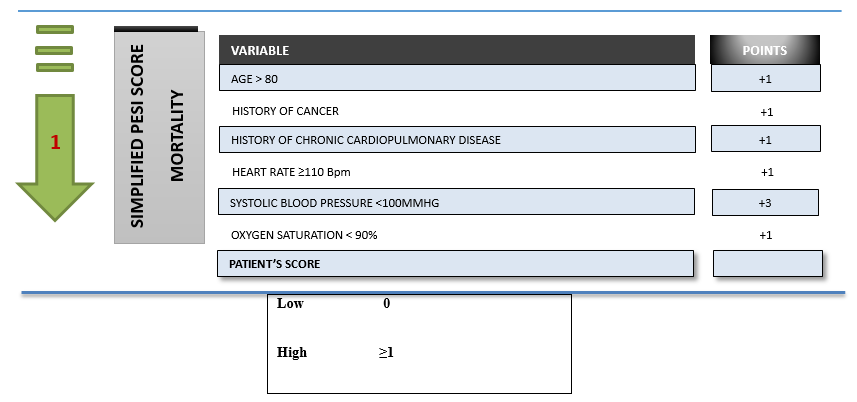
Table 2 Simplified PESI Score: Adapted from Konstantinides et al.1

Table 3 BOVA < 4: therapeutic anticoagulation will be initiated. Score ≥4 patient should be considered at high risk for a sub massive pulmonary embolus and prompt catheter directed thrombolysis initiated. Adapted from1

Table 4 HAS BLED Score: A score of 0-2 indicates low risk of bleeding; a score more than 3 indicate high risk of bleeding. Hypertension is defined as a systolic blood pressure >160mmgh. 1 point is awarded for each of abnormal renal or liver function. And drugs or alcohol3
PERT activation is triggered for:
The designated PE responder coordinates a team conference including critical care, cardiology, radiology, and hematology specialists to determine treatment priorities.2
Team roles and advanced management
A typical PERT includes:
Depending on severity, the therapeutic plan may include:
A structured Pulmonary Embolism Response Team pathway offers a pragmatic, multidisciplinary, and evidence-based model for managing acute PE. The inclusion of risk stratification scores (Geneva, PESI, BOVA), bleeding assessment (HAS-BLED), and team activation criteria improves both consistency and timeliness of PE management (1–3). By clarifying responsibilities across a multidisciplinary team and embedding decision support tools, the PERT pathway promotes standardized care and reduces variability in critical interventions. Such models have been shown to improve time to treatment, reduce complications, and potentially improve mortality.2
Clinical implications and outcomes
The PERT model supports best practices aligned with international guidelines and may serve as a benchmark for hospitals aiming to standardize PE management (1,2). Incorporating validated risk assessment, clear treatment escalation pathways, and structured team communication ensures improved coordination and patient-centered care delivery. The PERT pathway can also enhance audit readiness, promote guideline compliance, and support future quality improvement initiatives.
The multidisciplinary PERT framework described in this article demonstrates a reproducible, safe, and effective method for managing acute pulmonary embolism. Combining validated scoring tools, advanced imaging, and team-based rapid consultation supports timely and optimal PE treatment. Hospitals implementing this model can achieve better patient outcomes and strengthen quality of care.
The authors acknowledge the support of colleagues across critical care, cardiology, hematology, and radiology services who helped develop the pathway.
KS: Conceptualization, Writing–original draft, Writing–review and editing, Supervision.
The authors declare no conflicts of interest related to this publication.
No patient data are presented; pathway protocols described are available on reasonable request.
The authors declare no conflicts of interest related to this article.
No funding was received for this research from any public, commercial, or not-for-profit agency.
This manuscript is based on an institutional quality improvement pathway and complies with all ethical standards of the reporting institution.

©2025 Sewify, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.