Journal of
eISSN: 2373-6437


Research Article Volume 18 Issue 2
1Anesthesiology Consultant at Somosalle Group, Brazil
2Professor of Surgical Patient Care Universidade Federal de Campina Grande, Brazil
3Anesthesiologist at the National Cancer Institute (INCA), Brazil
4Head of the Anesthesiology Service of the National Cancer Institute (INCA) Anesthesiologist, Brazil
5Geneticist at the National Cancer Institute (INCA), Rio de Janeiro, RJ, CEP-INCA Coordinator, Brazil
6Anesthesiologist at the National Cancer Institute (INCA), Brazil
7Professor of Anesthesiology at the UFG Faculty of Medicine, Responsible for the CET-SBA of the HCUFG, Brazil
8Anesthesiologist of Hospital Anis Rassi, Brazil
9Master’s in labor economics, UFPB, João Pessoa-PB, PhD student in applied mathematics and modeling, Universidade Aberta de Lisboa, Portugal
Correspondence: Dr. Luiz Eduardo Imbelloni, Anesthesiology Consultant at Somosalle Group, Av. Epitácio Pessoa, 2356/203, Lagoa, 22411-072- Rio de Janeiro, RJ, Brazil, Tel + 55.11.99429-3637
Received: February 24, 2026 | Published: March 13, 2026
Citation: Imbelloni LE, Lacerda SG, Rivoli ALC, et al. Comparative study between morphine and lateral combined femoral-sciatic at a single site for postoperative analgesia in surgery involving both plexuses. J Anesth Crit Care Open Acce. 2026;18(1):34-38. DOI: 10.15406/jaccoa.2026.18.00648
Background: Lower limb orthopedic surgeries following motorcycle accidents can be performed with spinal anesthesia, and postoperative analgesia often involves morphine along with a local anesthetic. To achieve analgesia with peripheral nerve blocks, it is necessary to block the lumbosacral plexus from L2 to S3. This study aimed to compare the use of morphine with the combined lateral femoral-sciatic block with only one puncture site.
Methods: Patients aged 18 to 60 years, after a motorcycle accident with fractures of the distal femur, knee, and proximal tibia, were included in two groups for evaluation of postoperative analgesia after surgery under spinal anesthesia. Group MO received 100 µg of morphine combined with 0.5% hyperbaric bupivacaine. Group CFS received a lateral femoral-sciatic block, with 15 ml of 0.25% levobupivacaine injected into the femoral nerve and 25 ml of the same substance injected into the sciatic nerve, accessed by neurostimulation with a 150 mm needle. The quality of analgesia, side effects, and patient satisfaction were evaluated.
Results: There was no difference between the two groups. The time to access both nerves with the neurostimulator was 3:33±0:52 minutes, ranging from 2:04 to 5:51 minutes. The average analgesia time was 18±2 hours with morphine and 21±3 hours, being highly significant. The MO group presented pruritus, nausea, vomiting, and urinary retention, which decreased the degree of patient satisfaction. All patients in the CFS group did not present any complications. Patients were followed up by telephone until the 20th postoperative day without any reported anesthetic or analgesic complications.
Conclusion: In this study, morphine presented a high incidence of side effects, resulting in decreased satisfaction. In contrast, the combined lateral femoral-sciatic nerve block with a neurostimulator puncture site was easy to perform, provided longer-lasting analgesia, and had no side effects, resulting in a higher rate of satisfaction.
Keywords: Anesthetic techniques, Spinal anesthesia, Intrathecal morphine, Femoral nerve block, Sciatic nerve block, Nerve stimulator, Analgesia Postoperative
In virtually all lower limb surgeries, a combination of blocks of the two main nerves, the femoral and sciatic nerves, is required for complete anesthesia of one of the limbs (Figure 1). However, due to the different anatomical paths of both nerves, two puncture points are necessary to achieve a complete block. Procedures on the distal femur, knee, and proximal tibia involve innervation from nerves originating from the lumbosacral plexus, corresponding to branches from L2 to S3. The femoral nerve is the main nerve of the anterior compartment of the thigh, giving off sensory branches to the anterior aspect of the knee and a terminal saphenous sensory branch to the medial side of the leg.1. Meanwhile, the sciatic nerve is the main nerve of the posterior compartment of the leg, terminating as the tibial nerve and the common fibular nerve in the popliteal fossa.1 In many public hospitals (SUS), ultrasound equipment for peripheral nerve blocks is still not available, although the vast majority do have neurostimulators.
In 2003, the anterior femoral-sciatic blockade was performed in the supine position with only one puncture site.2 In 2010, a study was conducted comparing unilateral spinal anesthesia (USA) with anterior combined femoral-sciatic block (ACFSB) in unilateral and outpatient orthopedic surgeries, showing that USA resulted in shorter procedure time, fewer attempts, and earlier recovery from the combined femoral-ischial block, but with the same effectiveness.3 Subsequently, a lateral approach to the femoral and sciatic nerves with only one puncture site, with the aid of a peripheral nerve stimulator, was published, demonstrating a novel approach to both nerves.4 An epidemiological study conducted in 2015 of lower extremity fractures following motorcycle accidents found that fractures of the distal femur, knee, and proximal tibia are more frequent.5 The aim of this comparative study in patients undergoing distal femur, knee, and proximal tibia procedures after a motorcycle accident under spinal anesthesia was to evaluate the use of morphine in conjunction with local anesthetic and lateral combined femoral-sciatic block (LCFSB) at a single puncture site for postoperative analgesia. Data during spinal anesthesia were not included in this study.
According to CNS Resolution 196/96, the Research Ethics Committee of Famene approved the project on postoperative analgesia in orthopedic surgeries comparing the single-access lateral femoral-sciatic nerve block, number 76/11 and CAAE 0075.0.351.000-11, and all patients were informed and agreed to participate in the program and signed the free and informed consent form. During the pre-anesthetic visit, the project was detailed, explained to the patient and family, and recorded in an Excel spreadsheet (Figure 2). All patients between 18 and 60 years old with fracture of the distal femur, knee or proximal tibia victim of a motorcycle accident admitted urgently to the Hospital of the Brazilian Health System (SUS) and normovolemic, without heart or respiratory disease, mental disorder, neurological disease, without coagulation disorders, without infection at the lumbar puncture site L2 to L5, who did not present agitation and/or delirium, did not use an indwelling urinary catheter, with a hemoglobin level > 10g %, who were anesthetized under spinal anesthesia who were not admitted to the ICU. All orthopedists and residents in orthopedics and anesthesia were trained for the application of the comparative study.
No pre-anesthetic medication was used. Monitoring consisted of non-invasive blood pressure assessment, heart rate, and pulse oximetry. After venipuncture with a 20G or 18G catheter inserted into the hand or forearm, fentanyl 1 ml, midazolam 1 mg, or ketamine 0.1 mg/kg was administered before performing the subarachnoid block. All patients received a Ringer's lactate infusion. Patients were divided into two groups: standard service spinal anesthesia with 100 μg of morphine (Group MO) and spinal anesthesia with lateral combined femoral-sciatic block (Group CFS).
In the MO group, with the patient in lateral decubitus or seated position, the subarachnoid puncture was performed in the L2 to L5 interspace with a 27G Quincke-point needle via the paramedian or median approach, after anesthesia of the needle tract with 1% lidocaine. After the appearance of cerebrospinal fluid (CSF), 3 to 4 ml of 0.5% hyperbaric bupivacaine was injected, supplemented in the same syringe with 100 µg of morphine, and analgesia was provided and then assessed by morphine injection. Since morphine was administered together with the local anesthetic, the administration time was not calculated.
In the CFS group, spinal anesthesia was performed in the same way, but with 0.5% isobaric bupivacaine at a dose of 7.5 mg to 15 mg, without any adjuvant, and analgesia via LCFSB at the end of the procedure. At the end of the surgery, while the effects of spinal anesthesia are still present, with the patient in the supine position and using the technique described previously, using a single 150 mm needle Stimuplex® connected to an HNS 12 stimulator (0.1 msec stimulus at 2 Hz frequency with an initial current intensity of 0.5 mA) was inserted at point of the needle.3 The needle was advanced medially from the lateral thigh, about 6 cm from the apex of the greater tuberosity, cranial and anterior until movement of the quadriceps and patella related to the femoral stimulation, then 15 mL of the anesthetic solution 0.25% levobupivacaine (S75:R25) (Figure 3). Afterwards, the needle was removed until the subcutaneous tissue and redirected posteriorly and caudally to reach the sciatic nerve, identified by stimulation of the common fibular nerve or tibial nerve, confirmed by movements of the foot. Then, 25 mL of the same anesthetic solution was injected (Figure 3). The time required to locate the femoral nerve (patellar contraction) and the sciatic nerve (contraction in the foot) and inject the local anesthetics was assessed.
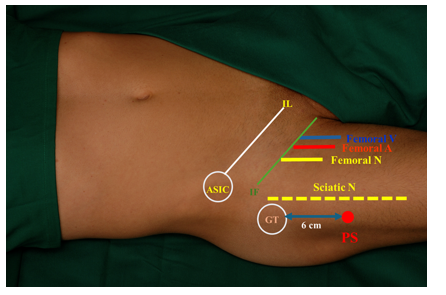
Figure 3 Combined femoral-sciatic nerve block with a single puncture site.
ASIC, Anterior Superior Iliac Crest; IL, Inguinal Ligament; IF, Inguinal Fold; GT, Greater Trochanter; PS, Puncture Site
After the injection, the duration of analgesia was evaluated in both groups, as well as side effects such as itching, nausea and vomiting, need for a urinary catheter, and other side effects. Before hospital discharge, patients were assessed based on their satisfaction levels using three questions categorized as: very satisfied, satisfied, and dissatisfied. Patients were provided with non-opioid analgesics for the treatment of postoperative pain at home. Patients were followed up by phone after hospital discharge to address any complaints related to the new technique on the 3rd, 5th, and 7th postoperative days.
Statistical analysis
Statistical analyses were performed using standard methods for comparative studies between two independent groups (MO vs CFS). Continuous variables were summarized as mean ± standard deviation (SD) or median (interquartile range), as appropriate. Group comparisons for quantitative variables were conducted using the Mann–Whitney U test (Wilcoxon rank-sum test), given the non-parametric approach adopted. Categorical variables were expressed as counts and percentages. Associations between qualitative variables and treatment group were assessed using the Chi-square test; when expected cell counts were small, the Fisher’s exact test was applied. All tests were two-tailed, and a p-value < 0.05 was considered statistically significant. Analyses were performed using R (R Foundation for Statistical Computing, Vienna, Austria).
The two groups did not differ in terms of demographic variables (Table 1). In the MO group, all patients were anesthetized with a 0.5% hyperbaric bupivacaine solution, and in the CFS group, all patients were anesthetized with a 0.5% isobaric bupivacaine solution. However, as part of the project, the various parameters of spinal anesthesia during surgery were not evaluated; only the duration of the surgery was. There was no significant difference in the duration of surgery, being 1:20±00:12 hours in the MO group versus 1:34±00:18 hours in the CFS group. After the injection, the duration of analgesia was evaluated in both groups, as well as side effects such as itching, nausea and vomiting, need for a urinary catheter, and other side effects. The time for performing the lateral CFS block was 3:33±0:52 minutes, ranging from 2:04 to 5:51 minutes for its completion, between the introduction of the needle first into the femoral nerve and injection of 15 ml of 0.25% levobupivacaine (S75:R25) and subsequently into the sciatic nerve and injection of 25 ml of the same anesthetic.
|
Variables |
Group MO |
Group CFS |
P-Value |
|
Age (years) |
39±10 |
39±12 |
0.967 * |
|
Weight (kg) |
69±10 |
68±11 |
0.5115 * |
|
Height (cm) |
169±7 |
167±9 |
0.2676 * |
|
Gender: F / M |
23 / 27 |
24 / 26 |
0.8412 ** |
|
ASA: I / II |
30 / 20 |
26 / 24 |
0.5459 ** |
Table 1 Demographic, qualitative, and quantitative variables (Mean±SD)
*Mann-Whitney test; **Fisher's exact test
The duration of analgesia produced by morphine was 18±2 hours (varying from 13 to 22 hours), while with 0.25% levobupivacaine at LCFSB, it was slightly longer, lasting 21±3 hours (varying from 16 to 28 hours), with significance (p = 0.000003956) (Figure 4). In the group with morphine in relation to side effects, itching was observed in 17 (30%) of patients, nausea and vomiting in 10 (20%) of patients, and urinary retention in 9 (18%) of patients. Urinary retention only occurred in males. In the lateral femoral sciatic nerve block group with a single puncture site, no hypotension, bradycardia, arrhythmias, nausea and vomiting, seizures, or urinary retention were observed in the PACU. With a dose of 100 mg of levobupivacaine divided between the two nerves, no symptoms of local anesthetic toxicity were observed.
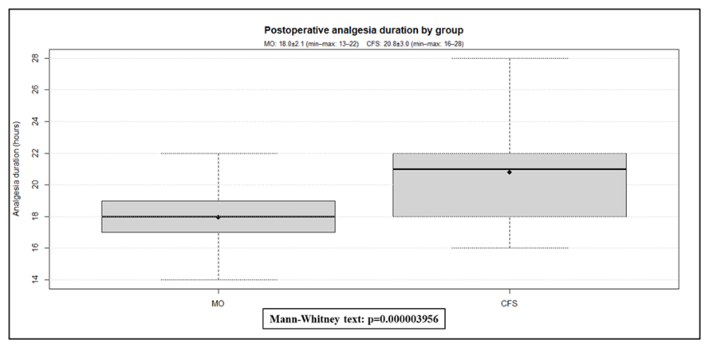
Figure 4 Post-operative analgesia in both groups.
(MO, Morphine; CFS, Combined Lateral Femoral-Sciatic Block)
Regarding patient satisfaction levels, there was a significant difference (p=0.001918), showing that LCFIB provided a very high level in all patients. In contrast, in the group that underwent intrathecal morphine, only 27 patients (54%) had the same level of satisfaction. The explanation for the lower satisfaction levels was due to complaints about side effects of the technique, such as itching, PONV, and urinary retention (Table 2). Despite the average age of the patients, none of the 100 who underwent spinal anesthesia with a 27-G Quincke needle complained of post-puncture headache. During scheduled telephone assessments, no complaints were observed from patients undergoing either type of postoperative analgesia for orthopedic motorcycle limb trauma surgeries.
|
Satisfaction |
Group MO Yes / No |
Group CFS Yes / No |
P-Value
|
|
Very satisfied |
27 / 0 |
50 / 0 |
0.001918 *** |
|
Satisfied |
2 / 14 |
0 |
|
|
Dissatisfied |
0 / 7 |
0 |
Table 2 Assessment of the level of satisfaction with postoperative analgesia treatment
***Chi-square test
This comparative study of morphine injection combined with local anesthesia and 0.25% levobupivacaine via the LCFSB with a single puncture site in a patient still under the effect of spinal anesthesia showed a significantly longer duration of analgesia, a lower incidence of side effects, and a higher degree of satisfaction among young patients undergoing orthopedic surgery of the lower limbs treated with LCFSB for postoperative analgesia. The side effects of intrathecal morphine were the cause of the lower satisfaction rate.
A retrospective study of 105 victims of motorcycle accidents that occurred in 2017 and were treated at a university hospital showed that 87 patients (82.9%) were male, with polyfractures in 61 patients (58.1%), with tibia fracture being the most frequent in 65 cases (61.9%).6 This study aimed to evaluate analgesia in the distal femur, knee, and proximal tibia, with better results when treated with local anesthetic compared to morphine. In the first study of anterior access for combined femoral-sciatic nerve block with a single puncture site, a mean time of 4.2 min (2.9 to 7.1 min) was obtained.2 In the study comparing the previous ACFSB with unilateral spinal anesthesia for orthopedic surgeries, the time to perform the block was 5.4±0.9 minutes.3 In the present study, conducted with the patient under spinal anesthesia, the time for access to both nerves via the lateral approach and injection of the local anesthetic dose averaged 3:33±0:52 minutes, ranging from 2:04 to 5:51 minutes. This value was lower than the two studies using the anterior approach, which block both nerves (femoral and sciatic).2,3
A 2015 meta-analysis of 10 RCTs comparing sciatic nerve access with neurostimulation (NS) and ultrasound (US) concluded that US guidance for sciatic nerve may improve the success rate of block and reduce the risk of vascular puncture.7 In this study, using NS and a 150 mm needle and only one puncture site, it was not compared with the use of US; however, no complications occurred during the procedure or in the postoperative period. In another study comparing combined femoral-sciatic nerve block via NS and US guidance, in 40 patients from each group, it was found that US-guided localization of both nerves outperformed NS-guided localization in execution time, needle insertion accuracy, failure rate, and occurrence of complications.8 Unfortunately, the authors do not describe the location for performing both the femoral nerve and the sciatic nerve; however, evaluating the average sensory block with US (10.67 minutes) and NS (16.68 minutes), it was much higher than in our study with a single puncture site.8
A randomized study with 60 patients comparing femoral nerve access with US and NS for postoperative analgesia following knee arthroscopy showed that both approaches did not show a statistically significant difference in efficacy, duration of analgesia, and patient satisfaction; however, needle repositioning was significantly less frequent with US.9 The results of this study and in experienced professionals using both techniques show the same success and duration of the block, with the same dose of local anesthetic. In the present study, intrathecal morphine and sciatic nerve block were compared with the NS technique alone.
In a retrospective study comparing a control group receiving continuous adductor canal block with 100 µg and 150 µg of intrathecal morphine, it was shown that both doses of morphine provide effective analgesia for total knee arthroplasty under spinal anesthesia; unfortunately, the study did not assess the side effects of intrathecal morphine.10 In our study, a fixed dose of 100 µg of morphine combined with 0.5% hyperbaric bupivacaine resulted in an incidence of itching in 30% of patients, 20% of nausea and vomiting, and 18% urinary retention, only in males. However, with LCFSB containing 0.25% levobupivacaine, none of the side effects observed with the use of morphine were noticed.
Morphine combined with local anesthetics for spinal anesthesia continues to be widely used for young patients with fractures of the distal femur, knee, and proximal tibia, particularly in cases of acute trauma and in the perioperative period, with doses ranging from 100 to 200 µg. In a recent article with patients who received only an opioid analgesic after hospitalization for a long bone fracture, and patients who received a combination of opioids and non-opioids at the time of hospital discharge showed an increased risk of developing a serious adverse drug reaction, showing that the concomitant prescription of non-opioid analgesics with opioids did not reduce the risk of subsequent serious adverse drug reactions.11 In this present study, patients were discharged home with non-opioid analgesics, and there were no reports of complications in the evaluation up to the 7th postoperative day in the group that received morphine.
In a recent study evaluating the addition of adjuvants to 0.5% hyperbaric bupivacaine, there was a decrease in the concentration of bupivacaine from 0.5% to between 0.27 and 0.37%, and in the glucose concentration from 8% to between 4.3 and 5.9%. However, the solution will always be hyperbaric, since it contains glucose.12 Femoral fracture in the elderly population is a common procedure, and often the patient is always in an antalgic position. Thus, access to the femoral nerve in the inguinal fold becomes somewhat difficult. Therefore, a lateral approach was used in 240 patients, with a single injection of 20 ml of 0.25% levobupivacaine (S75:R25) and 20 ml of 2% lidocaine with epinephrine via neurostimulator-assisted administration for pain relief before spinal anesthesia and providing postoperative analgesia, with a mean duration of 21.15±3.59, ranging from 13 to 30 hours.13 This lateral approach to the femoral nerve confirmed that there is no need for deep sedation, nor the use of opioids or dextroketamine for placement in the position for spinal anesthesia. Therefore, if a sciatic nerve block is necessary for surgery, the LCFSB technique described simply involves changing the direction of the needle from the inguinal region to access the sciatic nerve located below the femur bone.
In a laboratory study, clinical application and toxicity of levobupivacaine in excess enantiomeric form (S75:R25) in various applications such as epidural, brachial or lumbar plexus block, postoperative analgesia by bilateral pudendal nerve block, there is no report of toxicity with cardiac arrest.14 In this study, the evaluation of S75:R25 levobupivacaine in elderly patients with femur fracture provided a duration of analgesia with lumbar plexus block ranging from 14 to 33 hours, with a mean of 22±3 hours. The same results in LCFSB in both nerves for postoperative analgesia compared with morphine. This substance was used in LCFSB at a dose of 40 ml of the 0.25% solution, without any complications either in the immediate postoperative period or in the home evaluation for seven days post-operatively.
In comparison with separate access to the femoral and sciatic nerves via either US or NS, the time found in the various articles cited in the discussion was always longer than access to both nerves via the LCFSB. Furthermore, the lateral approach proved to be shorter than the anterior approach initially described and published in two articles. The combined femoral-sciatic nerve block in the recumbent position for unilateral lower limb surgery involving the distal femur, knee, and proximal tibia, from a lateral approach via a single skin puncture site with the aid of a peripheral nerve block, is an easy technique and presents better results for postoperative analgesia when compared with intrathecal morphine. Morphine, despite the usual doses used in this study, showed a high incidence of adverse effects, decreasing patient satisfaction, when compared to the combined lateral femoral and sciatic nerve block with a single puncture site, which had 100% patient satisfaction and no reported complications.
None.
None.

©2026 Imbelloni, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.