eISSN: 2377-4304


Prenatal ultrasonographic detection of labial fusion and genitourinary sinus is a rare entity and there are a few reported cases in the literature describing it. We describe a case of isolated urinary fetal ascites, labial fusion, genital urinoma associated with hydrometrocolpus and genitourinary fistula. Our case was in significant variance with what was published in literature in that the labial fusion had a lethal sequence on postnatal outcome. We presume that the presence of the tetrad of (fetal ascites, oligohydramnios, intrapelvic cystic structure and visualized urinary bladder) in a female fetus raise the suspicion of labial fusion with genitourinary sinus
Keywords: fetal ascites, hydrometrocolpus, labial fusion, genitourinary sinus, urinoma
Labial fusion is a common gynecological disorder in the pediatric population and is defined as complete or partial adherence of labia majora or minora. It is commonly seen at the age of 13-23 months with an incidence of 1.8%.1 Labial fusion can be congenital as in this case or acquired due to exposure to drugs as Danazol or due to congenital adrenal hyperplasia.2
Fetal hydrometrocolpus is one of the rarest causes of fetal cystic abdominal mass; the most frequent are those of renal etiology, bowel dilatation, and ovarian cyst.3 The causes of hydrometrocolpos may be vaginal anomalies, external genitalia malformation such as labial fusion,4 cloacal anomaly,5 and imperforate hymen.6
The mother was 23 year-old healthy 2nd gravida (previous caesarean delivery of a healthy full term new born) who was referred to our department as a case of hydrops fetalis. The Rhesus factor was RH+. The father was a healthy 26 year-old and there was no consanguinity or relevant family history. There was no history of teratogens exposure neither before nor during the current pregnancy. The ultrasonographic examination showed a single viable female fetus at 24 weeks of gestation according to composite sonographic assessment including BPD, HC and FL excluding AC because of fetal ascites.
Detailed anatomical scanning showed isolated fetal ascites, two pelvic cystic structures (Figure 1), large genital cyst (fetal sex was female) (Figure 2), severe oligohydamnios, pulmonary hypoplasia (chest circumference over abdominal circumference was 56%).
Doppler examination revealed that the anterior pelvic cyst was the bladder (two umbilical arteries running on each side) and the posterior pelvic cyst had a lower extension toward the labia and the vessel lateral to it showed doppler wave similar to uterine artery waveform (Figure 3).
We performed paracentesis of about 80cc ascetic fluid which was sent for biochemical analysis and the result was fetal urine.
Our provisional diagnosis was labial fusion with urinoma associated with hydrometrocolpus (urinary type) with genitourinary fistula.
The case was delivered by c-section by her request at 28 weeks of gestation due to premature rupture of membrane (she refused to undergo trial of VBAC).
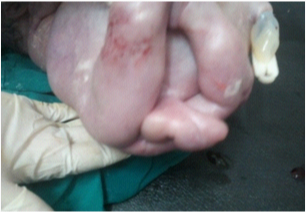
The postnatal findings revealed tense ascites, massive elongated fused labia with pinhole orifice (fluid comes out of the meatal orifice by squeezing (Figure 4), anal atresia, thoracic hypoplasia and club feet as a sequence of severe oligohydramnios.
Unfortunately the baby died after 2 hours from pulmonary hypoplasia and the parents refused autopsy.
In 2005, Shah et al.7 reported prenatal diagnosis of labial fusion and urinoma but without fetal ascites or hydrometrocolpus and the baby was doing well.
Puhl et al.4 reported a case of fetal urogenital sinus with consecutive hydrometrocolpos because of labial fusion diagnosed prenatal at 29 weeks of gestation and the prognosis was good and final reconstruction was done at 12 months of age.8
Camanni et al.9 reported a case of isolated fetal ascites secondary to persistent urogenital sinus and genitoplasty was done at 2 years old with 1 year follow up.
In an extensive review of nonimmune fetal ascites, Favre et al.10 reported ascites of urinary origin in 15 cases, posterior urethral valve were diagnosed in 14 cases and ureterocele in one.
After review of what was published in literature and to the best of our knowledge, our case is the first case report of such a severe labial fusion to the degree causing severe oligohydramnios and pulmonary hypoplasia that was in our opinion the cause of death in our case.
Also, although we did not have enough time to do cystography to the baby after delivery because of early neonatal death and although the parents refused autopsy but by logistic thinking the presence of the tetrad of (urinary ascites, severe oligohydramnios, and visualized urinary bladder and intrapelvic cystic structure) leave no possible explanation for the ascites except genitourinary sinus.
Though rare, our case should raise the suspicion of a possible labial fusion with urinoma and urogenital sinus in female fetus with ascites, oligohydramnios, visualized urinary bladder and intrapelvic cystic structure.
The underlying mechanism of such accumulation may be secondary to reflux of urine into peritoneum through the Fallopian tubes. The marked significant variance in our case from the previously reported cases is that in our case labial fusion had a lethal sequence on neonatal outcome.
Also we presume that the tetrad of (urinary ascites, severe oligohydramnios, visualized urinary bladder and intrapelvic cystic structure) in a female fetus is highly suggestive of labial fusion with urinoma and urogenital sinus.
None.
The authors declare no conflict of interest.

© . This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.