Journal of
eISSN: 2373-6437


Research Article Volume 18 Issue 1
Hospital General de Occidente, Department of Palliative Medicine and Pain, Mexico
Correspondence: Garcia Quintero Cristopher, Hospital General de Occidente, Department of Palliative Medicine and Pain, Mexico
Received: January 16, 2026 | Published: January 27, 2026
Citation: Oscar C, Cristopher GQ, Eduardo AOG, et al. Effect of mindfulness practice on parasympathetic activity evaluated using the Analgesia-Nociception Index (ANI) in healthcare personnel. J Anesth Crit Care Open Acce. 2026;18(1):12‒15. DOI: 10.15406/jaccoa.2026.18.00643
Introduction: Healthcare personnel face high levels of work-related stress, which impacts their well-being and performance. Mindfulness practice has been shown to reduce stress and improve emotional self-regulation, possibly through an increase in vagal tone and parasympathetic activity.
Objective: To evaluate the relationship between mindfulness practice and parasympathetic activity—measured through the Analgesia–Nociception Index (ANI)—in healthcare personnel.
Methods: Clinical, prospective, and longitudinal study in 52 healthcare professionals. ANI was compared between meditators and non-meditators under controlled conditions. Parametric and non-parametric analyses were performed, in addition to adjusted ANCOVA and bootstrap analyses.
Results: Meditators showed significantly higher ANI than non-meditators (t=2.760, p=0.008), with a moderate-to-high effect size (g=0.775). The effect remained significant after adjustments for age, sex, and time of measurement.
Conclusion: Mindfulness practice is associated with an increase in vagal tone and parasympathetic activity, objectively measured through ANI. This index could be used as a physiological biomarker of autonomic well-being in mind-body interventions.
Keywords: mindfulness, Analgesia-Nociception Index, autonomic nervous system, vagal tone, healthcare personnel
Work-related stress in healthcare personnel constitutes a growing public health problem. Even before the SARS-CoV-2 pandemic, healthcare professionals presented elevated levels of stress, anxiety, and burnout, which affects their performance, the quality of care provided, and their physical and mental health.1 During and after the pandemic, these indicators have intensified, highlighting an urgent need for effective strategies for emotional self-regulation and institutional well-being. Burnout, characterized by emotional exhaustion, depersonalization, and reduced personal accomplishment, is related to hyperactivation of the sympathetic nervous system and a decrease in parasympathetic modulation.2 Parasympathetic activity, less explored but crucial for autonomic balance, can be objectively measured through the Analgesia-Nociception Index (ANI), which reflects vagal modulation of cardiac variability. In parallel, mindfulness practices, based on full attention and present-moment awareness, have been shown to reduce stress and improve emotional regulation. At the neurophysiological level, these practices modify the activity of brain regions associated with interoception, emotional control, and autonomic modulation, such as the insula, hippocampus, and anterior cingulate cortex.3 The present study seeks to evaluate whether mindfulness practice is associated with greater parasympathetic activity measured objectively through ANI, in a sample of healthcare professionals.
Theoretical backgroundThe Mindfulness-Based Stress Reduction (MBSR) program developed by Kabat-Zinn4 introduced mindfulness to the clinical setting, showing positive effects in reducing anxiety, depression, and perceived stress. Recent studies have shown that sustained meditation practice increases heart rate variability (HRV), an indirect marker of vagal tone. ANI quantifies parasympathetic modulation of heart rate in a high-frequency range (0.15-0.5 Hz). Values range from 0 to 100, where high scores indicate parasympathetic predominance and, therefore, lower physiological stress. Originally validated in anesthesia,5 ANI has also proven useful in conscious subjects under controlled conditions. The present work proposes that mindfulness could favorably modulate vagal activity, increasing ANI values compared to non-meditating subjects.
JustificationChronic stress in healthcare personnel represents a threat to mental, cardiovascular, and immunological health. The possibility of objectively measuring autonomic balance through ANI offers a promising tool to quantify the physiological impact of mindfulness- based interventions. Providing empirical evidence about this relationship will allow the incorporation of mind-body programs in healthcare institutions to be justified.
HypothesisRegular mindfulness practice increases parasympathetic activity, measured through the Analgesia-Nociception Index (ANI), in healthcare personnel. This increase is proportional to meditation experience.
Objectives feneralTo evaluate parasympathetic activity through ANI in healthcare personnel and analyze changes associated with mindfulness practice.
SpecificClinical, prospective, longitudinal, non-blind study.
Participants52 healthcare professionals were included (20 meditators and 32 non-meditators). Inclusion criteria: age ≥18 years, without serious cardiovascular diseases or use of drugs that affect autonomic tone. All participants signed informed consent; the protocol was approved by the institutional ethics committee.
ProcedureMeasurements were performed in a controlled environment (temperature 22 °C, minimal noise), in supine position, eyes closed, and spontaneous breathing. Electrodes were placed in the right subclavicular region and V3 lead, recording three minutes of stable signal. ANI was measured using a PhysioDoloris® monitor (MDoloris Medical Systems, France).
VariablesStudent's t-test for independent samples, adjusted ANCOVA (age, sex, time), and robust methods were applied: bootstrap (10,000 replications) and permutations (10,000). Effect size measures were calculated: Hedges g, Cliff's delta (δ), and probability of superiority (CLES).
Data from 52 healthcare professionals were analyzed, of whom 20 reported regular mindfulness practice and 32 reported no such practice. In the overall sample description, the mean age was 28 years (SD = 4), with a similar sex distribution across both groups. Mindfulness practitioners showed higher Analgesia–Nociception Index (ANI) values compared to non-practitioners, with an average of 75 (SD = 12) versus 67 (SD = 13), respectively, suggesting a greater parasympathetic predominance among those reporting meditation experience (Table 1). The inferential comparison between groups indicated that meditators showed significantly higher ANI values, t(50) = 2.76, p = .008, supporting a meaningful physiological difference in autonomic modulation. This pattern can be observed in the graphical representation, where a greater concentration of high ANI values appears within the meditator group (Figure 1&2). The results remained consistent in an ANCOVA adjusted for age, sex, and time of measurement, revealing an average increase of 7.8 ANI units associated with mindfulness practice, β = 7.8, 95% CI [2.1, 13.5], p = .009 (Table 2).
|
Variable |
Total (n=52) |
Meditators (n=20) |
Not meditators (n=32) |
|
Age (Years, arithmetic mean) ± DE) |
28 ± 4 |
29 ± 3 |
27 ± 5 |
|
Male sex (%) |
44.2 |
45 |
43.8 |
|
ANI (arithmetic mean ± SD) |
68 ± 14 |
75 ± 12 |
67 ± 13 |
Table 1 General characteristics
|
Test |
Statistic |
P- Value |
Interpretation |
|
Student´s t- test |
t = 2.760 |
0.008 |
Significant difference |
|
ANOVA ( time of measurement) |
F = 1.807 |
0.175 |
Non significant |
|
ANCOVA adjusted for age, sex, and time |
β = +7.8 (IC95% 2.1–13.5) |
0.009 |
Significant group effect |
Table 2 Comparison of ANI between groups
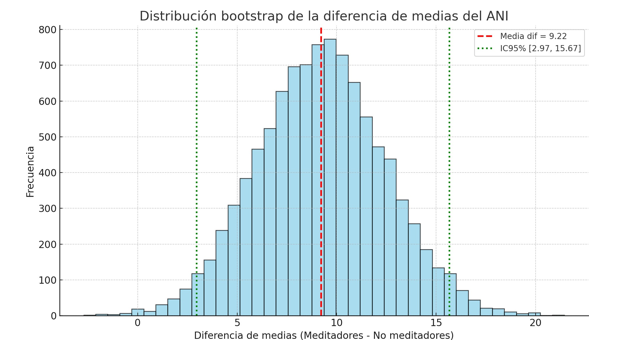
Figure 1 The bootstrap analysis with 10,000 replications showed a mean difference of 9.22 points in the Analgesia–Nociception Index (ANI) between meditators and non-meditators, with a 95% confidence interval ranging from 2.97 to 15.67. The distribution is unimodal and centered, indicating stable estimates.
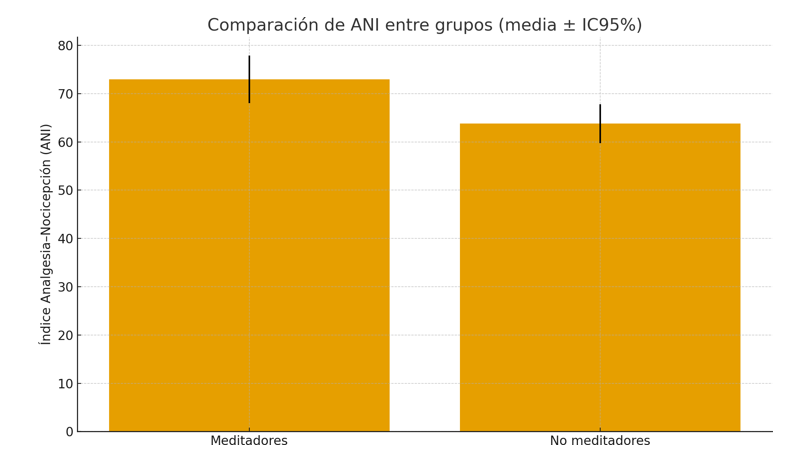
Figure 2 Meditators show a higher average ANI (~73) than non-meditators (~63), with a significant difference of ~10 points. This indicates greater parasympathetic activity in those who practice mindfulness, supporting its positive effect on autonomic balance
The effect size calculated using Hedges’ g was 0.78, corresponding to a moderate-to- large magnitude, indicating practical relevance in addition to statistical significance. The probability of superiority (CLES = 71.1%) suggests that there is approximately a 71% likelihood that a person in the meditator group will exhibit a higher ANI than a person without meditation practice. Likewise, Cliff’s delta showed a value of 0.422, confirming a moderate-magnitude difference between the groups (Table 3). To examine the robustness of the finding, a bootstrap analysis with 10,000 replications was performed, yielding an estimated mean difference of 7.6 ANI units (95% CI [1.8, 13.4]). This analysis revealed a unimodal and stable distribution of the simulated differences (Figure 2), while the permutation test reaffirmed statistical significance, p =.010. Taken together, these results consistently indicate that mindfulness practice is associated with greater parasympathetic activity among the healthcare professionals evaluated.
|
Method |
Statistic |
G5% CI |
Interpretation |
|
Hedges g |
0.775 |
0.196 – 1.354 |
Moderate-to-high effect |
|
CLES |
71.1 % |
— |
71% probability of higher ANI in meditators |
|
Delta de Cliff (δ) |
0.422 |
— |
Moderate difference |
|
Bootstrap (10,000 réplicas) |
Δ media = 7.6 |
1.8 – 13.4 |
Consistent |
|
Permutación (10,000 permutaciones) |
p = 0.010 |
— |
Significant |
Table 3 Effect size and robust methods
Participants who practiced mindfulness showed higher Analgesia–Nociception Index (ANI) values compared to those who did not meditate, and this difference was statistically significant (t = 2.760, p = 0.008). The effect size was moderate to high (Hedges’ g = 0.775; 95% CI [0.196, 1.354]), indicating that the difference is not only statistically significant but also practically meaningful. According to the probability of superiority (CLES), there is a 71% chance that a meditator will exhibit a higher ANI value than a non-meditator. This result is further supported by Cliff’s delta (δ = 0.422), which suggests a moderate difference between the groups.
When the analysis was adjusted for age, sex, and time of day of measurement, mindfulness practice continued to show a significant effect on ANI values, with an estimated average increase of 7.8 points compared to the non-meditator group (β =+7.8; 95% CI [2.1, 13.5]; p = 0.009). To assess the robustness of these findings, additional robust statistical methods were applied. The bootstrap analysis (10,000 replications) estimated a mean difference of 7.6 points (95% CI [1.8, 13.4]), and the permutation test again confirmed statistical significance (p = 0.010). Finally, no differences attributable to the time of ANI measurement were observed (F = 1.807, p = 0.175), suggesting that the effect is related to mindfulness practice rather than to the timing of the recording.
The results of this study confirm that regular mindfulness practice is significantly associated with a higher Analgesia-Nociception Index (ANI) in healthcare personnel. This finding is consistent with previous research suggesting that contemplative practices induce measurable neurophysiological and psychological changes in the autonomic nervous system.
Globally, multiple investigations have indicated that mindfulness induces parasympathetic predominance and a reduction in sympathetic tone, reflected in increases in heart rate variability (HRV), decreased respiratory rate, and improvements in cardiac coherence (Tang et al., 2009; Krygier et al., 2013; Lin et al., 2021). These changes are interpreted as greater autonomic flexibility, understood as the organism's ability to adapt to environmental demands without compromising physiological homeostasis. The present research provides complementary evidence by using ANI—a tool originally validated in anesthesiology—as an objective marker of such vagal modulation, which expands its applicability beyond the surgical setting toward contexts of occupational well-being and mental health. In the international context, studies conducted in Europe and Asia have demonstrated similar effects. For example, Lin et al. (2021) in Taiwan reported sustained increases in HRV after eight weeks of MBSR training in medical personnel, while Matousek et al. (2010) in Sweden observed significant reductions in salivary cortisol and perceived stress in hospital nurses. These results, together with those obtained in the present work, reinforce the hypothesis that attentional training and body awareness induce activation of afferent vagal pathways, facilitating states of physiological calm and emotional resilience.
Likewise, the findings are linked to Porges' polyvagal theory (2007), widely recognized in international neuroscience, which describes how stimulation of the ventral vagus nerve promotes prosocial behaviors, emotional regulation, and physiological safety. The increase in ANI observed in meditators can be interpreted as a quantifiable manifestation of this mechanism, constituting a biomarker of autonomic well-being. The validation of this marker in different cultures and clinical settings would favor its adoption in multicenter studies.
Compared to other biomarkers, ANI offers significant advantages: it is non-invasive, reproducible, and sensitive to rapid changes in vagal modulation. This makes it a tool of interest for international research aimed at evaluating the physiological impact of mind-body interventions (MBIs). The possibility of integrating ANI with other psychophysiological measures such as HRV, blood pressure, and cortisol would open new avenues to characterize the effects of mindfulness on autonomic homeostasis in a multidimensional way. Also, to our knowledge, this is the first study to use ANI to evaluate the impact of mindfulness in healthcare personnel in Latin America, making it highly relevant to highlight the importance of these practices in the hospital setting as well. However, comparison with global studies also highlights common methodological challenges: heterogeneity in training programs (MBSR, MBCT, or individual practices), interindividual variability in meditation experience, and insufficient control of contextual factors (sleep, caffeine consumption, circadian cycle). Future international studies should incorporate multicenter, randomized, and longitudinal designs that allow evaluation of the causal relationship between mindfulness practice and autonomic modulation through ANI. In addition, including culturally diverse samples would contribute to establishing the generalizability of findings and their cross-cultural relevance.7-16
In summary, the results of this study add to the international literature supporting the efficacy of mindfulness as a strategy for promoting autonomic health and preventing burnout in healthcare professionals. The adoption of objective physiological measures such as ANI strengthens the scientific rigor of this emerging field and favors the convergence between evidence-based medicine and mind-body interventions recognized by the World Health Organization as components of comprehensive well- being.
Mindfulness practice is associated with a significant increase in parasympathetic tone measured by ANI in healthcare personnel. ANI is proposed as an objective and reproducible biomarker to evaluate the physiological impact of mind-body interventions aimed at professional well-being and self-care. Implementing mindfulness programs in hospital settings could contribute to strengthening autonomic health and preventing burnout.
None.
None.

©2026 Oscar, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.