MOJ
eISSN: 2374-6939


Case Report Volume 8 Issue 3
Department of Orthopaedic Surgery and Sports Medicine, Simonian Sports Medicine Clinic, University of Washington, USA
Correspondence: Peter T Simonian MD, Simonian Sports Medicine Clinic, 729 N Medical Center Drive West, Suite 101, Clovis, CA 93611, USA
Received: May 08, 2017 | Published: June 6, 2017
Citation: Simonian PT, Simonian TL, Simonian LE (2017) Percutaneous Tension-Band Suture Technique for Distal Patella Fracture Fixation. MOJ Orthop Rheumatol 8(3): 00315. DOI: 10.15406/mojor.2017.08.00315
Patella fractures represent approximately 1% of all fractures.1 The objectives of surgical treatment include preservation of the patella to the greatest possible extent, precise anatomic reduction of the joint surface by stable fixation and restoration of the knee-extensor mechanism, thus allowing early mobilization.2,3 Posttraumatic osteoarthritis can result from articular incongruity.4 The most commonly used technique for managing patella fracture fixation involves a modified tension-band wiring technique.4-7 with longitudinal Kirschner wires (K-wires) and 18-gauge stainless steel wire in a figure-of-eight pattern looped over the anterior surface of the patella, through an extensile incision. The tension band technique neutralizes tension forces anteriorly produced by the extensor mechanism at knee flexion and converts them into stabilizing compressive forces at the articular surface.7 This technique was further modified by different authors using either K-wires or cannulated screws with different stainless steel wire configurations. These techniques using metallic wires can result in symptomatic hardware, with reported rates up to 60 %.3,8,9 For this reason, some have advocated the use of nonabsorbable sutures such as braided polyester, lowering the rate of revision surgery secondary to symptomatic hardware.3,10-14 Studied suture material has included number 5 Ethibond (Ethicon, Somerville, NJ, USA), number 5 Ti-Cron (Davis and Geck, Gosport, Hampshire, UK) and number 5 FiberWire sutures (Arthrex, Naples, FL, USA).
FiberWire has presented a significantly higher failure load than stainless steel wire. Furthermore, it was observed that unlike stainless steel, FiberWire maintained its initial stiffness until failure.15 A recent study demonstrated that a modified tension band using FiberWire sutures showed satisfactory clinical results with low incidence of complications and reoperations.10 The usual surgical intervention is carried out through an extensile skin incision with a substantial soft tissues dissection sufficient for fracture and joint-surface visualization. Wide surgical incisions are associated with a higher probability of postoperative adhesions.16 prolonged disability for work as well as a scarring.17 The presence of lacerations or abrasions around the operative site may delay the surgery through a traditional midline incision.1
In contrast, percutaneous surgical techniques preserve the vascular supply of patellar fragments, which may improve fracture consolidation. However, this treatment has been reported to be technically demanding and not applicable to all fracture patterns.18 Surgical treatment of transverse patella fractures with this percutaneous technique utilizing cannulated screws with a tension band wiring technique, combining the advantages of rigid internal fixation and minimally invasive surgery has shown to provide satisfactory clinical results and excellent knee functions, with less pain and low incidence of complications.19 We describe a case report of a transverse distal patella fracture treated with both the combined advantages of a minimally invasive percutaneous technique along with a non-metallic FiberWire suture tension band.
We report a case of a 15 year old female who sustained a left side transverse distal patella fracture (Figure 1) while participating in tack and field upon landing after long-jump. After a thorough discussion of non-operative verses operative treatment, the patient and her parents elected to move forward with fixation of the fracture to promote healing, allow early mobilization and minimize the risk of displacement. Because of minimal displacement, it was elected to move forward with a previously described suture tension band technique using #5 FiberWire.10 The unique aspect of this case is the percutaneous placement of this figure-of-8, tension band suture fixation (Figure 2).
Four small incisions were made, each measuring 3-5mm. Two on either side of the proximal patella tendon or two more on either side of the distal quadriceps tendon. Labeled 1-4 (Figure 2). A large straight Keith needle was used to pass the suture starting from point 1 to 2, through the patella tendon at the inferior pole of the patella (Figure 3). The free suture end from point 2 is subcutaneously retrieved to point 3 with a Hewson suture passer (Smith and Nephew, Andover MA) (Figure 4). This free end of this suture is then passed from point 3 to 4 is with a straight Keith needle, through the quadriceps tendon at the superior pole of the patella. Finally, the other free suture end is retrieved from point 1 and delivered to point 4 (Figure 5). The free suture ends are then tensioned and tied at point 4 (Figure 6), completing the figure-of-8 tension band. A small tenotomy scissor was placed into each of the four incisions freeing the bursa from the tension band suture. Once all skin adhesions were clearly released, the four small incisions were closed, each with a single nylon suture.

Figure 2 Diagram demonstrating percutaneous tension band suture technique. Numbers 1-4 represent the sequential placement of the sutures. A straight Keith needle is used to place the suture from point 1 to 2, through the patella tendon. The free suture end from point 2 is subcutaneously delivered to point 3 with a Hewson suture passer. The suture from point 3 is delivered to point 4 with a straight Keith needle, through the quadriceps tendon. Finally, the free suture from point 1 is delivered to point 4, subcutaneously with a Hewson suture. The free suture ends are tensioned and then tied at point 4.
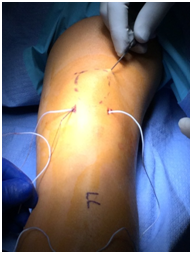
Figure 4 Hewson suture passer subcutaneous retrieval of the free suture end from patella tendon, point 2, and delivering to the quadriceps tendon, point 3.

Figure 5 Keith needle placing the retrieved suture through the distal quadriceps tendon, point 3 to 4.
We describe a successful treatment of a transverse distal patella fracture utilizing a novel percutaneous application of a previously reported suture tension band technique using #5 FiberWire.10 Immediate mobilization was started after surgery. The patient was allowed to weight-bear as tolerated with the leg locked in extension for the first 6 weeks after surgery. Immediate post-operative range of motion was initiated, limiting flexion to 90 degrees for the first 6 weeks. Range of motion was no longer limited after the first 6 weeks. This case demonstrates both the advantages of suture fixation and the advantages of percutaneous fixation. The suture fixation minimizes the chance of a second surgery to remove symptomatic metallic hardware. The percutaneous technique avoids wide surgical incisions which can be associated with a higher probability of postoperative adhesions.16 prolonged disability for work, as well as a skin scar formation.17 The percutaneous surgical technique preserves the vascular supply of patellar fragments, which may improve fracture consolidation.
None.
None.

©2017 Simonian, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.